Background
The Canadian Institute for Health Information (2017) projected that the older seniors’ population in Canada (those 75 years of age and older) will almost double in size within the next 20 years, from 2,600,000 to 5,700,000 people (6.2–10.4% of the overall Canadian population). In British Columbia, the older seniors’ population is expected to reach almost 850,000 by 2037 (Statistics Canada, 2020). Stonebridge and Hermus (Reference Stonebridge and Hermus2017) indicate that as the Canadian seniors’ population grows, health care services and supports will be strained. The incidence of frailty increases as people age, and frailty is associated with impaired functionality, which frequently requires ample resources to adequately address people’s complex health needs (see also Compton et al., Reference Compton, Owilli, Caine, Berendonk, Jouan-Tapp and Sommerfeldt2019).
Most seniors in Canada live at home and consistently indicate that they prefer to stay there for as long as possible (Compton et al., Reference Compton, Owilli, Caine, Berendonk, Jouan-Tapp and Sommerfeldt2019; Health Council of Canada, 2012; Mustel Group Market Research & Sotheby’s International Realty Canada, 2020). Aging in place generally requires a high level of in-home health services and the support of informal caregivers, usually family caregivers, to manage seniors’ daily activities and attend to their health care needs (Health Council of Canada, 2012). Previous research suggests that there is a significant gap in adequate and effective support for family caregivers who wish to help their loved ones die at home (Reinhard, Given, Petlick, & Bemis, Reference Reinhard, Given, Petlick, Bemis and Hughes2008; Robinson, Bottorff, McFee, Bissell, & Fyles, Reference Robinson, Bottorff, McFee, Bissell and Fyles2017). In the Canadian context, maintaining care supports is a critical step in efforts to meet the needs of seniors who choose to remain at home instead of living in long-term care (Hermus, Stonebridge, & Edenhoffer, Reference Hermus, Stonebridge and Edenhoffer2015). The BC Care Providers Association forecasts a high demand for new long-term care beds as a result of expected demographic shifts in our province. A portion of this demand could potentially be mitigated by ensuring that appropriate supports are in place in other areas of the continuing care sector, and by introducing and promoting new models of or approaches to care (Kary, Reference Kary2019).
Hospice palliative care (HPC) aims to relieve suffering and improve the quality of living and dying (Canadian Institute for Health Information, 2018). HPC services generally encompass medical (e.g., pain and symptom management), personal care (e.g., bathing, grooming, and dressing), and psychosocial services (e.g., psychological support, spiritual care) (Canadian Hospice Palliative Care Association, 2013). Psychosocial services in the palliative care context attend to one’s emotions, thoughts, attitudes, and behaviors, as well as the way in which a person relates to and interacts with their environment (palliAGED, 2021; World Health Organization, 2016). In HCP organizations, counsellors, social workers, and spiritual health professionals typically provide specialized psychosocial care to people experiencing life-limiting illnesses and to their families, including bereavement services. This structure is not universal, however, as different hospices provide various types of psychosocial services to their respective populations (Hospice Toronto, 2020; Hospice Yukon, 2021; Prince George Hospice Palliative Care Society, 2021).
A group of HPC professionals from British Columbia set out to assess the current state of HPC provided by hospices in British Columbia and to identify, with key stakeholders, how hospices can better support the challenges that the province will face considering the ongoing demographic shifts. The Provincial Hospice Working Group (PHWG) was established in 2019 with membership from the BC Centre for Palliative Care, BC Hospice and Palliative Care Association, the Sovereign Order of St. John, the Vancouver Island Federation of Hospices, and Victoria Hospice Society. The group’s strategy included a literature review, a survey of hospice organizations in British Columbia, a roundtable discussion with provincial HPC experts and stakeholders, and the development of a report with key findings and recommendations. This article reports findings of the literature review portion of said work.
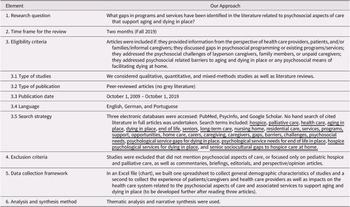
This literature review was undertaken in preparation for the PHWG roundtable discussion. The PHWG guided the development of our research question; the conclusions are, however, entirely those of the authors of this review. The authors had no access to the PHWG survey or its results prior to completing the review. The authors conducted this rapid review (RR) during their employment with Victoria Hospice Society, and no additional funding was sought or received for this study. The RR method is appealing in its ability to produce systematic results in a short amount of time (Tricco et al., Reference Tricco, Antony, Zarin, Strifler, Ghassemi and Ivory2015). RR is a type of systematic literature review in which some components of the systematic review method are simplified or omitted to produce a synthesis of available evidence, usually to support decision making in a short period of time without compromising the quality of findings (Haby et al., Reference Haby, Chapman, Clark, Barreto, Reveiz and Lavis2016). Although HPC services encompass medical, personal care, and psychosocial care services (Canadian Hospice Palliative Care Association, 2013), the PHWG was primarily interested in exploring the gaps in psychosocial care services and programs. Our review was guided by the question: Which psychosocial aspects of aging and dying in place identified in the literature point to gaps in programs and services?
This report follows the Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) Checklist (Tricco et al., Reference Tricco, Lillie, Zarin, O’Brien, Colquhoun and Levac2018) slightly modified for this rapid review (Appendix 1 – online only).
Methods
Protocol and Study Selection
Our approach followed the working definition of RR and recommendations outlined by Tricco et al. (Reference Tricco, Antony, Zarin, Strifler, Ghassemi and Ivory2015). The streamlined methods used in the current review included: limiting the literature search to peer-reviewed articles on three databases (PubMed, PsycInfo, and Google Scholar; no hand search, no contact with authors), limiting inclusion criteria by date and language, having one person screen articles and another verify screening, and presenting results in a narrative summary. We have focused on articles in English, German, and Portuguese according to the language proficiencies of the research team. Only studies that addressed psychosocial programming, psychosocial challenges, or psychosocial means of facilitating aging and dying in place were included. Studies not addressing seniors were excluded. We created a protocol to guide the RR, which is summarized in Table 1.
Table 1. Rapid review protocol summary

The initial protocol outlined was adjusted after work had begun. We decided to include “bereavement” and “grief” as terms in the search criteria, to exclude “screened studies for which we were unable to obtain full text” as well as “literature reviews without a thorough description of their review methods”. We also expanded the time frame of the search to “October 1, 2009 until May 1, 2020” to present updated information in this manuscript. Each category in the data collection framework for experiences/impact was further divided into “challenges” and “opportunities”.
Our study selection is summarized in Figure 1. The PsycInfo database search yielded a large number of items (59,795). After screening the first pages, we realized that there was an abundance of non-relevant entries. We then proceeded to filter results using each search terms as the first step in screening the results. This measure yielded a more manageable number of entries (2,111), which were then screened using established inclusion criteria. Screening and exclusion of abstracts was conducted by one reviewer and then verified by a second, who checked a random selection of excluded items. All full texts were read by two reviewers independently. Disagreements about exclusion of full texts were discussed until consensus was reached, and reasons for exclusion were recorded.

Figure 1. Flow chart of the literature search and selection process for inclusion in the review.
Data Abstraction
Data abstraction began using three articles (Grande et al., Reference Grande, Stajduhar, Aoun, Toye, Funk and Addington-Hall2009; Jack, Mitchell, Cope, & O’Brien, Reference Jack, Mitchell, Cope and O’Brien2016; Phongtankuel et al., Reference Phongtankuel, Scherban, Reid, Finley, Martin and Dennis2016) from our initial sample, and these guided the organization of data into a chart format. Each team member independently conducted a thematic analysis of the articles using a combined inductive (data-driven) and semantic (following explicit meaning of the data) approach (Braun & Clarke, Reference Braun and Clarke2006). Each member generated major themes guided by our research question. The content of one of the articles (Grande et al., Reference Grande, Stajduhar, Aoun, Toye, Funk and Addington-Hall2009) helped guide the development of the data collection chart, but was subsequently excluded from the review because the article’s review method was not thoroughly described.
