Human immunodeficiency virus (HIV) infection is a major global health problem, and nutritional disorders are often present in HIV+/AIDS patients. Early studies demonstrated weight loss and protein depletion, findings associated with body cell mass depletion in untreated patientsReference Kotler1. Poor nutritional status may be caused by different factors:
inadequate nutrient intake or absorption, metabolic alterations, hypermetabolism, or a combination of these;
alteration of the gastrointestinal tract;
drug-nutrient interactions.
Anorexia related to the psychological processes provoked by the pathology (mainly social isolation), biochemical changes, including an increase in the activity of the cytokines, a diverse drug intake, physical inactivity, and opportunistic diseases also lead to a decrease in food intakeReference Johnson, Albu, Engelson, Fried, Inada, Ionescu and Kotler2–Reference Wanke, Falutz, Shevitz, Phair and Kotler5.
Since the appearance of highly active antiretroviral therapy (HAART), a lower incidence of malnutrition, and an improvement of the survival and immunological functions of infected patients has been observed. However, this highly effective antiretroviral therapy is associated with lipodistrophy, related, in turn, to insulin resistance and its metabolic complications, such as impaired glucose tolerance, diabetes, and hypertriglyceridemiaReference Kotler1, Reference Shevitz, Wanke, Falutz and Kotler6, Reference Chen, Misra and Garg7.
The importance of nutritional support, in addition to the antiretroviral therapy in HIV+/AIDS patients, has been accepted. Nutritional support is needed to maintain optimum nourishment during the symptomatic period, in order to prevent further deterioration of the nutritional status during acute episodes of infection, and to improve the nutritional status during the stable symptom-free periodReference Sherlekar and Udipi8, Reference Polsky, Kotler and Steinhart9. Since 1989, the American Dietetic Association emphasised that nutrition intervention and education should be part of the health care provided to individuals infected with HIV, and they should be implemented at all stages of the disease10. It is also advocated that nutritional intervention should be applied early and individually, with periodic and constant screeningReference Fajardo Rodriguez and Lara del Rivero-Vera11. Some authors have pointed out that nutritional deficiency may influence the biological gradient and the natural course of the AIDS infectionReference Chandra12.
International literature considers that biochemical evaluation in AIDS patients must include at least serum levels of albumin, transferrin, total protein, and cholesterol, blood haemoglobin content and haematocrit. It is also considered that the depletion of some of these is indicative of protein deficiency or anaemia, respectively. On the other hand, routine indicators, such as the total number of lymphocytes and delayed hypersensitivity skin tests, are not useful as indices of nutritional state, due to the impact of the disease on immunological markersReference McCorkindale, Dybevik, Coulston and Sucher13. Moreover, some authors indicate that nutritional assessment of these patients should include a measurement of body composition, and analyses of nutritional parameters, including albumin, transthyretin, and C-reactive proteinReference Salomon, de Truchis and Melchior14.
The aim of this study was to evaluate the nutritional status of adults infected with HIV or with AIDS through the examination of their biochemical profile.
Methods and materials
Body weight and height were determined, and the BMI (kg/m2) calculated in 43 patients (19 HIV+ and 24 AIDS patients) between 26 and 44 years old, who attended Helios Salud, a health centre specialised in AIDS management. Blood samples were collected from fasting patients; 35 patients received HAART. 89 % presented CD4+ blood cell counts of >200 cells/ml and 60-75 % showed viral charges lower than 50 copies/ml. Plasma cholesterol, HDL and LDL cholesterol, triacylglycerol, total protein, apolipoproteins A-I and B (ApoA-I and ApoB) and fibrinogen concentrations were determined. Specific plasma proteins of potential utility in nutrition studies, including albumin, transthyretin, retinol binding protein (RBP) and the acute phase reactant ceruloplasmin were also determined. Total protein content was determined by the Biuret method, and specific proteins by quantitative radial immunodiffussion on plates (Diffuplate, Biocientifica SA, Argentina and Binding Site, UK). Results were compared to reference valuesReference Mancini, Carbonara and Heremans15–Reference Weisstaub, Feliu and Slobodianik17.
Total cholesterol, HDL and triacylglycerol concentrations were determined by enzymatic-colorimetric methods, and LDL was calculated with Friedwald's equation (LDL-cholesterol = total cholesterol - triacylglycerols/5+HDL-cholesterol). Reference values for total cholesterol, HDL, LDL, triacylglycerolsglycerides, were taken from the current guidelines for handling dislipidaemiaReference Kavey, Daniels, Lauer, Atkins, Hayman and Taubert18.
