Pulmonary embolism (PE) has an annual incidence of 0.50-0.69 per 1,000 in the general populationReference Naess, Christiansen, Romundstad, Cannegieter, Rosendaal and Hammerstrøm 1 and is a preventable cause of death among hospitalized patients. The rate of venous thromboembolism (VTE) (both PE and deep venous thrombosis [DVT]) among hospitalized patients with acute ischemic stroke (AIS) between 1979 and 2003 in a hospital discharge survey was found to be 0.51%, 0.74% and 1.17%, respectively.Reference Skaf, Stein, Beemath, Sanchez, Bustamante and Olson 2 The mortality related to PE can be as high as 24%Reference Carson, Kelley and Duff 3 but early treatment is highly effective.
Deaths occurring in first week after a large stroke are primarily due to direct effect of brain injury, while deaths occurring subsequently are due to preventable medical conditions like PE.Reference Skaf, Stein, Beemath, Sanchez and Olson 4 Patients with stroke are at higher risk of VTE due to bed rest, limb paralysis and increased pro-thrombotic state.Reference Davenport, Dennis, Wellwood and Warlow 5 Modern preventive therapy for VTE on a stroke unit can substantively reduce the occurrence of this common stroke-related morbidity.Reference Muir 6 , Reference Dennis, Sandercock, Graham and Forbes 7
Pulmonary embolism may be associated with AIS both as a concurrent or as a consequence of hemiplegia. The etiology of ischemic stroke is undetermined even after extensive investigations in roughly 25% of patients. These strokes are presumed to be embolic in nature and recently classified as Embolic Strokes of Undetermined Source (ESUS). Paradoxical embolism is believed to be an important cause for ESUS.Reference Hart, Diener and Coutts 8 Patients with paradoxical embolism are also at an increased risk for PE. Pulmonary VTE can result in increased right heart pressure leading to paradoxical embolism via right-to-left cardiac shunt such as a patent foramen ovale.
We report the modern prevalence of PE among stroke patients both as a concurrent diagnosis and as a consequence of hemiplegia.
All stroke patients in Calgary receive a stroke protocol CT and multiphase CT angiogram (CTA) (arch to vertex) at presentation. We retrospectively examined CTA of patients with AIS to determine the frequency of concurrent PE in AIS. A standard CTA stroke protocol examines the neurovasculature from the aortic arch to the vertex of the head, providing additional information on the angiography of the upper lobes of the lung including the hilum. This study was approved by the Conjoint Health Research Ethics Board at the University of Calgary. We screened all CTA studies of patients who presented to Foothills Medical Centre, Calgary with transient ischemic attacks or stroke. To identify the patients, we conducted a text search of our hospital radiology database from January 2015 to May 2016 for the word “pulmonary emboli” or “pulmonary thrombus” or “pulmonary artery thrombus” or “pulmonary thromboembolus” or “pulmonary artery thromboembolus“ or “lung infarction” or “pulmonary infarction” in stroke CTA reports. We identified 18 patients with our text search. The CTA images were reviewed by two stroke fellows independently. Eight patients were excluded from study as they had pulmonary artery enlargement without PE. Finally, we identified 10 patients from 3,132 unique patients (3,431 scans) and reviewed their charts for history and all diagnostic lab tests. Epidemiological profile, clinical presentation, vascular risk factors, imaging findings, treatment details, outcome and laboratory results were noted. Among investigations, transthoracic echocardiogram with bubble study results were specifically examined for the presence of patent foramen ovale. Admitted stroke patients were managed on the stroke unit at Foothills Hospital where it is part of our standard order set to provide pharmacological DVT prophylaxis with once daily subcutaneous enoxaparin or to use intermittent pneumatic compressions stockings where enoxaparin is contraindicated.
Ten unique cases were identified yielding a period prevalence of PE at 0.32. The mean age was 61.1 (range 25-88) and men to women ratio was 1. Stroke severity varied from National Institutes of Health Stroke Scale 4 to 24. Seven patients had concurrent upper lobe or saddle PE diagnosed at AIS presentation and three had PE diagnosed 2 days after hospital admission. DVT was identified in association with PE and AIS in seven patients. Three patients had a combination of femoral vein and popliteal vein DVT, two had femoral vein DVT only and two had popliteal vein DVT only (Table 1).
Table 1 Baseline characteristics of patients
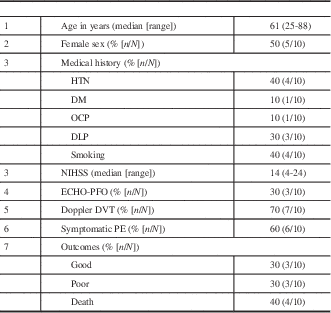
HTN=hypertension; DM=diabetes mellitus; OCP=oral contraceptive pills; DLP=dyslipidemia; NIHSS=National Institutes of Health Stroke Scale range from 0 to 42, with higher scores indicating more severe neurologic deficits; ECHO-PFO=echocardiogram positive for patent foramen ovale; DVT=deep vein thrombosis; PE=pulmonary embolism.