Once independent work was complete, we reconvened as a group to share our findings and discuss the identified themes in search of consensus. The final chart used for data abstraction included one page of demographic data: full citation, geographic location, expertise of the researchers, data collection method, study design, aim of the project, sample description, and setting of care. A second page of the chart focused on the psychosocial aspects of care and related services to support aging and dying in place, including the experiences of patients and caregivers, the experiences of health care providers, and impacts on health care systems. The term “caregiver” encompassed any unpaid caregiver, family-related or not. Within each category, we collected “challenges” and/or “opportunities”. Two team members read each article written in English and conducted data abstraction independently. Data abstracted was discussed when disagreements existed, until consensus was reached. The German-language articles were read by one reviewer, and data abstraction was conducted by the same person. Regrettably, no manuscripts written in Portuguese matched our inclusion criteria.
Quality Appraisal
All included literature was subject to quality assessment by two team members independently using validated tools, depending on the type of article: Mixed Method Appraisal Tool (MMAT) (Hong et al., Reference Hong, Pluye, Fábregues, Bartlett, Boardman and Cargo2018), Assessing the Methodological Quality of Systematic Reviews (AMSTAR 2) (Shea et al., Reference Shea, Reeves, Wells, Thuku, Hamel and Moran2017), or Health Evidence Quality Assessment Tool – Review Articles (Health Evidence, 2018). Quality assessments were discussed when disagreements existed, until a consensus was reached. No articles were eliminated during the quality appraisal phase.
Data Synthesis
Data were analyzed through thematic analysis. We followed the framework proposed by Braun and Clarke (Reference Braun and Clarke2006), using a data-driven approach to analysis because of the descriptive nature of this study. We also chose to provide a thematic description of our entire data set, rather than a detailed account of one aspect of the data. After reading and re-reading the abstracted data, each team member generated codes independently. Based on the number of times and ways in which themes were raised in the literature, associated codes were determined and ranked by their importance to our research question. We then gathered as a team to share findings, discuss the identified codes, and refine themes for consensus.
Results
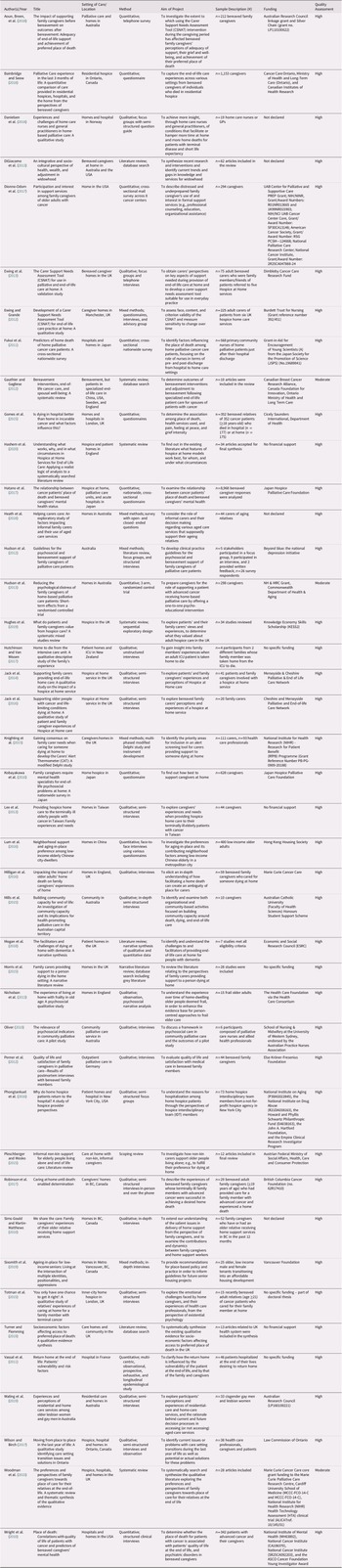
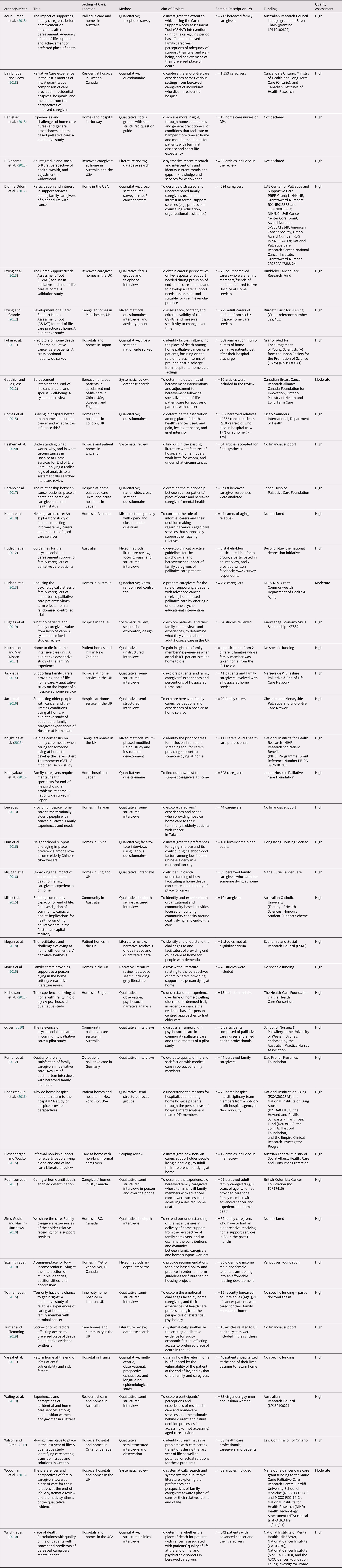
Included articles reported findings from a range of research study designs: qualitative (17 articles), quantitative (11 articles), mixed methods (5 articles), and literature reviews (9 articles). Roughly half of the articles were authored by researchers from the United Kingdom, only four were authored by researchers from Canada. The majority of articles (22 out of 42) included data obtained through interviews and/or focus groups. Five studies included patient primary data; 21 included caregiver primary data; and 3 included both. Table 2 summarizes the characteristics of the included articles.
