There has been a growing international endorsement of recovery principles as a foundation for mental health practice and services (Reference SladeSlade 2009). This is supported by a broad consensus, including the Royal College of Psychiatrists (Future Vision Coalition 2009), consolidated in government policy (HM Government 2011) and elaborated in authoritative guidance (Reference Shepherd, Boardman and BurnsShepherd 2010). The College included the development of recovery-oriented practice in its Fair Deal campaign (Reference Fitch, Daw and BalmerFitch 2008), and a position statement by consultant psychiatrists recommends that recovery principles should be incorporated into psychiatric practice across the whole spectrum of specialties (South London and Maudsley NHS Foundation Trust 2010).
Recovery is not a model. Rather, it reflects a set of guiding values. The most widely cited definition of recovery is:
‘Recovery is a deeply personal, unique process of changing one's attitudes, values, feelings and goals, skills and/or roles. It is a way of living a satisfying, hopeful and contributing life even with the limitations caused by illness. Recovery involves the development of new meaning and purpose in one's life as one grows beyond the catastrophic effects of mental illness.’ (Reference AnthonyAnthony 1993)
This definition describes the concept of ‘personal recovery’ (moving forwards in life), as distinct from ‘clinical recovery’ (getting better from symptoms or problems), which has traditionally been the focus of mental health services (Reference SladeSlade 2009).
The recovery approach in practice
Broad political, service and professional commitments to recovery leave many details to be worked out in terms of what application of a recovery approach means in practice with respect to specific care groups or settings. It has been suggested that a key challenge to organisations and practitioners is in supporting a shift in the nature of day-to-day interactions and the quality of experience for people who use services. This has been characterised as a shift from a core emphasis on treatment and adherence to one that is about enabling people to successfully manage their own difficulties through supporting self-management and self-directed care (Reference Shepherd, Boardman and BurnsShepherd 2010).
Existing frameworks
Psychiatrists have always practised within a number of legal, ethical and good practice frameworks that require them to work collaboratively: the Mental Capacity Act 2005 and the guiding principles of the Mental Health Act 1983 Code of Practice (Department of Health 2008) stipulate that people taking decisions under these Acts must respect diversity and give patients the opportunity to be involved.
These principles are further enshrined by professional bodies. For example, the General Medical Council's Good Medical Practice (2009) emphasises ‘working in partnership with patients’, and the Royal College of Psychiatrist's competency-based curriculum (2010) requires trainee psychiatrists to demonstrate ‘an understanding of the need for involving patients in decisions, offering choices [and] respecting patient's views’ (p. 44). The terms and conditions of the National Health Service (NHS) consultant contract specify involving patients in decisionmaking about their treatment as an associated duty and responsibility. The National Institute for Health and Clinical Excellence (NICE) guidance on medicines adherence (2009a) recommends a number of interventions for increasing people's involvement in decision-making about medication. These standards are clearly also at the heart of recovery-based practice.
Putting principles into practice
One of the frequently raised objections to adopting recovery as a basis for practice is that it does not represent the fundamental shift in approach that it claims, but that it is a restatement of core principles and values already agreed as foundational for medical practice, and that in effect ‘we are doing it already’ (Reference Davidson, O'Connell and TondoraDavidson 2006; South London and Maudsley NHS Foundation Trust 2010). To a significant extent this is true. However, there is evidence to suggest that these commitments to the principles of collaborative and personcentred approaches have not always translated into practice (Reference Seale, Chaplin and LelliotSeale 2006; Reference Marshall and BibbyMarshall 2011). There are likely to be important and complex reasons for this gap between values and practice and explicitly engaging with recovery ideas may help to identify ways in which practice could develop to address this. Further, the adoption of recoverybased practice is accompanied by progressive policy that encourages working out in detail the implications of guiding values and developing auditable strategies for implementation (Reference Shepherd, Boardman and BurnsShepherd 2010; HM Government 2011), such that the way in which values are put into practice is evidenced.
