CLINICIAN’S CAPSULE
What is known about the topic?
The prognostic implications of repeated shocks for out-of-hospital cardiac arrest are uncertain.
What did this study ask?
What is the association between the number of prehospital shocks and survival in patients suffering from an out-of-hospital cardiac arrest?
What did this study find?
Survival remains possible even after a high number of shocks for patients suffering from an OHCA.
Why does this study matter to clinicians?
The probabilities presented may prove useful in decision modelling to guide resuscitation efforts for these patients.
INTRODUCTION
Across North America, over 365,000 people suffer a non-traumatic out-of-hospital cardiac arrest (OHCA) each year.Reference Mozaffarian, Benjamin and Go 1 , Reference Gardner, Leather and Teo 2 Rates of survival for these patients remain low, with only 5% to 10% of all OHCA surviving to hospital discharge.Reference Mozaffarian, Benjamin and Go 1 , Reference Cournoyer, Notebaert and Iseppon 3 , Reference Weisfeldt, Sitlani and Ornato 4 However, patients with an initial shockable rhythm, such as ventricular fibrillation and pulseless ventricular tachycardia, have a better prognosis than patients whose initial rhythm is non-shockable (pulseless electrical activity or asystole).Reference Cournoyer, Notebaert and Iseppon 3 , Reference Rea, Cook and Stiell 5 – Reference Meaney, Nadkarni and Kern 7 This may be explained by shockable rhythms being a marker of earlier intervention (i.e., prior to deterioration to asystole) or simply that the single best available therapy for patients suffering from a cardiac arrest (defibrillation) is only effective in patients with these rhythms.Reference Waalewijn, Nijpels, Tijssen and Koster 8 – Reference Link, Berkow and Kudenchuk 12
The efficacy of a single shock to terminate a malignant ventricular arrhythmia is reported to be over 85% when using a biphasic waveform.Reference Morrison, Henry and Ku 9 However, because of refractory (ventricular fibrillation not responding to the initial shocks) or recurrent (returning ventricular fibrillation after a period of non-shockable rhythm) arrhythmias, more than one shock is often required.Reference Jouffroy, Ravasse and Saade 13 – Reference Hasegawa, Abe and Nagata 16 While the patients requiring more shocks may be expected to have worse outcomes, the precise prognostic implications of having a recurrent or refractory malignant arrhythmia remain uncertain, and many medical decisions, such as the timing of patient transport or the decision to cease resuscitation efforts, could be aided by more reliable early survival prognostication. This is especially true in prehospital settings with low rates of prehospital advanced cardiac life support (ACLS) for which this has not been described so far. As such, a better understanding of the implications of the number of shocks delivered could help improve prehospital resuscitation practices.Reference Morrison, Visentin and Kiss 17 , Reference Cournoyer, Notebaert and de Montigny 18
The main objective of this study was therefore to evaluate the association between the number of prehospital shocks delivered and the resuscitation outcomes (survival to discharge and prehospital return of spontaneous circulation [ROSC]) of patients suffering from an OHCA with an initial shockable rhythm, in a prehospital setting with low rates of prehospital ACLS. The secondary objective was to describe the number of shocks delivered in the specific population subgroup of patients having experienced prehospital ROSC.
METHODS
Study design and settings
This cohort study was derived from a registry of all OHCA occurring in the region of Montreal, Canada. It was carried out in association with the Hôpital du Sacré-Coeur de Montréal, the regional emergency medical services (EMS) agency (Urgences-santé) and the Université de Montréal and was approved by the Research Ethics Board of the Hôpital du Sacré-Coeur de Montréal with a waiver of written informed consent.
In Montreal, a single public tiered-response EMS agency coordinates all prehospital care for a population of over 2,000,000 people. First responders and paramedics treat patients suffering from OHCA using an automated external defibrillator when appropriate (ZOLL AED Pro® and ZOLL E series®, respectively, using a sequence of 120 J – 150 J – 200 J) and follow resuscitations protocols based on the American Heart Association guidelines.Reference Kleinman, Brennan and Goldberger 10 , 19 All paramedics can use an esophageal tracheal airway to assist ventilation during the resuscitation. 19 , 20 In up to 25% of OHCA cases, advanced care paramedics are dispatched to provide prehospital ACLS, which includes the administration of epinephrine and amiodarone and the use of the ZOLL E series defibrillator in manual mode.Reference Link, Berkow and Kudenchuk 12 , 20 In accordance with provincial law, advanced care paramedics do not perform endotracheal intubation. All of these defibrillators provide rectilinear biphasic waveform defibrillations.
