Shared decision-making is a collaborative process in which clinicians and patients make treatment decisions in partnership. Both partners bring valuable contributions to this process: patients share their experiences, values and preferences, and clinicians support patients in clarifying these, as well as providing clinical expertise and evidence-based information about treatment options. Jointly, they aim to reach an agreement on the best way to proceed. Reference Coulter and Collins1–Reference Charles, Gafni and Whelan3
Shared decision-making is considered particularly relevant for preference-sensitive decisions, where there are several reasonable treatment options and evidence does not support a clear best choice. Different options require the balancing of possible benefits against potentially significant adverse or as yet unknown effects. Reference Charles, Gafni and Whelan3–5 Most medication decisions in mental health fall into this category, which makes psychiatric medication management an important area for shared decision-making. Reference Deegan6
There are good reasons for encouraging adoption of shared decision-making in mental health. Many patients wish for greater participation in treatment decisions. Reference Adams, Drake and Wolford7 In chronic conditions, where long-term healthcare decisions are required, studies have shown that shared decision-making improves satisfaction, adherence and well-being. Reference Joosten, DeFuentes-Merillas, de Weert, Sensky, van der Staak and de Jong8 Shared decision-making is at the core of recovery principles which promote autonomy and self-management skills, as well as being considered essential for delivering patient-centred care. Reference Barry and Edgman-Levitan9 National and international government initiatives, Reference Coulter and Collins1,10–13 such as the UK Health and Social Care Act 2012 and the US Patient Protection and Affordable Care Act 2010, endorse shared decision-making, as do professional bodies 14–Reference Chaplin and Quirk16 and practice guidelines. 17–21 Shared decision-making is an expected element of all NHS care (Health and Social Care Act 2012, s. 23, 26). Although there is evidence of its benefits, and many patients want greater involvement, Reference Adams, Drake and Wolford7 the adoption of shared decision-making into routine clinical practice continues to be slow, Reference Joseph-Williams, Edwards and Elwyn22,Reference Legare, Stacey, Turcotte, Cossi, Kryworuchko and Graham23 especially in mental health 24
A range of interventions has been developed to promote implementation of shared decision-making, predominantly in physical health. 25–Reference Lloyd, Joseph-Williams, Edwards, Rix and Elwyn28 Although this is an evolving area, relatively few interventions focus specifically on treatment decisions in mental health. Reference Deegan6,Reference Hamann, Mendel, Meier, Asani, Pausch and Leucht29–Reference Charles, Gafni and Whelan33 Evidence is sparse regarding the effectiveness of such interventions in general, Reference Legare, Stacey, Turcotte, Cossi, Kryworuchko and Graham23,25 and in mental health settings in particular, Reference Duncan, Best and Hagen33 although some promising results have been reported. These include a study of in-patients with schizophrenia or schizoaffective disorder who received five sessions of shared decision-making training; Reference Hamann, Mendel, Meier, Asani, Pausch and Leucht29 a multifaceted programme based on shared decision-making concepts for primary care physicians treating patients with depression; Reference Loh, Simon, Wills, Kriston, Niebling and Haerter30 a peer-run Decision Support Centre in the waiting area of a psychiatric medication clinic; Reference Deegan, Rapp, Holter and Riefer31 and online resources supporting shared decision-making. 32 The limited evidence available points towards interventions being more effective when involving healthcare professionals and patients together, rather than only targeting one group. Reference Legare, Stacey, Turcotte, Cossi, Kryworuchko and Graham23
The Shared Involvement in Medication Management Education (ShIMME) project was set up to promote shared decision-making of service users (the term ‘service users’ was used in the ShIMME project and has been retained here) in medication decisions by delivering a specially developed training programme to three key stakeholder groups: service users, care coordinators and psychiatrists. (In the context of the ShIMME project ‘care coordinator’ refers to psychiatric nurses, social workers, occupational therapists, psychologists, support workers, peer workers and students training in these disciplines.) To our knowledge this is the first UK-based project to deliver and evaluate such an intervention that targets multiple stakeholders simultaneously.