Personal and self-determined perspectives
We would also suggest that the recovery approach not only reiterates but builds on these guiding values. In seeking to support the development of personal meaning and achievement of individually determined goals, recovery approaches would represent a significant shift of emphasis and commitment for psychiatric practice, rebalancing traditional focus on diagnosis and treatment with prioritisation of personal and self-determined perspectives. A key component of this shift would be the value and status that is ascribed to different forms of knowledge. Traditional prescribing practice is underpinned by scientific theory and a corresponding evidence base, central to which is the randomised controlled trial, which is taken as the gold standard in compiling treatment guidelines. The recovery approach values the evidence of personal narrative and places greater emphasis on the experiences and preferences of the individual. It has consequently been described as reflecting values-based practice, which is complementary to but also contrasted with evidence-based practice (Reference SladeSlade 2009).
The practitioner/service user relationship
Recovery-based practice, therefore, requires a change in the nature of the relationship between professionals and people using services. This has been identified as one of the ten key challenges with which organisations and services need to engage to support recovery (Reference Shepherd, Boardman and BurnsShepherd 2010), which may pivot around renegotiating issues of power, control and authority, as this journal has discussed before (Reference Roberts and HollinsRoberts 2007). This emphasis anticipates a transformation in relationships between practitioners and people who use services, such that both are considered experts, practitioners by virtue of their training and clinical experience and service users by virtue of their personal knowledge and lived experience (Reference DeeganDeegan 2006). The role of the professional is thus transformed from authority to coach who offers knowledge to support an individual in pursuing their personal goals (this journal, Reference Roberts and WolfsonRoberts 2004; Rethink 2011). It is important to emphasise that recovery-based practice does not, therefore, involve discarding scientific professional knowledge and evidence bases. Rather, these gain value in supporting outcomes when brought into a dialogue about how a person can actively participate in furthering their own recovery process (South London and Maudsley NHS Foundation Trust 2010).
In this article, we outline ways in which psychiatric practice could develop to reflect this shift, exploring how medication can best be understood to relate to the personal recovery process, describing practices that could support the use of medication as a self-management strategy and discussing how recovery-based practice could be maintained at times when people are unable to make choices or when their choices might compromise their own safety or the safety of others.
The role of medication in recovery: from ‘taking’ to ‘using’
Published personal narratives or ‘recovery stories’ and the results of research studies reflect a wide-ranging and highly individualised experience of psychiatric medication (Reference ColemanColeman 1999; Reference Mead and CopelandMead 2000; Reference Lapsley, Nikora and BlackLapsley 2002; Reference May, Gleeson and McGorryMay 2004; Reference DeeganDeegan 2005; Reference ReadRead 2009; Rethink 2009; Reference Cordle, Fradgely and CarsonCordle 2010; Reference Baker, Bovingdon and CampbellBaker 2011). Some people describe medication as essential to their recovery, often as a way of getting difficult symptoms under control and thus providing a foundation for building a meaningful life. Often there has been a process of finding the ‘right’ medication (one that is effective for them), which will have involved trial and error and negative experiences, as well as a process of coming to terms with the need to take medication for life to be manageable. Thus, accounts of positive and negative experiences of medication can coexist within the same story.
Concerns about medication are also often expressed, with some people feeling that the unpleasantness of the side-effects outweighs any benefits and could actually undermine recovery. There are accounts of people feeling disempowered and even traumatised by lack of information and choice about medication, including compulsory treatment. There are many accounts of how people have found other approaches to managing their difficulties to be beneficial, both alongside or instead of medication. These include psychosocial interventions and self-help strategies, described as ‘wellness tools’ (Reference Copeland and MeadCopeland 2004), ‘personal medicines’ (Reference DeeganDeegan 2005) or ‘self-management’ (Rethink 2003). However, many accounts describe these options as having limited availability or not being considered or offered with the same frequency as medication.
