First-episode psychoses, including schizophrenia, are currently best understood as neurodevelopmental illnesses arising from the interaction of assorted biological and psychosocial factors. Although an excess loading of genetic susceptibility and environmental risk factors may manifest in childhood through a range of non-specific, subtle behavioural changes, the vulnerability is usually silent until the onset of prodromal or psychotic symptoms in the mid-teens to early 20s (Reference Welham, Isohanni and JonesWelham 2009). Early intervention services were established on the basis of a number of fundamental principles. These include the notions (Reference McGlashan and JohannessenMcGlashan 1996; Reference McGorry, Edwards and MihalopoulosMcGorry 1996) that:
-
• intervention in the early stages of psychosis can change the trajectory of illness and ameliorate long-term prognosis;
-
• multicomponent intervention promotes psychosocial recovery, and reduces iatrogenic damage and carer burden;
-
• early targeting of non-responders can reduce treatment resistance.
The concept of the ‘critical period’ (Reference Birchwood, Todd and JacksonBirchwood 1998) – the first 3–5 years from psychosis onset, which in most people coincide with maximal neuronal and psychosocial plasticity and when, theoretically, the greatest impact on illness can be made – facilitated extension of the approach to include ‘indicated prevention’ in the prodromal stage (Reference Yung, Phillips and YuenYung 2003). In indicated prevention, special intervention programmes are targeted at individuals who are showing early signs and other related problem behaviours. The rationale was complemented by the assumptions of a clinical staging model proposing that treatment in the early rather than late stages of illness is more benign and results in better response and prognosis, thus minimising the need for traumatic and restrictive forms of care, including involuntary hospital admissions (Reference McGorry, Hickie and YungMcGorry 2006, Reference McGorry, Johanessen and Lewis2010a).
Melbourne, Australia, has a strong case for being considered the cradle of early intervention, with the pioneering Early Psychosis Prevention and Intervention Centre (EPPIC) established in 1992 (Reference McGorry, Edwards and MihalopoulosMcGorry 1996). The service, currently known as Orygen Youth Health Research Centre, subsequently expanded to provide intervention for all youth mental health problems. More recently, it drove the development of the ‘headspace’ consortium, a federally funded national youth mental health initiative to promote and support early intervention for young people with mental and substance use disorders (Reference McGorry, Tanti and StokesMcGorry 2007). There has been rapid expansion of early intervention services in many regions, notably Australia, Canada, Scandinavia and the UK. In England alone, 118 services are now operating (Reference Tiffin and GloverTiffin 2007).
It is important to note that ‘early intervention’ may refer to one of three service aims, all of which require different strategies (Reference SinghSingh 2010). It can mean improving outcomes in established cases of psychosis; or having an early detection component (for example, through community awareness campaigns and primary care education) to identify hidden morbidity, with the intention of reducing the mean duration of untreated psychosis (DUP) in the service’s cohort; or preventing the emergence of psychosis in individuals with prodromal symptoms through the establishment of prodrome clinics for help-seeking patients (Reference SinghSingh 2007). The presence of prodrome clinics and community awareness campaigns varies considerably, depending both on resources and embedded research endeavours. Although there is emerging evidence of the value of these components, they are often threatened by lack of finances. It is essential that service planners safeguard consistent funding to reflect these broader aims.
Strengths and limitations of variations in service models
Although early intervention services generally follow standardised principles of care (Box 1), they may vary in their model of service delivery (Box 2). Each variation has its strengths and weaknesses, and the model adopted in any particular service is often influenced primarily by feasibility and economies of scale rather than ideological frameworks.
BOX 1 Key principles of service provision in early psychosis
-
• Assertive community treatment model to facilitate the early identification and management of those with first-episode psychosis
-
• Youth-friendly in-patient and out-patient services
-
• Multidisciplinary, phase-oriented treatment coordinated by a case manager
-
• Focus on early detection, recovery and relapse prevention
-
• Low-dose antipsychotic medication
-
• Targeted psychological interventions
-
• Management of secondary comorbid conditions, including affective and substance use disorders
-
• Engagement of families, including the provision of psychoeducation
-
• Psychosocial recovery focus, including educational, vocational and residential support, with the aim of maintaining community engagement
BOX 2 Differences in service configuration
-
• Age range
-
• Case-load
-
• Duration of care
-
• Embedded v. stand-alone
-
• Centralised v. hub-and-spoke
-
• Hours of business
-
• Inclusion of research programmes
-
• Inclusion of specialised components
-
• Provision of health promotion and community awareness
-
• Provision of physical health monitoring
Age range
Although age ranges vary, services are generally divided into those with a low age cut-off (typically 24 or 25 years of age), to maintain a youth focus, and those with a higher cut-off (30 or even 40 years of age), to include as many people with early psychosis as possible. The principal advantage of a youth-focused service is that it provides developmentally appropriate interventions to the majority of those with a first-episode psychosis. The disadvantages are twofold.