Table 2. Characteristics of included articles
Thematic Analysis
Guided by our research question, we were able to identify specific challenges related to psychosocial aspects of care that pointed to gaps in services/programs. In addition, we were able to tease out potential opportunities from the widespread challenges that patients, caregivers, and health care providers faced. As we embarked on our analysis of the literature, we realized that many of the included articles not only focused on services directly related to psychosocial aspects of care, but also included medical and or practical factors important to support aging and dying in place with an impact on psychosocial health (Aoun, Ewing, Grande, Toye, & Bear, Reference Aoun, Ewing, Grande, Toye and Bear2018; Danielsen, Sand, Rosland, & Førland, Reference Danielsen, Sand, Rosland and Førland2018; Ewing, Brundle, Payne, & Grande, Reference Ewing, Brundle, Payne and Grande2013; Ewing & Grande, Reference Ewing and Grande2012; Fukui, Fujita, Tsujimura, Sumikawa, & Hayashi, Reference Fukui, Fujita, Tsujimura, Sumikawa and Hayashi2011; Gomes, Calanzani, Koffman, & Higginson, Reference Gomes, Calanzani, Koffman and Higginson2015; Hashem, Brigden, Wilson, & Butler, Reference Hashem, Brigden, Wilson and Butler2020; Hutchinson & Van Wissen, Reference Hutchinson and Van Wissen2017; Knighting et al., Reference Knighting, O’Brien, Roe, Gandy, Lloyd‐Williams and Nolan2015; Lee et al., Reference Lee, Melia, Yao, Lin, Chiu and Hu2013; Mills, Rosenberg, & McInerney, Reference Mills, Rosenberg and McInerney2015; Mogan, Lloyd-Williams, Harrison Dening, & Dowrick, Reference Mogan, Lloyd-Williams, Harrison Dening and Dowrick2018; Morris, King, Turner, & Payne, Reference Morris, King, Turner and Payne2015; Oliver, Reference Oliver2010; Phongtankuel et al., Reference Phongtankuel, Scherban, Reid, Finley, Martin and Dennis2016; Robinson et al., Reference Robinson, Bottorff, McFee, Bissell and Fyles2017; Sims-Gould & Martin-Matthews, Reference Sims-Gould and Martin-Matthews2010; Turner & Flemming, Reference Turner and Flemming2019; Waling et al., Reference Waling, Lyons, Alba, Minichiello, Barrett and Hughes2019; Wilson & Birch, Reference Wilson and Birch2017). We then expanded our original concept of “services/programs” to include practical and medical aspects of care. We identified four main themes: (1) lack of preparation for the journey ahead, (2) lack of attention to the whole person, (3) lack of collaborative and trusting relationships, and (4) facilitating caregiving at home. The first three themes are directly linked to our research question; the fourth one goes beyond the original goal and summarizes ways to address the challenges identified in the literature.
Lack of preparation for the journey ahead
Emotional turmoil. Both caregivers and patients experienced positive and negative feelings that changed as the end-of-life trajectory unfolded (Ewing et al., Reference Ewing, Brundle, Payne and Grande2013; Ewing & Grande, Reference Ewing and Grande2012; Hutchinson & Van Wissen, Reference Hutchinson and Van Wissen2017; Lee et al., Reference Lee, Melia, Yao, Lin, Chiu and Hu2013; Wilson & Birch, Reference Wilson and Birch2017; Woodman, Baillie, & Sivell, Reference Woodman, Baillie and Sivell2015). Positive feelings included peacefulness, a sense of giving back, and a sense of accomplishment in supporting the wishes of loved ones to die at home (Hammond & Baxter, Reference Hammond, Baxter, Holtslander, Peacock and Bally2019; Heath, Carey, & Chong, Reference Heath, Carey and Chong2018; Hutchinson & Van Wissen, Reference Hutchinson and Van Wissen2017; Lee et al., Reference Lee, Melia, Yao, Lin, Chiu and Hu2013; Robinson et al., Reference Robinson, Bottorff, McFee, Bissell and Fyles2017; Totman, Pistrang, Smith, Hennessey, & Martin, Reference Totman, Pistrang, Smith, Hennessey and Martin2015; Woodman et al., Reference Woodman, Baillie and Sivell2015). These positive responses contrasted with feelings of guilt and despair, particularly for caregivers who could not keep their aging person within a familial environment, or when patients’ end-of-life preferences were not fulfilled (Heath et al., Reference Heath, Carey and Chong2018; Woodman et al., Reference Woodman, Baillie and Sivell2015).
Caregivers’ physical and psychological health were impacted by the demands of the caregiving role, and depression and anxiety were often reported (DiGiacomo, Davidson, Byles, & Nolan, Reference DiGiacomo, Davidson, Byles and Nolan2013; Dionne-Odom et al., Reference Dionne-Odom, Applebaum, Ornstein, Azuero, Warren and Taylor2017; Jack, O’Brien, Scrutton, Baldry, & Groves, Reference Jack, O’Brien, Scrutton, Baldry and Groves2014; Totman et al., Reference Totman, Pistrang, Smith, Hennessey and Martin2015). Feeling homebound and sleep deprived contributed to the emotional distress of caregivers (Morris et al., Reference Morris, King, Turner and Payne2015; Robinson et al., Reference Robinson, Bottorff, McFee, Bissell and Fyles2017; Totman et al., Reference Totman, Pistrang, Smith, Hennessey and Martin2015). In addition, a sense of responsibility for patients’ well-being seemed to exacerbate the burden of caregiving (Totman et al., Reference Totman, Pistrang, Smith, Hennessey and Martin2015).
Depression and anxiety affected patients at end of their lives (Fukui et al., Reference Fukui, Fujita, Tsujimura, Sumikawa and Hayashi2011; Vassal, Le Coz, Hervé, Matillon, & Chapuis, Reference Vassal, Le Coz, Hervé, Matillon and Chapuis2011). Fukui et al. (Reference Fukui, Fujita, Tsujimura, Sumikawa and Hayashi2011) reported that palliative cancer patients experiencing depression and anxiety prior to discharge from hospital to home-care settings were less likely to have a home death than those who did not report depression and anxiety. Home death, however, was reported to positively influence bereaved caregivers’ mental health (Hatano et al., Reference Hatano, Aoyama, Morita, Yamaguchi, Maeda and Kizawa2017).
Grief, including anticipatory grief, was a major challenge for caregivers. They valued bereavement support, although they did not always receive it (Aoun, Breen, White, Rumbold, & Kellehear, Reference Aoun, Breen, White, Rumbold and Kellehear2018; Bainbridge & Seow, Reference Bainbridge and Seow2018; Ewing & Grande, Reference Ewing and Grande2012; Hughes, Noyes, Eckley, & Pritchard, Reference Hughes, Noyes, Eckley and Pritchard2019; Knighting et al., Reference Knighting, O’Brien, Roe, Gandy, Lloyd‐Williams and Nolan2015; Totman et al., Reference Totman, Pistrang, Smith, Hennessey and Martin2015; Woodman et al., Reference Woodman, Baillie and Sivell2015). The reactive, rather than proactive, nature of bereavement supports, or the lack of services were frequently seen as problematic and resulted in many caregivers foregoing support altogether (Hughes et al., Reference Hughes, Noyes, Eckley and Pritchard2019).
Relating to others. Loss of mobility associated with physical decline evoked an emotional response from patients, sometimes expressed as a sense of shame. For example, this feeling could, in turn, result in perceived social isolation, as patients avoided going outside because of their sense of shame about requiring walking aids (Nicholson, Meyer, Flatley, & Holman, Reference Nicholson, Meyer, Flatley and Holman2013). Loneliness and isolation were very common for aging and dying persons and their caregivers. These two commonly related experiences were compounded by the absence of a support network, frequently constituting the main barrier to aging and dying at home (Turner & Flemming, Reference Turner and Flemming2019). In general, these issues were inadequately addressed, with very little or no preparation for what was ahead (Hammond & Baxter, Reference Hammond, Baxter, Holtslander, Peacock and Bally2019; Mogan et al., Reference Mogan, Lloyd-Williams, Harrison Dening and Dowrick2018; Morris et al., Reference Morris, King, Turner and Payne2015; Pleschberger & Wosko, Reference Pleschberger and Wosko2015; Sixsmith et al., Reference Sixsmith, Fang, Woolrych, Canham, Battersby, Ren, Hankivsky and Jordan-Zachery2019; Totman et al., Reference Totman, Pistrang, Smith, Hennessey and Martin2015; Woodman et al., Reference Woodman, Baillie and Sivell2015).
…like that first night we came home from the hospital […] I was really sad, because suddenly when we left the hospital I realised we were on our own (Caregiver, Totman et al., Reference Totman, Pistrang, Smith, Hennessey and Martin2015, p. 501).
