International community treatment orders use and outcomes
Community treatment orders (CTOs) were established with the aim of providing treatment to patients under supervision and outside a hospital setting, even involuntarily. The discussion regarding their efficiency has been an ongoing debate in recent years, yet their use is expanding worldwide without enough empirical evidence to support it. Legislative grounds for CTOs have existed for decades in various regions, including Australia, New Zealand, the USA, Asia, Canada, the UK and Switzerland, but rates of usage and legislation vary. Generally, the administration of CTOs differs with respect to duration, links to treatment, threshold for compulsion and patient admission history (Dawson, Reference Dawson2005). Their similarities lie in the general practice that is followed; a mental health specialist issues the order, the patient is placed on a CTO, and the order is renewed at specific time-frames over several years (Table 1). Therefore, their differing functions, not only internationally but also area by area, make it impossible to compare between studies.
Table 1 CTOs in Australia, New Zealand, USA, Canada and Switzerland, Scotland, England and Wales
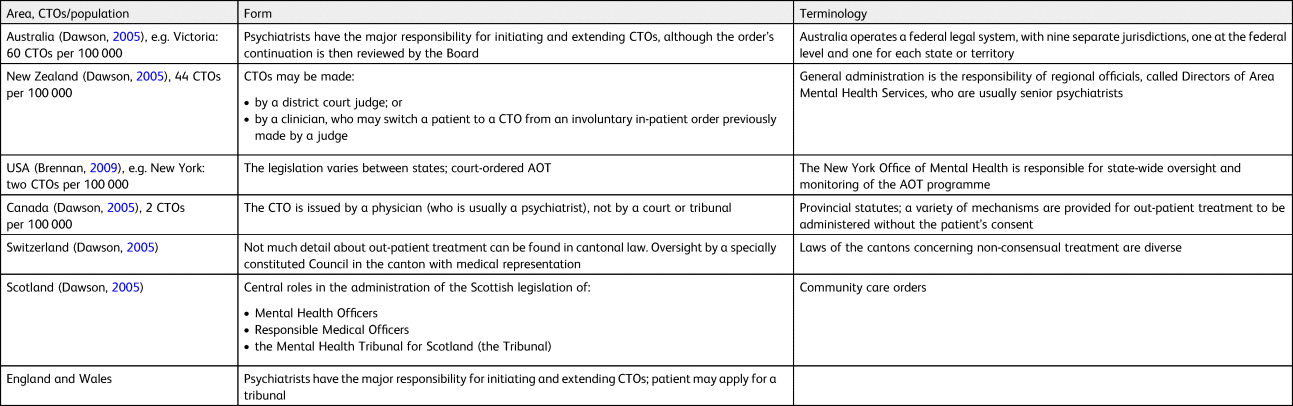
AOT, assisted out-patient treatment; CTO, community treatment order.
Important reviews, randomised controlled trials (RCTs) and anecdotal evidence suggest no benefits of CTOs in terms of patients' interests, no reduction in relapse rates or hospital bed days, and no improvement in adherence or quality of life (Steadman et al, Reference Steadman, Gounis and Dennis2001; Burgess et al, Reference Burgess, Bindman and Leese2006; Churchill et al, Reference Churchill, Owen and Singh2007; Kisely et al, Reference Kisely, Campbell and Preston2011; Burns et al, Reference Burns, Rugkasa and Molodynski2013). The OCTET 3 year follow-up found an association between CTO use and engagement with services, but whether this was due to the effects of the CTO or the severe course of the mental illness was not clear (Puntis et al, Reference Puntis, Rugkåsa and Burns2017). Rugkåsa and Burns have pointed out that the problematic nature of CTOs on clinical, ethical, legal, economical and professional grounds (Rugkåsa & Burns, Reference Rugkåsa and Burns2017) makes them inadequate for the purpose for which they were designed.
Most studies on the efficiency of CTOs have focused on outcome measures. In addition, the competing drive to reduce hospital use and the pressure on psychiatrists to manage risky behaviour is reflected by the quantitative focus of much research, e.g. hospital beds. It would be certainly rational to proceed with further RCTs to study the delivery of CTOs, but at this point it would be wise to stop and understand what we are trying to measure. Therefore, it is useful to examine global components that promote deficiencies of CTO use and attempt to improve them.
Factors that influence outcomes of CTOs
Targeting the right population
The use of CTOs tends to be higher for patients with psychotic disorders who lack insight and capacity to consent. Patients with low insight are more likely to experience relapse and be readmitted to the hospital (Churchill et al, Reference Churchill, Owen and Singh2007). Certainly, both patient factors (e.g. the nature of the illness, insight and personality factors) and CTO factors (e.g. conditions, duration, delivery and implementation) may all affect individual outcomes and overall efficacy. The utility of CTOs for substance misuse, personality disorders and management of risk of violence remains unclear (Ridgely et al, Reference Ridgely, Borum and Petrila2001), although it has been suggested that in the case of assisted out-patient treatment, they may reduce violence and risk of arrest (Link et al, Reference Link, Epperson and Perron2011). However, it has been demonstrated that it would take 238 OPC orders to prevent just one arrest (Kisely et al, Reference Kisely, Campbell and Preston2011).