Methods and measurements
The methods used to collect and extract the data for the initial registry have been described previously.Reference Cournoyer, Notebaert and Iseppon 3 , Reference Cournoyer, Notebaert and de Montigny 18 , Reference Cournoyer, Notebaert and de Montigny 21 Patient data are entered by the paramedic on a “run-sheet” following every call. Patients suffering from an OHCA are identified using these run-sheets. The pertinent information is then entered into a database that comprises demographic and clinical characteristics. Resuscitation outcome data were transferred from the discharge hospitals to the regional EMS agency or were readily available. The extracted data were subsequently validated.
Selection of participants
All patients age 18 years and older treated for an OHCA between April 2010 and December 2015 with an initial shockable rhythm, either ventricular fibrillation or pulseless ventricular tachycardia, were included in the present study. Patients with traumatic causes for arrest, do-not-resuscitate directives, or fitting “obviously dead” criteria (e.g., decapitation, advanced putrefaction) were excluded from both the registry and this analysis. 19
Outcome measures
The primary outcome measure was survival to hospital discharge. The secondary outcome measure was any occurrence of prehospital ROSC of a duration of more than 30 seconds.
Statistical analyses
The entire available population with an initial shockable rhythm was used in this analysis. Continuous variables are presented as means with standard deviations or median and Q1-Q3, as appropriate, and categorical variables are presented as frequencies with percentages.
For the main objective, to ensure that this analysis would be immediately applicable for physicians providing resuscitation care, the relationship between the number of prehospital shocks delivered and the probability of both resuscitation outcomes was first analysed in a way to reflect the dynamic nature of clinical decision-making, such that each level of analysis represents the likelihood of the resuscitation outcome up to that number of shocks (dynamic or Bayesian probabilities). For example, because all patients received at least one shock, the results presented at “1 shock” were derived from the entire cohort (and not from patients having received one shock only). Likewise, at “2 shocks,” all patients having received two shocks or more were kept in the analysis. This analysis can be interpreted as one would a Kaplan-Meier curve. For the alternative analysis, patients were separated in two groups according to the number of prehospital shocks they received: less than three or at least three. This cut-off has been previously proposed to differentiate patients with better and worse prognoses.Reference Holmen, Hollenberg and Claesson 14 Moreover, the shock energy is lower with the first two shocks (120 J and 150 J) compared with all subsequent ones (200 J).
Resuscitation outcomes (survival to hospital discharge and prehospital ROSC) of the patients included in these two groups were compared using Pearson’s chi-square tests. In addition, a multivariable logistic regression model was planned using a standard approach (enter method) adjusting for pertinent variables (i.e., age, sex, initial call time, bystander cardiopulmonary resuscitation [CPR], witnessed arrest, time from call to arrival of EMS personnel, presence of first responders, presence of advanced care paramedics, intubation using an esophageal tracheal airway) to assess the independent association between the number of prehospital shocks administered (used as a continuous variable) and the resuscitation outcomes.Reference Perkins, Jacobs and Nadkarni 22
For the secondary objective (describing the number of shocks necessary for patients having experienced ROSC over the course of their prehospital resuscitation), the appropriate measures of central tendency and dispersion of the number of prehospital shocks administered to that subgroup are presented as described previously. This analysis was necessarily limited to patients having experienced ROSC in the prehospital setting. That subgroup analysis was performed because, by definition, these patients had the potential to respond to treatment they received. The association between the number of prehospital shocks administered and survival to hospital discharge was also evaluated in this same subgroup of patients using the same methods described previously.
Statistical analyses were performed using SPSS Statistics 23 (IBM, Chicago, USA). All results are presented with their 95% confidence intervals (CI).
