CLINICIAN’S CAPSULE
What is known about the topic?
Taking photographs and educational videos are common in emergency departments (EDs), but little research exists about patients recording their own procedures.
What did this study ask?
What are patients’ reasons for video recording in the ED and the views of patients and clinicians toward this practice?
What did this study find?
Patients were in favour of ED video recording, whereas clinicians were not. Patients’ reasons and clinicians’ caveats for recording are provided.
Why does this study matter to clinicians?
This study provides a basis for the development of policy concerning video recording by patients in the ED.
INTRODUCTION
Smartphones are now ubiquitous in our society, and, as the technology improves and their use increases and is compounded by the rapid growth of social media,Reference Lyons and Reinisch 1 - Reference Tan, Hu and Brooker 4 it is no longer an uncommon practice for patients and their family members or friends to attempt to capture the patient–physician interaction in the emergency department (ED).Reference Tan, Hu and Brooker 4 - 7 In 2015, almost 73% of Canadians over the age of 18 owned a smartphone 3 ; therefore, it was expected that many patients would indicate that they owned a device capable of recording, which was the case for our study (81.8%). Currently, public policy on video recording in the healthcare setting is governed by provincial legislation and varies across Canada at each hospital or ED. 5 , 8 , 9 Although studies have looked at the use of video recording for educational and quality assurance purposes, as well as the value of recording the patient/clinician interaction in clinical settings,Reference Campbell, Sosa and Rabinovici 10 , Reference Hsieh 11 in our review of the literature, we found no studies quantifying how often patients are recording videos in the ED. We also found no studies detailing why patients want to record videos, or what the attitudes and practices of staff are concerning this practice.
In EDs within the Saskatchewan Health Authority, patients have been allowed to take pictures before, during, or after treatment of their injury, at the discretion of the staff, and as long as no identifying data or faces are included. The request to video record is increasing, which has generated some controversy among staff, who have concerns about patient and staff confidentiality and covert recording.Reference Kwok 12 - Reference Nolan, Ackery and Au 14 With no current policy in place, the purpose of this study was to examine and compare patient and clinician (both physicians’ and nurses’) perspectives regarding patients video recording their own procedures in the ED and to lay the groundwork for further research and policy development regarding video recording and recording, in general, by patients in the ED.
METHODS
Design
Patients and clinicians in the three urban EDs in Saskatoon, Saskatchewan, were asked to complete a short survey about video recording procedures and recording, in general. Based on an informal opinion poll of ED physicians before the study and looking at the statistics, we estimated that 3 to 6 patients would require sutures per day in Saskatoon EDs. Over the course of 4 to 6 weeks, this gave us a target goal of 100 to 200 patients. Patients and clinicians were recruited via a convenience sample of willing and eligible participants.
Patients were recruited to participate by on-shift nurses, physicians, and members of the research team (TO, AD, JS) based upon a triage complaint of laceration, potentially requiring sutures. These recruiters were briefed by the research team to both distribute surveys and direct patients where to deposit the completed surveys (into secure collection boxes behind the triage desk). Patient surveys were consistently distributed to eligible patients before their procedure in the waiting room or in the procedure room at an appropriate time, so as not to interfere with care. Members of the research team (TO, AD, JS) frequented the ED (four to five times per week) to maintain awareness of the study for working physicians and nurses throughout the study period.
Additionally, staff surveys were administered in person or placed in physician and nurse lounges and in physician hospital mailboxes. Secure collection boxes were placed in the staff lounges and behind the triage desk at each site, and these were emptied weekly.
Survey development
An internal focus group met to discuss and develop the survey consisting of both closed and open-ended questions. The questions were then pilot-tested with a small group of patients and clinicians, which resulted in satisfactory responses, prior to full distribution to all study sites. Ethics approval was obtained from the University of Saskatchewan’s Research Ethics Board, and operational approval was obtained from the Saskatoon Health Region prior to data collection. As indicated in the information provided to both patients and staff, consent was implied upon completion of the survey after the respondent read the consent/information sheet.