First, youth-focused services generally have a cutoff at age 25, and anyone older is treated by generic adult mental health services. This is a significant issue, as a substantial cohort develops psychosis between 25 and 35 years of age, especially women and people with bipolar disorder. Such patients are then treated in generic services, which are universally characterised by long delays in treating first-episode psychosis (Reference Norman and MallaNorman 2001; Reference Farooq, Large and NielssenFarooq 2009) as well as by iatrogenic damage (see the subsection on in-patient units later in this article), which leads to high rates of disengagement (Reference Garety and RiggGarety 2001; Reference McGorry, Johanessen and LewisMcGorry 2010a). Rather than compromising a youth-specific model at the expense of including the maximum number of people with first-episode psychosis, it may be better to compel the argument for promoting service reform in adult mental health by developing and resourcing similar models of early intervention across the age range.
Second, youth-focused services by definition treat those under 18 as well as those up to the mid-20s age cut-off, thus disrupting the traditional demarcation between child and adult psychiatry. This has resulted in debate as to whether early intervention services (and youth mental health services generally) are best managed by child and adolescent mental health services, adult mental health services or whether they should constitute separate entities (Reference Birleson and VanceBirleson 2008; Reference McGorry, Hazell and HickieMcGorry 2008). Although the development of youth-specific services appears intuitive and has an emerging evidence base in support of service reform (Reference McGorry, Tanti and StokesMcGorry 2007), there appears to be no definitive answer as to where they are best placed. The local solution in Victoria, Australia, has been to introduce health reform aimed at facilitating dedicated service streams planned and managed across a broad 0–25 years framework (Department of Health 2009).
Case-loads
Most early intervention services were established with fixed case-loads of 15 patients. However, many have found that service delivery has been compromised by budgetary constraints, resource realignment that lags behind demand, and delays in recruitment and infrastructure establishment (Reference Lester, Birchwood and BryanLester 2009; Reference Murphy, Simms and DowlingMurphy 2009). This often results in higher case-loads, compromising holistic early intervention treatment and/or more focused, evidence-based treatment of specific comorbid conditions such as post-traumatic stress disorder (PTSD). In the UK, where meeting target case-loads of 15 is linked to ongoing funding, case-loads tend to be maintained at the expense of other survival strategies, such as early discharge, age-range restriction, imposing waiting lists and reducing community development work (Reference Lester, Birchwood and BryanLester 2009).
In Australia, some services (EPPIC, for example) were originally set up with higher case-loads (Reference McGorry, Edwards and MihalopoulosMcGorry 1996) or have introduced the concept of ‘step-down’ care to cater for individuals who are either subject to a shared care arrangement or need minimal contact, allowing increased case-loads without compromising patient care (Reference McGorry, Nelson and AmmingerMurphy 2009).
Finally, there is increasing recognition of the need to develop ultra-intensive case management teams, with case-loads of 10, for patients with highest or unmet needs (Reference Crlenjak, Gee and DuffCrlenjak 2008).
Duration of care
Services vary in the tenure of care offered to patients, but the usual duration is 2–3 years. In the UK, early intervention services were established to provide a 3-year fixed term, whereas early intervention services in Australia provide up to 3 years, titrating length of care against need. There is increasing recognition that 2–3 years is not adequate for a significant minority of people with first-episode psychosis and some services now provide up to 5 years’ care for selected patients, to cover the critical period (Reference Murphy, Simms and DowlingMurphy 2009).
Stand-alone v. embedded services
Early intervention services may either be stand-alone, where they work only with first-episode psychosis, or embedded, where they are part of community mental health teams. A key benefit of the embedded model is the potential for more seamless continuity and shared responsibility for the early intervention cohort; the key disadvantage is the potential for dilution of the early intervention philosophy (Reference Murphy, Simms and DowlingMurphy 2009). The adopted model is often influenced by feasibility and economies of scale, rather than particular ideological frameworks. For example, healthcare providers with large catchment areas may have sufficient patients to justify a stand-alone early intervention service, whereas those serving smaller populations may not. Similarly, the ability to introduce a hub-and-spoke model, where services develop satellite clinics in a bid to tailor themselves to the needs of the community, may be a function of size.
