Obesity, a consequence of overeating and lack of exercise, is an important clinical and public health burden worldwide. In 2005, 23·2 % of the world's adult population was overweight, 9·8 % was obese, and the estimated total numbers of overweight and obese adults were 937 million and 396 million, respectively. By 2030, if recent secular trends continue unabated, the estimated absolute numbers of overweight and obese individuals will be 2·16 billion and 1·12 billion(Reference Kelly, Yang and Chen1). Because this increase in body weight is associated with a rise in CVD, type 2 diabetes, non-alcoholic fatty liver disease and hypertension(Reference Ogden, Yanovski and Carroll2, Reference Ogden, Carroll and Curtin3), programmes for the prevention and treatment of obesity should be a priority to face the challenge of this public health problem.
Both low-fat and low-carbohydrate diets have been shown to induce weight loss and reduce obesity-related co-morbidities; however, most but not all of the obese individuals who are participating in weight-loss strategies that involve diet and exercise reduce their initial body weight(Reference Klein4, Reference Norris, Zhang and Avenell5), and the improvement in weight between groups is small(Reference Norris, Zhang and Avenell5). Regarding diet, low-carbohydrate diets have been shown to promote a significantly greater weight loss than low-fat diets(Reference Samaha, Iqbal and Seshadri6), and low-carbohydrate diets had more favourable overall outcomes on atherogenic dyslipidaemia and glycaemic control(Reference Stern, Iqbal and Seshadri7, Reference Eckel8). Although it is routinely indicated for individuals participating in programmes for weight loss, exercise per se induces a small weight reduction. The combination of both exercise and diet results in marginal benefits compared with diet alone(Reference Eckel8, Reference Nordmann, Nordmann and Briel9). Because the primary gauge for successful obesity treatment should be focused on health improvement instead of body-weight reduction(Reference Kazaks and Stern10), behavioural treatment emerges as a useful approach in helping obese individuals lose weight(Reference Kazaks and Stern10, Reference Foster, Makris and Bailer11). Behavioural treatment aids in the identification of those factors that trigger overeating and the lack of physical activity, promotes the adoption of new responses, and reinforces the adoption of positive behaviours(Reference Simon, Von Korff and Saunders12). The goal of treatment is to initiate and maintain a process of problem solving to determine whether the removal or reduction of the causal factors promotes an appropriate manner of eating and greater weight loss(Reference Foreyt and Goodrick13). The central principle in behaviour therapy is that patients must learn dietary restraint to resist unhealthy eating habits(Reference Foreyt and Goodrick13). As a consequence, the behavioural approach is now integrated into most programmes for weight loss, inducing weight losses in the range of 9 to 13 kg(Reference Brownell and Kramer14, Reference Björvell and Rössner15). However, studies indicate that 30–35 % of patients regain weight in the first year after treatment and that 3–5 years later, at least 50 % of participants have returned to their initial weight or more(Reference Wadden and Foster16).
Thus, among the strategies used to increase the rate of successful weight loss in adults, cognitive behavioural treatment (CBT), a triphasic focal psychotherapy intervention, is the most well-established psychotherapeutic treatment of problematic psychosocial functioning that characterises eating disorders and obesity(Reference Wilfley, Welch and Stein17). In one of the studies using CBT strategies, Cresci et al. (Reference Cresci, Tesi and La Ferlita18) reported that the mean weight loss among subjects participating in a behavioural programme for the treatment of obesity was superior at 6 months compared with a similar group of subjects who received conventional treatment for obesity (2·0 (sd 3·9) v. 0·8 (sd 2·5) kg/m2; P < 0·05). Results showing the initial and long-term efficacy of CBT in the treatment of primary and secondary symptoms of binge-eating disorders(Reference Wilfley, Welch and Stein17, Reference Munsch, Biedert and Meyer19) and in the continuation of weight loss during follow-up(Reference Van Dorsten and Lindley20–Reference Golay, Buclin and Ybarra22) are consistent.
