CLINICIAN’S CAPSULE
What is known about the topic?
There is a paucity of data that is useful for emergency department (ED) physicians counseling women with symptomatic early pregnancies about the future risk of ectopic pregnancy.
What did this study ask?
What are the clinical outcomes of pregnant women discharged from the ED where ectopic pregnancy had not yet been excluded?
What did this study find?
Of the 230 ectopic pregnancies, 5.1% patients had a ruptured ectopic pregnancy after their index ED visit.
Why does this study matter to clinicians?
Given the risk of a final diagnosis of ectopic pregnancy and more importantly possible rupture, patient education of these risks is critical on discharge from the ED.
INTRODUCTION
Previous research describes that 6% to 16% of patients in their first trimester of pregnancy presenting to a healthcare provider with vaginal bleeding or abdominal pain will have an ectopic pregnancy.Reference Murray, Baakdah and Bardell1, Reference Barnhart2 Therefore, excluding an ectopic pregnancy is critical when caring for women presenting to the emergency department (ED) with vaginal bleeding or abdominal pain in early pregnancy.
To date, there is a paucity of prognostic data that may be useful for ED physicians counselling women with symptomatic early pregnancies about the future risk of ectopic pregnancy. The objective of this study was to determine the clinical outcomes of pregnant (less than 12 weeks’ gestational age) women discharged from the ED where ectopic pregnancy had not yet been excluded.
METHODS
Study design, setting, and population
This was a single-centre, retrospective medical record review of pregnant (<12 weeks’ gestational age), adult (≥18 years) women discharged from the ED of an academic tertiary care centre (annual ED census 60,000) in Toronto, Ontario with a diagnosis of ectopic pregnancy, rule out ectopic pregnancy, or pregnancy of unknown location (PUL) over a 7-year period (January 2010 to January 2017). This tertiary care institution has a high-acuity obstetrical care program, and a radiologist-interpreted transvaginal ultrasound (US) is available 24 hours a day, 7 days a week to rule out suspected ectopic pregnancy in ED patients. Emergency physicians at this institution do not perform a transvaginal US in the ED.
Study protocol
Using a computerized, structured, data abstraction form, trained research personnel reviewed the medical records and extracted patient data. The study protocol was approved by the institutional research ethics board.
Outcomes
The primary outcome was the proportion of women who had a ruptured ectopic pregnancy after being discharged from the ED where an ectopic pregnancy had not yet been excluded. Other pregnancy outcomes and related medical/surgical management were also reported.
Data analysis
Data were entered directly into a study-specific Microsoft Excel database (Microsoft Corporation, Redmond, Washington). Descriptive statistics were summarized using means with standard deviations (SD), medians with interquartile ranges (IQRs), or frequencies with 95% confidence intervals (CIs) where appropriate.
RESULTS
Of 661 suspected ectopic pregnancies in the ED, 550 patients were discharged from the ED where ectopic pregnancy had not yet been excluded (Figure 1). Of these, 230 (41.8%) had an ectopic pregnancy, and 28 (5.1%) patients had a ruptured ectopic pregnancy after their index ED visit (Figure 1).
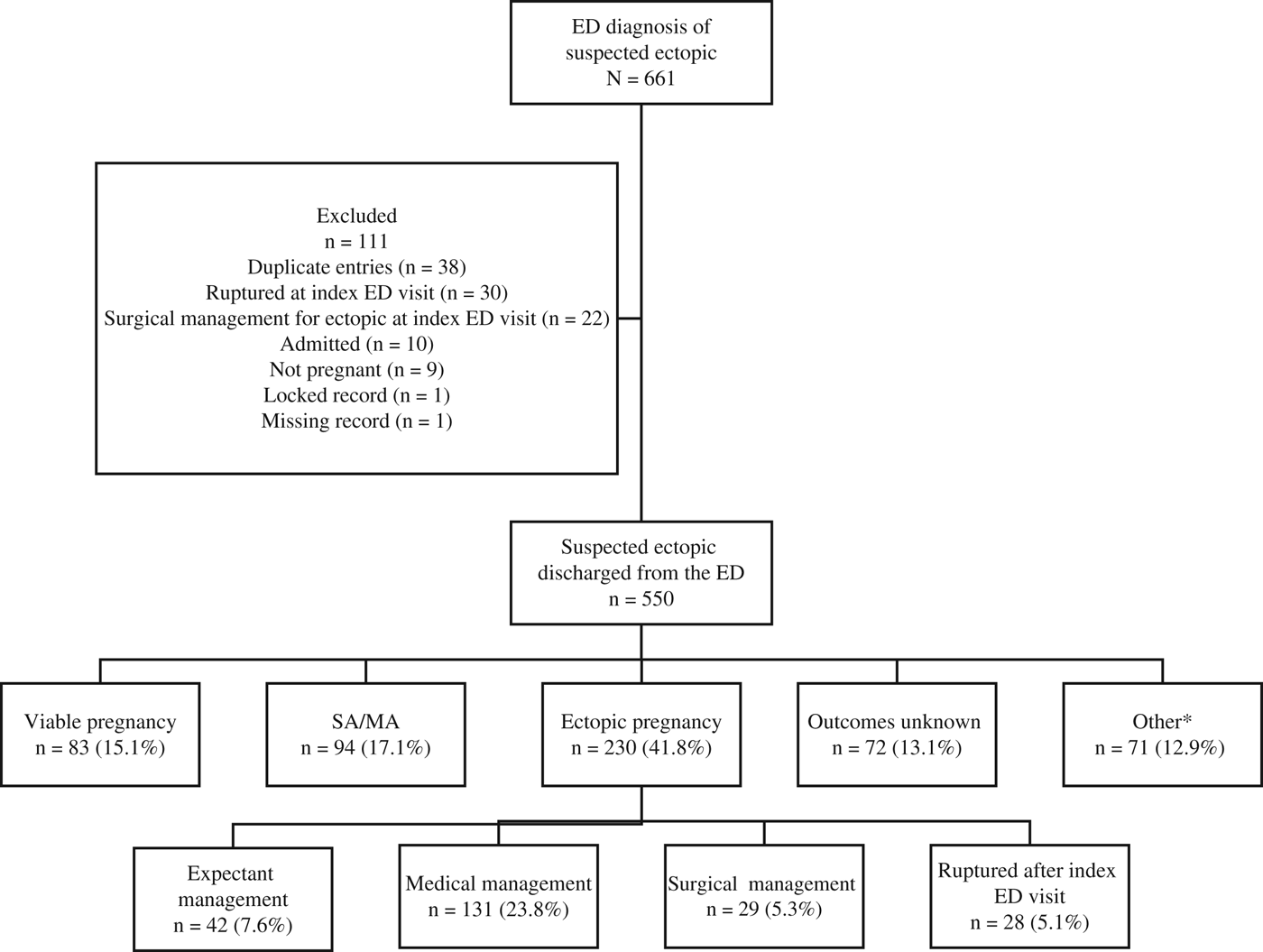
Figure 1. CONSORT diagram of included patients. *Includes therapeutic abortion, molar pregnancy, or resolution of beta human chorionic gonadotropin serum level with no location documented. ED=emergency department; SA/MA = spontaneous abortion/missed abortion
The mean (SD) patient age and gestational age were 32.0 (6.0) years and 6.3 (2.0) weeks, respectively. Risk factors for ectopic pregnancy (e.g., prior ectopic, history of pelvic inflammatory disease, in vitro fertilization) were similar for patients who did and did not have an ectopic pregnancy; 154 (28.0%) patients had a point-of-care US in the ED.
