INTRODUCTION
There are over 200 000 elderly residents in care homes with nursing facilities in England and Scotland [source: The state of social care in England 2005–2006: Commission for Social Care Inspection (CSCI) and The Care Commission, Scotland 2005]. While some of these care homes provide exclusively residential care, a majority have a varying proportion of patients requiring 24-hour nursing care. Those requiring nursing support have range of functional disability and disease. For many years it has been recognized that many of the elderly care-home residents are vulnerable to a variety of infections including healthcare-associated infections. It is now acknowledged that efforts to prevent and control healthcare-associated infections in the elderly should include the institution of good infection control practice not only in the hospitals but also in nursing homes [Reference Stone1, Reference Stone2]. The national guidelines [3] recommend that the nursing homes should receive 24-hour infection control support. Despite the existence of guidelines, many nursing homes have been found to have unsatisfactory infection control support and as such may be responsible for poor infection control practice in these nursing homes [Reference Tunney, Hughes and Magee4, Reference Mayon-White and Grant-Casey5].
The aim of this study was to evaluate whether enhanced infection control support in nursing homes has any impact in improving infection control practice in nursing homes.
METHODS
For the purposes of this study only care homes with nursing facilities were included and are referred to as nursing homes.
Twelve nursing homes in South London were included in the study between the period October 2005 and February 2007. The study was conducted as a cluster randomized trial (CRT). We chose cluster randomization because the intervention was naturally applied at the cluster level.
The nursing homes were randomized into two groups of six nursing homes. Matched-pairs randomization was done by number of residents. In one group (intervention group), the improved infection control measures described below were introduced. The other group of nursing homes served as the control group.
An Infection Control Team (ICT) consisted of a dedicated infection control nurse who was supported by a senior nurse specialist in infection control and an infection control doctor. The ICT facilitated the implementation of good infection control practice in each of the nursing homes in the intervention group. This included teaching and training for healthcare workers and other nursing-home staff in the prevention and control of MRSA, Clostridium difficile infection and other common infections including catheter-associated infections. The ICT also provided training on aspects of environmental cleanliness, hand hygiene and disposal of clinical waste, including sharps, as part of general training in infection control. The ICT provided personal alcohol-containing gels to improve hand hygiene. In addition, 24-hour telephone support for management of specific infection control problems such as the need for isolation of infected patients or other special measures required was also provided to the nursing homes in the intervention group.
Structured interviews were conducted with the managers of the nursing homes. The questions were based on previously recommended standards [6]. These guidelines detail the standards for accountability, processes, capability, monitoring and practice requirements for infection control in nursing homes. Questions not applicable to the nursing homes were excluded.
Hand hygiene facilities, environmental audit and compliance with safe disposal of clinical waste was audited using a previously validated standardized audit tool for monitoring compliance with infection control guidelines within the community including nursing homes [Reference Millward, Barnett and Thomlinson7]. This infection control audit tool provides organizations with a standardized method for monitoring clinical practice and the environment to enable staff to systematically identify where improvement is needed, to minimize infection risks and enhance the quality of patient care. Specifically the audit tool assesses the environment, ward/departmental kitchens, handling and disposal of linen, clinical waste management, safe handling and disposal of sharps and management of patient equipment [8].
Independent infection control nurses who were previously trained in community infection control audits performed the inspections of both groups of nursing homes at the beginning and end of the study. Scores were classified as minimal compliance (⩽75%), partial compliance (76–84%) and compliant (⩾85%).
Variables recorded at care-home level were: number of beds available, number of residents, gender and age distribution, proportion patients requiring nursing care, number of elderly mentally ill residents, percentage of patients with catheters, number of incontinent patients, number and distribution of care-home staff and agency staff. This information was obtained from the nursing-home managers.
The primary outcome measure was proportion of compliance with infection control guidelines set out in the infection control audit tool for the community.
Statistical methods
Comparison of compliance outcomes by group (control vs. intervention) was done using two-sample t tests on the differences from baseline to post-intervention Significance level was set at P<0·05. Data were analysed using Stata (Stata Corp., USA) and SPSS (SPSS Inc., USA) statistical software.
The study was approved by the Guy's and St Thomas' Hospitals Ethics Committee.
