The current pharmacological treatment of major depressive disorder is far from perfect. In recent meta-analyses, the overall effect size of anti-depressant drug treatment was estimated at 0.31 (Reference Turner, Matthews and LinardatosTurner 2008). Some authors even conclude that there are no good grounds to prescribe anti-depressant drugs to any but the most severely depressed patients (Reference Kirsch, Deacon and Huedo-MedinaKirsch 2008). Part of this limited efficacy is undoubtedly due to the complexity of major depressive disorder itself. What DSM–IV (American Psychiatric Association 1994) calls major depressive disorder is probably a mixture of syndromes which are very different not only in clinical appearance but also in neurobiological background, making it impossible for any drug to be effective in the majority of people with major depressive disorder. Another explanation is that we are urgently in need of drugs that tackle more directly the core neurobiological dysfunctions in major depressive disorder. The article by McIsaac and colleagues on antiglucocorticoids in psychiatry offers an excellent example of the search for such drugs (McIsaac, pp. 242–249, this issue). They convincingly review the literature that situates HPA axis dysregulation at the core of the neurobiology of major depressive disorder. The logic of developing antidepressant drugs that directly target the HPA axis is compelling. But will such drugs be more efficient than our current treatments? A critical review of the literature calls for modesty.
Antiglucocorticoid drugs
Compounds that have been studied include ketoconazole, metyrapone, aminoglutethimide, dehydroepiandrosterone (DHEA) and glucocorticoid receptor agonists or antagonists. Very recently, the Cochrane collaboration published an extensive review on available trials with these drugs (Reference Gallagher, Malik and NewhamGallagher 2008). The overall examination of the eight available trials (totalling 211 patients) was not able to show significant differences in treatment response to antiglucocorticoids compared with placebo. Looking at the trials separately, however, some interesting results are reported. A randomised controlled trial (RCT) involving 63 individuals with major depressive disorder (Reference Jahn, Schick and KieferJahn 2004) showed that adding metyrapone to standard antidepressants induced a more rapid, more efficacious and sustained treatment response. This trial awaits confirmation.
A stronger case could be made for DHEA. A small RCT involving 22 people with major depressive disorder (Reference Wolkowitz, Reus and KeeblerWolkowitz 1999) reported that DHEA is an effective antidepressant. This was confirmed more recently in a larger RCT (Reference Schmidt, Daly and BlochSchmidt 2005) in midlife-onset major and minor depression, and in a controlled study involving people with HIV and subsyndromal depressive disorder (Reference Rabkin, McElhiney and RabkinRabkin 2006). However, it is most uncertain that the antidepressant properties of DHEA are HPA-axis related. Dehydroepiandrosterone and its metabolite DHEA-S exert numerous functions: acting as a precursor to testosterone and oestradiol, each of which independently has been associated with mood effects; modulation of multiple neurotransmitter systems (Reference Pérez-Neri, Montes and Ojeda-LópezPérez-Neri 2008); regulation of pro-inflammatory cytokines such as tumour necrosis factor alpha and interleukin-6, which have been shown to be involved in major depressive disorder (Reference Lanquillon, Drieg and Bening-Abu-ShachLanquillon, 2000); and exerting antiglucocorticoid properties, as long-term exposure to DHEA affects the transcriptional activity of the glucocorticoid receptor (Reference Saponaro, Guarnieri and PescarmonaSaponaro 2007).
Mifepristone (RU-486) blocks progesterone and, at higher doses, cortisol receptors. A few RCTs have studied the drug for psychotic major depressive disorder (Reference DeBattista, Belanoff and GlassDeBattista 2006; Reference Flores, Kenna and KellerFlores 2006). They indicate the efficacy of RU-486 in reducing psychotic symptoms at the beginning of treatment, but showed no significant effect on mood symptoms. An RCT involving people with bipolar disorder equally demonstrated no significant difference in mood symptoms between patients treated with RU-486 and those receiving placebo (Reference Young, Gallagher and WatsonYoung 2004).
CRH receptor antagonists
As hypersecretion of corticotropin-releasing hormone (CRH) is thought to be at the core of major depressive disorder neurobiology, antagonising the CRH type 1 (CRH1) receptor at the level of the pituitary seems the logical thing to do. An early uncontrolled study was promising (Reference Zobel, Nickel and KünzelZobel 2000), and several RCTs are currently underway. One recent RCT compared the efficacy of a CRH1 receptor antagonist (CP-316,311), sertraline and placebo in the treatment of 123 people with major depressive disorder (Reference Binneman, Feltner and KolluriBinneman 2008). The trial was terminated after a preliminary analysis on 30 patients in each group showed no evidence for the efficacy of CP-316,311. It is interesting to notice that sertraline showed an effect that was larger than that of the SSRIs in the meta-analysis by Reference Kirsch, Deacon and Huedo-MedinaKirsch (2008). The results of other such trials have to be awaited.
Taken together, there is no evidence that drugs targeting the HPA axis will work in the treatment of major depressive disorder, let alone work better than the current generation of antidepressants. One problem may be that the primary cause of HPA-axis dysregulation in major depressive disorder remains unclear. In vitro studies indicate a hypofunction of the glucocorticoid receptor as the primary mechanism (Reference Carvalho, Juruena and PapadopoulosCarvalho 2008), in which case glucocorticoid receptor agonists might be more appropriate than antagonists. Furthermore, it is important to realise that current antidepressant treatments targeting monoamine systems already exert important effects on HPA-axis function, as shown by in vitro, animal and human studies (Reference Mason and ParianteMason 2006). At this stage, the most realistic hope is that drugs such as DHEA, metyrapone and RU-486 will have an added value as (add-on) treatments for specific subgroups with major depressive disorder. This will have to be examined further, as will alternative targets within the HPA axis, such as the arginine vasopressin receptor 1B.
MCQs
-
1 The overall effect size of current antidepressant drugs is estimated to be:
-
a 21%
-
b 31%
-
c 41%
-
d 51%.
-
-
2 Metyrapone was found to be effective in the treatment of major depressive disorder:
-
a in monotherapy
-
b as an add-on treatment
-
c both of the above
-
d none of the above.
-
-
3 Dehydroepiandrosterone exerts an antidepressant effect by:
-
a modulating multiple neurotransmitter systems
-
b regulating pro-inflammatory cytokines, such as tumour necrosis factor alpha and interleukin-6
-
c modulating the transcriptional activity of the glucocorticoid receptor
-
d all of the above.
-
-
4 Mifepristone, which has been tested in patients with psychotic depression, is efficacious in:
-
a improving mood symptoms
-
b improving psychotic symptoms
-
c both of the above
-
d none of the above.
-
-
5 Current antidepressant treatments targeting monoamine systems already exert effects on HPA axis function. This has been shown by:
-
a in vitro studies
-
b animal studies
-
c human studies
-
d all of the above.
-
MCQ answers
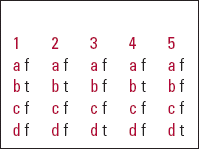
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | f | a | f | a | f | a | f | a | f |
| b | t | b | t | b | f | b | t | b | f |
| c | f | c | f | c | f | c | f | c | f |
| d | f | d | f | d | t | d | f | d | t |



eLetters
No eLetters have been published for this article.