Personal recovery is a unique, individual process, so it is unsurprising that medication has played very different roles, and at different times, in the recovery journeys of different people. We suggest that it is not only the potential effectiveness of the medication itself but the nature of the relationship that people have with their medication that can be thought of as supportive or unsupportive of personal recovery. The traditional experience has been a passive process of taking medication, following the direction of an expert professional. Indeed, the term ‘prescribing’ has these connotations, with the Oxford English Dictionary definition outside of medical contexts being ‘to state authoritatively that an action or procedure should be carried out’. A key component of recovery is taking up an active stance in relation to one's own difficulties. This would be better supported by a relationship with medication that is characterised by actively using it (Reference DeeganDeegan 1996), by making informed choices about its effects and how these relate to desired outcomes. This has been described as ‘using medication thoughtfully’ (Reference Lapsley, Nikora and BlackLapsley 2002: p. 65). The role of medication in supporting personal recovery can, therefore, be reconceptualised not just as a treatment but as one tool among many that a person can choose to use to help them achieve their personal recovery goals (Reference DeeganDeegan 1995; Reference Mead and CopelandMead 2000; Reference SladeSlade 2009). It is a tool that may gain in value and benefit if supported by the person's thought-out acceptance and commitment.
We recognise that, in some circumstances of risk and incapacity, people cannot fully participate in making choices about whether and how to use medication. While we believe these circumstances to be exceptional,Footnote a they are also the most problematic in terms of working out the detail of putting recovery principles into practice and we will discuss them in more detail later in this article.
Supporting an active stance in relation to medication
Making shared decision-making a reality
Shared decision-making, in which the expertise of both parties is recognised, has been identified as a desirable approach to prescribing practice by policy makers and healthcare professionals. There is evidence that is it effective (Reference Marshall and BibbyMarshall 2011) and that it supports recovery values (Reference Deegan and DrakeDeegan 2006). However, the accounts of people using mental health services, along with observations and surveys of psychiatric practice, all suggest that it is not fully implemented, with psychiatrists often using persuasion to improve adherence (Reference Seale, Chaplin and LelliotSeale 2006, Reference Seale, Chaplin and Lelliot2007; Reference Ranz and ManciniRanz 2008; Reference Baker, Bovingdon and CampbellBaker 2011). This has also led to a tendency for mental health workers to withhold information about possible adverse effects of medication (Reference Pollock, Grime and BakerPollock 2004; Reference Chaplin, Lelliot and QuirkChaplin 2007, this journal). For psychiatrists working within evidence-based frameworks, this is likely to reflect a view, based on training and research, that taking medication is in people's best interests. This contrasts with a recovery-based approach, with its emphasis on personal experience, choice and responsibility, allowing ‘the dignity of risk and the right to failure’ (Reference DeeganDeegan 2005) and the opportunity to learn from experience. For many psychiatrists, this will inevitably be a source of dilemmas and discomfort and, in addition to the possible strategies that we describe here, psychiatrists will need professional and organisational support that recognises that genuinely sharing decisions requires sharing of responsibility and risk.
Informing patients
There are many possible sources of information that people can use to support their decision-making about medication. However, they are all subject to well-understood biases and limitations. The outcomes and availability of data from randomised controlled trials, which are the cornerstone of the prescribing evidence base, may be influenced by funding sources, such as pharmaceutical companies, and will also say little about the experience of individuals or the longerterm impact of medications (Reference MoncrieffMoncrieff 2008; Reference ReadRead 2009; Reference SladeSlade 2009). Drawing on support from peers with their own experiences of mental health difficulties and referring people to the recovery stories of others has been identified as valuable for the personal recovery process (Reference SladeSlade 2009). However, personal accounts of medication usage will be representative only of one individual's experience and will be influenced by their personal values, priorities and lifestyle. Therefore, an important task in recovery-based prescribing would be to help people to be aware of both the range of sources and how to evaluate them. Some useful resources, reflecting a range of perspectives, are shown in Box 1.
BOX 1 Useful online sources of information about medication
Choice and medication website: www.choiceandmedication.org.uk
Offers people information about medication for mental health to enable them to make informed decisions.
National Prescribing Centre patient decision aids (anxiety, insomnia, schizophrenia): www.npci.org.uk/patient_decision_aids
The NPC has developed patient decision aids to help patients make difficult decisions about treatment when they need to weigh benefits against risks.