Losing the relationship once held with the dying person and grieving before the death was particularly challenging for caregivers (Totman et al., Reference Totman, Pistrang, Smith, Hennessey and Martin2015). On the other hand, patients did not wish to become a burden for caregivers, and this influenced their decisions regarding whether to remain at home (Turner & Flemming, Reference Turner and Flemming2019). Maintaining personal autonomy was particularly important for members of marginalized populations such as lesbian and gay older adults, who expressed concerns about discrimination, hostility, and potential elder abuse (Waling et al., Reference Waling, Lyons, Alba, Minichiello, Barrett and Hughes2019).
In many instances, having to advocate strongly for their loved one’s interests may have exacerbated the emotional distress experienced by caregivers (Totman et al., Reference Totman, Pistrang, Smith, Hennessey and Martin2015). In addition, family caregiver disagreements around decision making could add another layer to the emotional distress experienced by families of persons aging and dying at home (Wilson & Birch, Reference Wilson and Birch2017; Woodman et al., Reference Woodman, Baillie and Sivell2015).
Information and resources. Many patients aging and dying at home and their caregivers felt lost, and they were not always aware of the supportive resources available to them (Bainbridge & Seow, Reference Bainbridge and Seow2018; Dionne-Odom et al., Reference Dionne-Odom, Applebaum, Ornstein, Azuero, Warren and Taylor2017; Ewing & Grande, Reference Ewing and Grande2012; Hashem et al., Reference Hashem, Brigden, Wilson and Butler2020; Morris et al., Reference Morris, King, Turner and Payne2015; Woodman et al., Reference Woodman, Baillie and Sivell2015). General information needs (Wilson & Birch, Reference Wilson and Birch2017) and equipment retrieval and instruction in the home (Ewing et al., Reference Ewing, Brundle, Payne and Grande2013; Ewing & Grande, Reference Ewing and Grande2012; Hashem et al., Reference Hashem, Brigden, Wilson and Butler2020; Mogan et al., Reference Mogan, Lloyd-Williams, Harrison Dening and Dowrick2018; Robinson et al., Reference Robinson, Bottorff, McFee, Bissell and Fyles2017), as well as answers to questions related to legal proceedings and finances (Ewing et al., Reference Ewing, Brundle, Payne and Grande2013; Ewing & Grande, Reference Ewing and Grande2012; Hashem et al., Reference Hashem, Brigden, Wilson and Butler2020; Knighting et al., Reference Knighting, O’Brien, Roe, Gandy, Lloyd‐Williams and Nolan2015; Sixsmith et al., Reference Sixsmith, Fang, Woolrych, Canham, Battersby, Ren, Hankivsky and Jordan-Zachery2019; Wilson & Birch, Reference Wilson and Birch2017) were broadly highlighted as neglected aspects of care, adding to the burden of suffering and caregiving. DiGiacomo et al. (Reference DiGiacomo, Davidson, Byles and Nolan2013) reported that the loss of financial resources had an impact on the physical and mental well-being of widows, consequently having a negative impact on bereavement.
Remaining at home required support with housework, physical care, and navigating various systems. A lack of support in these areas negatively affected patients’ and caregivers’ ability to cope, and caused distress (Ewing et al., Reference Ewing, Brundle, Payne and Grande2013; Ewing & Grande, Reference Ewing and Grande2012; Knighting et al., Reference Knighting, O’Brien, Roe, Gandy, Lloyd‐Williams and Nolan2015; Morris et al., Reference Morris, King, Turner and Payne2015; Woodman et al., Reference Woodman, Baillie and Sivell2015). Some caregivers, however, had difficulty accepting help out of a sense of personal responsibility to their dying loved one, and occasionally felt judged as inadequate by direct observations from paid health care providers (Jack et al., Reference Jack, O’Brien, Scrutton, Baldry and Groves2014, 2016; Robinson et al., Reference Robinson, Bottorff, McFee, Bissell and Fyles2017). Persons aging and dying at home reported choosing to manage without help for many reasons, including the fear of losing autonomy, confidence, and personhood (Nicholson et al., Reference Nicholson, Meyer, Flatley and Holman2013; Turner & Flemming, Reference Turner and Flemming2019).
The meaning of home. An additional challenge was the need to change the overall home environment when the decision was made to care for a loved one at home. Home was described as more than a physical space in some articles; it was viewed as a site of intimate personal and socio-emotional relationships (Milligan et al., Reference Milligan, Turner, Blake, Brearley, Seamark and Thomas2016; Morris et al., Reference Morris, King, Turner and Payne2015). Caregivers reported that the home environment changed negatively as unfamiliar items such as commodes and lifts became part of their life (Morris et al., Reference Morris, King, Turner and Payne2015). There was a loss of privacy expressed by caregivers, and a feeling that their personal space shrank (Morris et al., Reference Morris, King, Turner and Payne2015; Woodman et al., Reference Woodman, Baillie and Sivell2015). Caregivers’ relationship with their home could change again after the death of their loved ones. Many people avoided some parts of the home or felt the need to redecorate to cope with the absence of the deceased (Milligan et al., Reference Milligan, Turner, Blake, Brearley, Seamark and Thomas2016; Morris et al., Reference Morris, King, Turner and Payne2015). DiGiacomo et al. (Reference DiGiacomo, Davidson, Byles and Nolan2013) pointed out that the death of a husband could directly affect the widow’s living arrangement (needing to move, for example) causing stress, anxiety, and depression.
Lack of attention to the whole person
Symptom management. Although the review’s focus was on the psychosocial aspects of care, much of the reviewed literature emphasized that the need to address physical symptoms of patients and caregivers was directly related to supporting the psychosocial aspects of aging and dying in place. Difficulties with managing patients’ symptoms were overwhelming for caregivers (Phongtankuel et al., Reference Phongtankuel, Scherban, Reid, Finley, Martin and Dennis2016; Woodman et al., Reference Woodman, Baillie and Sivell2015), and discomfort in dealing with medications and administering opioids was particularly challenging (Ewing et al., Reference Ewing, Brundle, Payne and Grande2013; Ewing & Grande, Reference Ewing and Grande2012; Hashem et al., Reference Hashem, Brigden, Wilson and Butler2020; Morris et al., Reference Morris, King, Turner and Payne2015)
[…] Symptom management is crucial as this is integral to psychosocial care because you can’t separate the physical from the patient’s psyche; it is the holistic aspects of care that results in quality psychosocial care (Healthcare provider, Oliver, Reference Oliver2010, p. 25).
Psychological support. In general, the challenge of managing crises at home was a common reason for emergency department admissions and hospitalizations, as caregivers felt the emotional burden of providing care in these situations (Ewing et al., Reference Ewing, Brundle, Payne and Grande2013; Ewing & Grande, Reference Ewing and Grande2012; Gomes et al., Reference Gomes, Calanzani, Koffman and Higginson2015; Hughes et al., Reference Hughes, Noyes, Eckley and Pritchard2019; Mogan et al., Reference Mogan, Lloyd-Williams, Harrison Dening and Dowrick2018; Phongtankuel et al., Reference Phongtankuel, Scherban, Reid, Finley, Martin and Dennis2016; Robinson et al., Reference Robinson, Bottorff, McFee, Bissell and Fyles2017; Wilson & Birch, Reference Wilson and Birch2017). Although psychosocial distress was commonly reported and may have required mental health professionals to support caregivers (Kobayakawa et al., Reference Kobayakawa, Okamura, Yamagishi, Morita, Kawagoe and Shimizu2016), this support was not always provided (Perner, Köhler, Brähler, & Götze, Reference Perner, Köhler, Brähler and Götze2012).
