It was the most horrific thing we have ever had to do to our parent. It will haunt us to our death. (Whyte, Lansfield, Dupuis, & Smale, Reference Whyte, Lansfield, Dupuis and Smale2008)
Introduction
Research evidence suggests that between 18 and 33 per cent of North American families of adults aged 85 and over have supported their relative’s move into a long-term care (LTC) home (Banerjee, Reference Banerjee, Armstrong, Boscoes, Clow, Grant, Hawaorth-Brockman, Jackson, Pederson, Seeley. and Springer2009; National Institute on Aging, 2006). With an increasingly aging population, particularly in the 80 and older cohort, and limited government capacity to fund community services for persons with heavy care needs, the prevalence of LTC placement is expected to increase dramatically (Gaugler, Duval, Anderson, & Kane, Reference Gaugler, Duval, Anderson and Kane2007; Tomiak, Berthelot, Guimond, & Mustard, Reference Tomiak, Berthelot, Guimond and Mustard2000). This will result in more families facing the difficult stage in their caring careers where they must support their relative’s move into and adjustment to an LTC home. While there is a growing literature illuminating families’ experiences with the transitional process, much of the literature focuses on the decision to pursue LTC home placement. None compares families’ experiences from different starting points such as home, retirement home,Footnote 1 or hospital.
This article reports the findings from one component of a larger, interpretive grounded-theory study on the LTC transition experiences of new residents, family members, and staff. The focus here is on family members’ experiences. Drawing on data from the larger study, this article (a) explores, from a retrospective viewpoint, family members’ experiences of and challenges faced at different stages or phases of the transitional process; (b) examines the role of where one starts in shaping the transitional experience; and (c) presents policy and practice recommendations aimed at enhancing the transitional process for family members during each transitional stage.
Background
Most family members strive to provide care to their relatives in the community for as long as possible, viewing LTC home placement as a sign of failure and a less desirable option than the more “humane” notion of community care (Peace, Reference Peace, Brechin, Walmesley and Peace1998; Victor Reference Victor, Laczko and Victor1992). This attitude towards LTC home placement is accompanied by the predominantly negative image of nursing homes and homes for the aged held by policy makers, academics, and the public, in which community care is portrayed as inherently good and institutional care as inherently bad (Banerjee, Reference Banerjee, Armstrong, Boscoes, Clow, Grant, Hawaorth-Brockman, Jackson, Pederson, Seeley. and Springer2009; Castel & Engberg, 2007; Gibler, Lumpkin, & Moschis, Reference Gibler, Lumpkin and Moschis1997; Kane, Reference Kane2001; MacDonald, Higgs, MacDonald, Godfrey, & Ward, Reference MacDonald, Higgs, MacDonald, Godfrey and Ward1996; Montgomery, Reference Montgomery1999; Smith, Reference Smith2004). Within this context, it is perhaps not surprising that family members describe nursing home placement as one of the most difficult life events they have ever faced (Kellet, Reference Kellet1999; Lewyeka, Reference Lewyeka1998; Wackerbarth, Reference Wackerbarth1999) and that emotional reactions such as avoidance, guilt, sadness, and regret accompany feelings of relief and peace of mind (Davies, Reference Davies2005; Davies & Nolan, Reference Davies and Nolan2004; Davisson & Mosher-Ashley, Reference Davisson and Mosher-Ashley2002; Lundh, Sandberg, & Nolan, Reference Lundh, Sandberg and Nolan2000; Nolan & Dellasega, Reference Nolan and Dellasega2000; Reuss, Dupuis, & Whitfield, Reference Reuss, Dupuis and Whitfield2005; Ryan & Scullion, Reference Ryan and Scullion2000; Sandberg, Lundh, & Nolan, Reference Sandberg, Lundh and Nolan2001; 2002).
Alongside the taboos attached to LTC home placement, there is also a growing realization that maintaining an older person at home can threaten the health and quality of life of both the older person and the family members in certain circumstances, especially when the older person requires substantial amounts of care (Baldwin, Harris, & Kelly, Reference Baldwin, Harris and Kelly1993; Dupuis, Epp, & Smale, Reference Dupuis, Epp and Smale2004). An extensive body of research evidence, for example, is available that documents the emotional, physical, and social consequences of providing care to a family member in the community (see Dupuis et al., Reference Dupuis, Epp and Smale2004 for a summary). Consequently, many family members will reach a stage in their caring careers when their relative’s needs exceed the family’s abilities to provide quality care in the community and when placement represents a better – sometimes the only – option, for themselves and their relative (Hasson & Arnetz, Reference Hasson and Arnetz2011; Lundh et al., Reference Lundh, Sandberg and Nolan2000; Nolan, Grant, Keady, & Lundh, Reference Nolan, Grant, Keady, Lundh, Nolan, Lundh, Grant and Keady2003; Zarit & Whitlach, 1992). In particular, nursing home placement has been identified as a significant transitional phase in the caring career requiring much further research (Aneshensel, Pearlin, Mullan, Zarit, & Whitlatch, Reference Aneshensel, Pearlin, Mullan, Zarit and Whitlatch1995).
A growing body of literature recognizes that pursuing placement for an older relative is a multiphased process that starts when families begin to contemplate the option of LTC home placement. Much research and theory on transitional care has focused specifically on the decision-making process in which family members decide to pursue LTC home placement and select appropriate facilities (Buhr, Kuchibhatla, & Clipp, Reference Buhr, Kuchibhatla and Clipp2006; Butcher, Holkup, Park, & Maas, Reference Butcher, Holkup, Park and Maas2001; Caron, Ducharme, & Griffith, Reference Caron, Ducharme and Griffith2006; Cheek & Ballantyne, Reference Cheek and Ballantyne2001; Gaugler, Pearlin, Leitsch, & Davey, Reference Gaugler, Pearlin, Leitsch and Davey2001; Mason, Auerbach, & LaPorte, Reference Mason, Auerbach and LaPorte2009; Park, Butcher, & Maas, Reference Park, Butcher and Maas2004). This phase of the transitional process has been found to involve highly charged emotional reactions such as guilt, sadness, uncertainty, and confusion. Researchers have shown that carers’ affective reactions are rarely addressed by professionals, and that systemic pressures to make decisions quickly complicate this phase (Davies & Nolan, Reference Davies and Nolan2004; Ryan & Scullion, Reference Ryan and Scullion2000). The support that carers receive from family members and friends can also be inadequate, which further challenges the decision-making process (Gaugler et al., Reference Gaugler, Pearlin, Leitsch and Davey2001). Some researchers have stated that a carer’s being told, either by professionals or by other family members, that it is time to consider placement helps ease the stress of decision making for carers (Gaugler et al., Reference Gaugler, Pearlin, Leitsch and Davey2001; Kellet, Reference Kellet1999; Ryan, Reference Ryan2002; Ryan & Scullion, Reference Ryan and Scullion2000). Others have suggested that this directive approach could result in family members’ feeling pressured to pursue placement, especially if carers assess the need for placement differently than do professionals and other family members (Caron et al., Reference Caron, Ducharme and Griffith2006; Davies & Nolan, Reference Davies and Nolan2006).
