INTRODUCTION
Both experts and patients agree that our health care delivery system has many opportunities for improvement.1–Reference Gandhi5 In recent health care system performance rankings by the Commonwealth Fund, Canada ranks ninth overall among 11 high-income countries.Reference Schneider, Sarnak, Squires, Shah and Doty6 In another study, 60% of Canadians reported that fundamental changes were needed in our health care system, and only 28% were “very confident” that they would receive high-quality care.Reference Schoen, Osborn, Doty, Bishop, Peugh and Murukutla7
The suboptimal performance of our current system is multifactorial.Reference Stange8 It is our role, as emergency physicians (EPs) at the intersection of the community and hospitals and of general and specialized care, to see these issues as opportunities for improvement. The burgeoning field of quality improvement and patient safety (QIPS) has had a growing impact on health care institutions in our country since the publication of the Institute of Medicine (IOM) reports almost two decades ago.Reference Kohn, Corrigan and Donaldson9,10 With its focus on smaller-scale iterative design, QIPS may be the most viable philosophy and science at our disposal to improve care delivery in our health system.
However, for EPs to improve care within their emergency departments (EDs) and hospitals, emergency medicine (EM) leaders and departments need to invest in QIPS as a framework. We are unaware of any national bodies that have provided recommendations to improve the system capacity to conduct QIPS work in the ED. The objectives of this 2018 CAEP Academic Symposium panel are to address this gap by:
• Identifying the barriers, facilitators and the current Canadian context for the pursuit of QIPS projects in the ED setting through a national survey and literature review.
• Providing guidance on the development of ED capacity aimed at supporting and leading interdepartmental QIPS projects, through best-practice recommendations on how to build a local QIPS program.
• Providing a collection of relevant resources available for ED clinicians interested in QIPS.
METHODOLOGY
Expert panel process
We formed an expert panel, which included nine EPs and one EM resident affiliated with six different Canadian medical schools. The expert panel members were explicitly selected based on their expertise, roles in QIPS, and geographic representation. They ranged in leadership roles from front-line clinicians to heads of quality programs, research program, and departments.
The panel developed a draft of a list of recommendations based on their academic expertise and professional experience, which was iteratively improved through a scoping review of the topic. Subsequently, the panel communicated with 14 of their personal contacts who are national experts on QIPS, for their commentary on the list. These included medico-legal experts, hospital executives, and EM academic leaders. Based on their feedback and through seven monthly teleconference meetings, the list was refined. The literature was then reviewed to confirm, support, and exemplify the recommendations.
Environmental scan of Canadian QIPS activities
As part of our preparatory work, we conducted a national survey of university EM department chairs, major academic hospital ED chiefs, and QIPS leads at all 17 Canadian university-affiliated academic centres. The objective was to better understand the operational and academic environments in which QIPS activities are taking place, and the full results have been published concurrently with this article in CJEM.Reference Kwok, Perry, Mondoux and Chartier11 It found significant local educational and academic efforts for QIPS in Canadian EM, with a discrepancy between the level of formal support/infrastructure and the output of such activities.Reference Kwok, Perry, Mondoux and Chartier11
CAEP 2018 Academic Symposium process
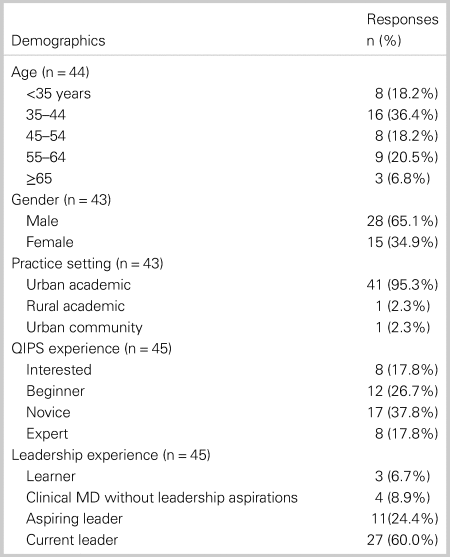
The results of the national survey and draft recommendations were presented at the 2018 CAEP Academic Symposium on May 26, 2018, in Calgary, AB, to an audience of 82 members. The panel used a four-prong technique to elicit feedback on the list of recommendations: 1) paper-based lists distributed to the Symposium attendees for written feedback; 2) verbal discussion between the panel and attendees; 3) Twitter comments/polls for those not on-site; and 4) an innovative crowd-sourcing platform called PollEverywhere® (San Francisco, CA, USA). Through this platform, the panel was able to collect the audience's demographics, their votes on each of the recommendations (i.e., accept, modify, and reject), and comments submitted on their smartphone or computer that were projected in real-time on the room's main screen. This allowed for semi-quantitative and qualitative feedback that supported the discussions at the Symposium and informed this paper. Table 1 shows a summary of the self-reported demographics of the 45 (54.9%) attendees who replied to the survey in real-time.