Having a specific point of contact for assistance, especially during times of crisis, provided reassurance while remaining at home; however, having someone to turn to was not always a reality (Ewing et al., Reference Ewing, Brundle, Payne and Grande2013; Ewing & Grande, Reference Ewing and Grande2012; Gomes et al., Reference Gomes, Calanzani, Koffman and Higginson2015; Hashem et al., Reference Hashem, Brigden, Wilson and Butler2020; Hughes et al., Reference Hughes, Noyes, Eckley and Pritchard2019; Knighting et al., Reference Knighting, O’Brien, Roe, Gandy, Lloyd‐Williams and Nolan2015; Mogan et al., Reference Mogan, Lloyd-Williams, Harrison Dening and Dowrick2018). Moreover, a lack of supports during times of transition, such as from hospice to home, was particularly detrimental to caregivers’ ability to cope, and took away from continuity of care (Bainbridge & Seow, Reference Bainbridge and Seow2018; Danielsen et al., Reference Danielsen, Sand, Rosland and Førland2018; Ewing & Grande, Reference Ewing and Grande2012; Hashem et al., Reference Hashem, Brigden, Wilson and Butler2020; Hutchinson & Van Wissen, Reference Hutchinson and Van Wissen2017; Jack et al., Reference Jack, Mitchell, Cope and O’Brien2016; Phongtankuel et al., Reference Phongtankuel, Scherban, Reid, Finley, Martin and Dennis2016; Robinson et al., Reference Robinson, Bottorff, McFee, Bissell and Fyles2017; Wilson & Birch, Reference Wilson and Birch2017; Woodman et al., Reference Woodman, Baillie and Sivell2015).
Spiritual support. Spiritual suffering, accompanied by a loss of confidence and feelings of guilt, was relatively common for patients (Vassal et al., Reference Vassal, Le Coz, Hervé, Matillon and Chapuis2011). Support to maintain spiritual well-being, however, was not always available (Bainbridge & Seow, Reference Bainbridge and Seow2018; Ewing et al., Reference Ewing, Brundle, Payne and Grande2013; Ewing & Grande, Reference Ewing and Grande2012; Morris et al., Reference Morris, King, Turner and Payne2015; Totman et al., Reference Totman, Pistrang, Smith, Hennessey and Martin2015). Acknowledging dread and being supported through fear was a critical issue mentioned in the literature. Bainbridge and Seow (Reference Bainbridge and Seow2018) found that a large number of close to 400 patients receiving end-of-life care rated satisfaction with spiritual support lower than satisfaction with other forms of support, independent of care setting.
You know, if you’re so gripped with fear about everything, you’re already kind of dead. (Caregiver, Totman et al., Reference Totman, Pistrang, Smith, Hennessey and Martin2015, p. 502).
Lack of collaborative and trusting relationships
Communication. Caregivers often felt unsupported, overlooked, and let down by health care providers when caring for people at home (Totman et al., Reference Totman, Pistrang, Smith, Hennessey and Martin2015; Woodman et al., Reference Woodman, Baillie and Sivell2015). Communication was particularly linked to the ability to age and die in place, and a lack thereof, negatively impacted the psychosocial well-being of patients and caregivers alike. Both groups highlighted poor communication with health care providers, which was worsened, in many instances, by a lack of empathy, avoidance of difficult conversations, and professionals failing to acknowledge patients’ and families’ preferences (Danielsen et al., Reference Danielsen, Sand, Rosland and Førland2018; Hashem et al., Reference Hashem, Brigden, Wilson and Butler2020; Mogan et al., Reference Mogan, Lloyd-Williams, Harrison Dening and Dowrick2018; Morris et al., Reference Morris, King, Turner and Payne2015; Perner et al., Reference Perner, Köhler, Brähler and Götze2012; Totman et al., Reference Totman, Pistrang, Smith, Hennessey and Martin2015; Wilson & Birch, Reference Wilson and Birch2017). This posed a major barrier to continuity of care and effective coping during the end-of-life process (Danielsen et al., Reference Danielsen, Sand, Rosland and Førland2018; Hashem et al., Reference Hashem, Brigden, Wilson and Butler2020; Totman et al., Reference Totman, Pistrang, Smith, Hennessey and Martin2015; Wilson & Birch, Reference Wilson and Birch2017).
Rapport. Lack of rapport with the at-home care team negatively affected the ability of patients and caregivers to form trusting relationships (Danielsen et al., Reference Danielsen, Sand, Rosland and Førland2018; Kobayakawa et al., Reference Kobayakawa, Okamura, Yamagishi, Morita, Kawagoe and Shimizu2016; Mogan et al., Reference Mogan, Lloyd-Williams, Harrison Dening and Dowrick2018; Morris et al., Reference Morris, King, Turner and Payne2015; Perner et al., Reference Perner, Köhler, Brähler and Götze2012). Health care providers’ attention to cultural and religious differences was also a gap in various situations, complicated by language barriers or needs related to faith-specific practices, for example (Morris et al., Reference Morris, King, Turner and Payne2015; Sixsmith et al., Reference Sixsmith, Fang, Woolrych, Canham, Battersby, Ren, Hankivsky and Jordan-Zachery2019; Totman et al., Reference Totman, Pistrang, Smith, Hennessey and Martin2015).
Death literacy. Lack of broad discussions regarding death, dying, and advance care planning, commonly addressed as “death literacy”, was considered a gap (Bainbridge & Seow, Reference Bainbridge and Seow2018; Ewing et al., Reference Ewing, Brundle, Payne and Grande2013; Gomes et al., Reference Gomes, Calanzani, Koffman and Higginson2015; Hashem et al., Reference Hashem, Brigden, Wilson and Butler2020; Wilson & Birch, Reference Wilson and Birch2017), as was support in decision making (Ewing & Grande, Reference Ewing and Grande2012; Knighting et al., Reference Knighting, O’Brien, Roe, Gandy, Lloyd‐Williams and Nolan2015; Robinson et al., Reference Robinson, Bottorff, McFee, Bissell and Fyles2017; Woodman et al., Reference Woodman, Baillie and Sivell2015). That, in turn, had an impact on patients’ and caregivers’ lack of understanding about illness progression and often led to difficulties when discussing life expectancy, which caused additional worry and distress to caregivers (Ewing & Grande, Reference Ewing and Grande2012; Hutchinson & Van Wissen, Reference Hutchinson and Van Wissen2017; Robinson et al., Reference Robinson, Bottorff, McFee, Bissell and Fyles2017). Preparing for the future was of utmost importance for both caregivers and patients (Fukui et al., Reference Fukui, Fujita, Tsujimura, Sumikawa and Hayashi2011; Hatano et al., Reference Hatano, Aoyama, Morita, Yamaguchi, Maeda and Kizawa2017; Hudson et al., Reference Hudson, Remedios, Zordan, Thomas, Clifton and Crewdson2012; Totman et al., Reference Totman, Pistrang, Smith, Hennessey and Martin2015):
…although you know kind of in the background, sometimes it helps when someone says it, you know, this is what you can expect (Caregiver, Totman et al., Reference Totman, Pistrang, Smith, Hennessey and Martin2015, p. 502).