The project was a partnership between Cambridgeshire and Peterborough NHS Foundation Trust (CPFT) and Anglia Ruskin University. Reflecting the strong collaborative ethos, service users were active team members jointly with academic researchers, mental health practitioners and other professionals working within CPFT.
This paper describes the stages of the ShIMME project: consultations about shared decision-making, development and implementation of a pilot intervention, and evaluation of feedback. It is one of several articles relating to the project. Reference Kaminskiy, Ramon, Morant and Walker34–Reference Morant, Kaminskiy and Ramon36
Method
Consultation phase
The initial phase of the project involved a literature review and consultation with local stakeholders about the process of shared decision-making. Data were collected via focus groups with practitioners and users of adult mental health services in CPFT. Four focus groups were conducted with service users (n = 27), two with psychiatrists (n = 4), one with community psychiatric nurses (CPNs, n = 10), and one with care coordinators other than CPNs (n = 8). Four individual telephone interviews were also conducted with psychiatrists. Discussion was generated in response to open questions about current practice in medication management, how decisions should ideally be made, perceived barriers to and facilitators of shared decision-making, and how shared decision-making training should be conducted. Consultation groups lasted around 90 min and were audio recorded. The anonymised transcripts were analysed using thematic analysis, Reference Braun and Clarke37 conducted with NVivo software (www.qsrinternational.com). This involved a detailed exploration of transcript texts by two team members who worked in collaboration to iteratively develop themes.
The following themes about shared decision-making in medication management, which are presented in more detail elsewhere, Reference Kaminskiy, Ramon, Morant and Walker34 emerged from this analysis and fed into the development of the training programmes.
-
1 Ongoing respectful, trusting, open and honest relationships are paramount – service users' concerns and experiences need to be heard and taken seriously.
-
2 Differences of power in the consultation can be complex and a barrier to shared decision-making – clinicians can underestimate the effect this has.
-
3 Access to reliable, user-friendly information is essential, including information about reducing or coming off medication and adverse effects of medication.
-
4 All available treatment options should be considered, including non-pharmacological treatments.
-
5 The process of shared decision-making needs to be flexible, taking into account preferences and situations which may change over time. Acute stages of illness or crisis situations were identified as times when shared decision-making would be likely to be more problematic.
-
6 Broader stakeholders (beyond service user and prescribe! Reference Coulter and Collins1 ) have important roles in the shared decision-making process (e.g. other professionals, carers).
-
7 There is currently significant variation in medication management and the extent to which this involves shared decision-making.
Training intervention: design
A multidisciplinary working group including service users, academic researchers, psychiatrists, a mental health nurse and a pharmacist met regularly to develop the training intervention. The results of the consultations, literature review and examples of existing practice fed into the development.
Training was designed to be delivered to service users, care coordinators and psychiatrists in parallel but separate groups. The aim was to optimise the impact of the intervention by delivering it simultaneously to key stakeholders who are actively involved in medication management, while addressing the specific training needs and concerns of each group. Each group was facilitated by a service user trainer, and either a psychiatrist (for service user and psychiatrist groups) or a mental health nurse (for care coordinator groups), allowing participants to learn from two relevant perspectives.
The programme employed a range of interactive learning methods. These included specially commissioned video material showing different clinical scenarios, small group exercises, general group discussions, use of testimonials and role plays. The resource materials and hand-outs covered a diverse range of views and approaches, to raise awareness and stimulate discussion. All participants had access to the public section of the project website (www.shimme.arcusglobal.com) as well as a secure discussion forum for their group.
The training programmes for the three stakeholder groups covered the same core content:
-
• background to the project
-
• key components of shared decision-making in the clinical encounter and rationale for promoting shared decision-making
-
• barriers to and facilitators of shared decision-making
-
• awareness of the effects of power imbalances in psychiatric consultations
-
• developing collaborative relationships
-
• importance of clarifying personal preferences, values and experiences in shared decision-making
-
• the concept of a ‘meeting of two experts’ in the clinical encounter, with personal experience and clinical expertise complementing each other Reference Deegan and Drake38
-
• accessing and appraising information about medication, including examples of decision aids
-
• raising awareness of adjuncts or alternatives to medication
-
• addressing issues around coming off or reducing medication
-
• trialling of versions of three paper-based tools developed for supporting and recording the shared decision-making process
-
• information about useful websites.