Plasma levels of zinc (Zn), copper (Cu), and selenium (Se) were determined in haemolysis-free plasma by flame atomic absorption spectrometry. For each mineral, a calibration curve was performed, using commercial standards19, 20. The Cu/Zn ratio was calculated, and compared with reference valuesReference Lockitch, Halstead and Wadsworth21. Statistical analyses were performed with the Student's t-test.The study was approved by the Ethics Committee of the University of Buenos Aires, and all participants gave written consent before recruitment.
Results
Table 1 shows the BMI, total protein concentration, and plasma levels of albumin, transthyretin, RBP, ceruloplasmin. No significant differences were observed in BMI, total protein concentration and plasma levels of albumin, transthyretin, RBP and ceruloplasmin, between HIV+ and AIDS patients. Table 2 shows the lipid profile, ApoA-I, ApoB and fibrinogen in the patients. Fibrinogen levels from the AIDS patients were higher than those of the HIV+ group. No statistical differences between the groups were observed in other biochemical parameters. Regarding the minerals status, there were no statistical differences in plasma Cu, Zn, and Se levels or in the Cu/Zn ratio between the HIV+ and AIDS groups. Zn (μg/ml): 2·04 (0·42) vs. 2·20 (0·64); Cu (μg/ml) 1·77 (0·35) vs. 1·83 (0·28); Se (μg/l): 47·6 (18·3) vs. 43·7 (13·7); Cu/Zn ratio: 0·91 (0·31) vs. 0·87 (0·20). Both groups showed plasma Zn and Cu levels within the highest reference values. About 70 % of the patients had plasma Se concentrations which were below 60 μg/l.
Table 1 BMI, and concentrations of total and specific plasma proteins in HIV+ and AIDS patients
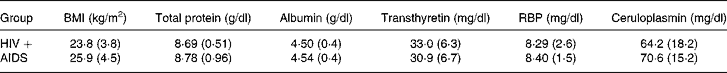
Data are mean (SD).
RBP, Retinol binding protein.
Table 2 Plasma lipid profile, and concentrations of apolipoproteins A-I and B and fibrinogen in HIV+ and AIDS patients

Data are mean (SD)
* Significantly different from HIV+ at P < 0·05.
Discussion
HIV-infected and AIDS patients showed albumin levels within the reference range. Different investigators have demonstrated that the levels of albumin, transthyretin, and C-reactive protein are predictors of survivalReference Melchior, Niyongabo, Henzel, Durack-Brown, Henri and Boulier4, Reference Salomon, de Truchis and Melchior14, Reference Lockitch, Halstead and Wadsworth21, Reference Niyongabo, Melchior, Henzel, Bouchaud and Larouze22. Short-lived proteins are very promising in the evaluation of the nutritional statusReference Niyongabo, Melchior, Henzel, Bouchaud and Larouze22. However, metabolic disorders caused by stress can also affect their concentrationReference Slobodianik Nora and De Girolami23–Reference Bernstein and Pleban25. In this study, we observed that 50-60 % of HIV+/AIDS patients presented plasma RBP levels close to the highest reference values, and 10 % of AIDS patients showed transthyretin values within the highest reference values. This behaviour was also described by Lopez Hellin et al. Reference López Hellin, Baena-Fustegueras, Schwartz-Riera and Garcia –Arumi26 in a group of postsurgical patients with high levels of stress. Only two patients with AIDS and one HIV+ patient showed transthyretin values lower than 20·0 mg/dl, this value is associated with protein deficiencyReference Niyongabo, Melchior, Henzel, Bouchaud and Larouze22, Reference Ingengleek and Young24. In contrast, previous results performed on forty-five children with AIDS, diagnosed according to the criteria of the Centers for Disease Control and Prevention, showed lower levels of transthyretin and RBP than laboratory reference valuesReference Slobodianik, Pallaro, Río, Barbeito, Strasnoy, Franchello, Casella, Torales, Giraudi and Ramos27. Around 40 % of HIV+ and AIDS patients presented ceruloplasmin levels above 65 mg/dlReference Mancini, Carbonara and Heremans15. It is interesting to remark that AIDS patients with transthyretin levels above 40 mg/dl presented ceruloplasmin concentrations over reference values, so this plasma fraction would be performing the role of acute phase protein. Fibrinogen levels were significantly higher in AIDS patients while total cholesterol, triacylglycerol, LDL and Apo B tended to be higher in the HIV+ patients, but the differences between groups did not reach statistical significance. These changes were described in several reports as complications related to the antiretroviral medication, especially regarding the levels of triacylglycerols and very low density lipoproteins (VLDL)Reference Carr and Cooper28.