Facilitating caregiving at home
Community resources. Maintaining social networks was very important for aging persons and caregivers alike, and these networks included not only family and friends but also community groups (Hughes et al., Reference Hughes, Noyes, Eckley and Pritchard2019; Mills et al., Reference Mills, Rosenberg and McInerney2015; Sixsmith et al., Reference Sixsmith, Fang, Woolrych, Canham, Battersby, Ren, Hankivsky and Jordan-Zachery2019; Totman et al., Reference Totman, Pistrang, Smith, Hennessey and Martin2015). Their support went beyond emotional support for caregivers through connection and empowerment including, in many cases, practical support such as assistance with financial planning and navigation (Mills et al., Reference Mills, Rosenberg and McInerney2015). DiGiacomo et al. (Reference DiGiacomo, Davidson, Byles and Nolan2013), however, pointed out that social support is not a one-size-fits-all construct, and satisfaction with its availability may vary depending on individuals’ unique needs and contexts.
Empowering opportunities for social connection offered the potential for meaning making among patients and caregivers or between caregivers (Mills et al., Reference Mills, Rosenberg and McInerney2015; Nicholson et al., Reference Nicholson, Meyer, Flatley and Holman2013; Totman et al., Reference Totman, Pistrang, Smith, Hennessey and Martin2015). Consistent, reliable social networking promoted connectedness and facilitated staying at home at the end of life (Lum et al., Reference Lum, Lou, Chen, Wong, Luo and Tong2016; Mogan et al., Reference Mogan, Lloyd-Williams, Harrison Dening and Dowrick2018; Woodman et al., Reference Woodman, Baillie and Sivell2015). Community resources focused on grief and bereavement represented an option to address anticipatory grief (Mills et al., Reference Mills, Rosenberg and McInerney2015). Further, bereavement support groups and interventions in the community may positively influence bereavement outcomes (DiGiacomo et al., Reference DiGiacomo, Davidson, Byles and Nolan2013; Gauthier & Gagliese, Reference Gauthier and Gagliese2012). Finally, public education initiatives focused on death and dying, particularly advance care planning, could prevent transition problems between care settings (Wilson & Birch, Reference Wilson and Birch2017).
Care at home. The presence of high-quality home care was a major facilitator of aging and dying in place, whereas poor quality of home care or inappropriate home environments were detrimental (Turner & Flemming, Reference Turner and Flemming2019). Care at home was provided mostly by nurses and health care support workers who may or may not be connected to a hospice. Establishing close collaboration among health care professionals, caregivers, and patients early in their trajectory was reported to be essential (Danielsen et al., Reference Danielsen, Sand, Rosland and Førland2018; Hughes et al., Reference Hughes, Noyes, Eckley and Pritchard2019). Trusting relationships with formal support networks based on reciprocal empathy and maintaining normality were seen as crucial. Such relationships had a positive impact on patients’ emotions and on caregivers’ ability to cope with their role (Danielsen et al., Reference Danielsen, Sand, Rosland and Førland2018; Hashem et al., Reference Hashem, Brigden, Wilson and Butler2020; Hudson et al., Reference Hudson, Trauer, Kelly, O’Connor, Thomas and Summers2013; Hughes et al., Reference Hughes, Noyes, Eckley and Pritchard2019; Jack et al., Reference Jack, O’Brien, Scrutton, Baldry and Groves2014; Sims-Gould & Martin-Matthews, Reference Sims-Gould and Martin-Matthews2010; Woodman et al., Reference Woodman, Baillie and Sivell2015).
I would say that one of the biggest ones [supports] for my mom is the companionship. Conversation, having a tea or coffee… they sit down. They have a cup of tea… she does what she needs to do but she’s also very good company for my mother (Caregiver, Sims-Gould & Martin-Matthews, Reference Sims-Gould and Martin-Matthews2010, p. 419).
Active general practitioner (GP) engagement in end-of-life care was seen as important in supporting the physical and mental well-being of the patient with whom they had a long-standing, trusting relationship. Home care teams also valued GPs’ long-term knowledge of the patients’ health, which enhanced continuity of care (Danielsen et al., Reference Danielsen, Sand, Rosland and Førland2018; Gomes et al., Reference Gomes, Calanzani, Koffman and Higginson2015; Hashem et al., Reference Hashem, Brigden, Wilson and Butler2020). Mogan et al. (Reference Mogan, Lloyd-Williams, Harrison Dening and Dowrick2018) highlighted that, “no matter the model of care provided, regular contact with a healthcare professional, and not necessarily a palliative care specialist, might play an important role in end-of-life care at home for people with dementia” (p. 1049). Care at home could be enhanced by professionals conducting systematic needs assessments with caregivers (Hammond & Baxter, Reference Hammond, Baxter, Holtslander, Peacock and Bally2019 ; Hudson et al., Reference Hudson, Remedios, Zordan, Thomas, Clifton and Crewdson2012 ; Wilson & Birch, Reference Wilson and Birch2017). These assessments should include psychological and physical health, social, spiritual, cultural, financial, and practical elements (Aoun, Breen, et al., Reference Aoun, Breen, White, Rumbold and Kellehear2018; Hudson et al., Reference Hudson, Remedios, Zordan, Thomas, Clifton and Crewdson2012; Jack et al., Reference Jack, O’Brien, Scrutton, Baldry and Groves2014). Aoun, Breen, et al. (Reference Aoun, Breen, White, Rumbold and Kellehear2018) found that bereaved caregivers who received a nursing intervention that assessed needs before the death reported benefits. They perceived their support needs as being better met and experienced less strain than the control group who did not receive equivalent interventions.
Caregivers pointed out that proactive equipment training provided by the health care team would help them support their loved one’s desire to die at home (Ewing et al., Reference Ewing, Brundle, Payne and Grande2013; Ewing & Grande, Reference Ewing and Grande2012; Hashem et al., Reference Hashem, Brigden, Wilson and Butler2020; Mogan et al., Reference Mogan, Lloyd-Williams, Harrison Dening and Dowrick2018; Robinson et al., Reference Robinson, Bottorff, McFee, Bissell and Fyles2017). They reported feeling reassured particularly when they received validation from formal caregivers related to the task that they were doing (Jack et al., Reference Jack, O’Brien, Scrutton, Baldry and Groves2014).
Made me feel that we were doing everything we should do, there’s always a doubt in your mind that “oh, what if?,” “should I do this; should I do that?’, but they allowed you to stand back and think “actually, there isn’t anything else that we can do; this is the best it is” (Caregiver, Jack et al., Reference Jack, O’Brien, Scrutton, Baldry and Groves2014, p. 135).
Hospice care. Hospice at home, hospice day care, or community-based hospice programs were highlighted as successful facilitators of aging and dying in place (Bainbridge & Seow, Reference Bainbridge and Seow2018; Hashem et al., Reference Hashem, Brigden, Wilson and Butler2020; Hughes et al., Reference Hughes, Noyes, Eckley and Pritchard2019; Jack et al., Reference Jack, O’Brien, Scrutton, Baldry and Groves2014, 2016; Mogan et al., Reference Mogan, Lloyd-Williams, Harrison Dening and Dowrick2018; Woodman et al., Reference Woodman, Baillie and Sivell2015). Hospice clinical staff teams were recognized as highly trained to support not only the medical needs, but also the psychosocial needs of patients and caregivers (Hashem et al., Reference Hashem, Brigden, Wilson and Butler2020; Jack et al., Reference Jack, O’Brien, Scrutton, Baldry and Groves2014, 2016). Features such as the emotional and practical support to caregivers offered by night-sitting services (e.g., reassurance and peace of mind that patients were being looked after) were reported to be integral supports for caregivers (Hashem et al., Reference Hashem, Brigden, Wilson and Butler2020; Hughes et al., Reference Hughes, Noyes, Eckley and Pritchard2019; Jack et al., Reference Jack, O’Brien, Scrutton, Baldry and Groves2014).