However, to the best of our knowledge, there are no current data about what type of energy-reducing diet, when combined with CBT, produces the best initial treatment outcome. Thus, the aim of the present study was to evaluate the efficacy of adding CBT to either low-carbohydrate or low-fat diets in the treatment of weight loss of obese women.
Experimental methods
With the approval of the protocol by the Research Committee of the Mexican Social Security Institute, a randomised clinical intervention study was carried out in Durango City in northern Mexico, from July 2007 to June 2008.
Participants
Obese women from the same neighbourhood and similar social and economic strata were invited to participate in the study. A total of 105 obese women with an average age and BMI of 45·4 (sd 10·4) years (range 25–61 years) and 36 (sd 4·3) kg/m2 (range 31·2–47·8 kg/m2) were enrolled. All participants gave their written informed consent to participate in the study.
Pregnancy, hypothyroidism, heart failure, and renal and hepatic disease were exclusion criteria.
Obese women were assigned to study groups using two-stage random procedures. In the first stage, a total of fifty-five (52·4 %) women were randomly assigned to receive CBT, and fifty women were assigned to the control group. In the second stage, within each group, women were randomly selected to receive either low-carbohydrate (LC) or low-fat (LF) diets. Four groups were assigned for analysis: CBT–low-carbohydrate diet (CBT-LC); CBT-low-fat diet (CBT-LF); control group with low-carbohydrate diet (C-LC); control group with low-fat diet (C-LF).
The women in the study were followed for 6 months. The primary trial end-point was the percentage of weight loss. The final distribution of the population in the study is shown in Fig. 1.
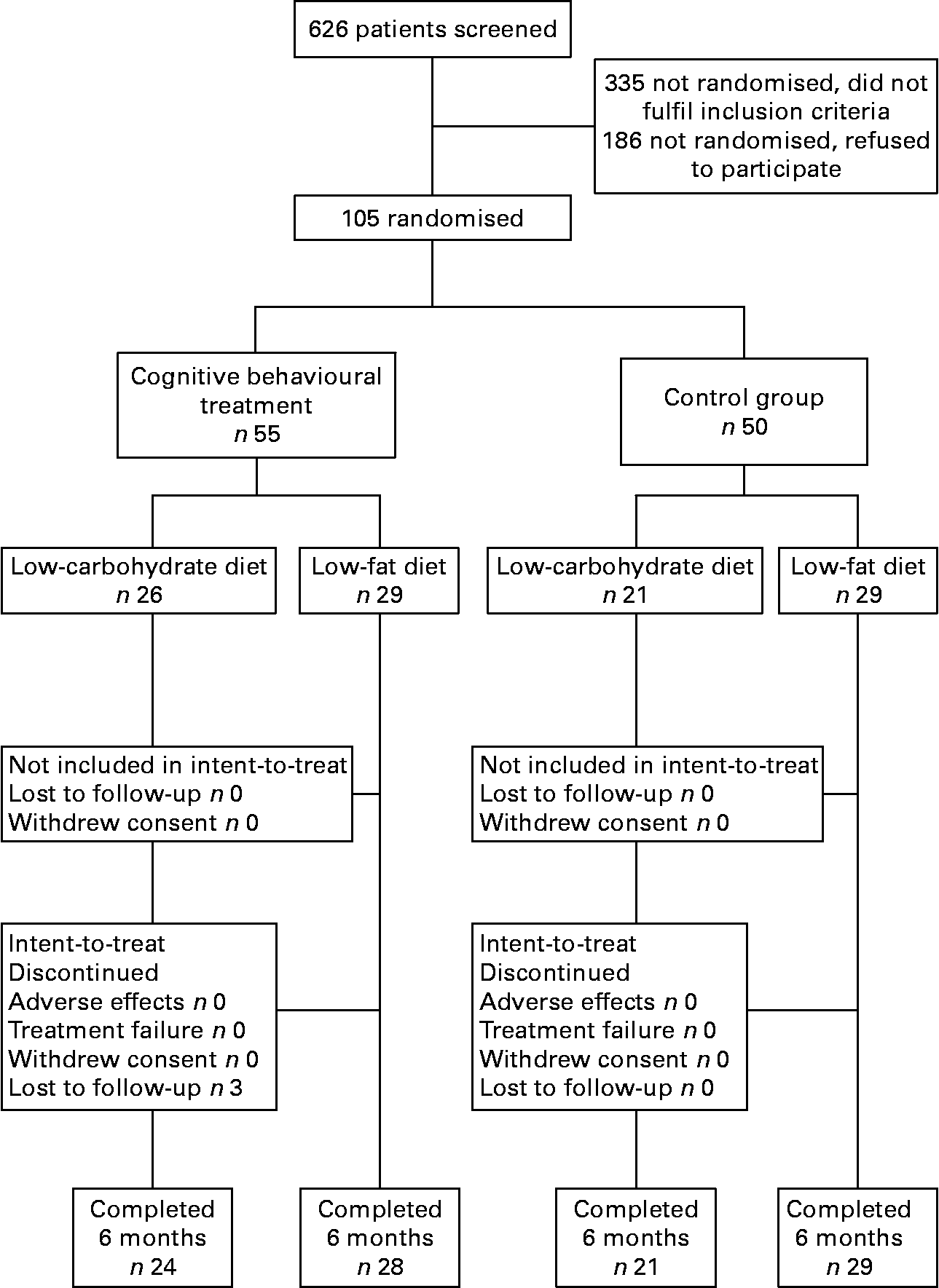
Fig. 1 Study participant flow diagram.
Treatment programme
