EXECUTIVE SUMMARY
INTRODUCTION
The Canadian Association of Emergency Physicians (CAEP) recognizes the role of point-of-care ultrasound (POCUS) as a valuable adjunct to the delivery of excellent emergency care. With this document, the CAEP Emergency Ultrasound Committee (EUC) updates the previous CAEP POCUS position statementReference Henneberry, Hanson and Healey1 and provides an expanded framework and series of recommendations, based on the current evidence, to guide emergency departments (ED) and their POCUS programs in the delivery of high quality patient care. Evaluating and summarizing the evidence for the use of POCUS is challenging because, unlike other diagnostic tests where research is primarily focused on test performance, the value of POCUS is further scrutinized in terms of patient-oriented outcomes and system performance measures, such as time to diagnosis or length of stay. Add to this the operator-dependent nature of POCUS, and, not surprisingly, the application of POCUS literature becomes understandably complex.
The recommendations reflect the authors’ synthesis of a combination of test performance metrics, patient-oriented outcomes, and system performance measures (when available). To date, there is still a paucity of prospective POCUS research focused on patient-oriented outcomes, but the authors do believe there is sufficient evidence in the current literature to support the recommendations within this document.
LIST OF RECOMMENDATIONS
The following summary of recommendations is expanded with detailed discussion in the full online version of this position statement.
Scope of practice
The role of POCUS in the practice of emergency medicine (EM) in Canada continues to evolve. The current evidence supports the integration of several potentially life-saving POCUS applications as core skills of the specialty. This list mirrors that of the CAEP EUC's recommended EM Residency emergency ultrasound curriculum.Reference Olszynski, Kim, Chenkin and Rang2
• Focused assessment with sonography for trauma (FAST includes abdominal and thoracic applications.)
• Identification of abdominal aortic aneurysm (AAA)
• Identification of first trimester intrauterine pregnancy (IUP)
• Thoracic ultrasound (including identification of pneumothorax, hemothorax, pleural effusion, and interstitial lung syndrome)
• Focused cardiac ultrasound (including assessment of global cardiac activity, gross left ventricular systolic function, right ventricular size, presence of pericardial effusion, and inferior vena cava calibre)
• Ultrasound-guided vascular access (including peripheral and central vascular access)
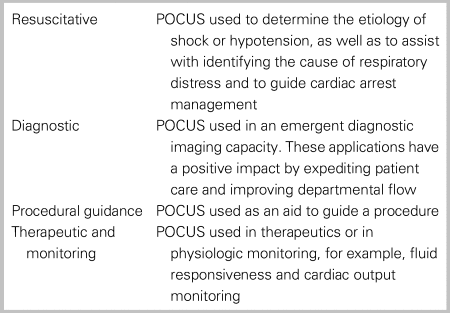
This document adopts the evolving approach of collating applications into the following groups: resuscitative, diagnostic, procedural, and therapeutic/monitoring (Table 1; also see Appendix 1). In addition, a clinical, presentation-based approach is recommended where selected applications are combined, to differentiate a diagnosis.
Table 1. POCUS scope of practice in emergency medicine
Training and competency
Training in POCUS should incorporate a significant amount of experience scanning patients in a clinical setting. Such experience may be supplemented by scanning workshops or training sessions that involve volunteers or POCUS simulation. The key features of this learning phase relate to optimizing the physician's skills in generating optimal images, interpreting the images, and incorporating the images into clinical decision-making.
Recommending methods of training and assessing proficiency in POCUS continue to stimulate debate. The CAEP EUC has published, in collaboration with EM training programs, a series of core POCUS objectives for EM residents and recommends that moving forward, completion of residency provides evidence of competency in these applications.Reference Olszynski, Kim, Chenkin and Rang2 For physicians who did not receive POCUS training during residency, the CAEP EUC recommends that the following three components of training be considered essential when appraising a physician's POCUS credentials and determining corresponding privileges:
1. Clearly defined introduction to the POCUS skill
2. Traineeship with supervision that may include scanning in both the clinical and non-clinical setting. This training phase should maximize exposure to both normal and abnormal findings and should include exposure to a representative sample of model/patient body habitus.