The support of a palliative care team for caregivers supporting their loved ones at home gave them the ability to continue with normal life as much as possible (Jack et al., Reference Jack, O’Brien, Scrutton, Baldry and Groves2014, 2016; Morris et al., Reference Morris, King, Turner and Payne2015). Hospice at home helped to relieve the strain on caregivers, gave people time to balance their own lives with new duties, and had positive effects on bereaved caregivers’ mental health (Jack et al., Reference Jack, O’Brien, Scrutton, Baldry and Groves2014, 2016; Wright et al., Reference Wright, Keating, Balboni, Matulonis, Block and Prigerson2010).
She did the ironing for me – it sounds like such a simple little thing – but it meant the next day instead of sitting doing the ironing I took mum out for the day, and just being able to do that was just … it was just so nice. (Caregiver, Jack et al., Reference Jack, O’Brien, Scrutton, Baldry and Groves2014, p. 136).
Direct telephone lines for support (Hashem et al., Reference Hashem, Brigden, Wilson and Butler2020; Hughes et al., Reference Hughes, Noyes, Eckley and Pritchard2019; Mogan et al., Reference Mogan, Lloyd-Williams, Harrison Dening and Dowrick2018) as well as crisis intervention teams (Danielsen et al., Reference Danielsen, Sand, Rosland and Førland2018; Mogan et al., Reference Mogan, Lloyd-Williams, Harrison Dening and Dowrick2018; Phongtankuel et al., Reference Phongtankuel, Scherban, Reid, Finley, Martin and Dennis2016) were opportunities identified for future exploration. Caregivers pointed out that initiation of respite care or increased hours of respite services could also better support their caregiving role by allowing them to address their own need for rest (Ewing et al., Reference Ewing, Brundle, Payne and Grande2013; Ewing & Grande, Reference Ewing and Grande2012; Hashem et al., Reference Hashem, Brigden, Wilson and Butler2020; Hughes et al., Reference Hughes, Noyes, Eckley and Pritchard2019; Jack et al., Reference Jack, O’Brien, Scrutton, Baldry and Groves2014; Knighting et al., Reference Knighting, O’Brien, Roe, Gandy, Lloyd‐Williams and Nolan2015; Robinson et al., Reference Robinson, Bottorff, McFee, Bissell and Fyles2017). Anticipatory rather than reactive care was referenced as an opportunity to prevent distress and reduce hospital admissions (Hashem et al., Reference Hashem, Brigden, Wilson and Butler2020; Hughes et al., Reference Hughes, Noyes, Eckley and Pritchard2019).
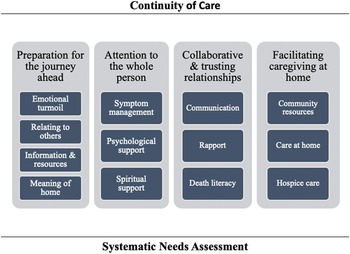
Figure 2 summarizes the challenges and opportunities we identified.

Figure 2. Summary of Semantic Analysis Results.
Discussion
We set out to identify psychosocial aspects of aging and dying in place that would point to gaps in programs and services, in preparation for a discussion with key stakeholders within the British Columbia hospice palliative care sector. That discussion would explore how hospices can best support British Columbia’s communities through the ongoing and accelerating demographic shifts. The multitude of psychosocial, practical, and medical issues emerging from an aging population demonstrates the current shortfall in programs and services but, conversely, highlights promising opportunities to address those gaps. Lack of attention to the whole person (dying person and caregivers), lack of preparation for the journey ahead, and lack of collaborative and trusting relationships were gaps affecting the psychosocial well-being of patients and caregivers that permeated most of the reviewed literature. We believe that a blend of initiatives in the community to maintain and expand social networks, combined with an integrated palliative approach to care within the health care system and an expansion of HPC in the community, can better support patients and caregivers alike, and mitigate some of the challenges that currently limit options for aging and dying in place.
The importance of community networks to support people experiencing loneliness, isolation, and the demands of caregiving highlighted in the literature we reviewed, was not a surprise. The Compassionate Communities and Compassionate Cities (CCC) movement, which started in the late 1990s, brought health promotion ideas to palliative care, building on community development strategies to support the dying person and their families (Kellehear, Reference Kellehear2013). CCC normalizes seeking and accepting emotional, social, and practical help from members of the community (family, friends, neighbours, schools, and workplaces – also called “informal social support”), encouraging the development of local caring social networks to support end-of-life care (Aoun, Breen, et al., Reference Aoun, Breen, White, Rumbold and Kellehear2018; Kellehear, Reference Kellehear2013). Aoun, Breen, et al. (Reference Aoun, Breen, White, Rumbold and Kellehear2018) pointed out that informal social support helps with emotional bonds, provides practical assistance, and improves the perceived sense of belonging for bereaved caregivers. Although CCC strategies may better prepare people for the journey ahead and positively impact their psychosocial well-being, Librada-Flores, Nabal-Vicuña, Forero-Vega, Muñoz-Mayorga, and Guerra-Martín (Reference Librada-Flores, Nabal-Vicuña, Forero-Vega, Muñoz-Mayorga and Guerra-Martín2020) recently showed that there is little and low-quality evidence about CCC development and assessment models. As the CCC movement is consolidated as an important approach to supporting the psychosocial well-being of the dying person and their caregivers, we echo Librada-Flores et al. (Reference Librada-Flores, Nabal-Vicuña, Forero-Vega, Muñoz-Mayorga and Guerra-Martín2020)’s call for a systematic documentation of the processes involved in CCC implementation and the development of an evaluation framework to measure CCC’s impact and effectiveness.
Attending to the needs of the whole person, integrating physical, psychosocial, and spiritual aspects of patient and family care is central to HPC (Hammond & Baxter, Reference Hammond, Baxter, Holtslander, Peacock and Bally2019). HPC aims to relieve suffering and improve the quality of living and dying (Canadian Institute for Health Information, 2018). A recent report from the Canadian Institute for Health Information highlights that community palliative care increases the likelihood that older people will remain at home; few Canadians, however, receive palliative care at home in their last year of life (Canadian Institute for Health Information, 2018; Tanuseputro, Budhwani, Bai, & Wodchis, Reference Tanuseputro, Budhwani, Bai and Wodchis2017). In the last 15 years, to address the changes in illness trajectories (i.e., people are living longer with life-limiting illnesses), the HCP concept has been expanded, shifting from a specialized service available to few at the end of life to an integrated approach to care, available to people living at home and in the community with life-limiting illnesses, at any point in their trajectory (Hammond & Baxter, Reference Hammond, Baxter, Holtslander, Peacock and Bally2019). An integrated palliative approach to care focuses on meeting patients’ and their families’ full range of needs—physical, psychosocial, and spiritual—throughout the course of an illness, or the process of aging, and in all settings where they live and receive care (Canadian Hospice Palliative Care Association, 2015). The approach does not imply, however, the need for increased specialist palliative care delivered upstream in the illness trajectory but, rather, enhancing supports embedded in the everyday care processes, wherever people happen to be and whoever their health care providers are (Sawatzky et al., Reference Sawatzky, Porterfield, Lee, Dixon, Lounsbury and Pesut2016). The integration of a palliative approach to care into generalist practice and the expansion of community palliative care could, and perhaps should, address the demand for innovative approaches to support people who wish to age and die in place.
An important gap that we pinpointed was in communication among patients, families, and health care providers, which was directly linked to poor continuity of care, affecting patient and caregiver coping and the establishment of trusting relationships. Although the literature we reviewed has not directly linked training and strong communication skills, enhancing training in this area is a feasible opportunity to improve the exchange of information for all concerned. Paladino et al. (Reference Paladino, Bernacki, Neville, Kavanagh, Miranda and Palmor2019) caution, however, that education alone will not be a sufficient measure to address the need to improve, for example, conversations about serious illness between health care providers and patients and families. They argue that system-level changes must support the integration of these conversations into clinical practice, which in turn will improve trust and support coping.