Because obesity is frequently associated with mood disorders, such as anxiety and depression(Reference Onylike, Crum and Lee23), all women in both groups received weekly psychological support for treatment or prevention of depression and anxiety. In addition, women in the CBT and control groups received weekly sessions of 1 h for diet and exercise advice. Additionally, women in the CBT group received an intervention that included behavioural strategies, cognitive skills and relapse prevention techniques to identify factors that trigger overeating and the lack of physical activity and for promoting the use of new responses to these triggers.
All sessions for women in both groups were individually conducted by trained personnel of the Biomedical Research Unit. Diaries of both diet and exercise were completed by participants and reviewed at each visit. Recommendations for exercise were walking, dancing, bicycling or swimming for 30 min per d, on at least 5 d per week.
Total energy intake was calculated based on 125 kJ/kg per d (30 kcal/kg per d) of ideal body weight. The LC diet was based on the following percentage of total energy intake per nutrient: 27 % protein, 28 % fat and 45 % carbohydrate. The LF diet was based on 21 % of daily energy intake from fat, less than 10 % saturated fat, 25 % protein and 54 % carbohydrates(Reference Lichtenstein, Appel and Brands24, Reference Yancy, Olsen and Guyton25). Adherence to diet and exercise was assessed every week by personal interviews with the female participant and a family member living with her.
Hepatic disease, serum creatinine level ≥ 15 mg/l, severe life-limiting medical illness, active participation in other dietary programmes and the use of weight-loss drugs were exclusion criteria.
Definitions
Obesity was defined as a BMI ≥ 30 kg/m2(Reference Bantle, Wylie-Rosett and Albright26). CBT, a triphasic focal psychotherapy, was based on behavioural strategies, learning cognitive skills and prevention techniques of relapse. CBT includes strategies for keeping food and activity records, activity of progressive relaxation, nutrition education, techniques for eating, strategies for recognising and solving problems and cognitive restructuring(Reference Wadden and Foster27).