Mind information booklets: www.mind.org.uk/help/medical_and_alternative_care
Provide free information about a range of treatments, including medication, psychological and complementary therapies.
Rethink website: www.rethink.org/living_with_mental_illness/treatment_and_therapy/index.html Provides information about a range of treatments and medication, including Only the Best (Rethink 2006), a guide to help people to find the best antipsychotic and mood stabiliser medication for them.
Coming Off Psychiatric Medication website: www.comingoff.com
Gives information about psychiatric medication and the withdrawal process, from people who have used and withdrawn from medication and clinicians who have supported this process.
Alternative strategies
Alongside supporting people to weigh the costs and benefits of medication options, a recovery-based approach would also incorporate raising awareness of alternative strategies that people have found useful in managing their difficulties. There is now substantial evidence for the benefits of supporting people in self-management across the whole of medicine, although clinicians may need help to develop the relevant attitudes and skills (Health Foundation 2011). This may be an area where psychiatrists currently feel less confident and less equipped (Reference Ranz and ManciniRanz 2008). The College's competency-based curriculum for psychiatric training (Royal College of Psychiatrists 2010) explicitly requires trainees to be ‘aware of strategies to enhance patient understanding and potential self-management’ (p. 57), dicati inng that this is supported as a future direction for the profession. Reference DeeganDeegan (2008a) describes how questions and information about ‘personal medicines’ can be included in psychiatric consultations. A wealth of evidence is available to demonstrate the impact of particular activities on well-being, which is summarised in the Ten Keys for Happier Living that underpin the current strategy from Action for Happiness (www.actionforhappiness.org). These could be used by psychiatrists as the basis of social prescribing (Care Services Improvement Partnership 2009), where people are told how to link to a variety of activities that could improve their mental health, including arts, exercise and time in the natural environment, or to direct people towards techniques to improve their mood and management of emotions.
Selecting the best tool for the individual
Exploring information about medication and personal medicines may guide a decision but ultimately there will be a need to evaluate which tools are useful for a particular person. Within a recovery-based approach, decisions about using or changing medications, including different types or doses, can be treated as collaborative experiments (Reference Deegan and DrakeDeegan 2006). This involves agreeing on the aim of using or changing the medication, identifying ways of monitoring the effects and agreeing what action will be taken if the experiment is unsuccessful. A simple measuring scale or other self-monitoring tool might be used as a way of keeping track of experience over time, providing a basis for discussing the results of the experiment. The person's informal support network might also be involved (Reference DeeganDeegan 1995). In this way, decisions can be based on the evidence of research, experiences of clinicians and other people who have taken the medication, and a structured approach to collecting the evidence of personal experience.
Balancing demands
Fully engaging with shared decision-making is a demanding process for clinicians in requiring more time and practical resources but also in the degree of uncertainty for both the prescriber and the person taking medication. This may contribute to the disparity between aspirations for practice and the lived experience of people taking medication as described above. However, there is evidence that the way in which prescribing is carried out influences how effectively medicines are used and even the effectiveness of the medicines themselves (Reference Britten, Riley and MorganBritten 2010, this journal; Reference MintzMintz 2011). Using the recovery stories of others can be a helpful strategy to inspire hope for people engaged in the personal recovery process and, in this spirit, we offer in Box 2 an example of a successful approach to prescribing based on recovery principles.
BOX 2 Decision support centres
Reference DeeganDeegan et al (2008) describe an evaluation of a peer-run decision support centre, established to assist shared decision-making practice at an out-patient psychiatric medication clinic in the mid-west of the USA. People attending for medication appointments were given 30 minutes in the centre before meeting with their prescriber, where they received support from peers in using a computer program to:
-
• hear personal accounts of recovery;
-
• reflect on their ‘personal medicines’ (things they did to support their own wellness);
-
• rate their symptoms and functioning since their last visit;
-
• report how they had been using their medication;
-
• identify common concerns and goals for their meeting with the prescriber.