3. A summative assessment of knowledge (including clinical integration and comprehension assessments) and an image generation assessment that includes an observed practical exam
Training for invasive POCUS applications, for example, transvaginal, transesophageal echocardiography, and procedural POCUS, may require a greater reliance on simulation. Incorporating simulation into the training for these applications has been shown to be effective and beneficial.Reference Kneebone, Scott, Darzi and Horrocks3–Reference Fair, Mallin and Mallemat5
Increasingly, non-physician healthcare providers are using POCUS to enhance their clinical practice. Encouraging evidence exists for both emergency medical services (EMS)/prehospital applicationsReference Brun, Bessereau and Levy6–Reference McCallum, Vu, Sweet and Kanji15 and applications used by nurses.Reference Bahl, Pandurangadu, Tucker and Bagan16,Reference Crager, Cinkowski and Gharahbaghian17 It is recommended that POCUS training of these clinicians should include the three components described previously, albeit via a tailored pathway that reflects context and scope of practice.
A growing number of Canadian medical schools have incorporated POCUS into their undergraduate medical education.Reference Steinmetz, Dobrescu, Oleskevich and Lewis18 There is evidence that this can enhance student knowledge and learning of traditional examination skills and also increase student satisfaction.Reference Olszynski, Anderson, Trinder and Domes19 Emergency physicians are well placed and encouraged to facilitate and provide leadership in these programs.
POCUS fellowships are well established in Canada (www.PoCUS.ca), and The Royal College of Physicians and Surgeons of Canada (RCPSC) has recently approved an Area of Focused Competence Diploma.20 Emerging EM POCUS leaders are encouraged to use these programs.
Physicians are expected to keep current with evidence and advances in POCUS practice throughout their careers and are supported by the Canadian colleges in their continuing professional development (CPD) and lifelong learning goals.
Emergency POCUS program management
Emergency POCUS program management includes components of program leadership, monitoring and quality assessment recommendations, as well as machine choice and maintenance. Recommendations are provided to assist EDs in developing POCUS leaders and to help those leaders develop expertise and establish robust programs that will enhance patient care.
All EDs with POCUS equipment should have a named physician (POCUS Lead) designated and responsible for development and maintenance of the emergency POCUS program. In smaller and rural hospitals, this role may be assumed by those with other quality improvement responsibilities (see Appendix 5 for Rural EM recommendations). Academic centres and larger EDs should have a POCUS Program Director. Recommended responsibilities for these positions are detailed in the full document and may include administration, education of trainees and staff, quality, and research. EM POCUS leaders are expected to have completed additional POCUS training and, in academic centres, have completed POCUS fellowships or the equivalent.Reference Olszynski, Kim, Chenkin and Rang2 Regional POCUS leadership is recommended, with regional academic centres and their associated geographically located smaller EDs collaborating with respect to program management.
POCUS program quality is not only dependent on robust training and competency, but also documentation standards, image archiving (where applicable), and defined quality management process. Recommendations for these are detailed in the full document. Many larger and academic EDs in Canada are archiving images and clips for every examination performed. This is considered best practice and strongly recommended. A local POCUS quality program is the responsibility of the POCUS Lead (with the appropriate support and resources) and will include ongoing review, support, education, and development.
A POCUS program requires resources, including physician time and administrative support. Departments are expected to balance the competing demands placed on resource allocation in order to support successful program delivery. Many larger academic centres will already have implemented much of these mentioned. Others will have EM quality programs in place that could be expanded to include POCUS quality. Smaller hospitals will have to consider which of the previous recommendations are achievable locally and what support is available regionally, for example, regional archiving, regional POCUS education, and competency development.
An ultrasound machine must be immediately available to an attending emergency physician in the ED at all times. The CAEP EUC recommends that EDs should have a minimum of at least one machine for every distinct clinical area and strongly consider the provision of one ultrasound machine for every attending emergency physician on shift. Recommended ultrasound machine specifications are detailed in the full document.
Programs should have a clear policy for infection control, that includes machine hygiene (including keyboard, controls, screen, and cart) and the transducers.21–26
Pediatric emergency POCUS
Pediatric emergency medicine (PEM) has embraced the potential of POCUS to improve care for their patients.Reference Vieira, Hsu and Nagler27 Recommended core POCUS competencies for PEM physicians include eFAST, Focused Cardiac, Thoracic, IUP, Soft Tissue, and Vascular Access. Although clinical indications and use of POCUS in adults and children overlap greatly, our recommendations consider the important differences existing between the two populations. These are detailed in the full document and include resuscitation, lung, neck, ocular, renal/bladder, skull fracture, abdomen, testes, hip and fractures.