Depression and anxiety were measured using the Beck Anxiety Inventory (BAI) and the Beck Depression Inventory (BDI) scales, which consist of twenty-one items each, that have been previously validated in the Mexican population. The BAI and BDI provide reliable information about characteristics, attitudes, and symptoms of anxiety and depression. Diagnosis of depression and anxiety was based on the following scale of BAI and BDI: 0–13 points; absent; 14–15 points, mild; 16–19 points, moderate; ≥ 20 points, severe(Reference Beck, Emery and Greenberger28, Reference Beck, Rush and Shaw29).
Measurements
The applied questionnaires covered demographic characteristics and medical conditions. Measurements included blood pressure, total body fat, waist circumference, weight and height.
In the standing position, weight and height were measured with the women in light clothing using a fixed scale with a stadiometer (Tanita TBF-215; Tanita, Tokyo, Japan). The precision of weight and height measurements was 0·1 kg and 0·01 m. BMI was calculated as weight (kg) divided by height (m) squared. Waist circumference was measured halfway between the last rib and the iliac crest. Total body fat was measured by bioelectric impedance using a body composition analyser (Tanita TBF-215; Tanita) with 0·1 % increments. Anthropometric measurements were performed at baseline and every month.
Using a Baumanometer (Microlife AG, Heerbrugg, Switzerland) and stethoscope (3M Littman Classic II; 3M Medica GmbH, Neuss, Germany), the technique used for the measurement of blood pressure was the one that was recommended in the Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure(Reference Chobanian, Bakris and Black30).
Assays
A venous whole-blood sample was collected during fasting. Serum glucose and TAG were determined by the glucose-oxidase and enzymic methods, respectively. Laboratory measurements were performed at baseline and post-test. The intra- and inter-assay variations were 2·1 and 1·5 %, respectively, for the glucose-oxidase method and 2·0 and 3·0 %, respectively, for the enzymic method. Measurements were performed in an Express 500 clinical chemistry autoanalyser (Ciba Corning, Diagnostic Corp., Overling, OH, USA).
Statistical analysis
The pre-planned intention-to-treat analysis of the primary study end-point was done for all the randomly allocated participants (Fig. 1). Differences between the groups were assessed using the unpaired Student's t test (Mann–Whitney U test) and the χ2 test (for qualitative variables). Data between baseline and post-test within the same group were analysed using the paired Student's t test (Wilcoxon test). Differences between more than two groups were analysed by one-way ANOVA with the Bonferroni post hoc t test.
All data were processed and analysed using the statistical package SPSS for Windows version 15.0 (SPSS, Inc., Chicago, IL, USA).
Results
There were three women (2·8 %) who dropped out, all from the CBT group (Fig. 1). Women in both groups received an average of 6795 (sd 12·64) kJ/d during the 6 months of treatment. Adherence to diet and exercise was reached by 91 % of the women in both groups.
Women in the LF diet groups exhibited higher rates of diabetes (17·5 v. 2·0 %; P = 0·009) and hypertension (46·6 v. 21·0 %; P = 0·006) compared with women in the LC groups.
The baseline characteristics of participants are shown in Table 1. There were no significant differences between the groups for obesity measurements, fasting glucose, or TAG levels.
Table 1 Baseline characteristics of the women allocated to receive the low-carbohydrate (LC) or low-fat (LF) diet
(Mean values and standard deviations)
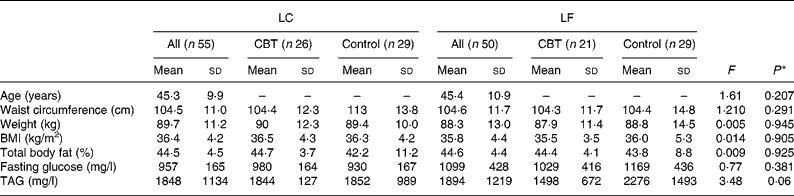
CBT, cognitive behavioural treatment.
* P value estimated by one-way ANOVA with Bonferroni post hoc test.