RESULTS
The nursing homes varied in the facilities provided and the number and type of residents in the control nursing homes (A–F) and intervention nursing homes (G–L) (Table 1). One of the nursing homes in the control group (nursing home A) had a substantially higher number of nursing care beds compared to other nursing homes in either of the groups. Nursing homes also varied in the provision of elderly mentally ill (EMI) beds. Only two nursing homes in the control group and three in the intervention group provided EMI beds.
Table 1. Characteristics of the nursing homes
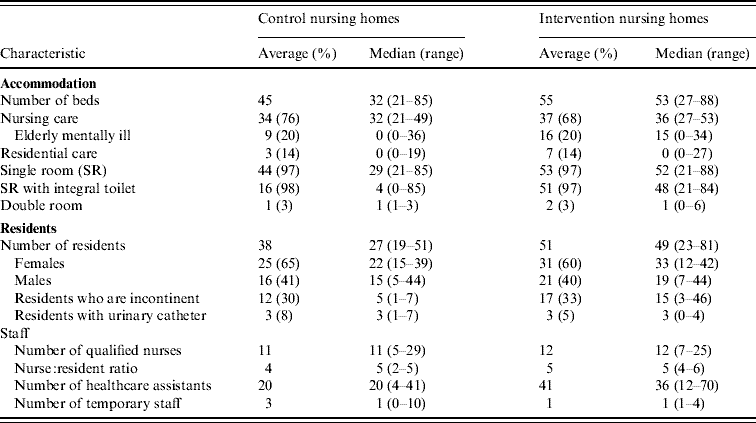
Infection control organization
The infection control organization and implementation of guidelines were assessed in each of the nursing homes at the beginning of the study. The responses to some of the key questions in the structured interview are summarized in Table 2. None of the nursing homes were compliant with all the recommendations.
Table 2. Infection control management: responses to key questions
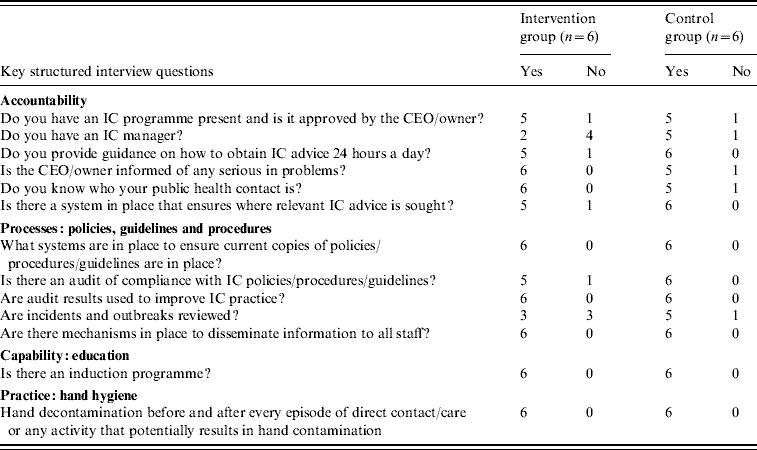
CEO, Chief executive officer (if the nursing home is part of a larger corporation); IC, infection control.
Infection control audit before and after intervention (Tables 3 and 4)
Hand hygiene facilities
At the time of baseline observations, hand hygiene facilities were variable in both groups. In the control group, only one nursing home was compliant in provision of adequate hand hygiene facilities and in the intervention group two nursing homes were compliant. At the time of final observations, three of the control group and four of the intervention group were compliant. There was no statistical difference in compliance between the two groups at baseline and final observations.