Training and competency assessment for PEM POCUS applications follows the same recommendations as those outlined in the previous section on training and competency.
Emergency POCUS research
The CAEP EUC would not be able to make these recommendations without the body of evidence provided by quality POCUS research. With a greater focus on outcome-centred research, researchers will need to establish networks to design and run the large-scale multi-centre studies required to answer these important patient outcome questions that remain unanswered.Reference Lewiss, Chan and Sheng28
SUMMARY TABLE
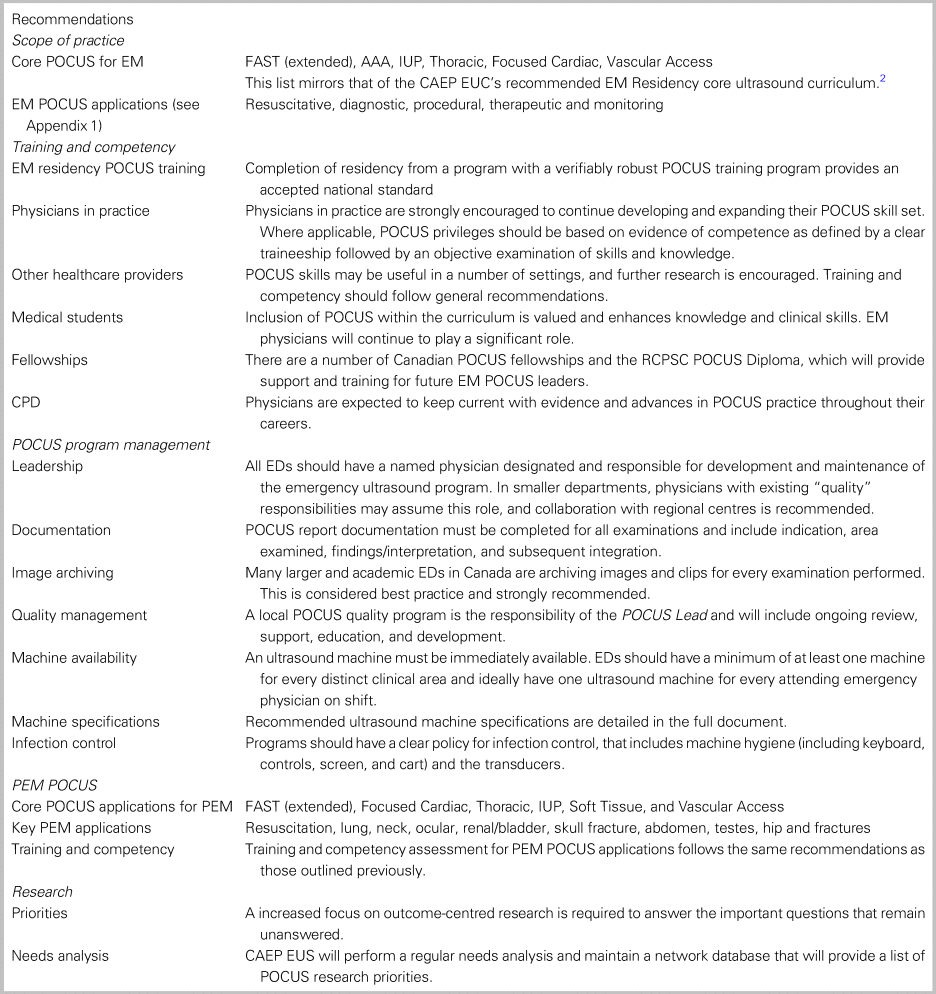
Table 2 shows the recommendation categories and themes. The complete list of recommendations is detailed in the full online document.
Table 2. Summary of recommendation categories and highlighted themes
GOING FORWARD
These recommendations are intended to provide both motivation and support while being adopted by Canadian EDs. It is anticipated that the rate and completeness of adoption will vary depending on department size, leadership, and resources. The CAEP EUC will continue to provide leadership and support towards improving EM POCUS standards and will complete and publish an annual survey to measure adoption of the recommendations.
CONCLUSION
The future of POCUS in EM will be influenced by patient outcomes, research, medical school curricula, and technological advances. Local and national leadership is needed to ensure that future generations of emergency physicians will integrate POCUS seamlessly as part of their everyday practice to the benefit of their patients.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/cem.2019.392
Competing interests
None declared.