Nolan et al. (Reference Nolan, Walker, Nolan, Williams, Poland and Curran1996) identified four factors that support positive decisions. They suggest that anticipation (rational thought and forward planning), participation (active involvement in the decision), exploration (discussion of alternate options and conflicting emotions), and information (on available facilities) are all factors necessary for carers to perceive decisions as positive choices. Yet, research conducted in a variety of health systems in different Organisation for Economic Cooperation and Development (OECD) countries including Australia, the United Kingdom, Ireland, Sweden, the United States, and Canada has found that these pre-move conditions are rarely met in practice (Caron et al., Reference Caron, Ducharme and Griffith2006; Davies & Nolan, Reference Davies and Nolan2003; Dellasega & Nolan, Reference Dellasega and Nolan1997; Kellet, Reference Kellet1999; Lewyeka, Reference Lewyeka1998; Sandberg et al., Reference Sandberg, Lundh and Nolan2001; 2002).
Anticipating and subsequently supporting a relative’s move into LTC has also been identified as an important phase in the transitional process although significantly less research has focused on these elements of the transitional process. The research that does exist suggests that elevated emotional responses such as worry, frustration, and uncertainty are commonplace during these phases (Strang, Koop, Dupuis-Blanchard, Nordstrom, & Thompson, Reference Strang, Koop, Dupuis-Blanchard, Nordstrom and Thompson2006). These negative emotional reactions appear to be exacerbated by systemic factors such as incongruence between carers’ readiness for placement and bed availability, conflicting information about waiting times, rigid admissions practices and processes, and inappropriate placements such as mismatches with roommates or levels of care (Davies, Reference Davies2005; Nolan & Dellasaga, 2000; Pearson, Nay, & Taylor, Reference Pearson, Nay, Taylor, Nolan, Lundh, Grant and Keady2003; Reuss et al., Reference Reuss, Dupuis and Whitfield2005; Ryan, Reference Ryan2002; Strang et al., Reference Strang, Koop, Dupuis-Blanchard, Nordstrom and Thompson2006).
Conceptual models that identify the conditions that support or impede positive transitions for family members are only beginning to emerge. Reuss et al. (Reference Reuss, Dupuis and Whitfield2005), who analyzed the transitional experiences of 21 family carers in Ontario, Canada, proposed three stage-related conditions and four non-stage-related conditions associated with carers’ experience of relief, empowerment, and acceptance. According to the model, critical time points (stages) that can facilitate or impede the transition are (a) preparation for the move (e.g., appropriate time to make decisions, adequate information provided, all options explored), (b) the nature of the waiting process (e.g., clear and reasonable waiting periods), and (c) the ease of the move itself (e.g., flexible admission practices; welcoming supportive environment). Four conditions found to impact the transitional process are (a) quality of communication (e.g., open and clear communication between staff and families), (b) control over the process (e.g., inclusion in decision making; acknowledging and respecting families’ knowledge bases), (c) support from others (e.g., instrumental and emotional support from family/friends and service providers), and (d) family/residents’ perceptions (e.g., acceptance of placement, perceptions of care).
Researchers (Davies, Reference Davies2005; Davies & Nolan, Reference Davies and Nolan2003; 2004; 2006), who analysed the experiences of 48 family carers in Britain, identified three phases to the transitional process: (a) making the best of it (decision-making phase), (b) making the move (admission), and (c) making it better (post-move adjustment). They also noted five conditions that were relevant to all three stages: (a) being in control (e.g., able to maintain ownership of decisions); (b) being in the know (e.g., having access to all relevant information to play a full and active role in the life and care of the older person); (c) feeling supported (e.g., others are aware of the consequence of the move, are willing to listen and are there for the family); (d) working together (e.g., being able to work with health and social care staff to ensure the best care for the older person); and (e) feeling no pressure (e.g., being encouraged to take time to make decisions).
Both of these transitional-process models note the importance of similar factors – such as support, good communication, and control – and begin to detail how these factors can be maximized at important time points in the transitional process. However, the stages/phases and experiences within them differ slightly, and some conditions are better explicated by stage/phase than others. For example, facilitating open and clear communication between service providers and family members may look different at each stage of the process. Families will feel more or less in the know and part of a team (working together) if they experience particular opportunities to provide or receive information at different stages of the process.
Although our understanding of the conditions that support families’ positive transitional experiences is growing, research is needed that explores each stage/phase of the transition process separately. Furthermore, most existing studies have not distinguished between different types of transitions – for example, from home, from hospital, or from other locations – potentially masking important differences in the transition experience related to starting point.
In this study, we sought to build on the available literature and theories by identifying the interventions, conditions, and systems that contribute to or hinder a positive transitional process for families prior to, during, and immediately following their relative’s transitions into an LTC home, taking into consideration the starting point of the move. We also aimed, in this study, to identify how the presence or absence of supportive factors may impact families’ preliminary adjustment to LTC home placement.
Methods
Recruitment and Sample
Family members were recruited from three privately owned LTC homes in Toronto, Ontario, with 120, 180, and 192 beds respectively. The size and type of ownership represented in these homes is typical of most LTC facilities in Ontario (Berta, Laporte, & Valdmanis, Reference Berta, Laporte and Valdmanis2005). As with all LTC homes in Ontario, the facilities selected are publicly regulated under the Ontario Long-Term Care Homes Act (2007).
In Ontario, as in other provinces in Canada, individuals access LTC through a single entry point system. More specifically, individuals pursuing LTC home placement apply through one of 14 local community care access centres (CCACs) where they undergo a standardized assessment administered by a care coordinator. This system aims to ensure that individuals are appropriately placed within the continuum of care. Individuals considered eligible for LTC home admission are those in need of high levels of daily personal care (typically about 2.5 hours per day), 24-hour nursing care or supervision, and a secure environment (Berta, Laporte, Zarnett, Valdmanis, & Anderson, Reference Berta, Laporte, Zarnett, Valdmanis and Anderson2006). An informational interview conducted with key staff persons responsible for the admission process at each of the three facilities revealed similarities in the admission procedures used at each of the three facilities.