Inclusion and exclusion criteria
Patients>17 years of age entering any of the Saskatoon EDs with at least one laceration requiring sutures were invited to participate. Patients without the capacity to consent or with life and/or limb-threatening injuries were excluded from the study. ED physicians and nurses were also recruited to participate. Unit clerks, security personnel, and any other non-medical staff were excluded from the study because they are not directly involved in the clinical care of patients.
Data analysis
Descriptive statistics were calculated for age, sex, and profession as well as the dichotomous variables related to experiences with recording and whether recording should be allowed. The chi square test was used to examine differences between groups for categorical variables, substituting the Fisher exact test when more than 20% of expected cell sizes were less than 5. Sufficient data were collected from the open-ended questions to quantify the responses for analysis. All data were analysed using SPSS (v. 23.0).
RESULTS
Over the 2-month collection period, 92.4% (110/119) of patients, 62.7% (37/59) of physicians, and 47.6% (119/250) of nurses responded to the survey. The participant demographics are outlined in Table 1, in addition to some background patient data, which were collected from the survey. Although responses were not directly correlated with the participants’ ages, our results did reveal that 50% of patients were<35 years old, and 75% of patients were<50 years with a mean age of 41 years. Additionally, patients and physicians were predominantly male, whereas nurses were predominantly female.
Table 1 Participant demographics
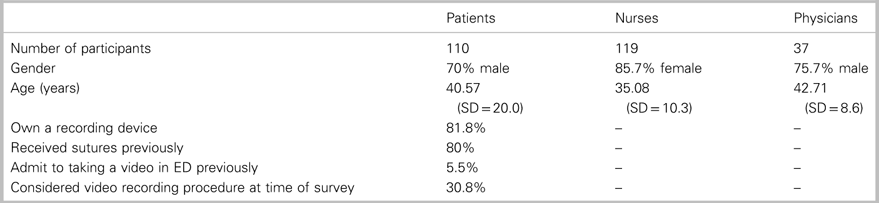
SD=standard deviation.
With regard to video recordings of procedures, 35.3% (42/119) of nurses and 83.8% (31/37) of physicians indicated that, in the past, they had experienced a patient who wanted to record his or her procedure, and 55.9% (19/34) of the physicians and 33.9% (19/56) nurses had allowed that patient to record. Proportionately, 42.9% (15/35) of physicians and 49.5% (51/103) of nurses indicated that if the patient asked to take a video of the procedure, they would allow the patient to do so.
Patients and clinicians were also asked about recording, in general. These results are presented in Table 2. Whereas 61.7% (66/107) of patients were in favour of allowing video recordings by patients in the ED, only 28.1% (41/146) of clinicians were in favour of allowing it (p=0.000). Concerning allowing audio recordings in the ED, 48.6% (51/105) of patients were in favour of it, whereas only 19.0% (28/147) of clinicians were in favour of audio recording (p=0.000). There were no significant differences between nurse and physician responses. There was a statistically significant difference between clinician and patient responses concerning video and audio recordings, but there was no significant difference between the groups for “selfies” (pictures).
Table 2 Proportion of patients and clinicians responding “yes” to recordings in the ED
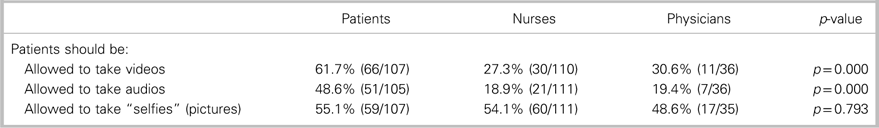
Physicians and nurses were asked: “Why do you think patients would want to video a procedure?” Likewise, patients were asked: “If you were to take a video of the procedure (suturing of your laceration), please explain your reason for doing so (what would you do with the video?).” Responses to these questions were grouped into themes with results presented in Table 3.
