Skin and soft-tissue infections (SSTIs) can be caused by many agents [e.g. Streptococcus species and methicillin-susceptible Staphylococcus aureus (MSSA)], but recently a substantial increase of methicillin-resistant S. aureus (MRSA) SSTIs has been reported [Reference Elixhauser and Steiner1]. The reporting of hospital discharge data is mandatory for all acute-care hospitals in the USA and the resulting dataset has been the sole source for certain analyses [Reference Elixhauser and Steiner1, Reference Klein, Smith and Laxminarayan2]. The strengths of hospital discharge data include their ability to capture information regarding all hospital discharges, to standardize disease categories by using the International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM) codes [3], and to capture electronic records of hospitalizations. Weaknesses include coding errors and failure to take account of outpatient and emergency care visits.
Combinations of diagnostic codes have been used to define MRSA SSTI because no single ICD-9 or ICD-10-CM code exists for MRSA SSTI [Reference Hasty4]. Multiple codes relate to SSTI; others are associated with S. aureus infection as a whole and, before October 2008, a separate code denoted any bacterial infection with penicillin resistance, which had been used as a proxy code for methicillin resistance; since then a separate code has been introduced to designate methicillin resistance. Combinations of these three sets of codes have been used to describe trends in MRSA hospitalizations [Reference Elixhauser and Steiner1]. Although these studies demonstrate an increase in MRSA incidence, research evaluating the accuracy and representativeness of using hospital discharge data with these combinations of ICD-9-CM codes is limited.
To provide insight into the strengths and limitations of using hospital discharge data and ICD-9-CM codes to describe paediatric MRSA SSTI trends, hospital discharge data were compared with data collected during a 6-month active surveillance period for paediatric patients with laboratory-confirmed community-acquired MRSA SSTI and who were hospitalized in Los Angeles County (LAC) during 2003 (considered the reference standard). This analysis (1) determined the sensitivity and positive predictive value of multiple ICD-9-CM code combinations to calculate MRSA SSTI hospitalization incidence rates for 2003; (2) determined the representativeness of using a set of three groups of ICD-9-CM codes to define MRSA SSTI for 2003; and (3) calculated the trend of hospitalization incidence for MRSA SSTI in children in LAC during 1998–2006 compared to trends of other SSTIs.
During 5 May–7 November 2003, the LAC Department of Public Health (DPH) required physicians and hospital infection control practitioners to report paediatric patients who were hospitalized with MRSA infection. Patients with presumed healthcare-associated acquisition of MRSA were not reported. Medical records were collected and reviewed to verify the diagnosis of an MRSA infection leading to hospitalization. Additional information collected included patient demographics, home address, primary diagnosis, laboratory results, length of hospital stay, isolate source, treatment, and outcome. Patients were selected if they were a LAC resident, were aged <18 years in the study period and had a laboratory-confirmed MRSA SSTI leading to hospitalization in LAC; these cases were considered the standard as they were laboratory confirmed.
All LAC acute-care hospitals, except federally administered institutions, are required to transmit hospital discharge data on every admission to the California Office of Statewide Health Planning and Development (OSHPD). The OSHPD hospital in-patient discharge database includes, among other variables, basic demographic information (e.g. age, sex, and race/ethnicity), county of residence, dates of hospitalization, principal and ⩽24 secondary diagnosis codes categorized using ICD-9-CM. The available dataset does not include any person-specific unique identifiers.