A combination of selective sampling procedures and theoretical sampling strategies were used to determine which family members to interview for the study. Initially, family members invited to participate in the study were selected if they identified themselves as the primary family carer, supported a relative’s admission within a month to six weeks of the commencement of the study, and resided in the same city as their relative. Family members representing different relationship types (e.g., spouses, adult children) were also sought at this stage (Coyne, Reference Coyne1997; Glaser, Reference Glaser1978; Schatzman & Strauss, Reference Schatzman and Strauss1973). Staff members at each facility assisted in the selection process by identifying and initially approaching potential participants. Family members who agreed to learn more about the study were contacted by telephone by a member of the research team who ensured their eligibility and described the study in more detail. If eligible family members confirmed their willingness to share their experiences during the transition process, a date, time, and place for the interview was arranged. The names of those who agreed to participate were not shared with the facilities.
Theoretical sampling was used later in the study process as interviews were analysed. This process helped to “fill out” the themes and explore how alternate circumstances impacted patterns and categories initially emerging from the data (Charmaz, Reference Charmaz2006; Glaser, Reference Glaser1992). For example, in the larger study, researchers began to note possible key differences by starting point when they began examining pre-move processes and experiences for different carers. Consequently, sampling family members supporting moves from different starting points such as home, hospital, or retirement home was initiated to more fully explore these key differences in experience and further develop emerging concepts. Sampling for different starting points continued until no new categories emerged from the data and theoretical redundancy was reached (Luborsky & Rubinstein, Reference Luborsky and Rubinstein1995; Patton, Reference Patton2002).
Twenty family members (17 women and three men) – three sons, three daughters-in-law, 10 daughters, three wives, and one granddaughter – were interviewed before theoretical saturation was reached. Family members participating in this study identified themselves as primary carers (16 study participants) or as sharing the care equally with another family member who did not participate in the study (4 participants). Seven family members co-resided with their relative prior to initiating placement.
Thirteen family members were caring for a relative who had a diagnosis of dementia at the time of admission to the LTC facility. The remaining family members were caring for relatives with progressive medical conditions that had become difficult to manage in the community, such as chronic obstructive pulmonary disease and diabetes. Six family members moved a relative from a retirement residence, eight family members moved a resident from hospital, and six family members moved a resident from home. New residents were age 75 or older and had been in the nursing home from eight days to five weeks, with an average of 20 days (three weeks).
Data Collection Process
In-depth, semi-structured, active interviews were conducted with primary family carers who had recently admitted a relative into one of the three Ontario LTC facilities. Active interviews are conversational in nature, emphasize the collaborative and interactional process between the researcher and participants in the course of meaning-making, and recognize that all knowledge is co-constructed (Holstein & Gubrium, Reference Holstein and Gubrium1995). In keeping with the study’s main objectives, an initial interview guide explored families’ positive and negative experiences during each temporal phase in transitional care – the decision-making period, the waiting period, the move itself, and the post-move adjustment. The initial guide also explored families’ recommendations to support optimal transitions for each temporal phase. As themes began to emerge, we used subsequent interviews to explore these themes in order to capture a deeper understanding of them. Interviews were conducted in family members’ homes, over the telephone, in the LTC home, or in a café, wherever individual family members felt most comfortable. Interviews were between 60–90 minutes in length.
The research was conducted in accordance with the standards of the Tri-Council Policy Statement for Ethical Conduct for Research Involving Humans (CIHR, NSERC, SSHRC, 1998 with 2000, 2002, and 2005 amendments). Procedures were approved by the Health Sciences Research Ethics Board at the University of Waterloo and McGill University. Procedures were also approved by the LTC homes’ ethical boards.
Data Analysis
All interviews were tape recorded, transcribed, and analyzed using a four-staged method of analysis consistent with a grounded-theory approach (Charmaz, Reference Charmaz2006; Glaser & Strauss, Reference Glaser and Strauss1967; Patton, Reference Patton2002). In the first stage of initial coding, each transcript was examined for ideas or observations that were treated independent of one another and noted in the margins of the text. In the second stage, these initial observations were examined, and the researchers attempted to determine their meaning based on other evidence included in the transcript, the literature, and their own knowledge of LTC home placements. At this stage, observations were turned into preliminary, descriptive, and interpretive categories. Preliminary broad categories such as reasons for the move to LTC and reactions to the current move were developed at this second stage of the analytical process. In the third stage, the researchers began focused coding by re-examining preliminary categories to further refine the categories and begin identifying connections and patterns both within and between categories.
Constant comparisons within each case and between different cases (e.g., different starting points, different phases in the transition, different types of carers) were conducted to explore similarities and differences in the transition experiences. At this stage, for example, patterns between descriptions of reasons for the move to an LTC home were noted and understood to be related to starting point (retirement home, hospital, or home), and key differences in the experiences by starting point were noted. The core category acceptance process shaped by starting point was developed. In the fourth and final stage of analysis, emergent themes were interpreted based on the existing literature, particularly the work of Nolan et al., (Reference Nolan, Walker, Nolan, Williams, Poland and Curran1996) who developed a framework for decision making, and of Reuss et al., (Reference Reuss, Dupuis and Whitfield2005) and Davies & Nolan (Reference Davies and Nolan2006; 2004; 2003), who developed frameworks for understanding transitional experiences at different phases for family members. At this final stage, for example, the impact of starting point by transitional phase was further examined with special attention to how starting point impacted pre-move, moving, and post-move experiences and when, if at all, starting point did not play a role in the placement experience.
Findings
Acceptance Process Shaped by Starting Point
The emotional complexity involved in pursuing LTC home placement was profound for all family members in this study. Carers from all starting points summarized their experiences with supporting their relative’s transition to an LTC home as “heartbreaking”, “devastating”, and, “the worst thing [they] ever had to do”. Faced with these intense emotional reactions, supportive processes and practices during pre-move, moving, and post-move phases were of paramount importance to foster carers’ acceptance of placement as a positive option.