Table 3. Infection control audit
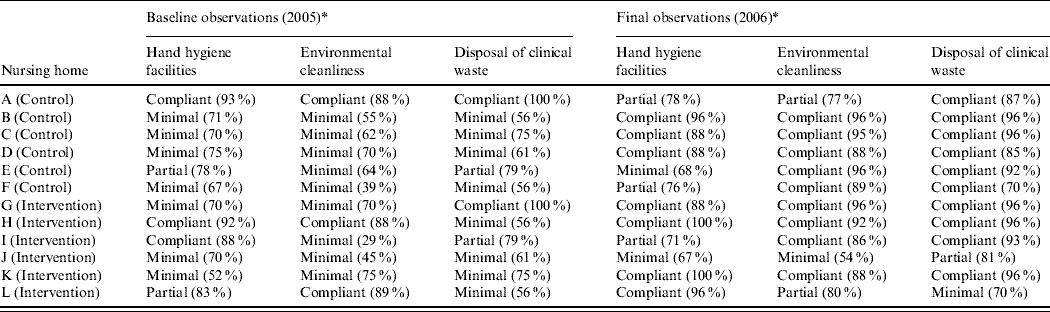
* Scores were classified as minimum compliance (⩽75%), partial compliance (76–84%) and compliant (⩾85%).
Table 4. Statistical analysis of changes in compliance before and end of study

CI, Confidence interval; T1, baseline observations; T2, final observations; n.s., not significant.
Environmental cleanliness
At the time of baseline observations, environmental cleanliness was variable in both groups. In the control group, only one nursing home was compliant in an audit of environmental cleanliness and in the intervention group two nursing homes were compliant. At the time of final observations, five of the control group and four of the intervention group were compliant. There was no statistical difference in compliance between the two groups at baseline and final observations.
Disposal of clinical waste
At the time of baseline observations, adequate facilities for disposal of clinical waste were variable in both groups. In the control group, only one nursing home was compliant in provision of adequate facilities in each of the control and intervention groups. At the time of final observations, five of the control group and four of the intervention group were compliant. There was no statistical difference in compliance between the two groups at baseline and final observations.
DISCUSSION
Given the vulnerability of elderly and frail residents of nursing homes to infections, infection control arrangements in nursing homes in the UK are included in the inspections by the regulatory authorities. For 2005–2006, CSCI (England) data show that 27% of older people's homes with nursing facilities did not meet national minimum standards for hygiene and infection control (response of Chairman of CSCI, 2 March 2007, Hansard). Similarly, the Care Commission in Scotland found that in 2005, 21% of the inspected nursing homes did not meet at least one recommendation about infection control and of these 10% did not meet a regulatory requirement (review of cleanliness, hygiene and infection control in nursing homes for older people 2005, Scottish Commission for Regulation of Care, 2005).
Furthermore, many nursing homes have unsatisfactory infection control support and as such may be responsible for poor infection control practice in these nursing homes.
In a classic study in the USA, Haley et al. established that an effective infection control programme supported by an infection control nurse and infection control physician was highly effective in reducing infections in hospitals [Reference Haley9]. Although it may not be possible to undertake all aspects of a comprehensive infection control programme in nursing homes, it is conceivable that improved infection control support may improve infection control practice in nursing homes. Tunney et al. reported that in a questionnaire-based survey of nursing homes in Northern Ireland, only 23% of the nursing homes had any visits from the public health departments and 75% of the 318 respondents expressed a desire for more information on MRSA and infection control support [Reference Tunney, Hughes and Magee4]. As a result the authors of that report concluded that these nursing homes needed additional support and monitoring mechanisms. In an audit of infection control practice in 42 nursing homes in England, Mayon-White & Grant-Casey reported that these nursing homes listed among their educational needs free in-service lectures, guidelines and action plans [Reference Mayon-White and Grant-Casey5]. Similar findings have been described in audits of infection control facilities in the USA [Reference Khabbaz and Tenney10, Reference Mody11].
However, it is unclear whether insufficient infection control training and support for the staff in the nursing homes is responsible for poor practice. Furthermore, there is currently insufficient evidence to conclude that improved support will necessarily lead to improvement in infection control practice.
To the best of our knowledge this is the first reported prospective CRT to study the effect of enhanced infection control training and support on infection control practice in nursing homes.
In the following sections we discuss the results, their implications and the limitations of the study.
Overall, there was partial or poor compliance with the guidelines in the intervention and control groups. Although we used the Scottish guidelines, the subsequently published infection control guidelines for nursing homes in England make similar recommendations. We are concerned whether compliance with these guidelines is feasible in smaller nursing homes.