Of the study participants, twenty-six (47·3 %) and twenty-nine (52·7 %) women were assigned to the CBT-LC and CBT-LF groups, respectively, and these study groups were compared with twenty-one (42 %) and twenty-nine (58 %) women in the C-LC and C-LF diet groups, respectively.
Low-carbohydrate groups
At baseline, there were no significant differences in body weight, BMI or body fat between the women in the CBT-LC and C-LC groups. At post-test, women in the CBT-LC diet group significantly decreased their TAG concentrations compared with women in the C-LC group (Table 2).
Table 2 Characteristics of the women who received the cognitive behavioural treatment (CBT) with the low-carbohydrate (LC) diet (CBT-LC) and of the control group with the LC diet (C-LC)
(Mean values and standard deviations)
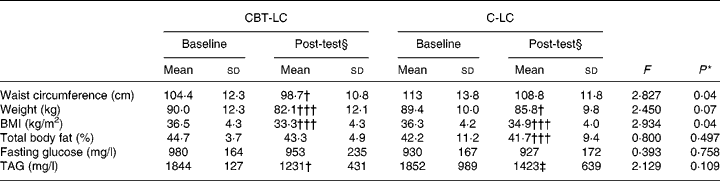
* P value estimated by one-way ANOVA with Bonferroni post hoc test.
Mean value, within each group, was significantly different from that at baseline: † P < 0·05, ††† P < 0·0005 (paired t test).
‡ Mean value was significantly different from that of the CBT-LC group at post-test (P < 0·05).
§ At 6 months after initiation of the diet treatment.
At baseline, the rates of depression (54 and 62 %; P = 0·82) and anxiety (62 and 66 %; P = 0·98) were similar in both the CBT-LC and C-LC groups; although the decrease in depression and anxiety between baseline and post-test was higher in the CBT-LC group, there were no significant differences between the groups ( − 53·8 and − 38·9 %, P = 0·48 for depression; − 60 and − 36·8 %, P = 0·29 for anxiety in the CBT-LC and C-LC groups, respectively).
Low-fat diet groups
No significant differences were documented in weight, BMI and body fat between the women in the CBT-LF and C-LF groups at baseline. However, at post-test, women in the CBT-LF group had significantly decreased body fat, weight, BMI and TAG concentrations compared with women in the C-LF group (Table 3).
Table 3 Characteristics of the women who received the cognitive behavioural treatment (CBT) with the low-fat (LF) diet (CBT-LF) and of the control group with the LF diet (C-LF)
(Mean values and standard deviations)
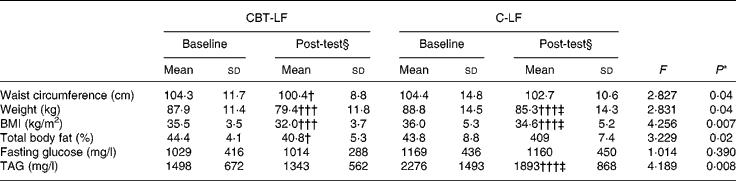
* P value estimated by one-way ANOVA with Bonferroni post hoc test.
Mean value, within each group, was significantly different from that at baseline: † P < 0·05, ††† P < 0·0005 (paired t test).
‡ Mean value was significantly different from that of the CBT-LF group at post-test (P < 0·05).
§ At 6 months after initiation of the diet treatment.
Similar to the results seen for the LC groups, at baseline, the rates of depression (52·4 and 62 %; P = 0·70) and anxiety (76·1 and 65·5 %; P = 0·62) were similar in the CBT-LF and C-LF groups; however, at post-test, the decrease of depression and anxiety, although higher in the CBT-LF group, showed no significant differences ( − 63·6 and − 44·4 %, P = 0·44 for depression; − 56·2 and − 36·8 %, P = 0·32 for anxiety in the CBT-LF and C-LF groups, respectively).