Data analysis also revealed that the starting point of a relocation – that is, whether a relocation was initiated from home, retirement home, or hospital – had a profound effect on family members’ experiences with accepting the need for and timing of their relative’s move into LTC (pre-move phase), and on believing that the selected LTC home was a positive environment for their relative (post-move phase). LTC home policies and processes were also important in shaping family members’ experiences during and following the move. However, data analysis showed that these facility-level factors were not as effective in fostering family members’ post-move acceptance when their pre-move acceptance was compromised by conditions attributed to the relocation’s starting point.
Pre-Move Process from Home: Acceptance through Reflection and Escalating Needs
Families supporting relatives’ relocation from home consistently described the reflection and reassurance they required to help them recognize and accept that the time for LTC home placement had arrived. As one daughter stated, “We knew that this was coming so we sort of accepted it but I still wondered, is this the right decision? Should we be doing this? Is this the right time? Should we wait a bit longer?” (daughter, 01). Similarly, a spousal carer described her emotional acceptance of LTC home placement to have emerged following many conversations initiated by family and social service workers wherein she was encouraged to contemplate LTC home placement. She stated: “Intellectually, I knew my family and social worker were right. It’s the emotional thing you have to deal with” (spouse, 02). Given the apprehensions they described, families valued care managers, other professionals, or other family members who took the time to listen to their reflections and uncertainties and who reassured them by confirming their sense that the time had come to initiate LTC home placement. As one daughter- in-law said, “You know what helps? Support from family and just reassurance that you’re doing the right thing” (daughter-in-law, 03).
For many, the initial awareness that LTC home placement may need to be considered came months and sometimes years before this more-intensive period of reflection and contemplation. Families often identified workers or other family members who tried to help them anticipate the eventuality of placement long before they themselves believed relocation would be required. One daughter- in-law described such a conversation with a day program worker: “She said you’re going to have to look for a facility ‘cause there may come a point where you may not be able to look after her anymore” (daughter-in-law, 03). These periods were seen as more informational in nature and were not described as points in time when family members were actively considering relocation as an option.
Families supporting their relatives’ relocation from home appeared most likely to accept relocation when their relative’s needs were so constant that families could no longer meet them with the community support available. These carers described the need to reassure and help their relatives manage their medications, meals, and household tasks multiple times in a day even when community or private services were in place. As one daughter said, “I couldn’t do it anymore. It was just physically too much for one person if you can understand that” (daughter, 04). Another adult daughter said,
Just basically – with her falls, not eating properly (she was diabetic so she wasn’t taking her insulin and she was legally blind so we weren’t even sure if she was reading the numbers right when she was testing her sugar) – and we finally said look, we can’t do this anymore, running over there all of the time. I think it’s [time] we have to look at other alternatives. (daughter, 01)
With escalating care needs, acceptance of placement from home was typically reached when imminent placement was required.
All family members placing a relative from home in this study eventually accessed an LTC home placement under a “crisis status” – a designation within LTC home policy that ensures a bed is offered within 72 hours. For some family members, agreeing to a crisis designation meant that they also had to accept a bed from any of the LTC homes in their health network rather than choose from among several possibilities that they selected. One daughter-in-law described waiting for a bed under this latter circumstance as “some kind of double hell” (daughter-in-law, 05). This was not the case for all carers as some home care agencies had adopted internal policies that guaranteed a bed in one of the LTC homes selected by families, even when placement was under a crisis designation. In practice, all family members in this study who placed their relatives from the community were offered beds in one of their facilities of choice, suggesting that care coordinators worked hard to ensure that facility choice was respected.
In sum, families supporting relatives’ relocation from home most typically described a pre-move process that involved an intensive period of active reflection and contemplation. When families experienced opportunities to process uncertainties and apprehensions, received pro-active information about options such as the initiation of a crisis designation for placement, and had some control over the selection of facilities, they described the pre-move process as positive and supportive and were able to emotionally accept the need for placement. Most families placing relatives from this starting point reported these positive pre-move conditions. While family members could recall conversations months and sometimes years before this period, they appeared to become activated to consider and accept relocation when the care requirements of their relatives became impossible for them to meet. As such, placement was typically accepted as a viable option from home when and only when it was imminently required.
Pre-Move Process from Retirement Residence: Mounting Complaints with Little Time for Reflection Thwarts Acceptance
All families relocating a relative from a retirement residence reported knowing that, when admitting their relatives, relocation to a nursing home might at one time be necessary. Like their counterparts supporting relocations from home, this awareness did not in and of itself position them to recognize when the time had come to consider LTC home placement as a viable option.
All families relocating a relative from a retirement residence spoke of being alerted that their relative’s needs were beginning to exceed the residence’s capacity to provide safe and quality care. Accordingly, it was the facility and not the families who initially recognized and suggested that LTC home placement was required. Most families were first prompted to consider LTC home placement through a series of complaints related to their relative’s functioning in the residence. These complaints placed stress on families and on their relatives and often led families to pressure their relatives to function better so they could remain in the retirement facility. As one adult son said,
We’d be getting complaints of “she’s late for dinner” or “she’s late for this” or she’s … things like that, and that stuff was becoming an irritant at times because all of a sudden we’re trying to tell her, “Mom, you should do this” or “Mom, you should do that” and you know – what are we doing to a poor lady?
He continued, “She was being made to feel that you’re a bad person because [she was] not coming [to dinner] on time” (son, 06).
Eventually, most families supporting a move from this starting point were told directly by residential care staff, most typically by the care directors, that they had to pursue LTC home placement for their relative. Preceding this process, some families were invited to discuss or take part in an assessment to determine if LTC home placement was warranted. This helped them to accept the notion of LTC as a viable option during the pre-move process. As one adult son stated, “We got a lot of help – from the person at the residence and then the person that interviewed her and assessed her; you know, she was very objective, and so we knew this is really something that she needs” (son, 06). However, some families were unilaterally told that it was time to pursue LTC home placement without the opportunity to explore their reactions, contemplate their options, or participate in a formal evaluation of the resident’s care needs. One adult daughter, for example, described receiving a call at work from the director of care informing her that “they couldn’t cope” with her mother anymore “because she needed too much extra care and she’d have to [be] placed in a nursing home”. She continued, “This came sort of out of the blue because nobody had mentioned anything to me about it” (adult daughter, 07). She questioned why the director of care did not call her on her day off when she would have been in her home or the retirement residence and would have felt more equipped to discuss and contemplate the issues.
