CLINICIAN'S CAPSULE
What is known about the topic?
Feedback on the quality of cardiopulmonary resuscitation (CPR) during cardiac arrest is a critical component for the delivery of high-quality CPR.
What did this study ask?
How are Canadian emergency physicians assessing the quality of CPR, and what are barriers to implementation of feedback devices?
What did this study find?
CPR quality is frequently assessed using inaccurate methods, and only a minority of clinicians use feedback technology because of a lack of availability.
Why does this study matter to clinicians?
Clinicians should recognize inaccurate methods of assessing CPR quality and implement more objective methods such as feedback devices to improve resuscitation care.
BACKGROUND
In Canada, approximately 40,000 cardiac arrests occur annually.1 The survival rate is variable, ranging from 3%–35%.Reference Meaney, Bobrow and Mancini2 High-quality cardiopulmonary resuscitation (HQ-CPR) is an essential skill and has been shown to improve survival.Reference Hostler, Everson-Stewart and Rea3 Despite this, studies show that health care providers struggle to provide guideline-compliant CPR during cardiac arrests.Reference Meaney, Bobrow and Mancini2 CPR feedback devices have provided a means of delivering objective feedback on the quality of chest compressions during cardiac arrest.Reference Meaney, Bobrow and Mancini2 Improved CPR performance through the use of devices in training and clinical care have the potential to improve patient outcomes.Reference Meaney, Bobrow and Mancini2,Reference Hostler, Everson-Stewart and Rea3 Currently, it is unclear how emergency physicians (EPs) are assessing chest compression quality and if feedback devices are being utilized. In this study, we aimed to describe current practices of monitoring CPR quality during cardiac arrest, to determine if Canadian EPs are using CPR feedback devices, and to identify eventual barriers to their implementation.
METHODS
Study design
We conducted a national survey to determine current practices of assessing CPR quality during cardiac arrests in the emergency department (ED). Ethics approval was obtained from the University of Calgary Conjoint Health Research Ethics Board. Consent was implied upon participation in the survey.
Study setting and population
In this cross-sectional study, an online survey was administered to physician members of the Canadian Association of Emergency Physicians (CAEP) over a six-week period between September and October 2016. Three emails were sent at two-week intervals to all participants to serve as reminders for survey completion. Pediatric EPs were excluded. The denominator of EPs at the time of distribution was 1,735.
Survey content
After a literature review, survey questions were developed that targeted our objectives. The majority of questions were multiple choice with an option for comments. Pilot testing of the survey was conducted in an independent group of EPs to ensure the clarity of questions and were modified accordingly. Pilot survey data were excluded. SurveyMonkey™ was utilized for distribution and data collection.
Statistical analysis
Data were exported to Microsoft Excel (2018, Version 16.23). Responses were summarized and analyzed using descriptive statistics.
RESULTS
The total response rate was 19% (323/1,735). The survey was sent to 1,743 recipients with eight email bounce backs and eight mistakenly sent to registered nurses who were excluded, making 323 the final number of surveys analyzed. The majority of respondents were geographically located in Ontario (43.3%), Quebec (12.2%), and British Columbia (12.9%). See Table 1 for respondent characteristics.
Table 1. Respondent characteristics.
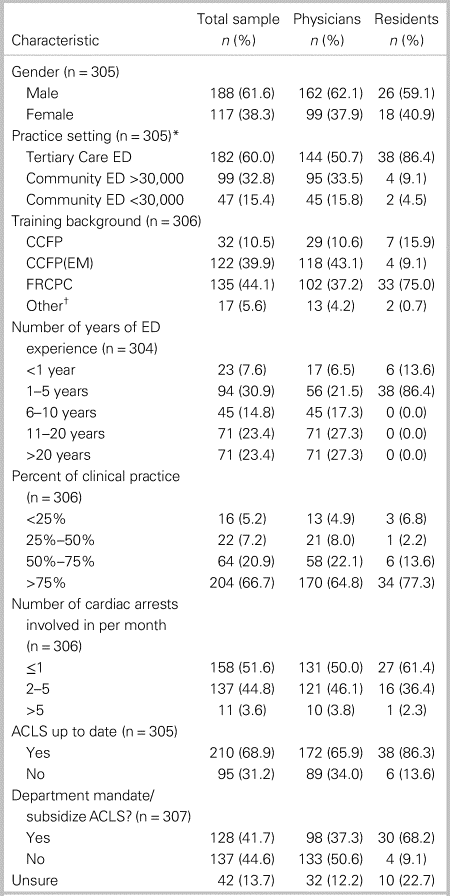
ACLS = Advanced Cardiovascular Life Support; CCFP = Canadian College of Family Physicians; CCFP(EM) = Canadian College of Family Physicians Emergency Medicine; ED = Emergency Department; FRCPC = Fellow of the Royal College of Physicians of Canada.
*Some respondents worked at multiple practice settings. Respondents may have also skipped various questions, which is why n is variable for different characteristics.
†Critical care, FACEP (Fellow of the American College of EM), ABEM (American Board of EM), CSPQ (Certificat de Spécialiste de la Province de Québec), FRCPC-other, MD, R2, Surgical internship, pre-specialty era (1983).
Of note: Total number of residents numbered 44. For this question, a few respondents typed in family medicine resident but skipped previous question of PGY resident status, which is why the total number is different.