To determine the predictive value of ICD-9-CM codes, the May–November 2003 OSHPD data were compared with laboratory-confirmed case data reported to LAC DPH since these dates coincided with the individual case reporting period. Only data from hospitals that reported cases of MRSA SSTI were included so that the hospital discharge data represented the same hospitals as reported cases. To describe trends in MRSA SSTI, the OSHPD datasets were used that included admissions for the years 1998–2006 from all non-federal LAC hospitals. The following ICD-9-CM codes were used to define SSTI: 680.0–681.00 (carbuncle and furuncle), 681.10, 681.9–682.9, 684, 686.8, or 686.9 (cellulitis and abscess). For MRSA, the combination of the S. aureus ICD-9-CM code (041.11) and the penicillin-resistance (V09.0) codes was used, i.e. MRSA SSTI was defined by the V09.0 code, the S. aureus code and one SSTI code. When SSTI was the primary code for a MRSA SSTI case this combination was defined as the reference definition. MSSA was defined as any S. aureus ICD-9-CM code without the penicillin-resistance code and Streptococcus infections were defined by ICD-9-CM codes 041.0–041.09. To define MSSA SSTI and Streptococcus SSTI, hospital discharges that were coded with both a SSTI code and a respective bacterial infection code were used.
Basic demographic information was described by using frequency and means. Sensitivity and positive predictive values of each of the ICD-9-CM groups were calculated by comparing hospitalized patients with laboratory-confirmed infection and a particular set of codes with all other hospitalized laboratory-confirmed cases. Specificity and negative predictive value could not be calculated due to the lack of a comparative group of hospitalized children with negative laboratory tests for MRSA SSTI. To determine representativeness of the reference ICD-9-CM code, we compared patients' age, sex, race/ethnicity, and length of hospital stay for laboratory-confirmed cases meeting the definition with all other patients not meeting this definition. ANOVA was used to test the difference in means in age and length of hospital stay. χ2 test was used to examine differences in frequencies of race/ethnicity and sex. Alpha was set at 0·05.
Hospitalization incidence per 100 000 residents was calculated for children aged <18 years at time of admission by using hospital discharge data for 1998–2006. The numerator was either the number of MRSA SSTI cases, by the reference definition, the number of MSSA SSTI cases, or the number of Streptococcus SSTI cases. The denominator was the year-specific LAC population for children aged <18 years and was a longitudinal population estimate based on 1990 or 2000 census data. Age adjustment was performed by direct standardization with the 2000 U.S. census standard population for children aged <18 years. Trends of MRSA, MSSA, and Streptococcus SSTI were plotted by hospitalization incidence per 100 000 residents for 1998–2006. Data were managed and analysed in Microsoft Access 2003 (Microsoft Corporation, USA) and SAS version 9.1 (SAS Institute, USA).
In total, 140 hospitalized paediatric patients with laboratory-confirmed MRSA SSTI were reported from 31 hospitals during May–November 2003. Patients had a mean age of 6·5 years; approximately half were female, and approximately half were Hispanic. The most common diagnoses were cellulitis (41%), abscess (44%), and abscess and cellulitis (11%). No deaths occurred. Of the 140 cases, 133 (95%) had exact matches to records in the hospital discharge data from 29 different hospitals and could therefore be linked. Table 1 illustrates the sensitivity and positive predictive value of multiple ICD-9-CM combinations. Most, 78% (n=104), of reported laboratory-confirmed cases had hospital discharge codes that included an ICD-9-CM code for SSTI; 73% (n=97) of cases had SSTI listed as the principal diagnosis. S. aureus was coded for in 47% (n=62) of the cases; 38% (n=50) of the reported laboratory-confirmed cases were coded as V09.0 (resistant to penicillin) in the discharge database. Sixteen percent (n=21) of cases did not have a code for SSTI, S. aureus, or penicillin resistance. A total of 74 012 hospital discharges occurred among LAC residents aged <18 years through 29 LAC-reporting hospitals during the study period (Table 1), of which, 889 (1·2%) had an ICD-9-CM discharge code for SSTI, 390 (0·5%) for S. aureus, and 190 (0·3%) for penicillin resistance. The reference definition had the highest positive predictive value (49%) for confirming a case of MRSA SSTI in the hospital discharge data.