Table 1. Self-reported demographics of responding attendees from Panel 1 on QIPS at the 2018 CAEP Academic Symposium on Leadership
RECOMMENDATIONS
As a provider or leader interested in developing a local EM-based QIPS program, the following steps are recommended to increase the feasibility and sustainability of initiatives that will lead to improved patient care (Table 2).
Table 2. Recommendations from Panel 1 on QIPS of the 2018 CAEP Academic Symposium on Leadership

Recommendation 1. Use patient or provider stories to create urgency and engagement for a culture of improvement
Effective change management through QIPS requires building a platform that will engage individuals and enable the procurement of necessary resources. This case for system-level change may be built through seminal literature,Reference Kohn, Corrigan and Donaldson9,10 local patient/provider stories or broader goal setting by inspiring leaders.Reference Reinertsen, Bisognano and Pugh12 Breakthrough performance goals, as well as local aim and vision, are required to improve system-level performance and execute QIPS projects.Reference Nolan13–Reference Boyle, Cleugh and Long15 One key success factor to achieve these is engaging physicians, providers, and administrators in a common purpose, as they are more likely to support change when they understand the “why” behind the movement.Reference Reinertsen, Bisognano and Pugh12,Reference Reinertsen, Gosfield, Rupp and Whittington16 Over time, a platform for quality at a system and local level will enable improvement and shift to an organizational culture of improvement.
Recommendation 2. Engage all relevant stakeholders for the coordination of QIPS work, which may include institutional, departmental, university, and regional leadership, as well as patients
Specific stakeholders and support will vary depending on the institution, but they should typically include ED leadership and senior hospital leaders such as chairs of the institutional quality/safety committee or affiliated university academic leaders, as well as patients.Reference DeWalt, Powell and Mainwaring17,18 Reciprocally, members of the ED QIPS team may seek membership on hospital or university-wide QIPS committees to ensure communication and alignment and to enable collaboration. Although the support from the various stakeholders would ideally include financial resources and should be confirmed in writing, other goals may include support through administrative access to hospital resources (e.g., data analyst and QIPS experts).
Recommendation 3. Create a formal ED QIPS committee with goals, terms of references, and clearly defined roles and responsibilities
The creation of a diverse ED QIPS committee (ideally co-led by a physician and non-physician) supports successful and sustainable QIPS initiatives in the clinical setting. The terms of reference, responsibilities and goals, should support the vision previously determined with the relevant stakeholders.Reference DeWalt, Powell and Mainwaring17 Having a physician champion is crucial for the engagement of other physicians in the development of new QIPS initiatives, and the same holds true for nursing and interprofessional leadership.19 Regularly planned meetings (e.g., monthly or quarterly) and a clear reporting structure will increase accountability, alignment, opportunities, and momentum for the committee.20 Three-way communication focused on project progression between the QIPS committee, the front-line providers interested in participating in projects, and the leadership team (both ED and hospital-wide) is essential. The ultimate goal is to have the QIPS committee serve as a vector to align the workforce and leaders on projects and priorities, as opposed to being tasked with the conduct of all aspects of improvement and operations of the ED.
Recommendation 4. Secure funding, resources, and protected time required to enable successful ongoing QIPS work
A comprehensive literature review of local contextual factors found that funding, general resources, and time were most positively associated with QIPS success,Reference Kaplan, Brady and Dritz21 and workload was most negatively related to successful implementation.Reference Alexander and Hearld22 Funding alone is, therefore, not sufficient for QIPS success, and resources and time also play an important role.Reference Kaplan, Froehle, Cassedy, Provost and Margolis23 These findings highlight the importance of protected time for front-line caregivers to perform meaningful QIPS work. They also emphasize the importance of access to resources that could include access to individuals with QIPS methodological expertise, administrative support, project management, and data and analytics support. Without access to these crucial elements of successful project design, implementation, and evaluation, it may be unreasonable to expect success. Depending on the size of the ED and the scope of the QIPS projects, these resources could be supported and shared across departments, hospitals, or the university.