Table 3 Proportion of patient and clinician responses concerning reasons for patients taking a video of their procedure
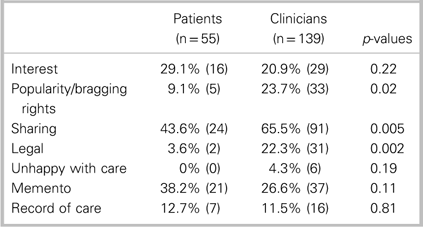
Physicians and nurses were asked: “If a patient asked you whether he or she could take a video of a procedure (i.e., the suturing of a laceration), would you allow it? (yes or no) Why or why not?” The reasons that they provided have been grouped into themes and are presented in Table 4. A more detailed discussion will follow. Note that participants may have had more than one type of comment per question.
Table 4 Proportion of clinicians in favour of allowing or not allowing video recording
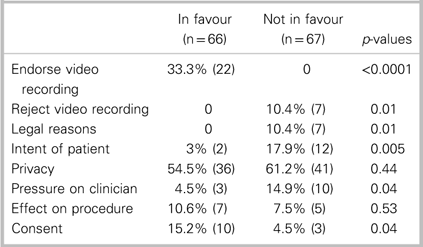
DISCUSSION
Although patient privacy is highly regulated by provincial legislation, much of the burden for privacy is placed on clinicians, leaving patients with relatively few regulations to follow. 5 , 7 , 8 This situation provides patients with greater freedom to record a patient–physician interaction. Current policy on ED video recording within the Saskatchewan Health Authority leaves the decision to record to the physician’s discretion.Reference Lyons and Reinisch 1 , 5 Patient privacy and autonomy serve as primary concerns in healthcare, and therefore, in the ED, the privacy and autonomy of other patients and staff members are also a major issue that must be addressed. Video recording policies must be developed in a hospital-specific manner because this is a highly controversial topic, and opinions and practices vary across the country.
Our study found that patients were more in favour of being allowed to record, regardless of the type of media (video, audio, or “selfies”). This could indicate a lack of awareness on their part of the different adverse outcomes that might arise, 7 in particular, for video and audio recording in the ED setting. Physicians and nurses differed significantly from patients in their support for both video and audio recordings. These clinicians included numerous comments about confidentiality and anonymity related to the lack of privacy in the treatment areas of the ED, which could lead to inadvertent videos or audios of other patients and staff and therefore to violations in patient and staff confidentiality.
Of the physicians that participated in the study, over 80% indicated that they had a patient request to video record in the past. The proportion of clinicians who had received a request was significantly higher for physicians than for nurses, most likely because physicians would have been the recipients of the request as the person performing the procedure. Our survey also revealed that 30.8% of patients self-reported that they had contemplated taking a video of their procedure on the day of the survey.
Most often, responses to the question as to why clinicians would or would not allow recording were caveats and concerns, rather than explicit reasons for or against. Of the 66 clinicians who indicated that they would allow patients to video, only 22 provided statements that gave a reason for endorsing the choice. These were mostly in support of the patients’ right to video their own body or to have a record of care. Of those who were not in favour of allowing patient videos, some simply found it inappropriate, whereas others indicated concerns about legal action and the inability to guarantee the intended use for the video, as well as lack of control over the distribution.
With regard to reasons for recording, patients and clinicians reported with similar frequency: “interest by patient” and “memento keeping and/or record of care,” and both reported “sharing” as a reason, although clinicians at a higher rate. Neither patients nor clinicians indicated that the video recording would result in better patient care. Patients mostly said share with friends and family, whereas clinicians more often specified social media, indicating a heightened awareness of the potential for wider dissemination. At the same time, more clinicians suggested that it may be because the procedure would be seen as novel or “cool” for the patients, and the recording would be shared to boost self-image. In addition, clinicians also suggested that patients might record for potential legal action or as retribution if they were unhappy with care, giving rise to the concerns raised with respect to knowing the patients’ true intent when deciding to permit video recordings.