Families that did not have the opportunity to reflect on and process decisions with staff from the retirement residence described a feeling of abandonment or expressed disappointment in the level of care offered at the residence. As one adult daughter said, “She was on this floor where she was supposed to be getting extra personal care, and it seemed to me that place kept decreasing the care” (daughter, 08). She considered a reduction in care rather than deterioration in her mother’s abilities as the primary reason for pursuing LTC home placement.
In sum, a series of complaints about the resident’s ability to function in the facility often preceded a direct discussion with families about the need for LTC home placement. This was stressful on families and residents, who worked hard to improve the situation and appease the staff at the residence. These complaints were rarely experienced as positive interactions and did not, in and of themselves, activate family members to consider relocation. Most families in this study recalled at least one direct conversation with residential staff during which they were told that LTC home placement was required. If families were given opportunities to discuss and reflect on this option, they felt supported and eventually came to accept the need for LTC home placement. If families were not given this opportunity, they were left to feel disappointed and abandoned by the residence, an outcome that challenged their acceptance of LTC as a desirable option.
Pre-Move Process from Hospital: Acceptance Forced Not Reached
Family members moving a relative from hospital described the process as “horrendous”, “terrible”, and “frustrating”. One adult daughter who questioned whether her father really needed LTC home placement recalled being told countless times: “This is the process, we must do this, you know we can’t hold up an acute care bed, we can’t hold up an acute care bed” (adult daughter, 09). The notion that taking time to reflect and explore options would block a hospital’s care system was prevalent in all family member accounts from this starting point, thereby limiting opportunities for reflection, contemplation, and emotional acceptance.
Families also described being pressured to make immediate decisions regarding facility choices. As one adult daughter stated, “The social worker kept pressuring me every day that I was there: ‘you have to choose one, you have to choose one because you know we could send him home, we need the beds.’” Threats of being sent home or being charged thousands of dollars to remain in hospital were commonplace when families were perceived to be taking too long to select facilities. In addition to the time pressures, families repeatedly indicated that they were not provided with direction on what to look for or ask when visiting facilities. One adult daughter, describing the information she received from the hospital when selecting facilities, said, “They just give you a list of homes and basically throw you to the wolves” (daughter, 11).
Adding to the pressure of hospital placements were the limited facility choices family members actually had from this starting point. All families placing relatives from hospital in this study were told that they had to select one facility with an idle bed among their choice of facilities. This meant one of the facilities they had to choose was one that had a bed available immediately, something that changed on a daily basis. Consequently, some relatives would visit facilities with idle beds and select them the next day, only to be informed the facility was “no longer on the idle list” (daughter, 10). Others described visiting low-quality facilities that were “atrocious” (daughter, 11) and “felt like warehouses” (daughter, 12), suggesting that the homes had available beds because people didn’t want to be in them. This complicated the task of facility selection because families came to realize that selection was more of an illusion than a reality. As one daughter observed,
Really, the hospital says, “We’ll tell you what, you have to make an application, but you sign it and we pretend that that’s your choice.” I would have been happier if the hospital just said “Because we can’t keep you in an acute care bed we’re gonna transfer you here,” then [there would be none of] this sort of pretence that this “let’s pretend that the family has a choice, let’s pretend that the patient has a choice” – there really is no choice. (daughter, 09)
Overall, families placing relatives from hospital were pressured rather than supported and had little control or input over all aspects of the pre-move process. Families were expected to make quick decisions with inadequate information and had no time or opportunity to process their emotional reactions so that they could accept placement as a viable option for their relative.
The Moving Process: Facility Factors Paramount in Balancing Administrative Demands and Emotional Care
Families from all starting points were expected to accept a bed offer within 24 hours and move their family member into the LTC facility a day or two later. This quick turnaround was described as unreasonable for some who wished they had a few more days to organize moving trucks, work schedules, and additional supports for the move. Some families stated that this quick time frame did not allow them the necessary time to sit and process the move with their relative or to facilitate a pre-placement visit. As a result, few residents had the opportunity to see their rooms or the facilities they were moving to prior to the actual day of the move. Families who were given long projected wait times (e.g., three years) were especially frustrated when they were offered a space within months and only given a day to accept a bed and then move. As one adult daughter said, “It was just the, the suddenness you know, them telling you that you had three or four years’ wait before you could get in the place you wanted, and then coming and telling you [one month later] that you have to move in 24 hours” (daughter, 08). This was most typical of relocations from retirement homes since the families in this study that were moving relatives from home and from hospital were aware that their moves would be relatively immediate.
When families were given some flexibility around the time of admission, or the option to “reserve” a space by paying for a bed to delay a move for a few days, it was appreciated. This appeared to be particularly important to family members supporting relatives’ relocation from home as these moves involved making important decisions about what to bring and what to leave behind, organizing moving vans, and finding strategic ways to inform their family members that they had to leave their home and move into an LTC home. It was also important for family members supporting retirement home relocations who were given ample time to select facilities and were expecting longer wait times.
All family members noted that the day of the move was a long process that required the combination of administrative responsibilities (completing financial and medical paperwork) and emotional work (reassuring the resident). Those who had the support of other family members on the day of the move noted that this facilitated the experience for themselves and especially for their relative as someone could be with their relative during the whole moving process. Those who were unaware of the administrative requirements expected of them (including reviewing documents and signing contracts) felt pulled between the expectations of the facilities and their family members’ needs for support and reassurance. As one adult daughter said,
You find all that out the day that you go there and Mom was wondering where I was – “well, Mom I had to go upstairs and do this.” So if I knew all that I could fill it all out if I had that package ahead of time and I could spend more time with her because, your first day is so – critical, right – and so emotional. (daughter, 04)
Surprisingly, although families supporting transitions from home or retirement home felt generally well-informed during the pre-move phase, these same individuals did not always have the admission information they required on moving day. In fact, the most common reason cited for receiving pro-active information about moving-day policies and practices was having prior contact with someone at the LTC home who was familiar with admission practices of a particular home. Unfortunately, this information was rarely available to families.