In addition to the core content, the service user groups focused on:
-
• practising setting personal goals and identifying preferences
-
• making use of a personal well-being plan and self-help resources
-
• looking beyond medication to enhance well-being, drawing on Deegan's work on ‘personal medicine’ Reference Deegan39
-
• introduction to assertiveness
-
• how to access information about medication, including a talk by a National Health Service (NHS) trust mental health pharmacist, who was available for further discussion afterwards
-
• supported ‘hands-on’ experience exploring relevant websites.
Besides the core content, the care coordinator training focused on adopting the role of a ‘shared decision-making coach’, supporting service users to play a more active part in the shared decision-making process Reference O'Sullivan and Rae35 The programme for psychiatrists focused on competencies and resources that support embedding shared decision-making into routine clinical practice while acknowledging real-life challenges.
Training intervention: delivery
All training group participants were recruited from CPFT community mental health services: service users from the rehabilitation and recovery pathways; and professionals from these services and from assertive outreach teams. Service users were invited to participate by their care coordinators and psychiatrists and care coordinators were approached by team managers. In total, 47 service users, 12 psychiatrists and 35 care coordinators took part in the training.
Training was held in three different locations to reduce travelling for participants. Service users were reimbursed for travelling costs and received a fee (£40) for completing an evaluation before and after the programme.
The training was delivered in small group settings (2–12 participants), with each cohort completing their course of training together. An atmosphere of trust, acceptance and respect was encouraged. Participants had the opportunity for informal interaction before and after sessions as well as during breaks. Facilitators and project team members could be contacted between sessions for additional support.
Service user training groups were structured into four 2h sessions, meeting fortnightly After the training, two follow-up sessions were offered for ongoing support. Care coordinators met three times, at monthly intervals, for 1.5 h. Psychiatrists had two 2 h sessions, one month apart, with an online self-study component. For organisational reasons one multidisciplinary team of clinicians received their training together in a single day.
Evaluation
The experience and impact of the training intervention was evaluated by collecting quantitative and qualitative data anonymously from participants at different stages of the project.
After providing baseline data, participants and facilitators completed a short questionnaire after each session, and participants completed a longer one immediately after the final training session. The questionnaires explored what the participants had hoped to learn from the programme, their views on its content and impact, and feedback on particular sessions, practical aspects, teaching methods and support materials.
Analysis of quantitative and qualitative data examining the impact of the intervention at a 12-month follow-up, as well as an economic analysis, will be reported on separately.
Results
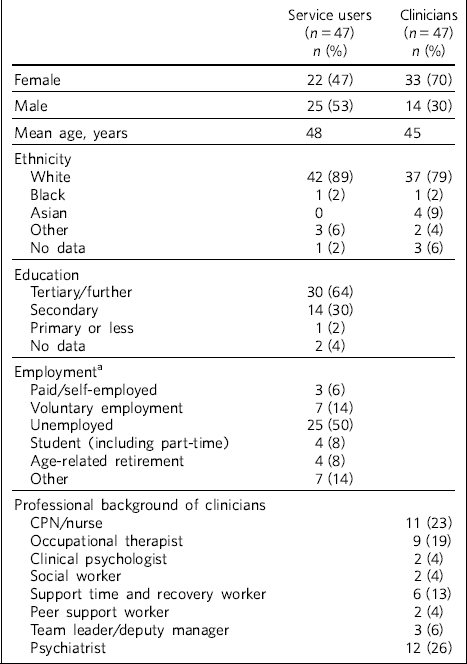
Although care coordinators and psychiatrists were mostly trained in separate groups, their demographic and feedback data are reported as one group of clinicians. Demographic and attendance data for service users and clinicians are shown in Table 1 and Table 2.