Both groups, who answered either “yes” or “no” to allowing a patient to take a video, had concerns about privacy and pressure on the clinician, as well as issues related to the procedure. Outright objections included the possibility of recording the faces of staff and patients as well as audio recording of other patients. Others indicated that it was fine with these restrictions: “not my face,” “no faces,” “no audio,” or “no genitals” indicating the need for a policy fully defined in these areas. The concern around audio recording suggests that a policy should not be limited to video recording, because audio recording might occur without the video, and has the potential to be easily conducted covertly. Many clinicians indicated the importance of obtaining consent prior to making a recording. It was unexpected that none would bring up the issue of covert recording; however, it may be that regulating the need for consent might discourage covert recording. Many clinicians indicated the importance of obtaining consent prior to making a recording. Some clinicians did not want to agree to have the procedure videotaped because of performance anxiety. Although some literature has addressed these concerns with learners,Reference Ellis 15 , Reference LaDonna, Hatala and Lingard 16 we have found no research as to the effects of being recorded in the ED. Some clinicians expressed concern that it would be fine if it did not interfere with the procedure; others indicated that agreement would depend on the nature of the procedure.
In keeping with the suggestion that a policy be developed for public and private spaces within the medical setting, 5 , 7 our study revealed the following information (under the premise that a complete ban of video recording is not feasible in a given situation). We believe that it would be most appropriate to develop a policy for private spaces only allowing the video recording of procedures in ED rooms meeting a specific set of criteria – that the room has walls and a closed door, no faces or genitals or confidential personal health information are shown (or heard), the video focuses on the procedure, and the verbal consent of all parties present has been obtained. Video or audio recording of any type in a public space should be prohibited primarily due to the lack of privacy and consent by other individuals who may be shown or heard in the recording.
Further opportunities for research in this area, including the development of a succinct policy on patient video recording in the ED, should further tailor the discussion towards specific conditions that must be met to maintain privacy and confidentiality. This should include addressing the time constraints in the ED, because additional procedures, such as obtaining consent and verifying the content of videos, could add considerable time to a patient’s visit. In addition, patients’ autonomy to video record their own medical procedures as a means of personal documentation must be further examined from a legal standpoint, specifically related to feasibility in a busy ED and consistency between different health regions. With the merging of the province into a single health authority, it needs to be determined whether urban and rural EDs would work under the same policy or would require different procedures. 17 Although it was not addressed in this study, it would be interesting to see whether there were any differences in findings based on gender and age categories. Finally, it would be interesting to explore how patient perspectives may differ concerning “teaching videos” in the ED versus patient-recorded videos.
LIMITATIONS
Sample size
A reasonable sample of clinicians was obtained for this study, but the patient group was limited in size and limited to a specific complaint. Although issues around patient care did not arise as reasons for the video, it may be that inviting participants with a broader array of complaints will contribute to the discussion as to the necessity of recordings and circumstances in which they might be relevant to better care.
Self-reporter bias
Participants self-reported their answers, so there is the potential that participants may not have answered honestly or remembered events correctly. However, the confidential nature of the survey should have dispelled any reasons for participants to fabricate answers.
Location bias
This study was completed in urban EDs. There is the potential that we could see different results in a rural setting. For example, with a smaller community that is less formal, perhaps physicians would be more inclined to allow patients to video or audio record procedures.
Sampling bias
Because our study included a convenience sample of patients and clinicians, the study population may not be completely representative of the entire population. However, our return rate was high enough to compensate for this shortcoming.
CONCLUSION
Although most patients would like to record procedures performed on them, most clinicians do not support this activity in the ED. Because less than half of clinicians would approve, and given the extent of their caveats and concerns, careful consideration must be given to confidentiality and legal issues when developing a policy. Further research should be done to establish a proper policy on video recording in the ED that is relevant to each hospital. Furthermore, national professional organizations like the Canadian Medical Association, Canadian Association of Emergency Physicians, and College of Family Physicians of Canada could develop policies to guide their members. At this time, we recommend that video or audio recording of any type in a public space should be prohibited without privacy and consent by other individuals who may be shown or heard in the recording. Recordings should be allowed only in private spaces in the ED that meet a specific set of criteria: the room has walls and a closed door, no faces or genitals or confidential personal health information are shown (or heard), the video focuses solely on the procedure, and the verbal consent of all parties present has been obtained.
Financial support: Andrew Donauer (medical student) received a scholarship as part of the Dean’s Summer Research Fund at the University of Saskatchewan, College of Medicine.
Competing interests: None declared.