Families who were greeted at the LTC home immediately felt welcomed and described the admission as supportive and compassionate, whereas those who had to find their own way to the resident’s room and wait for a staff person to initiate the admission felt lost and unsupported. As one woman who placed her mother described it:
My daughter and I are sitting around for about maybe 45 minutes to an hour before anybody even came in. I said, “Well, what should I do next?” Nobody came in to say, “OK, this is what you need to do or this is what we have to do.” …. I think if they had someone spend a bit of time with you that very first hour you are in there, even just to listen to your concerns and your fears and your emotions – just to be there. I felt like we were just, “here, you’re going here” and … I was just overwhelmed. (daughter, 01)
The factors that supported a positive moving experience included prior information on the process of the admission and the items required, flexibility with the timing of the move, and immediate support and direction on arrival. The presence of other family members was also described as helpful as it allowed carers to balance the administrative demands of the admission with the emotional needs of the resident. When these conditions were met, families described having confidence in the facility and feeling comfortable when leaving their relative for the night. Families who anticipated longer wait times were particularly challenged when they were not provided with flexibility on admission dates and times, which our study found was typical of retirement home placements.
Post-Move Adjustment: Facility Factors and Resident Reactions Make a Difference
The caring, respectful nature of staff was noted as being important to all family members in this study. When staff knocked on a door before entering a room, greeted family members by name, spoke in a friendly, reassuring, calming tone to residents, and pro-actively volunteered specific information about their relatives, families felt that the staff members were connecting with their relative as a person, which provided comfort to them. Families that had to push for information, such as results from medical tests, questioned the extent to which staff members cared about their relative’s well-being.
Communicating with staff in the first few weeks about residents’ unique characteristics was also important to families. As one adult daughter said,
I think there are things that families understand, particularly if you have a patient with dementia, [that] inviting this information from families within the first few weeks is important because otherwise you can get off to the wrong start if you don’t have that conversation. (daughter, 12)
Another carer who felt that the communication was good particularly appreciated that the staff constantly asked her for information about her mother. The importance of this level of communication, particularly within the first few days of placement, was that it seemed to reassure families that they were considered partners in the care process. As one adult daughter stated, “It helps that everybody’s so friendly and good and [that] they’re not trying to replace you, but they’re trying to do all the heavy care that you can’t do yourself anymore” (daughter, 08).
Families’ adjustment processes were intimately tied to those of their relatives. As one spousal carer commented, “I guess I’ll get used to it when he gets used to it” (spouse, 13). In some cases, families noted improvements in their relative’s quality of life which they suggested was instrumental in facilitating their own adjustment. One daughter-in-law noted that her mother-in-law was “more at ease” (daughter-in-law, 05); another spouse commented that her husband was now able to mobilize and use the washroom when he had previously been dependent on incontinence products; a daughter noted that her mother “looks brighter and more enthusiastic” (daughter, 08); a son and his wife said their mother (-in-law) “is always happy and doing something” when they visit (son, 14); and a spouse felt that “something good is happening to [her husband] because he’s not as confused” (spouse, 02). These improvements served to reinforce their view that the placement decision had led to an improvement in their relative’s quality of life, something contrary to most views of LTC home placement.
The Impact of Pre-Move Processes and Starting Points on Post-Move Adjustment
Family members who had positive pre-move experiences largely determined by where they moved from also appeared to cope better when faced with post-move challenges such as imperfect communication, the occasional unfriendly staff member, or residents who were not readily adjusting. For these carers, a few negative post-move experiences did not affect the validity of their decision to pursue LTC home placement nor their confidence that things would improve. For example, one adult daughter, who placed her mother from home with a lot of support and pre-move reflection, observed that her mother had been questioning the need for placement and was asking to go home. Despite this reaction, the daughter stated with confidence, “I do think my mom will settle nicely into LTC and she can have some quality of life” (daughter, 15). Another adult son who described his pre-move process from a retirement residence as positive – because he was given the opportunity to reflect on his options and participate in an assessment of his mother’s care needs – acknowledged that his mother was not completely happy but said, “I expected a period of adjustment where she would get used to her surroundings … but I think she’ll be OK, it’ll take time to adjust” (son, 06). Seemingly in both cases, positive pre-move processes helped these carers’ adjustment to LTC home placement despite their relative’s apprehensions and difficulties.
Conversely, negative pre-move experiences often complicated the adjustment process, making it more difficult for family members to adapt. One daughter, for example, whose father was placed from hospital, where she felt pressured rather than supported, appeared unsure if she or her father would ever adjust. She stated: “I know I did the right thing deep down, now how do I deal with it without having a breakdown?” Later on in the interview, she reiterated her concern for her own adjustment by asking, “How do I go on from here?” (daughter, 10). A spousal carer who had a difficult pre-move process from hospital stated that “Any time you hear or see something negative it really bothers you; you wonder, well, should he be there or should I try to take him home and, you know, follow another course or something?” This spouse recounted the numerous times, following an incident her husband had with another resident, or her husband’s expressed desire to go home, that she had told staff “I wanna take him home, I don’t want him to stay here” (spouse, 16). In both cases, these family members were not provided with opportunities to reflect on and contemplate placement as a viable option and therefore did not reach a level of acceptance at the pre-move stage. Still struggling to accept the placement decision, negative experiences post-placement quickly caused family members to wonder if they had done the right thing by supporting their relative’s relocation, which continued to make acceptance of the move difficult.
In sum, carers who had the opportunities and support needed during the pre-move phase to emotionally accept LTC home placement as a viable and necessary option appeared better able to manage post-move complications. This was most typical when placing relatives from home where family members described active periods of contemplation and reflection supported by family, friends, and/or professionals. It was also facilitated in retirement home placements when facility-led discussions invited families to reflect on and process the need for LTC home placement. Carers placing relatives from hospital were most challenged in this regard as none were offered opportunities that helped them emotionally process and accept this option at the pre-move stage.
Study Limitations
The interviews informing this study were retrospective in nature, taking place shortly after a relative’s transition into LTC. Future prospective work with a longer post-adjustment period may serve to further illuminate how pre-move processes from different starting points impact carer adjustment over time.
Family members go through a range of health care transitions throughout their caregiving careers, including the transition from home to acute care, from acute care to rehabilitation, from LTC to hospital, and occasionally the transition from LTC to home. Future research is needed to examine similarities with other transitional processes and their impact on carer adjustment (Cameron & Gignac, Reference Cameron and Gignac2008; Coleman & Berenson, Reference Coleman and Berenson2004).
Discussion
Conditions that Support Acceptance and Adjustment to a Long-Term Care Home Placement for Family Members
The study findings reveal important connections between the factors previously identified in the literature to support positive transitions and the location from which transitions occurred. In their model of transitional care processes, for example, Ruess and colleagues (2005) noted that preparation for a move to an LTC home is an important and distinct component of the transition process and a necessary condition for positive transition experiences. They observed that the conditions which maximize preparation include these: (a) appropriate time to make decisions, (b) adequate information upon which to make decisions, and (c) adequate exploration of options and emotions. Findings from our study revealed that pre-move processes unraveled differently for families supporting a relative’s transition from hospital, retirement home, or home. These differences had an impact on family members’ experiences accepting the need for and timing of their relative’s move into LTC (pre-move phase), and on believing that the selected LTC home was a positive environment for their relative (post-move phase). These differences are noteworthy because they point to considerations that could guide policy and practice for each type of transition.