Table 1. Sensitivity and positive predictive value of different ICD-9-CM combinations for MRSA skin and soft-tissue infection (SSTI), compared with laboratory-confirmed paediatric-associated cases, Los Angles County (n=133)
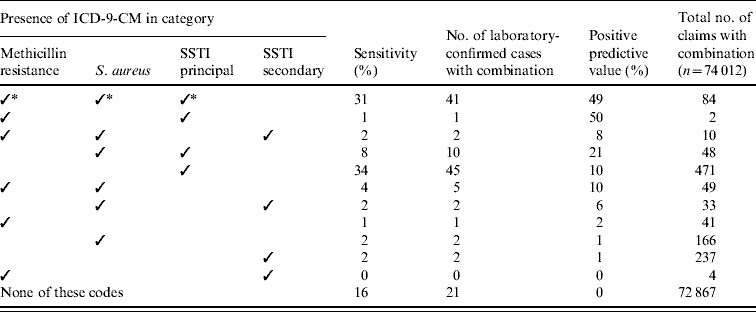
* Reference code.
We compared the 41 cases meeting the reference definition with the 87 cases having other listed code combinations and found no statistically significant difference between mean age and length of stay between the groups or in frequency of race/ethnicity and sex.
A total of 1348 MRSA SSTI, 1020 MSSA SSTI, and 210 Streptococcus SSTI paediatric cases occurred during 1998–2006. There was a sharp increase in MRSA SSTI discharges in 2002 but MSSA incidence rates increased steadily over time, whereas streptococcal SSTI incidence rates remained the same (Fig. 1).
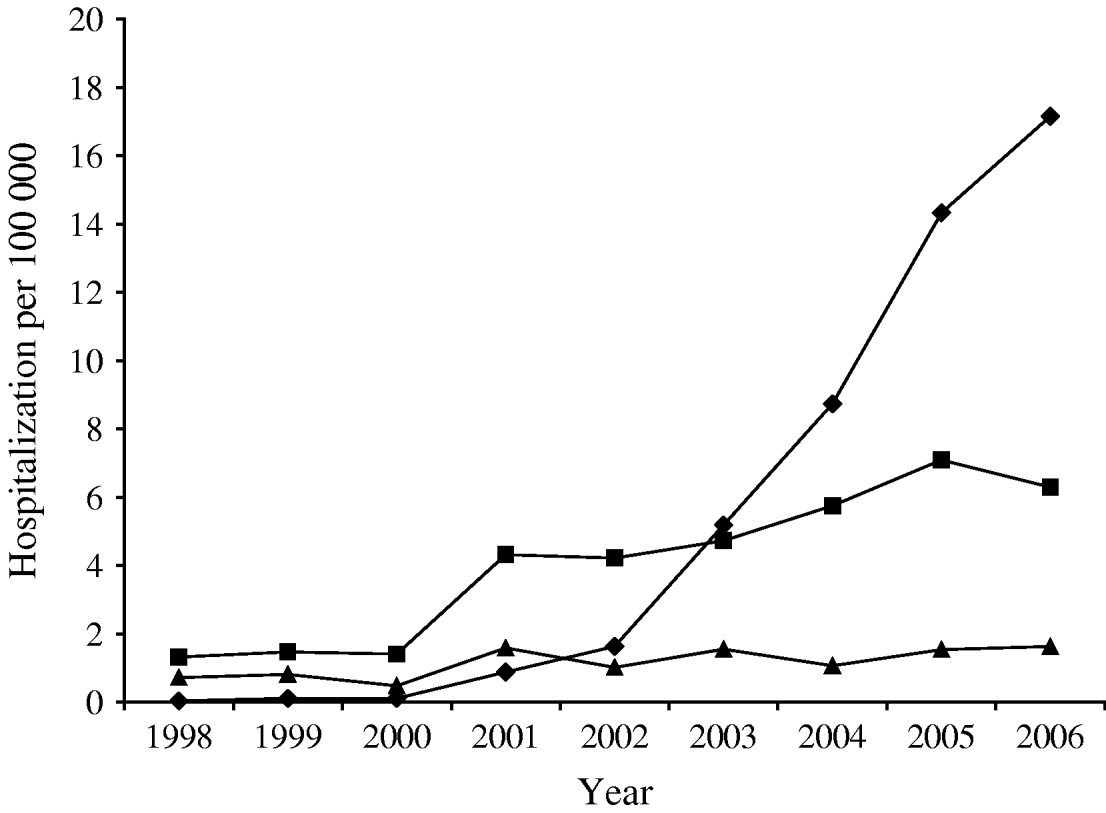
Fig. 1. Age-adjusted trend of hospitalization across time, 1998–2006 for methicillin-resistant Staphylococcus aureus (MRSA, –◆–), methicillin-susceptible S. aureus (MSSA, –▪–), and Streptococcus species (–▴–) skin and soft-tissue infection (SSTI) cases in paediatric patients, Los Angeles County.