Expanding HPC in the community through “Hospice at Home” programs may be another important part of the system-level changes necessary to improve the psychosocial well-being of patients and caregivers at end of life, while also supporting the desire to age and die in place. “Hospice at Home” is not a novel concept (Ahn et al., Reference Ahn, Song, Choi, Jho, Park and Sung2019; Rees-Roberts et al., Reference Rees-Roberts, Williams, Hashem, Brigden, Greene and Gage2019; Shepperd, Gonçalves-Bradley, Straus, & Wee, Reference Shepperd, Gonçalves-Bradley, Straus and Wee2016); Shepperd et al. (Reference Shepperd, Gonçalves-Bradley, Straus and Wee2016) demonstrated that it increased the likelihood of people dying at home. However, not all “Hospice at Home” programs are made equal. Hashem et al. (Reference Hashem, Brigden, Wilson and Butler2020) argue that these programs are composed of a diverse range of services based on local needs and adapted to different contexts. These researchers highlight some key areas of service that match the results of our own rapid review: access to medications, the support of skilled staff that includes rapid response, continuity of care, anticipatory care, and attention to caregivers through practical and emotional support (including mentorship in the use of equipment and help through crisis). Health care providers’ having excellent communication skills is paramount to the success of “Hospice at Home” programs.
HPC is especially tailored to address coping and distress associated with life-limiting illnesses (Hammond & Baxter, Reference Hammond, Baxter, Holtslander, Peacock and Bally2019), both of which were major gaps pointed out in the literature that we reviewed. An important feature of HPC is the engagement of volunteers. Since its inception, volunteers have been fundamental to the HPC movement (Morris et al., Reference Morris, King, Turner and Payne2015). They fulfill many roles, such as providing companionship or practical and emotional support, including bereavement support and advocacy, both in the community and in institutional settings (Claxton-Oldfield, Reference Claxton-Oldfield2015; Diamond, Llewelyn, Relf, & Bruce, Reference Diamond, Llewelyn, Relf and Bruce2012; Pesut, Hooper, Lehbauer, & Dalhuisen, Reference Pesut, Hooper, Lehbauer and Dalhuisen2014; Vanderstichelen et al., Reference Vanderstichelen, Houttekier, Cohen, Van Wesemael, Deliens and Chambaere2018). Caregivers reported that bereavement volunteers helped them gain perspective and hope for the future by exploring strategies to overcome difficulties, providing insight, and building a consistent, trusting relationship outside the caregivers’ regular social networks. Certain social traits of bereavement volunteers also contributed to the overall satisfaction felt by caregivers, such as listening skills, encouraging reflection, and remaining non-judgemental (Diamond et al., Reference Diamond, Llewelyn, Relf and Bruce2012).
Hospice volunteers often receive education and training, and in most cases, it is a mandatory prerequisite to taking on any role in assisting with end-of-life care (Diamond et al., Reference Diamond, Llewelyn, Relf and Bruce2012; Woitha et al., Reference Woitha, Hasselaar, Van Beek, Radbruch, Jaspers and Engels2015). When investigating the impact of volunteers in hospice care, Block et al. (Reference Block, Casarett, Spence, Gozalo, Connor and Teno2010) demonstrated that hospice programs with high use of volunteers per patient, per day had high ratings in terms of overall quality, as perceived by bereaved family members. On the other hand, Kellehear (Reference Kellehear2013) described a CCC initiative adopted by a Hospice in England in which volunteers were recruited to support frail and vulnerable people, including those with life-limiting illnesses. The hospice provided a short training in care, and volunteers from the community committed to regularly visiting people at home. Although this network of volunteers was established to address loneliness and isolation, early audits and evaluations revealed reduction in use of unscheduled health care services by people receiving the volunteer support. Despite the positive impact of volunteers described in the literature, Claxton-Oldfield (Reference Claxton-Oldfield2015) stated that hospice-trained volunteers are underutilized in Canada and that more needs to be done to promote their value to patients and families.
We suggest that a network of hospice-trained volunteers in the community has the potential to address many of the challenges related to psychosocial care identified in the literature. Volunteers can act as a point of contact for patients and families, helping local networks to access the resources they need, thus supporting continuity of care, an underlining gap voiced by patients and families alike that affects their psychosocial well-being. To this end, our organization is currently developing a volunteer-led program to support caregivers in the community.
A key strength of this RR is its practical application, an inherent goal of RRs. Our results were presented at the PHWG roundtable event held on November 2019, and they contributed meaningfully to the decisions made by participating British Columbia HPC stakeholders. The quality of the research included in the review was generally high, which suggests high validity and reliability for our findings. RRs have limitations, however, as components of the systematic review process were simplified or omitted to produce information in a timely manner (Khangura, Konnyu, Cushman, Grimshaw, & Moher, Reference Khangura, Konnyu, Cushman, Grimshaw and Moher2012). Tricco et al. (Reference Tricco, Antony, Zarin, Strifler, Ghassemi and Ivory2015) highlights that poor quality of reporting is one major pitfall for RRs. We addressed this issue by recording, and therefore reporting, our approach in detail, allowing reproducibility of the research. Limiting the search to three databases may have introduced publication bias, thereby incidentally omitting relevant publications. And yet, expanding searches to include articles written in three languages partially overcame this limitation. The majority of articles included in the current RR were qualitative studies or had a qualitative component to them, potentially limiting the generalizability of our results.
Final Considerations and Implications for Practice
As the senior population grows, our health care system faces new challenges to support a great number of Canadians who desire to age and die at home. The present study identified a number of challenges related to psychosocial aspects of aging and dying in place. Equally important, however, were the opportunities we identified to overcome these challenges. We then identified ways to leverage these opportunities:
-
• Expansion of the CCC movement encouraging the development of local caring social networks to support end-of-life care
-
• Implementation of an integrated palliative approach to care, which includes training of nurses, GPs, and health care support workers in palliative care principles
-
• Health care provider (HPC professionals and non-HPC professionals) education and training focused on communication skills and the psychosocial and spiritual aspects of end-of-life care
-
• Caregiver education related to end-of-life topics, including resilience, coping, and death literacy
-
• Expansion of “Hospice at Home” programs focused on preparation for the future and response to crisis (use of validated tools to identify patients’ and caregivers’ holistic needs)
-
• Expansion of hospice-trained volunteer networks in the community including providing support to local caring social networks
We would also argue that all stakeholders, including caregivers, should be involved in the development of any initiative to overcome challenges affecting opportunities for living and dying at home, and that initiatives should document processes and develop an evaluation framework to measure their impact and effectiveness.
Although the BC Care Providers Association forecasts a high demand for new long-term care beds with the expected demographic shifts in our province, enhancing supports to local caring networks, implementing an integrated palliative approach to care, and expanding HPC in the community may mitigate this demand and ease the path toward Canadians’ widely preferred choice of aging and dying at home.
Acknowledgements
We thank Laura Hebert for her participation in the first stages of this review (from protocol development until completion of data abstraction). We also thank Anke Krey for summarizing, conducting data abstraction, and providing quality appraisal of the German articles.
Supplementary Materials
To view supplementary material for this article, please visit http://doi.org/10.1017/S071498082200023X.
Availability of data and materials
All data generated or analysed during this study are included in this published article.
Authors’ contributions
Both authors contributed to the design and execution of the review, synthesis, interpretation of results, and reporting. Both authors read and approved the final manuscript.
Funding
This review did not receive any external funding.