Figure 2 shows the proportion of weight loss between baseline and post-test in the groups in the study. Weight loss among women in the CBT-LC and C-LC diet groups was 8·7 and 4·0 %, respectively (P < 0·0001), whereas in the CBT-LF and C-LF diet groups, weight loss reached 9·7 and 3·9 %, respectively (P < 0·05). The weight loss was greater among women in the CBT-LF group compared with women in the CBT-LC group (P = 0·049); on the other hand, the difference between the C-LC and C-LF groups was not significant (P = 0·75).
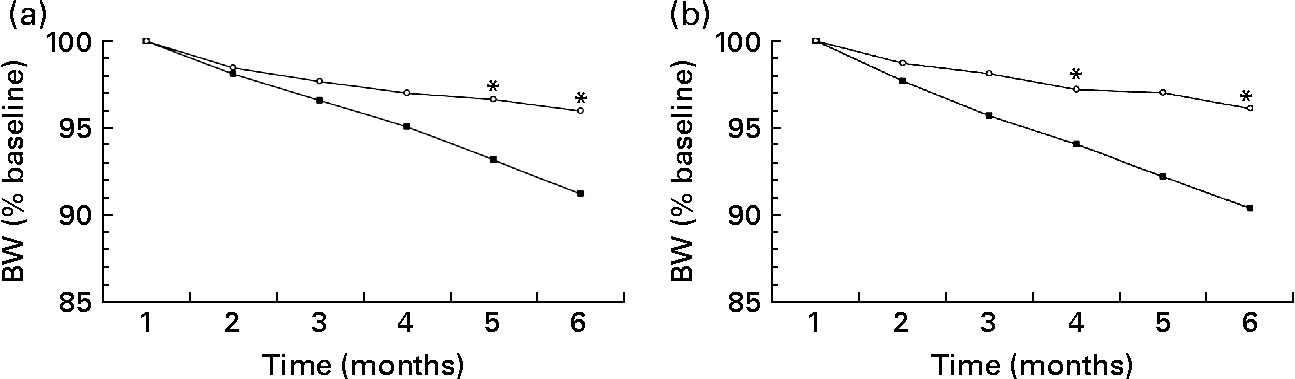
Fig. 2 Body-weight (BW; % of baseline) in women with (■) and without (○) cognitive behavioural treatment who received a low-carbohydrate diet (a) or a low-fat diet (b). At 6 months of treatment, weight loss in the women who received cognitive behavioural treatment and the low-fat diet was significantly lower than weight loss of the women in the cognitive behavioural treatment who received the low-carbohydrate diet. On the other hand, there were no significant differences between the women who received the low-fat and the low-carbohydrate diet, in the control groups. * Mean value was significantly different from that of the women who received the cognitive behavioural treatment (P < 0·05).
Discussion
The present results showed that adding CBT to either an energy-restricted, low-carbohydrate diet or to an energy-restricted, low-fat diet produces significantly greater short-term weight loss compared with diet alone. In addition, the present results also show that adding CBT to a low-fat diet produces higher short-term weight loss than adding CBT to a low-carbohydrate diet.
Because obesity has emerged as a major public health problem, several recommendations for diet and lifestyle changes for the prevention of obesity and its complications have been made(Reference Foster, Wyatt and Hill31). As one of the multiple strategies for weight loss, a behavioural programme could facilitate compliance in the adoption of required lifestyle changes(Reference Wadden, Butryn and Wilson32), identify those factors that trigger inappropriate eating and unsuitable habits of physical activity, and promote learning for achieving realistic goals for lifestyle changes(Reference Foster33).
Individuals who combine energy-restriction diets and exercise with CBT may expect to lose about 5 to 10 % of pre-intervention body weight over a period of 4 to 6 months(Reference Wilfley, Welch and Stein17, Reference Yanovski and Yanovski34). Foster et al. (Reference Foster, Makris and Bailer11) reviewed several weight-loss studies based on behavioural strategies showing an average weight loss of 9·6 kg during the first 21 weeks of treatment. In accordance with previous reports, the present study provides evidence that weight loss is greater among obese individuals undergoing CBT and that an important weight loss takes place in the first months of treatment. Furthermore, to the best of our knowledge, the present study is the first that includes a CBT component in a unique design that allowed us to evaluate the efficacy of adding CBT to different types of diets; our finding suggests that adding CBT to the management of obesity improves outcomes across different diets.