Table 1 Demographic characteristics of participants
| Service users (n = 47) n (%) |
Clinicians (n = 47) n (%) |
|
|---|---|---|
| Female | 22 (47) | 33 (70) |
| Male | 25 (53) | 14 (30) |
| Mean age, years | 48 | 45 |
| Ethnicity | ||
| White | 42 (89) | 37 (79) |
| Black | 1 (2) | 1 (2) |
| Asian | 0 | 4(9) |
| Other | 3 (6) | 2 (4) |
| No data | 1 (2) | 3 (6) |
| Education | ||
| Tertiary/further | 30 (64) | |
| Secondary | 14 (30) | |
| Primary or less | 1 (2) | |
| No data | 2 (4) | |
| Employment a | ||
| Paid/self-employed | 3 (6) | |
| Voluntary employment | 7 (14) | |
| Unemployed | 25 (50) | |
| Student (including part-time) | 4 (8) | |
| Age-related retirement | 4 (8) | |
| Other | 7 (14) | |
| Professional background of clinicians | ||
| CPN/nurse | 11 (23) | |
| Occupational therapist | 9 (19) | |
| Clinical psychologist | 2 (4) | |
| Social worker | 2 (4) | |
| Support time and recovery worker | 6 (13) | |
| Peer support worker | 2 (4) | |
| Team leader/deputy manager | 3 (6) | |
| Psychiatrist | 12 (26) | |
CPN, community psychiatric nurse.
a. More than one answer possible.
Table 2 Session attendance

| Patients | Care coordinators | Psychiatrists | |
|---|---|---|---|
| Sessions offered | 4 × 2 h | 3 × 1.5 h | 2 × 2 h |
| Cohorts training delivered to | 6 | 2 + 1 (team training day) | 2 + 1 (team training day) |
| Attendance | 37 (79%) attended at least 3 sessions of 4 |
20 of 21 (95%) attended at least 2 sessions of 3 14 attended team training day |
6 of 10 (60%) attended both training sessions 2 attended team training day |
The mean length of contact with mental health services for service users was 17 years. The most common reported diagnoses were schizophrenia, schizoaffective disorder or psychosis (n = 28, 60%), followed by depression (n = 12, 26%), bipolar affective disorder (n = 9, 19%), personality disorder (n = 5,11%), anxiety (n = 4, 9%) and post-traumatic stress disorder (n = 4, 9%). Some participants reported multiple diagnoses. The majority of service users received state benefits (n = 43, 92%), with n = 39 (83%) on a disability living allowance.
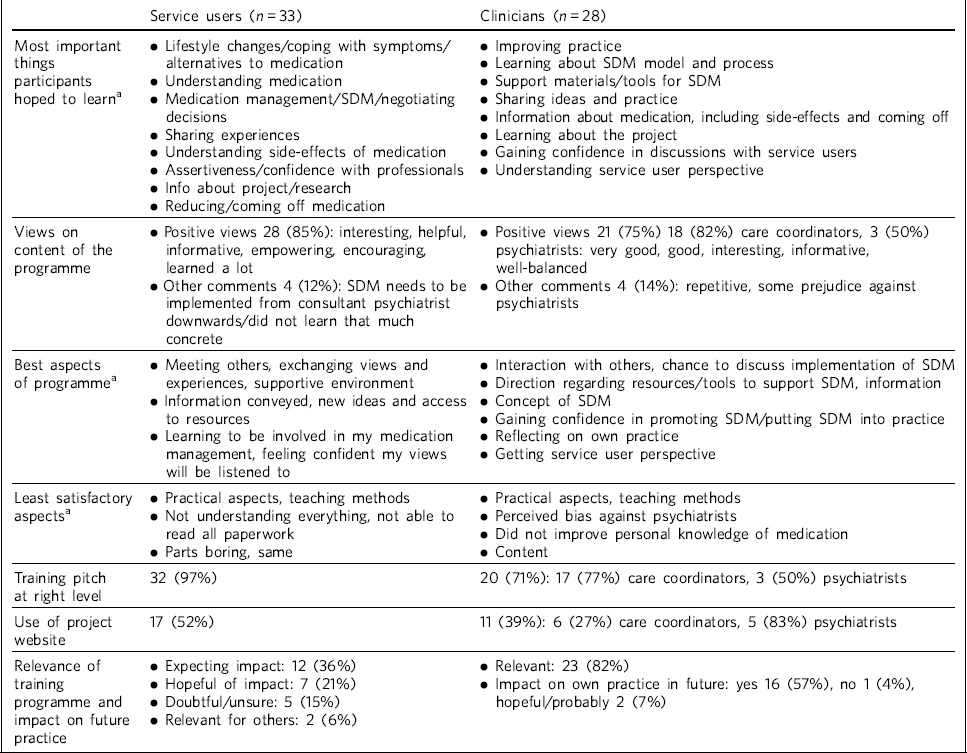
Immediate post-programme feedback was given by 61 (65%) participants: 33 (70%) service users and 28 (60%) clinicians, including 22 (63%) care coordinators and 6 (50%) psychiatrists. Before starting the programme, service users mostly hoped to learn about ways to cope with their symptoms not solely focused on medication, to understand their medication better and to negotiate decisions. Clinicians were particularly interested in improving their practice, learning about the model and process of shared decision-making, availability of support materials, and sharing experiences with colleagues.