This study differs from previous MRSA SSTI studies using hospital discharge data because we examined the accuracy and representativeness of ICD-9-CM hospital discharge data, compared to laboratory-confirmed cases of hospitalized children with MRSA SSTI. We found that a combination of three sets of ICD-9-CM codes (the reference definition) had one of the highest positive predictive values, although only 49%. Furthermore, those laboratory-confirmed cases meeting the reference definition were representative of all reported MRSA SSTI cases, in terms of age, sex, race/ethnicity, and length of hospital stay, compared to cases coded in other ways. Although the proportion of Hispanics in the study is substantial, it is commensurate with the general LAC population where 60% of children aged <18 years are Hispanic.
Hospital discharge data do not include emergency department or outpatient visits; therefore, not all paediatric-related cases are included. Many SSTI cases may be seen in these settings. For example, Hasty et al. [Reference Hasty4] found that 22% of children visiting an emergency department for SSTI had positive cultures for MRSA. Additionally, using this cluster of ICD-9-CM codes for case-finding underestimated the burden of MRSA SSTI, as only 31% of all confirmed cases were accurately identified by these codes. However, other ICD-9-CM code combinations resulted in lower positive predictive values apart from the combination of two cases of SSTI with penicillin resistance which had a positive predictive value of 50%. Consequently, although the incidence of MRSA SSTI might be underestimated, there is value in using these codes to determine trends in hospitalization. The denominator for the positive predictive value includes all cases with a certain combination of ICD-9-CM codes but patients not represented in the numerator (a case) may have been diagnosed with nosocomial MRSA SSTI or other SSTIs. As no comparison group of children who were negative for community-acquired MRSA infection was collected, discharged patients may have included unreported cases of community-acquired MRSA. Consequently, the resulting positive predictive values may have been biased towards the null.
A dramatic increase was observed in paediatric MRSA SSTI incidence in LAC for 1998–2006. During the same period, a steady increase in the number of MSSA SSTIs also occurred, but no change was evident in the number of streptococcal SSTIs, the latter finding being probably indicative that the increase of SSTIs caused by all S. aureus was not due to more hospitalization of children with SSTIs. Of note, the concurrent rise in MSSA SSTIs might in part be the result of miscoding of MRSA as MSSA as was the case for 10% of our laboratory-confirmed cases. Comparison of reported paediatric laboratory-confirmed cases with the total data showed that not all cases are coded the same way. Reasons for this might include charts being coded before laboratory results were available, poor clinician documentation or simple misclassification. The majority of confirmed MRSA SSTI cases were correctly coded as SSTI but the use of this code alone captures skin infections other than those caused by MRSA. A misclassification bias was evident in hospital discharge data, but it is non-differential (towards the null). Thus, the use of a case definition with a higher positive predictive value (e.g. the reference definition) can be an accurate means of representing the trend of MRSA SSTI cases but not necessarily yield a precise incidence of disease.
The use of hospital discharge data has its shortcomings. For example, hospitals that did not report cases to LAC DPH during the 6-month period might have coded differently from those that did report cases. Further, a networked-model health management system is better able to track patients' activities and link the laboratory isolation of infectious agents with SSTIs. In addition the lack of unique patient identifiers in hospital discharge data means duplicates cannot be removed, particularly regarding multiple hospitalization of patients.