Recommendation 5. Local data must be available to identify and prioritize opportunities for improvement, guide project selection and design, and track improvements
System-level metrics and data are necessary for system improvements, with regular feedback loops being an essential component.Reference Reinertsen, Bisognano and Pugh12 Access to local and timely data in some form is important to all QIPS initiatives.24 Preliminary and historical data (e.g., patient safety incident reports) are useful to understand root causes and the magnitude of adverse events, set improvement goals, and benchmark against peers.24–Reference Farbstein and Clough26 While near real-time updates and accepted benchmarks help the most, in many settings, these data may not be available. Leaders should then facilitate QIPS team members to have access to organizational resources such as decision support services or information technology to query existing databases with new questions. If there is no database to query, QIPS team members can be empowered and supported to collect their own data through direct observation or chart review, even if the sample size is small.27 As QIPS efforts move forward, prospective purposeful data collection enables measuring the effect of any intervention.Reference Boyle, Cleugh and Long15,Reference Varkey, Reller and Resar28–Reference Johnstone, Hendrickson and Dernbach30
Recommendation 6. Encourage, support, and recognize training in QIPS methodologies for EM physicians and all health care providers including support staff
QIPS team skills have been identified as an important contextual factor in QIPS success.Reference Kaplan, Froehle, Cassedy, Provost and Margolis23 The importance of training in QIPS is underscored by the prominence of quality and safety competencies and milestones in CanMEDS 2015.Reference Frank, Snell and Sherbino31 To build a successful QIPS program, EDs should focus on:
1. Encouraging a minimum QIPS literacy requirement for physicians to ensure commitment to system improvements and capacity for project involvement;
2. Providing QIPS continuous professional development (CPD) opportunities and training sessions for nurses, allied health providers, and trainees to support interdisciplinary teams; and
3. Providing and supporting enhanced QIPS learning opportunities for individuals who are interested in leading QIPS projects, including nurturing mentorship relationships.
Numerous approaches and levels of QIPS training have been developed in recent years, ranging from the basic online modules to graduate-level experiential degrees and including a variety of certificates, practical opportunities, and workshops.Reference Mondoux, Chan, Ankel and Sklar32 We developed a comprehensive list of QIPS educational opportunities and resources, available online on CAEP's website at https://caep.ca/qips-resources/.
Recommendation 7. Interprofessional, cross-departmental, and patient collaboration is vital for the design of broad-based projects to ensure engagement of stakeholders
Most QIPS projects affect multiple stakeholders including patients and providers from other departments.19 Various tools can be used for “stakeholder mapping,” which allows a deeper understanding of the project contributors’ expected involvement based on power and interest.Reference Chartier, Cheng, Stang and Vaillancourt33,Reference Bryson34 Additionally, a challenging, but important, facet of QIPS projects is the involvement of patients and families, when feasible. This is done to align the work with the expectations of those who arguably matter most, to ensure their perspectives and values are incorporated. Increasingly, approaches and toolkits are being developed to facilitate this important part of QIPS projects and bring the patients’ voice to the table.35 Finally, obtaining the support of an executive sponsor, who will openly support and promote the project, open doors, and facilitate buy-in, is crucial to the success of QIPS projects.Reference Rotteau, Webster and Salkeld36
Recommendation 8. Use an established QIPS framework and adapt interventions to your local context
The systematic use of an improvement framework or methodology is essential to improve systems reliably rather than individual providers’ variable behaviours.Reference Lynn, Baily and Bottrell37–Reference Berwick39 The Model for Improvement, Plan-Do-Study-Act (PDSA) cycles, SMART aim statements, Six Sigma, Toyota Production System/Lean Production, and Root cause analysis are common examples of methodologies utilized in health care today.Reference Boyle, Cleugh and Long15,24 Given that all methodologies share common features (e.g., goal setting, systematic observation and analysis, rapid cycle improvement, and iterative measurement), ED leaders creating a new QIPS program should likely start by training a core group on one methodology and spread the chosen methodology through their group. Over time, expanding the methodological repertoire to enable different approaches to different problems will likely increase the success rate of QIPS initiatives.