Their responses were then forwarded electronically to the prescriber and the report was reviewed in the consultation. Decision-making aids (such as a balance sheet of costs and benefits) were then used to make shared decisions about how the person would use their medication or other strategies they had identified. The centre also provided informal peer support and access to information about medication via the internet.
The evaluation comprised focus groups, which included medical practitioners working at the clinic and clients. Medical practitioners felt that they gained a more holistic understanding of their client's needs and clients could communicate more effectively about their concerns so that they were able to be more actively involved in the prescribing process. Clients found that the personal accounts of recovery inspired hope. They also felt that using the computer program meant that their concerns were more likely to be heard and they found it useful to be able to track their progress.
Resolving conflicting perspectives
Supporting personal meanings
Finding meaning and developing a personally satisfactory account of mental health difficulties and distress is described as a key component of personal recovery (Reference May, Gleeson and McGorryMay 2004; Reference SladeSlade 2009). However, these accounts are often divergent from the biomedical and biopsychosocial models espoused by the majority of mental health workers. ‘Lay understandings’ have been identified as a factor in non-adherence to psychotropic medications, as highlighted in this journal (Reference Britten, Riley and MorganBritten 2010) and are often understood as reflecting a lack of insight (Reference SladeSlade 2009), which may then become a target for intervention in itself. Such individual clinical conflicts take place within the context of considerable controversy about the mode of action of psychiatric medication, whether it specifically treats an underlying brain disease or operates through a more generalised sedating or stimulant effect. These hypotheses relate to wider unresolved debates about the causes of mental distress or disorder and the relative role of biological, psychological and social factors (Reference BregginBreggin 1993; Reference Read, Mosher, Bentall, Read, Mosher and BentallRead 2004; Reference MoncrieffMoncrieff 2008).
To support personal recovery, practitioners may need to engage with people in a process of searching for meanings that are useful to them, rather than providing a particular framework for understanding their experience. This corresponds to the shift from ‘expert’ to ‘coach’ mentioned above. It would require the practitioner to attend to the person's existing ideas and beliefs about what has happened, before discussing with the person how there are multiple ways of making sense of, and therefore attempting to address, their problems and thinking with them about what they feel would be most useful to them (Reference May, Gleeson and McGorryMay 2004). Many people with psychosis value their experiences, or some aspect of them, and it is possible to support people to find ways of living with unusual experiences and beliefs that are less distressing or problematic for them and others (Reference Romme and EscherRomme 1993; Reference ColemanColeman 1999; Reference KnightKnight 2005). However, there are others who believe that experiences are best understood as an illness that needs to be treated (Reference AllenAllen 2006). A biomedical or biopsychosocial model should, therefore, be represented in this discussion, along with the use of medication as an associated strategy. Long-term perspectives illustrate how preferred models of understanding and choices of treatment shift over time and, because recovery is an ongoing process, it seems likely that support for people in the search for meaning will also need to be continuing and responsive to new experiences.
Although an individual may not favour a biomedical explanation of their difficulties or experiences, they may still find medication useful in achieving their recovery goals. Reference MoncrieffMoncrieff (2008) argues that, despite uncertainty about how psychiatric drugs operate, the individual may still consider their effects desirable, for example in helping them feel calmer, less frightened or confused and improving sleep. Discussion of medication could, therefore, focus on its likely effects and whether the individual would find these helpful. Rather than viewing medication as a specifically biomedical treatment for a mental illness, framing it as an empirical strategy, with costs and benefits, that people can use to manage their mental states is supportive of the personal meanings necessary for recovery and may serve to resolve conflicting perspectives.
Safety and compulsion
The call from the recovery movement for increased responsibility for, and respect for the choices of, people using mental health services has led to concerns about potential negligence, described as ‘leaving people to rot with their rights on’ (Reference Davidson, O'Connell and TondoraDavidson 2006). At such times, it would be both irresponsible and unsupportive of longer-term personal recovery for mental health workers not to intervene, as this journal has reported (Reference Roberts, Dorkins and WooldridgeRoberts 2008). Under these circumstances, depending on whether someone is detained, practice is guided by either the Mental Capacity Act 2005 or the Mental Health Act 1983 Code of Practice (Department of Health 2008).