To apply hospitalization trends to all cases of MRSA SSTI, one should account for changes in practice over time. LAC physicians in 2003 often treated patients in an in-patient, rather than outpatient, setting, as MRSA was then relatively rare in LAC; the county had its first MRSA SSTI outbreak in 2002. Patients who were hospitalized probably had more severe infections, although our analysis did not examine severity and so, the demonstrated upwards trend probably underestimates the burden of all MRSA SSTI cases but highlights the most severe of these. Moreover, codings have changed since 2003. Code V09.0 was standardized by the National Center for Health Statistics' ICD-9-CM Coordination and Maintenance Committee (U.S. Department of Health and Human Services, Centers for Disease Control and Prevention) to be a surrogate for methicillin resistance. Hospital coders might not have become familiar with the new code immediately and as the disease became more prevalent and the codes were used more, the precision and accuracy of the data might have changed.
Unlike other hospital discharge data sets, the OSHPD database can hold ⩽24 secondary diagnoses codes. A study examining common diagnoses and procedures noted an increase in sensitivity, specificity, and reliability using 25 fields compared with five fields [Reference Romano and Mark5]. Thus, our ability to detect cases might have been improved with our dataset compared to studies that used fewer diagnoses codes. Errors in California's OSHPD data have been noted by others. Green & Wintfeld [Reference Green and Wintfeld6] reported a 9% (95% confidence interval 7·2–10·8) difference in principal diagnosis between the database and medical records while another group that compared self-reported conditions from the California Teachers Study to OSHPD data [Reference Marshall7] found that only 7% of infectious diseases were reported by the cohort in the OSHPD data. As the current study did not confirm diagnosis with medical records, the reason for underreporting of infections in OSHPD is unclear but is probably indicative of coding and coding procedures.
Differing combinations of ICD-9-CM codes have been used to define MRSA. Elixhauser & Steiner [Reference Elixhauser and Steiner1] used the V09.0 code alone to define MRSA in a healthcare cost and usage project. As V09.0 is also used for penicillin resistance, other infections (e.g. penicillin-resistant pneumococcal infections) might have been captured. Their study did not give a definition of SSTI but noted that 46 000 hospital stays resulting from MRSA infection, for all ages, had the principal diagnosis of skin and subcutaneous tissue infections; 6·2% of those patients were aged <18 years. Two other studies [Reference Klein, Smith and Laxminarayan2, Reference Kuehnert8] using the National Hospital Discharge Survey defined MRSA in the same way and used the S. aureus-related codes 038.11, 482.41, and 041.11. They determined the number of MRSA infection cases by multiplying the number of S. aureus cases by the proportion of methicillin-resistant infection recorded in The Surveillance Network database. In these studies, SSTIs would be categorized under ‘other S. aureus infections’ and Klein et al. [Reference Klein, Smith and Laxminarayan2] also noted an increase in hospitalization during 1999–2005.
In conclusion we have demonstrated the accuracy and representativeness of sets of ICD-9-CM codes in hospital discharge data for identification of MRSA SSTI cases. Although lacking sufficient precision for incidence calculations these data might provide an alternative for passive surveillance of incidence trends for MRSA SSTI. The recent introduction of a single code for MRSA means that only two codes are necessary to define MRSA SSTI. Nevertheless, the need to use previous ICD-9-CM and ICD-10 codes remains as databases preceding the adoption of the single code will provide important baseline incidence rates for MRSA and allow review of trends over the last decade.
ACKNOWLEDGEMENTS
The authors gratefully recognize Diana Bensyl, Ph.D., Susan Hathaway, R.N., Grace Run, M.S., David Dassey, M.D., Michael Jhung, M.D., M.P.H., Rachel Gorwitz, M.D., M.P.H. and Van Ngo, M.P.H. The findings and conclusions in this report are those of the authors and do not necessarily represent the official position of the Centers for Disease Control and Prevention.
DECLARATION OF INTEREST
None.