Admission CTA head and neck stroke protocol detected PE in seven patients, whereas CT chest detected PE in the remaining three patients. Five patients had unilateral segmental PE, three patients had bilateral segmental PE, one patient had main pulmonary artery trunk PE and one patient had a saddle PE (Figure 1). Four patients were clinically asymptomatic and six were symptomatic with cardiorespiratory symptoms of PE.

Figure 1 CT angiogram and neck stroke protocol showing patients from this series with (A) saddle pulmonary embolus [PE], (B) segmental PE, and (C) subsegmental PE.
We suspected VTE causing PE and paradoxical embolism via a patent foramen ovale in three patients based upon the quartet of concurrent findings: DVT, PE identified at stroke admission, patent foramen ovale demonstrated on echocardiography and embolic ischemic stroke. Clinically we suspected thrombophilia as an underlying mechanism in four patients but a complete thrombophilia work up was not done in all patients. All patients were treated with intravenous unfractionated heparin except one patient who developed thrombocytopenia and was switched to argatroban. Outcome at discharge was death in four, significant neurological disability in three (modified ranking scale score 4-5) and the remaining three patients had good and independent clinical recovery. The cause of death in two patients was massive PE and malignant middle cerebral artery (MCA) stroke with herniation in two others.
Pulmonary embolism was far less common in this modern series occurring at half the prevalence compared with prior studies.Reference Skaf, Stein, Beemath, Sanchez, Bustamante and Olson 2 From the Registry of the Canadian Stroke Network, Pongmoragot et al.Reference Pongmoragot, Rabinstein, Nilanont, Swartz, Zhou and Saposnik 9 included all AIS patients admitted to participating institutions and among 11,287 patients with AIS, PE was found in 89 (0.78%). Pulmonary embolism was more common among patients with severe stroke, history of cancer, previous DVT/PE. Pulmonary embolism was associated with lower long-term survival, greater disability and longer length of stay. Importantly most PE was detected concurrently at presentation rather than as a consequence of stroke-related hemiplegia, and both symptomatic and asymptomatic PE were identified using the stroke protocol CTA. Modern prevention using both stroke unit care with early mobilization, combined with enoxaparin or intermittent pneumatic compression stockings, is the likely reason for the reduced the rate of PE. Further, the acute treatment of stroke, both medically with thrombolysis and endovascularly, may have resulted in a reduction in the proportion of strokes with high-risk hemiplegia.
Most patients in our series had segmental or subsegmental PE. The clinical implications of these subsegmental PE, which are more likely to be asymptomatic, are unknown. In an analysis of the 383 pulmonary angiograms from the PIOPED study, which included patients with symptomatic presentations, the proportion of subsegmental PE was only 6%.Reference Stein and Henry 10 The greater use of CTA imaging, means that segmental and subsegmental PE can be detected incidentally. Although all patients with a PE diagnosis were treated in our center, there is a lack of consensus on whether this is necessary. The risk of hemorrhage may be higher than the risk of major thromboembolic complications.Reference Perrier, Howarth and Didier 11 , Reference Stein, Goodman, Hull, Dalen and Matta 12 In the setting of concurrent acute stroke, PE resulting in hypoxia can worsen existing cerebral ischemia. Medical thrombolysis (with alteplase using the stroke dosing protocol) may solve both problems, but the subsequent decision to anticoagulate or not requires careful judgment. Heparins are generally not used in stroke because they are associated with a greater risk of major hemorrhageReference Sandercock, Counsell and Kane 13 and withholding heparins in the setting PE may expose the patient to a risk of a major thromboembolic event.
Limitations of our study include the standard CTA technique, which only includes the proximal pulmonary arteries and upper lobes. We may have missed lower lobe pulmonary emboli. Further, the small number of events (PE) identified warrants confirmation in future studies.
Pulmonary embolism is now increasingly rare in AIS. However, it may be a marker of an underlying pro-thrombotic state, can be discovered at presentation with modern imaging, be uncommonly associated with a right-to-left intracardiac or intrapulmonary shunt and portends a poorer prognosis. Further work is needed on therapeutic strategies. Stroke physicians, emergency physicians and radiologists should be aware of and look for PE on stroke protocol CTA studies, concurrently with AIS imaging evaluation.
Statement of Authorship
PVE and MDH reviewed concept and design, drafted the manuscript, and provided critical revision of the manuscript content. DS and SD drafted the manuscript and provided critical revision of the manuscript. All authors read and approved the final manuscript.
Disclosures
The authors have nothing to disclose.