The Wellness Recovery Action Plan
Both people with lived experience and advocates of recovery-based practice acknowledge the need for others to intervene at times of crisis. The development of a ‘crisis plan’, outlining preferred supporters, interventions and criteria for activating and inactivating the plan, is a core component of a Wellness Recovery Action Plan, a widely used self-management tool (Reference Copeland and MeadCopeland 2004). This approach can maintain the person's involvement and ensure that treatment decisions continue to be guided by their values and preferences (Reference Deegan and DrakeDeegan 2006). Helping people to prepare such documents at times when they are stable is therefore essential to a recovery approach. However, it is important to be honest with people about the limitations on the practitioner in respecting their choices (Reference Noordsy, Torrey and MeadNoordsy 2000). Crisis plans can be made in the form of advance statements, as described in the Mental Capacity Act. However, with the exception of advance decisions (which are refusals of particular treatments), these can be overridden, and in general such statements are trumped by the amendments to the Mental Health Act made in 2007.
Exploring strategies to maintain recovery
Where it is not possible to abide by a person's previously expressed preferences (either in the absence of a plan or where it has proved insufficient), the Mental Health Act Code of Practice (Department of Health 2008) requires that psychiatrists engage fully with the person's wishes. Reference Roberts, Dorkins and WooldridgeRoberts and colleagues (2008) describe in this journal a number of strategies through which a recovery-based process can be maintained in relation to medication when someone is detained. These include exploring people's previous experiences of medication, the ways in which they are making sense of their difficulties and what other strategies they might find helpful, as well as offering people choice from a more limited range of options, such as choosing between possible medications and when, where and how they would like the medication administered. As many people with mental health difficulties are distressed by the idea of putting themselves or others at risk (Reference Langan and LindowLangan 2004), a collaborative approach to risk assessment and management, where the person is engaged in a process of identifying strategies to help them remain safe, is likely to be both effective and beneficial.
Distinguishing ‘me’ from ‘it’
Reference Mead and HiltonMead & Hilton (2003) describe how a strategy of externalising problems derived from White's (1990) approach to narrative therapy can be effective as part of this process. This approach capitalises on the value in recovery of distinguishing ‘me’ from ‘it’ (Reference Davidson and StraussDavidson 1992) by encouraging people to see the problem as a separate entity from themselves, to allow them to think about the influence the problem is having on their lives and how they might take action against it. The person supporting them can then unite with them in their struggle against the problem. Instead of focusing on controlling risky behaviours, this approach could enable a dialogue with the person about their preferred ways of behaving (which are likely to be less risky) and whether and how medication, alongside other strategies, could support them in resisting the influence of the problem.
Post-crisis planning
Personal recovery is conceptualised as a journey in which there will be inevitable setbacks, so times of crisis and compulsory treatment could usefully be recontextualised as learning experiences, rather than thought of as failures. The Wellness Recovery Action Plan concludes with ‘post-crisis planning’, which provides an opportunity, after a crisis has resolved, to reflect on how things could have been handled differently. As part of this process, it may be helpful for mental health workers to find a way to acknowledge the person's feelings about any actions that were taken against their wishes and to negotiate with them to develop or revise a crisis plan to prevent similar situations in future, as previously proposed in this journal (Reference Copeland and MeadCopeland 2008). The National Institute forbHealth and Clinical Excellence (2009b) guideline on schizophrenia recommends that people should be given the opportunity to record their own account of rapid tranquillisation in their notes and this approach could be extended to other forms of compulsory treatment and people with other diagnoses.
Enforced medication outside of crises
There may be times outside of clear crisis situations where there is a perceived need to enforce medication as a strategy to manage future risk (Reference Langan and LindowLangan 2004). A full discussion of a recovery-based approach to risk management is beyond the scope of this article. However, such an approach, involving working collaboratively with the person using services, emphasising strengths and supporting choice and the development of self-management skills, has been identified as best practice (Department of Health 2007). Again, there has been only slow and partial implementation of this guidance, and ‘changing the way we approach risk assessment and management’ is identified as another of the key organisational challenges for implementing recovery (Reference Shepherd, Boardman and BurnsShepherd 2010), which will be supported by an NHS Confederation guidance paper in due course (Reference Boardman and RobertsBoardman 2013).