RESULTS
During the study period (April 1, 2010, to December 31, 2015), among 7,134 patients in the OHCA registry, 1,788 had an initial shockable rhythm and were included. Their demographic and clinical characteristics are presented in (Table 1). Less than a third of the included patients (536, 30%) received treatments from an advanced care paramedic. A total of 977 patients (55%) were administered one or two prehospital shocks, whereas 774 (45%) were administered three or more. Among all included patients, 583 (33% [95% CI 30%-35%]) survived to hospital discharge and 961 (54% [95% CI 51%-56%]) experienced prehospital ROSC (Table 2). Included patients were administered a median number of two shocks (Q1-Q3: 1-5) (see Table 2).
Table 1 Demographic and clinical characteristics of the included patients
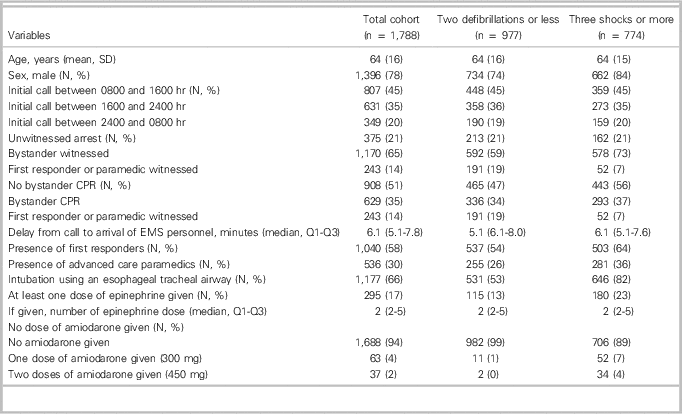
CPR = cardiopulmonary resuscitation; EMS = emergency medical services; SD = standard deviation.
Table 2 Resuscitation outcomes of patients with an initial shockable rhythm

ROSC = return of spontaneous circulation.
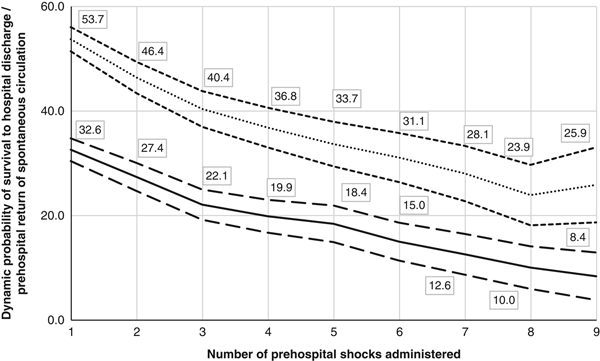
The dynamic probabilities of survival and prehospital ROSC, according to the number of prehospital shocks having already been delivered, irrespective of whether the previous shocks were successful, are presented in (Figure 1. The probability of survival begins at 33% (95% CI 30%-35%) for patients having received at least one shock and gradually lowers to 8% (95% CI 4%-13%) following nine shocks, without a pronounced inflection point. The same is observed for the probability of prehospital ROSC, which begins at 54% (95% CI 51%-56%) and lowers to 24% (95% CI 18%-30%) following nine shocks.

Figure 1 Dynamic probabilities of survival to hospital discharge (full line) and prehospital return of spontaneous circulation (dotted line) with their respective confidence intervals (large dash and small dash) according to the number of prehospital shocks already administered.
Patients having received three shocks or more were less likely to survive to hospital discharge (22% v. 41%, odds ratio [OR]=0.41 [95% CI 0.33-0.50], p<0.001) than their counterparts (see Table 2). They were also less likely to experience prehospital ROSC (40% v. 64%, OR=0.38 [95% CI 0.31-0.46], p<0.001) (see Table 2). In multivariable logistic regression models, the number of prehospital shocks received was independently associated with lower odds of survival (adjusted OR [AOR]=0.88 [95% CI 0.85-0.92], p<0.001; Hosmer-Lemeshow goodness of fit test: p=0.28; c-statistic=0.81) and with lower odds of prehospital ROSC (AOR=0.85 [95% CI 0.82-0.88], p<0.001; Hosmer-Lemeshow goodness of fit test: p=0.35; c-statistic=0.80) (Table 3 and Appendix 1 [online]).
Table 3 Multivariate analysis for the survival to hospital discharge outcome, adjusted for the number of shocks, demographic, and prehospital variables

AOR = adjusted odds ratio; CI = confidence interval; CPR = cardiopulmonary resuscitation.