Expectations of the programme were largely met in both groups, with the majority of participants expressing a positive view about its content. In all groups, the opportunity for discussion and exchange of views with peers was highlighted as the best aspect of the programme. In addition, service users valued the clarity of the information conveyed, access to resources and the prospect of greater collaboration in consultations. Clinicians also appreciated access to resources and the information given, as well as the opportunity to reflect on their own practice, particularly in the case of psychiatrists.
There was little negative feedback. Just over half of service users (n = 17, 52%) and the majority of clinicians (n = 20, 71%) did not identify any aspects of the programme as being ‘least satisfactory’. Some service users mentioned dissatisfaction with practical aspects or teaching methods, and a few referred to difficulties reading all the paperwork/understanding everything. A small number of psychiatrists expressed concerns about a perceived bias against their profession. Most participants felt the training was pitched at the right level. Use of the project website was variable, with about half of service users visiting it outside sessions. Most psychiatrists visited the website, but only a few care coordinators did. The online forum was not used by any of the groups.
Most clinicians rated the training programme as relevant to their clinical practice, but fewer expected that what they had learned would shape their future practice. Over half of service users expected or were at least hopeful that the programme would affect future practice.
A summary of the post-programme feedback is given in Table 3.
Table 3 Summary of feedback
| Service users (n = 33) | Clinicians (n = 28) | |
|---|---|---|
| Most important things participants hoped to learn a |
|
|
| Views on content of the programme |
|
|
| Best aspects of programme a |
|
|
| Least satisfactory aspects a |
|
|
| Training pitch at right level |
32 (97%) | 20 (71%): 17 (77%) care coordinators, 3 (50%) psychiatrists |
| Use of project website |
17 (52%) | 11 (39%): 6 (27%) care coordinators, 5 (83%) psychiatrists |
| Relevance of training programme and impact on future practice |
|
|
SDM, shared decision-making.
a. Listed in order of frequency.
Discussion
The ShIMME project was a small-scale exploratory project with an emphasis on service users co-leading in all aspects, while aiming to ensure the views of all key stakeholders were integrated into the development and delivery of the training intervention.
The training programme was well received overall, demonstrating the feasibility of providing group-based training in shared decision-making to service users and practitioners in NHS community settings. In this case, service user participants were drawn from the rehabilitation and recovery pathways which serve people with chronic and often severe mental health problems. Demographic data from participants indicated high levels of chronicity and disability. The positive feedback, good attendance and engagement from this group suggest that taking part in shared decision-making training is possible and worthwhile for people experiencing a range of mental health challenges.