Measurement of compliance with infection control practice
Comparison of the baseline observations with observations made at the end of the study showed that that at the beginning of the study, there was overall poor hand hygiene facilities, environmental cleanliness and disposal of clinical waste in the intervention and control groups. At the end of the study, both groups showed substantial improvement in compliance with hygiene facilities, environmental cleanliness and disposal of clinical waste. The greatest improvement was seen in disposal of clinical waste and the least improvement was seen in hand hygiene facilities. However, there was no statistical difference between the intervention and control groups.
It is conceivable that the impressive improvements in disposal of clinical waste could be due to the recent legislation regarding disposal of clinical waste and awareness of legal consequences for failing to dispose of such waste safely [Hazardous Waste Regulations (2005) and The Carriage of Dangerous Goods and Use of Transportable Pressure Equipment Regulations 2004 (CDGTPE) and the CDGTPE (Amendment) Regulations 2005].
It was encouraging to note that there was an improvement in cleanliness of the environment in both groups. An increase in general awareness among nursing-home staff and patients may have contributed to this improvement.
The only exception to the overall trend of improvement was ‘nursing home A’ where the compliance in all three areas of observation (hand hygiene, environmental cleanliness and disposal of clinical waste) deteriorated at the end of the study. The reasons for this deterioration are not clear.
Limitations of the study
As a first study to explore the effect of infection control support in nursing homes we acknowledge that our study had several limitations.
The number of nursing homes included in the study was relatively few and as such the study may have been inadequately powered to detect the differences. In addition all nursing homes were not identical in their facilities, e.g. single rooms, and this may have contributed to differences in compliance with infection control practice.
A principal limitation of the study was that were not able to assess hand hygiene compliance. As the originators of the hand hygiene compliance tool recommended by the Department of Health (England), we were acutely aware of the importance of measuring hand hygiene compliance [12]. However, because a majority of the residents were allocated single rooms, it was felt that hand hygiene compliance through direct observation within the confines of a single room would be intrusive and subject to the ‘Hawthorne effect’ [Reference Haas and Larson13]. We attempted to use counting of used personal alcohol gels as a surrogate marker of compliance but despite our best efforts, we were unable to persuade the staff to consistently return used bottles. The difficulties in accurately measuring hand hygiene compliance in hospitals has been described in a recent review [Reference Haas and Larson13]. We suggest that measuring hand hygiene compliance can be even more challenging in a nursing-home setting.
Although we could not detect major differences between the intervention and control groups, the managers were frequently unable to produce corroborative evidence to support their responses to the structured interviews. We also found that the guidelines on the structured interview did not reflect the requirements of varying sizes of the nursing homes included in this study. A further limitation was that prior to randomization all participating nursing homes had to be informed of the aim of the study. It is therefore possible that the responses to the interview may have been biased. Furthermore, the outcome variables (hand hygiene facilities, environmental cleanliness, and safe disposal of clinical waste) were only indirectly addressed by the intervention, which consisted of teaching, training, and support of an infection control team. The outcome variables are more related to the nursing-home management, therefore the pre-intervention interview may have resulted in improvements in both groups due a ‘Hawthorne effect’.
We did not assess the impact of enhanced infection control support on nursing-home-acquired infections with organisms such as MRSA as an outcome of the intervention as no reliable surveillance mechanisms were available in the nursing homes included in the study. For assessing nursing-home-acquired infection with MRSA it would have been necessary to screen all residents. We were not given ethical approval to repeatedly screen and identify individual residents as it may lead to stigmatisation within their place of domicile. Without identifying individual patients, it would have been difficult to monitor nursing-home-acquired infections.
CONCLUSION
Since infection control practice improved in the intervention and control groups, we could not demonstrate that provision of short-term, enhanced, infection control support had a significant impact in infection control practice in nursing homes. Further research is necessary to identify whether long-term support and other infection control strategies are necessary to improve infection control practice in nursing homes. Such studies should also attempt to address the limitations identified in this paper.
ACKNOWLEDGEMENTS
We thank Dunhill Medical Trust for funding this project and Ecolab for free supply of the alcohol gels; the staff and residents of all the cares homes who took part in this study and John Knightly, Louise Oxford, Camilla Piper, Nergish Desai, David Tucker for their support and help.