Of the 550 patients with a suspected ectopic pregnancy, 329 (59.8%) had a transvaginal US during their index ED visit. Of these, 157 (47.7%) were diagnosed with an ectopic pregnancy; 143 patients had initial US results, suggesting a suspicious adnexal mass. Of these, 124 (86.7%) went on to have an ectopic pregnancy. Of the 221 (40.2%) patients who did not have a transvaginal US during their index ED visit, 73 (33.0%) were diagnosed with an ectopic pregnancy.
Two hundred twenty-three (40.5%) patients with a suspected ectopic pregnancy had a PUL on the US that took place at or within 72 hours following the index ED visit. Of these, 40 (17.9%) had a viable pregnancy, 57 (25.6%) had a spontaneous or missed abortion, 42 (18.8%) had an ectopic pregnancy, 38 (17.0%) had unknown outcomes, and 46 (20.6%) had other outcomes that included a therapeutic abortion, molar pregnancy, or a resolution of βHCG with no location documented.
DISCUSSION
The primary objective of this study was to determine the clinical outcomes of pregnant women discharged from the ED where ectopic pregnancy had not yet been excluded, a higher risk cohort of patients discharged from the ED. Our results show that 41.8% of patients discharged from the ED with a suspected ectopic pregnancy are subsequently diagnosed and managed for an ectopic pregnancy, and 5.1% ruptured after their index ED visit.
Our findings of pregnancy outcomes following a transvaginal US showing a PUL are similar to previously reported studies from outpatient gynecology clinics.Reference Condous, Timmerman and Goldstein3-Reference Richardson, Gallos and Dobson6 Surprisingly, despite the 24 hours a day, 7 days a week availability of transvaginal US to rule out suspected ectopic pregnancy, only 59.8% of patients had a transvaginal US during their index ED visit. Current guidelines recommend that all higher risk patients with PUL warrant further investigations with transvaginal US.7, Reference Morin, Cargill and Glanc8 Non-adherence to these recommendations may result in patients being incorrectly diagnosed, having an ectopic pregnancy overlooked, or being inappropriately reassured about viability. These findings stress the importance of following current recommendations, because maternal morbidity and mortality can be reduced with an early diagnosis of ectopic pregnancy.Reference Morin, Cargill and Glanc8 Future research should focus on barriers and solutions to accessing a timely transvaginal US.
LIMITATIONS
This study has several limitations. It was conducted in a single-centre tertiary care institution with a high-acuity obstetric care program, and the results might not be generalizable to other settings. This study did not include search terms such as first trimester bleeding, vaginal bleeding, pregnancy or miscarriage, because we were interested in identifying only higher risk ED patients and describing their management. Therefore, these results should not be extrapolated to all ED patients experiencing first trimester complications. Due to the retrospective nature of this study, we can only report what was documented in the patient chart. It is possible that ED clinical management was dictated by US results from outpatient settings, point-of-care ultrasound findings, or presence of known risk factors for ectopic pregnancy not documented in the chart.
CONCLUSIONS
These results may be useful for ED physicians counselling higher risk women with symptomatic early pregnancies about the risk of ectopic pregnancy after they are discharged from the ED. Given the risk of a final diagnosis of ectopic pregnancy and more importantly, possible rupture, patient education of these risks is critical on discharge from the ED.
Competing interests
None declared.