Current state of CPR assessment
Physician team leaders were most commonly responsible for evaluating CPR quality (310/465). A second physician (55/465) or a bedside nurse (61/465) also evaluated CPR quality (55/465). Rarely, a respiratory therapist was responsible for CPR assessment (27/465). Only 12.1% (38/315) of those surveyed use feedback devices to assess CPR quality. Visual assessment (41.2%; 133/323) and pulse check (29.7%; 96/323) were the most common methods of assessing CPR quality (see online supplementary materials, eFigure 1). Regarding ventilation (38.3%; 118/308) were observed for rate and volume, with 58.8% (188/320) using direct visual observation.
When the team leader oversaw the CPR quality assessment, most, 67.4% (217/322), stood at the foot of the bed, 25.8% (83/322) preferred the side, and 5.0% (16/322) preferred the head of the bed.
Opinions on feedback devices
The majority of those surveyed (72.3%; 227/314) believed that feedback devices are needed as part of care in the ED. A minority (12.1%; 38/315) utilized CPR feedback devices as part of clinical practice.
Perceived barriers to feedback devices
Multiple reasons were identified as to why respondents did not utilize CPR feedback devices (see online supplementary materials, eFigure 2). If resources/funding were readily available, 87.2% (273/313) of respondents said they would use them. When asked to explain why they would not use feedback devices, even if available, 40.4% (17/42) mentioned a lack of evidence, and 28.6% (12/42) did not think there was an added benefit to the interventions they already provide.
DISCUSSION
The 2015 Heart and Stroke Foundation of Canada resuscitation guidelines recognize audiovisual feedback devices as a tool that may be used for optimization of CPR performance.4 Use of feedback devices has demonstrated improvement in CPR quality for both in- and out-of-hospital cardiac arrest.Reference Hostler, Everson-Stewart and Rea3 Evidence suggests that increasing chest compression depth is a predictor of achieving return of circulation (ROSC) and improved short term survival.Reference Talikowska, Tohira and Finn5 Observational studies utilizing porcine models have shown an association between feedback-directed chest compressions and survival.Reference Chopra, Wong, Ziegler and Morrison6 However, survival benefit in humans attributed to the use of feedback devices remains inconclusive.Reference Hostler, Everson-Stewart and Rea3,Reference Kirkbright, Finn and Tohira7
Our survey found that most respondents assess quality of CPR by visual assessment. A study of health care providers found that the overall accuracy of visually assessing CPR quality was 65.6%.Reference Jones, Lin, Nettel-Aguirre, Gilfoyle and Cheng8 Accuracy improved when viewed from the side (70.8%) compared with the usual foot of the bed (68.8%).Reference Jones, Lin, Nettel-Aguirre, Gilfoyle and Cheng8 Another study found a large discrepancy if comparing visual assessment of CPR quality with objective data collected by manikins.Reference Gonzalez, Martinez and Cerda9 To optimize the accuracy of assessment, it may also be beneficial to delegate a “CPR coach” who assesses compressions from the side of the bed.
The second preferred way to assess CPR quality was real-time pulse check. The United Kingdom Resuscitation Council recommends against using carotid or femoral pulses to evaluate the quality of chest compressions.Reference Gwinnutt, Davies and Soar10 A pulse found in the femoral region may be of venous origin rather than arterial.Reference Connick and Berg11 Our survey demonstrates a common practice that is inaccurate, highlighting a need for further education and better use of tools to give more accurate feedback on CPR quality.
Aside from feedback devices, end-tidal CO2 (ETCO2) monitoring was one of the least common methods of monitoring CPR quality in our study. Studies have shown an association between ETCO2 levels and outcome, particularly in the first 20 minutes. High levels (>20 mm Hg) are associated with increased survival, and very low levels (<10 mm Hg) are associated with increased mortality.4 Factors such as initial rhythm, bystander CPR, duration of arrest, and use of bicarbonate influence ETCO2 values, confounding the interpretation of capnography during CPR. Guidelines recommend a titration of CPR performance to a goal of >20 mm Hg. However, the relationship among ETCO2, compression depth, rate, and fraction is unclear.Reference Meaney, Bobrow and Mancini2,Reference Chopra, Wong, Ziegler and Morrison6
Identified barriers
One of the main barriers was the lack of availability of feedback devices and resultant unfamiliarity with its clinical use. The common theme underpinning this barrier seems to be the perceived lack of benefit and adequacy of current care.
Limitations
Our study had several limitations. Our response rate was 19% that limits our ability to accurately describe current practice. We surveyed CAEP members, so we might have missed a large proportion of EPs in Canada. Additionally, the practice described cannot be translated outside the ED. There might also have been a clustering effect in which individuals in certain institutions or provinces practice similarly. There is potential for sampling bias as ED physicians interested in this topic or those who hold strong views for or against feedback devices might have been overrepresented. It is also possible that the design of our survey might have influenced how participants responded.
CONCLUSION
Among the Canadian EPs who responded to our survey, only a minority use feedback devices to assess quality of CPR during cardiac arrest. The majority of respondents assess quality of CPR by standing at the foot of the bed and utilize visual assessment and palpation methods that are notoriously inaccurate. The primary barrier to feedback device use was the unavailability in the ED.
SUPPLEMENTARY MATERIAL
The supplementary material for this article can be found at https://doi.org/10.1017/cem.2019.382
Competing interests
The authors have nothing to disclaim. There are no conflicts of interest. This research received no specific grant from any funding agency, commercial, or not-for-profit sectors.