It remains unclear for which populations CTOs are more successful. It may be that RCTs with negative results have not included the group of patients that could benefit the most. Determining the most appropriate populations may help clinicians to identify patients with similar characteristics, resulting in a successful treatment plan. It is, however, useful to consider the reasons behind the introduction of CTOs. Placing patients with traits of risky behaviours (based on genetic factors, patient's previous history and the nature of the disorder) will help supervision and monitoring on CTOs only if it can be combined with continuous clinical and therapeutic support, which could decrease the number of cases at risk for arrest. With this practice, ideally, the order could prevent patients from engaging in borderline behaviours. Second, such practice could eliminate the pressure on clinicians' side not to use a CTO, given the possibility of negative patient outcomes, e.g. harming themselves or others; this is a critical clinical consideration given the political and public pressures on clinicians. A CTO could be ordered only for patients with severe and persistent mental illness accompanied by high risk of aggression; this could act as a protective mechanism with the appropriate support, together with monitoring the progression of the patient's mental illness. However, there are still steps to be taken to improve the delivery of CTOs, including the need to efficiently and significantly reduce the rate of arrest in patients with high-risk profiles.
Clinical decision-making
The ‘potential for treatment compliance’ appears to be the primary focus in decision-making. Assessing this requires consideration of many factors, including the type of mental disorder, insight, treatability, history of adherence, engagement with services and risk. Decisions may also be significantly dependent upon a patient's insight. If insight is viewed as a neurobiological deficit of illness and amenable to treatment, the potential for improvement of a patient that could allow them to recover decision-making capacity (DMC) could provide an ethical justification for enforcing adherence in the patient's best interests (Dale, Reference Dale2010). One could argue that the best candidates for a CTO are patients who are able to consent. However, competent patients are not necessarily good candidates for a CTO. Patients with DMC have adequate insight to opt for voluntary community treatment without a CTO (Newton-Howes & Ryan, Reference Newton-Howes and Ryan2017). However, it is worth noting that while a patient's DMC puts them in a better position, insight is not necessarily connected with treatment adherence, especially if the patient has a history of high-risk behaviour or has a severe relapse profile (Dawson & Mullen, Reference Dawson and Mullen2008). The decision to discharge someone from a CTO not only concerns the development of insight, but also clinical improvement, adherence to treatment, and reduced risk to self or others (Link et al, Reference Link, Epperson and Perron2011).
Regarding patients with DMC, we are aligned with the opinion that those patients can express a preference for a future treatment when DMC might be lost, and that under such circumstances, treatment can proceed with a CTO (Szmukler, Reference Szmukler2015). However, shouldn't all patients be able to consent to future treatment at the time that they retain DMC? What happens with patients who do not retain DMC but have not consented in the past to the possibility of such treatment? A solution is to decrease the rate at which patients with no DMC are considered for CTOs. Reforms of mental health acts in many Australian jurisdictions now discourage forced psychiatric treatment in patients who have DMC (Callaghan & Ryan, Reference Callaghan and Ryan2016). Although using CTOs in patients with no DMC is considered ethical by many, this is with the assumption that CTOs do bring about an improvement into a patient's mental status.
Perspectives of patients about treatment
Patients tend to be ambivalent about CTOs. There is actual and perceived coercion and restriction, but the prospect of a shorter in-patient stay is appealing and may be perceived as less restrictive. Studies from New Zealand have found that patients generally find CTOs supportive (Gibbs et al, Reference Gibbs, Dawson and Ansley2005). For most, the restrictions did not unduly hinder them, and many valued the access to services. These orders can bring a sense of security and can be viewed as a step towards community stability, despite reduced treatment choice. Stability in the community can also reduce stigma, outweighing for some the associated feelings of restriction, but this would need parallel insight orientation work to have long-term benefits. Critical factors that affect patient experience include the quality of therapeutic relationships and support from services (Rugkåsa & Canvin, Reference Rugkåsa and Canvin2011).
A Norwegian study investigating positive patient outcomes reported that those experiencing assertive community treatment under a CTO had the highest recovery rates, compared with patients who were not placed under a CTO. In addition, those under a CTO found secure housing, sounder finances and access to the normal benefits offered by society to be of great importance (Lofthus et al, Reference Lofthus, Westerlund and Bjørgen2018). It is therefore essential to satisfy basic needs under a CTO, which may contribute to improved perceptions of patients towards their treatment. Other contributory factors towards a good recovery could involve flexibility, close communication, close monitoring of medication and social inclusion. Restriction under a CTO may be viewed more positively if there is flexibility and close communication regarding the treatment, which may change perceptions of CTOs as not just the enforcement of adherence to treatment but the provision of a safe environment for the patient's own clinical, personal and social recovery. Such changes in ordinal mental services would be difficult to achieve, but small steps towards this realisation could offer at least some improvement in the mental health of patients under a CTO, who might feel that their life is not progressing, which is negative for their recovery (Stensrud et al, Reference Stensrud, Høyer and Granerud2015).
Conclusion
CTOs aim to improve engagement and treatment adherence. One perspective is that their paternalistic style contributes to patients becoming disengaged from mental health services, while another is that supervision might help patients to improve their mental health when recovery is difficult to achieve. It would, however, be valuable to research the area further to justify the use of CTOs at an international level and ensure they are targeting the most appropriate populations, while enhancing decision parameters and the conditions under which a patient is placed on a CTO. Clinical research tends to use quantitative approaches, but the use of mixed method designs in research on patients' recovery can offer improved insights and provide novel perspectives. Each patient experiences treatment, their own mental status, and mental health services in a different way; this may contribute to the mixed results reported by various studies, along with the difficulties of obtaining reliable data and making comparisons across different methodologies. Thus, we need pluralistic approaches in addition to traditional study designs that can provide novel information regarding the delivery of CTOs.
Acknowledgements
We thank Dr Susham Gupta, Dr Peter MacRae and Professor George Ikkos.




eLetters
No eLetters have been published for this article.