* Reference category.
† Not calculated due to collinearity.
Among the 961 patients who experienced prehospital ROSC, 556 (58% [95% CI 55%-61%]) survived to hospital discharge and 320 (33%) received three prehospital shocks or more (see Table 3). The median number of prehospital shocks they received was 2 [Q1-Q3: 1-3] (see Table 3). Among patients who experienced prehospital ROSC, patients having received three prehospital shocks or more were also less likely to survive to hospital discharge (50% v. 62%, OR=0.62 [95% CI 0.47-0.81], p<0.001) than their counterparts (Appendix 2 [online]). In a multivariable logistic regression model, the number of prehospital shocks administered was independently associated with poorer survival to hospital discharge (AOR 0.95 [95% CI 0.89-1.00], p=0.045).
DISCUSSION
In this large cohort of OHCA presenting with a shockable initial rhythm, the number of shocks was independently associated with lower rates of prehospital ROSC and survival to hospital discharge. Moreover, although outcomes were significantly worse with more shocks, no clear inflection point in the dynamic probabilities could be identified. These probabilities presented may well prove useful in decision modelling to guide resuscitation efforts, especially for settings with low rates of prehospital ACLS for which this had not been described so far.
In the present study, it was observed that the probability of survival to discharge in patients with an initial shockable rhythm diminishes gradually with the number of defibrillation attempts from 33% at the first to 8% at the ninth. Similarly, the probability of prehospital ROSC diminishes gradually from 54% to 26% after nine defibrillations. Interestingly, these results are similar to the ones observed by Holmen et al. for the survival outcome (1-3 shocks=42.9% and >10 shocks=7.5%), despite differences in prehospital care between the studies.Reference Holmen, Hollenberg and Claesson 14 Indeed, most patients received ACLS interventions in Holmen’s study (73% received epinephrine), whereas the majority did not in the present study (17% received epinephrine). This observation would seem to corroborate the finding that prehospital ACLS does not appear to increase the medium-term outcomes of patients suffering from OHCA, even for patients with a shockable rhythm.Reference Cournoyer, Notebaert and Iseppon 3 , Reference Holmen, Hollenberg and Claesson 14 , Reference Stiell, Wells and Field 23 , Reference Kudenchuk, Brown and Daya 24 On the other hand, Jouffroy et al. observed higher probabilities of prehospital ROSC than in the present study, perhaps explained by on-site prehospital ACLS provided by a specialized physician in that study.Reference Jouffroy, Ravasse and Saade 13 Although not clearly associated with improved survival to hospital discharge, ACLS interventions (e.g., vasopressors and antiarrhythmics) have been shown to increase the rate of ROSC.Reference Cournoyer, Notebaert and Iseppon 3 , Reference Stiell, Wells and Field 23 , Reference Olasveengen, Sunde and Brunborg 25 On the other hand, Hasegawa et al. observed a slightly higher survival in their cohort compared to the present one, but only included patients with a witnessed collapse who are known to have a better prognosis.Reference Rea, Cook and Stiell 5 , Reference Hasegawa, Abe and Nagata 16 While these studies presented outcomes for patients having received a selected number of shocks, the present study is the only one to present probabilities that are easily usable by providers during the resuscitation.
In the current study, no clear inflection point could be observed in the dynamic probabilities of survival. On the contrary, in the studies of Hasegawa and Jouffroy, cut-offs of three and four shocks were proposed to predict survival and prehospital ROSC.Reference Jouffroy, Ravasse and Saade 13 , Reference Hasegawa, Abe and Nagata 16 The absence of an obvious inflection point indicates that the arbitrary use of a specific cut-off is probably not sufficiently sensitive or specific to allow them to be used independently of other factors in clinical decision-making.