An increased focus on the emotional and cognitive processes associated with overeating has led to the detection of patterns that are potential causal factors of obesity. In this regard, the goal of CBT is to initiate and maintain a process of problem solving to determine whether the removal or reduction of the putative causal factors results in more prudent weight-management behaviours(Reference Foreyt and Goodrick13). After achieving a desirable weight, patients are encouraged to maintain body weight through a programme for continuing support. The present study shows that, irrespective of the type of diet, CBT strategies improve the outcomes of programmes for weight loss, a finding that supports the potential synergies of CBT and energy-restricted diets(Reference Eldredge, Stewart Agras and Arnow35–Reference Shelley-Ummenhofer and MacMillan37). Therefore, the combination of therapeutic strategies that improve a patient's knowledge of skills to avoid behaviours that lead to excessive intake with the low-energy diets is a promising approach for the treatment of obesity that is feasible in daily routine primary care.
In addition, women who received CBT support significantly reduced their serum TAG levels compared with the correspondent control groups. Previously, it has been shown that both low-fat and short-term low-carbohydrate weight-loss diets significantly decreased postprandial lipaemia and resulted in similar changes in fasting TAG levels. In this way, a decrease in body mass has been suggested to be the main factor involved in the improved postprandial lipaemia, independent of diet composition(Reference Volek, Sharman and Gómez38). In this regard, the greater reduction in the TAG levels that was observed among women who received CBT support in the present study could be related to the greater weight loss and to the positive changes in cognitive skills that CBT promotes for developing healthier attitudes that reinforce a healthier lifestyle. Other studies highlight that obese subjects with diabetes or the metabolic syndrome show a relative improvement in TAG levels on a carbohydrate-restricted diet than on a fat-restricted diet(Reference Samaha, Iqbal and Seshadri6).
Controversy about the optimal type of diet for weight loss is not related solely to metabolic outcome. In this regard, some studies show that a low-carbohydrate diet promotes higher weight loss than low-fat diets(Reference Samaha, Iqbal and Seshadri6, Reference Shai, Schwarzfuchs and Henkin39), but others highlight that a fat-restricted diet provides a high degree of satiety and promotes a higher reduction of body weight and better long-term adherence(Reference Knopp, Walden and Retzlaff40). Further research is needed to understand why diets with similar energy restriction but different macronutrient compositions produce different effects on weight loss.
Limitations of the present study that deserve to be mentioned are the following: (a) since we only studied women, the present results cannot be applied to men; (b) the short period of intervention prevented the evaluation of the long-term efficacy of combining CBT and a low-fat diet for weight loss; although similar results have been reported in other populations that show that the maximum weight loss is usually achieved during the initial phases of treatment, the long-term clinical efficacy of CBT as a strategy for weight loss remains to be established.
Conclusion
The present results showed that adding CBT to either a low-fat diet or a low-carbohydrate diet produced significantly greater short-term weight loss in obese women compared with diet alone. These findings support the efficacy of CBT in breaking previous dietary patterns and in developing healthier attitudes that reinforce a healthier lifestyle.
Acknowledgements
The present study was supported by grants from the Fundación IMSS, A.C.
H. R.-H. contributed with the original idea and design of the study; U. A. M.-A. and R. R.-V. designed and applied the treatment for depression and anxiety; F. R.-H. contributed with the design of diets used; M. R.-M. performed the statistical analysis; F. G.-R. contributed with the statistical analysis and wrote the manuscript draft. All the authors approved the final manuscript draft.
None of the authors has any conflict of interest.