Recommendation 9. Encourage reward mechanisms and incentive structures that align with the goals of the program team members
The sustainability planning of projects and programs is an oft-forgotten, but crucially important, factor to ensure the continuous engagement of providers in system improvements.Reference Chartier, Vaillancourt, Cheng and Stang40,Reference Ham, Kipping and McLeod41 The development of reward mechanisms and incentives structures are an important element to achieve continuing engagement and sustainability, but they must be developed by the local stakeholders based on their “needs” and “wants” while being feasible within the local environment.Reference Scoville, Little, Rakover, Luther and Mate42
Although financial incentives are easily conceptualized and more tangible benefits to participation, they are challenging in the current resource-constrained environment of health care. Instead, in academic medical centres, this may take the form of ensuring that clinician-scholars in QIPS are given equal opportunity for academic advancement compared with their researcher and educator colleagues (e.g., as “clinician improvers”). This may be done through the celebration, promotion, and support of the academic dissemination of their work.Reference Shojania and Levinson43,Reference Mondoux, Frank and Kwok44 At the hospital and health system levels, this may include non-monetary improvement or leadership awards, work/schedule arrangements, or cost savings being re-invested in the ED (i.e., gain-sharing approach), as well as career advancement for those who contribute to successful QIPS projects and improve the patient experience (e.g., supporting CPD or leadership opportunities). Indeed, the QIPS skills necessary for successful improvement processes are often transferable to leadership and administrative responsibilities.
Recommendation 10. In centres with no QIPS experience, consider starting small by focusing on a project or specific deliverable instead of a program
The recommendations outlined above can be modified and applied to a QIPS project or specific deliverable instead of a program of QIPS. A successful initiative can then be used as a foundation to change culture toward the acceptance of iterative and ongoing improvement work and building a QIPS program. Options for a foundational project include starting with a small, engaging, and feasible deliverable or collaborating with and supporting colleagues on a larger initiative.
When starting with a first QIPS initiative, ensure that it aligns with organizational priorities and make it relevant and engaging to stakeholders. Using a systematic approach such as the one elaborated in the CJEM QI Primer Series or by using the SQUIRE guidelines would improve the odds of success.Reference Chartier, Cheng, Stang and Vaillancourt33,Reference Chartier, Vaillancourt, Cheng and Stang40,Reference Chartier, Stang, Vaillancourt and Cheng45,Reference Ogrinc, Davies and Goodman46 Another key starting point is to identify QIPS training opportunities for health care providers and support staff. Initial training options include online and distance learning opportunities such as the Institute for Healthcare Improvement (IHI) open school.47 Stakeholder engagement including multi-disciplinary teams, leadership, administration, and patients and families would be particularly important in achieving a successful initial QIPS project or deliverable and building a culture that is supportive of quality improvement.
CONCLUSION
Continuously improving the delivery of health care services is essential, but difficult, and QIPS methodologies have been shown to increase the likelihood of success and sustainability of improvement projects. Our national needs assessment survey demonstrated a discrepancy between the current level of infrastructure and resources allocated to ED QIPS activities compared with the level of academic output and operational efforts. As the field and our community mature, there is an opportunity for ED providers and leaders to move away from stand-alone improvement projects and toward programs of QIPS in their ED. Our expert panel developed recommendations based on expert opinion, a scoping review, and involvement of QIPS experts. We also developed an online QIPS training repository, with the goal of providing EM practitioners with useful links, examples, and resources. Although many steps may occur concurrently and local setting will dictate adaptations, these recommendations provide guidance for the development of a program of QIPS in the ED. Our hope is that these recommendations will contribute to the advancement of the field of QIPS in EM in Canada and, ultimately, improve patient care.
Acknowledgements
The authors acknowledge the input of the 14 experts who helped refine the recommendations, who include (alphabetically): Paula Blackstien-Hirsch, Dr. Lisa Calder, Dr. Amy Cheng, Dr. Alan Gobb, Dr. Scott McKay, Dr. Michael Lewell, Dr. Rod Lim, Jackie Schleifer Taylor, Dr. Howard Ovens, Dr. Paul Pageau, Dr. Timothy Rutledge, Dr. Jennifer Thull-Freedman, Dr. Stephanie VandenBerg, and Dr. Jim Worthington, as well as Danielle Porplycia for her help with preparation of the manuscript.
Competing interests
None declared.