The present results further our understanding of the prognostic implications of multiple shocks. One possible interpretation of this analysis is that all patients with an initial shockable rhythm, even those where a large number of shocks was administered, have a chance of survival well over the often suggested threshold of medical futility in resuscitation.Reference Morrison, Visentin and Kiss 17 Indeed, survival nearing 10% is likely sufficient to conclude that such patients not be considered for prehospital termination-of-resuscitation.Reference Holmen, Hollenberg and Claesson 14 , Reference Morrison, Visentin and Kiss 17 , Reference Group 26
The observation that more shocks are associated with worse resuscitation outcomes is likely explained by two factors. Firstly, requiring more shocks implies a longer period of CPR, which is strongly associated with the resuscitation outcomes.Reference Goto, Funada and Goto 27 In addition, the patients responding more rapidly to a shock might have a less severe underlying disease (e.g., infarct size, genetic predisposition) or a shorter delay before its treatment.Reference De Maio, Stiell, Wells and Spaite 28 – Reference Aouizerat, Vittinghoff and Musone 30 Nevertheless, it bears noting that a third of the patients who experienced ROSC required three shocks or more.
Another important interpretation of this analysis is that it might be critical to ensure the efficiency of first shocks. The best way to improve first-shock success is most likely to reduce the delay between circulatory collapse and the initial defibrillation attempt, which likely implies both optimizing the prehospital organization of care services and increasing public access to automated external defibrillators.Reference Stiell, Wells and Field 31 – Reference Briard, de Montigny and Ross 33 Increasing the energy of initial shocks has also been proposed as a way to improve their efficiency, but evidence is lacking so far to support such a practice.Reference Morrison, Henry and Ku 9 , Reference Anantharaman, Tay and Manning 34 , Reference Emmerson, Whitbread and Fothergill 35 Whether adding a short acting beta-blocker to the pharmaceutical cocktail that these patients receive early in resuscitation efforts or attempting a double sequential defibrillation remains a promising avenue for future research.Reference Driver, Debaty, Plummer and Smith 36 – Reference Hajjar, Berbari and El Tawil 38
LIMITATIONS
By design, all patient data were derived from information available in the EMS patient record. As such, it was not possible to know whether multiple shocks were administered because of a refractory versus a recurrent arrhythmia. It is possible that patients suffering from a recurrent arrhythmia would have a better prognosis than patients suffering from a refractory arrhythmia and, consequently, that these two populations’ dynamic probabilities of survival differ. It was also not possible to know whether some patients had received defibrillation attempts from a public-access defibrillator prior to the arrival of emergency responders. Having these data available could have flattened the dynamic probabilities curve even more and increased the difference observed between groups. Neurologic outcomes were unavailable in this study. It would have been interesting to evaluate these outcomes because patients with a high number of shocks might be at a higher risk of brain ischemia and of poor neurologic outcomes than the majority of patients surviving from an OHCA. Given the nature of the prehospital system in the Montreal region, only a minority of patients received antiarrhythmic medications. Although these have never been shown to increase the long-term survival of patients with OHCA, they do increase the rate of ROSC and could also influence the rate of recurring or refractory arrhythmias (and consequently shocks), which could make the present results less generalizable in settings with high rates of prehospital ACLS.Reference Kudenchuk, Brown and Daya 24 Additionally, although this study included a large and comprehensive multicentre data set of OHCA, caution would be recommended in extrapolating these results to regions with differences in the geographic parameters, availability of advanced care services, treatment standards, or patient demographics.
CONCLUSIONS
Survival remains possible even after a high number of shocks for patients suffering from an OHCA with an initial shockable rhythm. In a prehospital setting with low rates of prehospital ACLS, the probability of survival to hospital discharge for these patients diminishes gradually with the number of defibrillation attempts from 33% to 8% after nine shocks have been administered. There does not seem to be an evident inflection point in the probabilities of survival that would predict bad resuscitation outcomes, and the number of shocks received should not influence treatment decisions alone. Requiring more shocks is independently associated with worst outcomes in that population. Future studies should describe the dynamic probabilities of good neurologic outcomes of two specific subgroups of patients requiring multiple shocks, patients with a refractory arrhythmia, and patients with a recurrent arrhythmia.
Financial support: This project received funding from the “Département de médecine familiale et de médecine d'urgence de l'Université de Montréal” and the “Fonds des urgentistes de l'Hôpital du Sacré-Coeur de Montréal.”
Competing interests: Dr. André Denault is part of a speakers bureau for Medtronic, Edwards, Masimo, and CAE Healthcare. All other authors have no conflict of interest to declare.
SUPPLEMENTARY MATERIAL
To view supplementary material for this article, please visit https://doi.org/10.1017/cem.2018.437