Feedback indicated that service user participants were interested in being actively involved in managing their mental health, including gaining a better understanding of medication and exploring a range of other strategies to foster well-being. Clinicians showed an interest in improving their practice by learning about shared decision-making.
Members of all the stakeholder groups gave positive feedback about the group-based training, allowing for the exchange of ideas and experiences with peers. This was also reflected in facilitator comments about the supportive atmosphere and participants' enjoyment of meeting with each other in the service user groups. Interaction with peers seemed to be an important aspect of the whole programme.
There may also be advantages in service users and clinicians attending joint training groups, allowing participants from different backgrounds to work together on an equal basis and to gain a better understanding of others' perspectives without the pressures and structures of the clinical encounter. The involvement of carers and important others might bring further benefits.
The feedback about the content, approach and pitch of the teaching within the group of psychiatrists was not quite as positive as in the other groups. The reasons for this are likely to be multifaceted and would warrant further exploration, with possible adjustments of the programme. Away to enhance acceptability and engagement would be to encourage more psychiatrists to become involved in shared decision-making training and development of tools. Reference Lloyd, Joseph-Williams, Edwards, Rix and Elwyn28 Use of the project website was limited, in particular by care coordinators and service users. Technical difficulties with the website might have contributed to this, but comments during sessions indicated that some participants, particularly service users, had low IT confidence and limited internet access outside the training sessions. Future training programmes will need to provide non-digital resources, as well as supporting access and use of IT resources.
The project team developed three paper-based tools to support the process of shared decision-making, which were trialled in training groups and repeatedly revised. Although useful, these would need to be integrated into the existing electronic records system to be truly effective in promoting, supporting and documenting the process of shared decision-making without significantly affecting consultation time. At present this remains a challenge, but there have been some promising recent developments. Reference Lenert, Dunlea, Del Fiol and Kelly Hall40
Both groups of clinicians considered the training relevant to their clinical practice, although they appeared uncertain whether the programme would influence their future practice. This might be due to concerns about additional barriers to implementation or aspects of the training itself. Despite their positive feedback about the programme, service users were also cautious about its impact. This might reflect the perception that they have little influence in making significant changes to their healthcare delivery or doubts about positive initiatives being translated into clinical practice.
While this pilot programme had the limitations of a modest number of participants, not all of whom provided feedback, the consultation data from local stakeholders, the development of the training programme and the feedback from participants were all encouraging. Drawing on experiences from this project, CPFT has been working towards implementing shared decision-making across the trust by embedding shared decision-making into its procedures, raising awareness and offering training to practitioners across the trust (www.promise.global/sdm.html). The associated Recovery College (www.cpft.nhs.uk/about-us/recovery-college-east.htm), which is open to service users, family, friends and staff, also included training in shared decision-making. The pilot project benefitted from a supportive environment within the trust, and the success of implementation in other organisations would depend on their own local conditions.
The complexity and difficulty of implementing shared decision-making in a mental health setting should not be underestimated. Reference Morant, Kaminskiy and Ramon36,Reference Farelly, Lester, Rose, Birchwood, Marshall and Waheed41 For it to truly become a routine part of clinical practice, changes in attitudes and behaviours are necessary among all parties involved, as well as the wider society. Reference Morant, Kaminskiy and Ramon36,Reference Marshall and Bibby42 Psychiatrists are well placed to take on a leadership role in promoting shared decision-making within health services and should also be pivotal in explaining the benefits of increased patient autonomy and responsibility to the general community.
Funding
This project was funded by the National Institute for Health Research, Research for Patient Benefit (RfPB) Programme (PB-PG-0909-20054). Views expressed are those of the authors and do not necessarily represent those of the NHS, the NIHR or the Department of Health.
Acknowledgements
We thank all ShIMME project team members, service users and practitioners, as well as Dr Fiona Blake, Sheena Mooney, Mary Jane O'Sullivan and others for critically reviewing the manuscript. We are grateful to Prof. Matthew Large for his contributions as part of the BJPsych Bulletin Author Mentoring Scheme.






eLetters
No eLetters have been published for this article.