Conclusions
It is apparent that recovery values reflect those already underpinning good psychiatric practice and overlap with commitments already made to future professional competencies. However, there is evidence to suggest that these are not consistently translated into practice and this may account for the experiences of people using services, the voices of whom have substantially contributed to the development of the recovery approach and the ambitions for system transformation that it embodies. We have attempted to describe how recovery values would require a fundamental reorientation in the relationship between psychiatrists and people using services, such that personal experiences and meanings take on equal value to scientific evidence and theory so that practice is explicitly driven by values such as inclusion, choice and empowerment.
Adopting recovery as a basis for practice would require psychiatrists to put people's goals and preferences in the foreground, offer their knowledge as relevant and help people to make informed choices about how to make sense of and manage their difficulties. We believe that adopting the practices described in this article would support a recovery-based approach to the use of medication.
Within the Devon Partnership NHS Trust, we have developed good practice guidance to for practitioners on implementing recovery principles in relation to prescribing and medicines management, which incorporates these and other strategies (Devon Partnership Trust Recovery and Independent Living Professional Group 2010). This was adopted by the College's Fair Deal campaign as an illustration of implementing recovery in practice. It has much in common with established good practice principles, but it also extends these to a degree that has been described as a ‘paradigm shift’ (Reference SladeSlade 2009), with the attendant challenge for practitioners to develop new ways of thinking about and relating to people experiencing mental health difficulties. There will need to be an ongoing process of working out what it means in practice for all mental health workers and, in particular, of continually engaging with the tension between promoting autonomy and professional responsibilities.
We offer our thoughts and locally developed guidance as a contribution to continuing development and debate. We also recognise that there is a need for further work focused on the implementation of these ideas and evaluation of whether they effectively support people in using medication successfully to support them in their personal recovery.
MCQs
Select the single best option for each question stem
-
1 Services that focus on personal recovery:
-
a are aimed at reducing symptoms
-
b ensure that people follow their treatment plans
-
c offer standardised interventions
-
d support people in building a meaningful and valued life through personalised strategies
-
e do not provide medication.
-
-
2 Medication supports personal recovery:
-
a by effectively treating symptoms
-
b by effectively preventing relapse
-
c by providing a tool that people can use to achieve personal recovery goals
-
d because it is the only available option for many people
-
e only when the person agrees with their diagnosis.
-
-
3 People can be supported to take an active stance towards their medication by:
-
a a process of shared decision-making in which they make informed choices
-
b being given clear instructions on how to take their medication correctly
-
c being told that medication is essential to manage their symptoms
-
d being given reassurance that professionals know which medication they need
-
e having their medication changed if they continue to experience symptoms.
-
-
4 In a recovery-focused conversation about medication:
-
a the person is encouraged to accept their diagnosis
-
b there is a discussion about the likely effects of the medication and whether these will help the person reach their recovery goals
-
c the person is not given much information about the medication, as this can reduce adherence
-
d the person is told that they will need medication for the rest of their life
-
e the person is encouraged not to ask others about their experience of medication.
-
-
5 When a person has a crisis plan for use at times when they cannot safely make choices for themselves:
-
a the crisis plan should be respected at all times
-
b the crisis plan should be ignored if the person is detained under the Mental Health Act
-
c the crisis plan should be ignored if the person's relatives disagree with it
-
d the crisis plan may provide a useful guide to the person's wishes but can be overridden by the Mental Health Act
-
e if the plan could not be followed in a crisis, the person should be discouraged from using a crisis plan in future.
-
MCQ answers
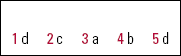
| 1 | d | 2 | c | 3 | a | 4 | b | 5 | d |



eLetters
No eLetters have been published for this article.