Figure 1 integrates factors that emerged in this study with those identified in other transition models to build a more comprehensive model on the conditions that support acceptance and adjustment to an LTC home placement for family members. The model provides guidance for future policy and practice decisions.
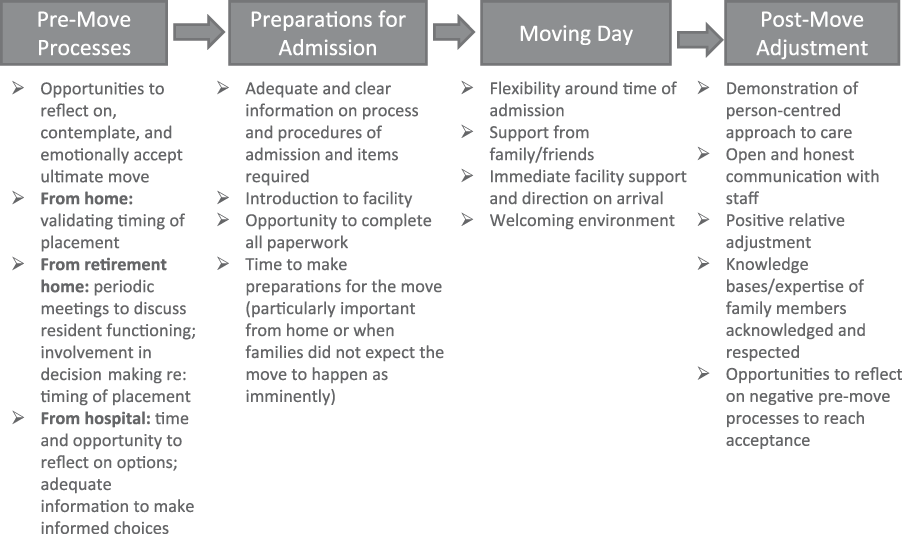
Figure 1: Conditions that support acceptance and adjustment to a long-term care home placement for family members
Pre-Move Processes from Home
Overall, families supporting a relative’s move from home to an LTC home described a supportive pre-move process. Families in these situations were provided with opportunities to discuss their conflicting emotions regarding placement, receive validation that placement was indeed warranted, discuss selection criteria for appropriate homes, and work together with care managers to determine if immediate placement was warranted. Families in these circumstances felt more confident in their decisions and appeared to reach a level of emotional acceptance that placement was a necessary and viable option.
Our study found that family members supporting relocations from home described a process of abstractly thinking about LTC well before they took the steps towards placement planning (e.g., completing an application; exploring different homes) (Caron et al., Reference Caron, Ducharme and Griffith2006; Nolan & Dellasega, Reference Nolan and Dellasega2000; Strang et al., Reference Strang, Koop, Dupuis-Blanchard, Nordstrom and Thompson2006). In many of these cases, family members could recall family, friends, or professionals prompting them to anticipate and think about the eventuality of placement well before they began truly contemplating placement. These conversations were described as informative but did not, in and of themselves, prompt family members to actively plan for placement.
Within the context of rapidly growing care demands, family members were able to reflect on and contemplate the notion of placement as an option. This meant that carers supporting transitions from home most typically accepted the need for placement when placement was required. Unfortunately, current policies and practices cannot accommodate the immediate need for placement from home unless a crisis designation is initiated. The punitive repercussions of this actuality include the expectation that families accept any bed offered to them despite their preferences.
The first-available-bed provision is prevalent in many Canadian provinces (see, for example, British Columbia Ministry of Health, 2011; Nova Scotia Department of Health and Wellness, 2011). Although facility choice was respected by service providers supporting families in this study, it was seemingly service provider compassion and not standard policy that ensured that outcome. It is timely for policies and practice to more closely align with the natural trajectory of care. Rather than expecting family members to rationally anticipate and plan for placement well in advance of need, policies and processes should recognize the emotional complexities involved in accepting placement and instead expect that carers pursuing LTC from the home environment can only reach these decisions when they are faced with demands they can no longer meet.
Pre-Move Process from Retirement Home
Family members who supported a relative’s move from a retirement home described the decision as facility driven and based largely on mounting complaints from the retirement home. Like their counterparts in supporting transitions from a relative’s own home, all knew when admitting their relatives that nursing home placement might at one time be required. This generalized awareness and knowledge, however, did not help them to recognize and identify that the time for nursing home relocation had arrived. Further, the mounting complaints – intended to raise their awareness and acceptance that placement was warranted – functioned to place stress on families and their relatives and rarely if ever helped them to recognize and prepare for the understanding that LTC home placement may be indicated. Periodic, scheduled meetings with family members to discuss their relative’s functioning within the retirement residence may serve to help families from this starting point anticipate the possibility of LTC home placement and help prepare them for an eventual placement; it may also be experienced as more supportive than the ad hoc phone calls many families described receiving.
In some cases, families in our study had been invited to one meeting at the retirement residence to discuss placement, and to contemplate and explore whether other options existed (i.e., hiring additional help). These family members seemed more readily able to adapt to the decision and consider LTC home placement as a positive choice for their relative. Families who were told directly that LTC home placement was necessary without the opportunity to discuss and contemplate this decision described feelings of helplessness, rejection, and distress during this pre-move phase which complicated other stages of the transitional process.