The changes of fibrinogen in this study supports previous studies on HIV+/AIDS infants (M.S. Feliu, unpublished results), and stress the importance to include fibrinogen in the periodic nutritional monitoring of these patients. The global analysis of the results shows an alteration in the lipid profile of HIV+/AIDS patients, and emphasises the need to design appropriate nutritional treatments. This would allow an early evaluation of cardiovascular risk and the implementation of therapeutic guidelines, along with the specific retroviral treatment and adequate food selection, to exert a positive effect on plasma lipids, an important factor of cardiovascular riskReference Myers, Rifai and Tracy29, Reference Stein30.
On the other hand, Treitinger et al. observed a decrease in the HDL-fraction, triacylglycerol, and albumin levels with an increase in haptoglobin concentration, as indicators of the progression of the disease in HIV+-infected patientsReference Treitinger, Spada, da Silva, Hermes, Amaral and Abdalla31.
Several investigators have pointed out that a Cu/Zn ratio >1·0 is associated with an increase in mortalityReference Lai, Lai, Shor-Posner, Ma, Trapido and Baum32. In our study, about 30 % of AIDS patients showed a Cu/Zn ratio higher than 1 while 21 % of HIV infected patients did. Moreover, these patients suffered deterioration of the immune system, indicated by the lower number of CD4+ lymphocytes. This would be in agreement with Lai et al. Reference Lai, Lai, Shor-Posner, Ma, Trapido and Baum32, who proposed that the Cu/Zn ratio would be a useful predictor of survival in HIV infection. Besides,.Moreno et al. Reference Lai, Lai, Shor-Posner, Ma, Trapido and Baum32 indicate that serum copper determination would be a helpful marker in the progression of the infection towards AIDS, and in other chronic infectious diseases.
Serum zinc levels in the studied individuals were within or over normal values; this finding agrees with a preliminary study performed in HIV+/AIDS children, but differs from data reported by other authors for adult patients, which indicated a decrease in serum Zn concentrationReference Moreno, Artacho, Navarro, Perez and Ruiz López33, Reference Pallaro, Barbeito, Strasnoy, Franchello, Giraudi, Ramos and Slobodianik34. It is important to remark that Wellinhausen et al. Reference Wellinghausen, Kern, Jochle and Kern35 also demonstrated a decrease in Zn levels in 23 % of a HIV+-infected population, which is in agreement with our resultsReference Wellinghausen, Kern, Jochle and Kern35. Due to the importance of Zn to the immune system, the assessment of this mineral is very important in order to optimise the results of the nutritional treatment and drug therapy and its incorporation into the diet must be considered.
In addition, 65-70 % of the studied population showed decreased plasma Se levels when compared to reference values; this fact is in agreement with international literatureReference Baum, Shor-Posner, Lai, Zhang, Lai, Fletcher, Sauberlich and Page36, Reference Bogden, Kemp and Hans37. The same observation was made in a preliminary study on infected childrenReference Pallaro, Barbeito, Strasnoy, Franchello, Giraudi, Ramos and Slobodianik34. Different authors indicate a sharp relationship between selenium deficiency and the deterioration of the immune system; they consider this biochemical parameter as an independent predictor of survival for patients infected with HIVReference Wellinghausen, Kern, Jochle and Kern35, Reference Baum, Shor-Posner, Lai, Zhang, Lai, Fletcher, Sauberlich and Page36. Our results stress the importance of analyzing the possible effect of the addition of selenium in the prevention and treatment of AIDS-related pathologies.
Bogden et al. Reference Bogden, Kemp and Hans37 have reported that depression of the nutritional status begins in the first stages of HIV-1 infection, which can contribute to the progression of the disease.
Our preliminary study, performed on HIV+ and AIDS patients belonging to low and medium socioeconomic groups, with access to health care services, shows some differences in some biochemical parameters: an increase in fibrinogen and a trend to decreased transthyretin levels. Therefore, the nutritional status of infected patients is different at different stages of the disease. Moreover, these findings support previous studies on HIV+/AIDS-infected infants, and emphasise the importance of incorporating functional biochemical parameters in the periodic nutritional assessment of these patientsReference Pallaro, Barbeito, Strasnoy, Franchello, Giraudi, Ramos and Slobodianik34, Reference Pallaro, Barbeito, Strasnoy, Franchello, Giraudi, Ramos and Slobodianik38. This would allow an early evaluation of the nutritional status, and the assessment of an appropriate tailored nutritional support, implemented along with the specific retroviral treatment. This would aim at delaying the evolution of the disease, and might improve the prospects of survival and quality of life of these patients.
Conflict of interest statement
This study was funded by the University of Buenos Aires (B-060). The authors have no conflict of interests to declare. The manuscript is in partial fulfillment of the Doctor's Degree of MS, fellow of University of Buenos Aires. The article was discussed and co-written by all authors (MS, SF, NHS).