Facilities for older adults exist in the context of a continuum of care aimed at providing “the right services, in the right place at the right time” (Alexander, Reference Alexander, Stephenson and Sawyer2002). At present, provinces across Canada appear to be reallocating funds away from LTC facilities and instead to promote aging-at-home strategies that support other forms of assisted living in the community such as retirement homes (Banerjee, Reference Banerjee, Armstrong, Boscoes, Clow, Grant, Hawaorth-Brockman, Jackson, Pederson, Seeley. and Springer2009). Furthermore, policy directives grounded on a community care ethos which considers LTC homes to be the least desirable option (Davies & Nolan, Reference Davies and Nolan2003; Peace, Reference Peace, Brechin, Walmesley and Peace1998) continue to push the level of care required for LTC home admission up to a higher level which suggests that those who may have once been admitted to LTC homes are forced to consider other options such as retirement homes. This trend is likely to result in more transitions from retirement home to LTC home in the future. Yet, staff in retirement homes seemed less prepared to support families in preparation for making the transition to an LTC home, suggesting an urgent need for building capacity in this area in both retirement and assisted living facilities (Ball et al., Reference Ball, Perkins, Whittington, Connell, Hollingsworth and King2004; Cheek, Ballantyne, Byers, & Quan, Reference Cheek, Ballantyne, Byers and Quan2006; Mead, Eckert, Zimmerman, & Schumacher, Reference Mead, Eckert, Zimmerman and Schumacher2005).
Pre-Move Processes from Hospital
Families moving their relatives from hospital to an LTC home described all aspects of the pre-moving experience as horrendous. From this starting point, families were operating under intense pressure, with little support and information to guide them. Further, while they were asked to make life-changing decisions, the lack of control and opportunities for reflection they actually had from this starting point was apparent in all interviews. There was no time to help families and residents process and accept placement as a viable option, little information provided to help family members make informed decisions, and no opportunities for family members and their relatives to choose between meaningful options because options did not exist.
North American statistics suggest that almost half of all admissions to LTC homes are done from hospital settings (Jones, Reference Jones2002), and yet hospitals appear to be the least prepared of any starting points to support a positive transition to an LTC home. In fact, findings from the current study reveal that the pre-move experiences from hospitals are consistently negative and should form the focus of future research to inform policy change. This research should include an analysis of the barriers to providing ideal pre-move conditions and possible solutions to address those barriers from the perspectives of family members, service providers, and health administrators.
Moving Processes: Preparations for Admission and Moving Day
Families’ experiences with the moving process itself were most influenced by systemic and facility-related factors. Whether a family’s relative moved from home, hospital, or retirement home, the time between receiving a bed offer and the expectation of accepting a bed was minimal. When families were provided with some flexibility regarding the date and time of the move, no matter from where they started, they had more control over the moving process itself. This time often allowed them the opportunity to visit the facility once more, move furniture in, and rally additional familial support for the day of the move. In our study, families supporting relocations from retirement homes were particularly distressed when they were informed they would need to move immediately, following a shorter than expected wait time. Our findings on the conditions facilitating the moving process support those of other researchers (Davies & Nolan, Reference Davies and Nolan2004; Reuss et al., Reference Reuss, Dupuis and Whitfield2005).
Currently, LTC home funding policies discourage flexibility because funding depends on bed occupancy; consequently, facilities pressure families to move in quickly so that they can maintain their occupancy levels (Ministry of Health and Long-Term Care, 2010). The implications of this funding policy on family members’ experiences should not be minimized. Not only does this policy mean that families must organize the move with limited time, but that they also have less opportunity to organize support for themselves on the day of the move. Yet in our study, we found that families who enjoyed the presence of other family members on the day of the move felt they were better able to balance the administrative demands of the admission process with the emotional needs of their older relative and generally described a better admission process. In addition to providing families with pragmatic information such as typical length of admission (described by families as approximately 6 hours) and the documentation required prior to the move, facilities that prepare families for admission day should instruct families to consider rallying additional support to help them balance the administrative and emotional demands of the move day. No families in our study reported receiving that type of direction.
These findings add specificity to Ruess et al.’s (2005) model. While their model emphasized the importance of support from family and friends at all stages of the process, our study findings reveal that the presence of additional family members on the move day was particularly beneficial to family members who felt better able to balance administrative demands with residents’ needs. Family members who lack this level of other family or friend support may benefit from volunteers within the facility or staff specifically assigned to provide this type of support and assistance on the actual move day. Alternately, facilities could provide families with opportunities to complete paperwork prior to the admission day, thereby allowing them to focus on their relative’s emotional needs on the day of the move.
The importance of being immediately greeted and expected on the move day was emphasized by all family members in this and other studies (Davies & Nolan, Reference Davies and Nolan2004; Reuss et al., Reference Reuss, Dupuis and Whitfield2005). Administrators should note that additional staffing on the day of an admission is optimal to ensure that resources are available to provide the intensive support required to make older adults and their relatives feel welcomed and reassured.
One quality indicator typically used to assess quality care in a nursing home is staff/resident ratio. This ratio is calculated by summing the total number of hours each staff worked in a given year with the total number of residents occupying the home in a given year and dividing by 365 days (Berta et al., Reference Berta, Laporte, Zarnett, Valdmanis and Anderson2006). Another possible indicator of a home’s quality level is the number of staffing hours for admissions given that studies have repeatedly shown the value that families place on this additional support. From a practice perspective, staff must recognize the importance of immediate support. For many families, this level of attention alleviated considerable initial stress and anxiety and acted as a reassurance that the facility’s quality of care was acceptable, thereby easing their older relative’s adjustment to the new environment.
Post-Move Adjustment
Factors found to help family members adjust following the move included residents’ positive reaction to the move (e.g., noted improvement in mood or functioning) and a perception that residents were receiving good quality of care as evidenced by friendly, respectful staff who volunteered and sought information related to the residents’ daily care such as interventions received, results attained, and reactions and activities noted. The impact of the residents’ reaction to the move on carer adjustment has been noted elsewhere (Davies & Nolan, Reference Davies and Nolan2006; Dellasega & Nolan, Reference Dellasega and Nolan1997; Reuss et al., Reference Reuss, Dupuis and Whitfield2005).
The significance of open communication between staff and families immediately following an LTC admission should not be minimized. Efforts made by staff to update families on their relatives’ daily routines and to solicit information from family members communicated to families that staff were looking to work with, rather than for, them and were reassured that the staff practiced person-centered care.
Most notably, the findings illuminated the connection between pre-move experiences and post-move adjustment. Families that were not given the opportunity to emotionally accept placement in the pre-move phase were more susceptible to experiencing adjustment issues post-move. They had less confidence in the ability of LTC homes to meet their relatives’ needs, anticipated more problems, and continually questioned the placement decision. This was most typical of families relocating their relatives from hospital. In fact, most family members placing relatives from home or from a retirement home were able to reassure themselves that, with time, they and/or their relative would adjust when particular conditions were met. This finding emphasizes the potential ongoing impact of the pre-move process and experiences on family members’ adjustment to LTC home placement as well as the need to ensure that the pre-move experience is positive and supportive.