Research programmes
The establishment of early intervention services has enabled crucial evidence to be amassed (Reference McGorry, Johanessen and LewisMcGorry 2010a). Hybrid clinical–research programmes hold key advantages (Reference Good, Brewer, Kopola, Ehmann, MacEwan and HonerGood 2004). Supplementary research resources can lead to enhanced and more comprehensive care, with patients, carers and staff having ready access to cutting-edge evidence. Evidence-based practice can be more easily assessed in a clinical setting, and the embedding of research and clinical frameworks in a single service enables ongoing, efficient evaluation of the work of both. Furthermore, such a unit can attract leading international researchers and clinicians.
It is important that embedded research resources do not become an exploitative rationale for reduced public funding of early intervention services. Similarly, the misperception that scarce clinical resources are being diverted to support research requires containment. Such polarising perspectives serve only to dilute the advantages pointed out by Reference Good, Brewer, Kopola, Ehmann, MacEwan and HonerGood et al (2004).
Specialised components
Comprehensive early intervention services ideally incorporate a number of additional components such as those listed in Box 3.
BOX 3 Additional service components
-
• A prodrome clinic
-
• Community and referrer education and awareness campaigns
-
• Dedicated in-patient services
-
• A crisis team
-
• Specialised subprogrammes such as group programmes
-
• Physical health monitoring
Prodrome clinics
Prodrome clinics target help-seeking individuals identified as likely to be at incipient risk of developing psychosis. Their key advantage is that those who meet intake criteria have a better chance of responding to the benefits of early intervention, such as ameliorating the severity of, and extent of trajectory into, crystallised illness. A further advantage is that prodrome clinics also identify cohorts of patients at risk of developing non-psychotic disorders. The challenge here is to differentiate presentations, as the early stages of both psychotic and non-psychotic disorders have overlapping phenotypes (Reference McGorry, Nelson and GoldstoneMcGorry 2010b). Prodrome clinics, then, are ideally positioned to further refine our understanding of illness genesis across the diagnostic spectrum.
A key disadvantage is that prodrome clinics fail to cater for the majority of those with first-episode psychosis, as these individuals generally do not seek help. This suggests a need to review intake criteria and increase public awareness. Other problems include an excess of false positives, which leads to the risk that early intervention services will become overburdened, and the issue of treating individuals at ultra-high risk of psychosis; even in the presence of psychosis-like symptoms, only 40–60% progress to psychosis (Reference van Os, Linscott and Myin-Germeysvan Os 2009). This triggers anxieties and strong debate over whether to treat prodromal symptoms with antipsychotics. Certainly, methods to improve the detection of true cases, including the determining and measuring of premorbid risk factors, need continual refinement (Reference MurphyMurphy 2010).
Current international clinical guidelines are conservative and suggest a generalist approach to treatment during the prodrome, with monitoring and psychosocial interventions (International Early Psychosis Association Writing Group 2005). Positive results have been reported for a number of intervention studies. These include randomised controlled trials (RCTs) of cognitive–behavioural therapy (CBT), low-dose risperidone and essential fatty acids, and open-label trials of antidepressants, aripiprazole and the amino acid glycine (for review see Reference McGorry, Nelson and GoldstoneMcGorry 2010b). Olanzapine was not found to be beneficial (Reference McGlashan, Zipursky and PerkinsMcGlashan 2006).
Early prodromal symptoms – negative symptoms, anxiety and depression – can merge imperceptibly with attenuated psychotic symptoms until precipitation into frank psychosis occurs. Initiation of antipsychotics in the early prodrome may be unhelpful, since these early symptoms are largely refractory to antipsychotic medication (Reference Murphy, Chung and ParkMurphy 2006). Symptom-specific treatments such as antidepressants and CBT are likely to be of more benefit. They also serve to minimise iatrogenesis arising from the ‘treatment’ of false positives. In true cases, it is the onset of attenuated psychotic symptoms that is likely to represent the start of the individual’s psychosis, not the diagnostic classificatory requirements for established symptoms of prolonged duration (World Health Organization 1992; American Psychiatric Association 1994). It is not until such symptoms begin that antipsychotics are likely to be beneficial, although initiation at this stage can significantly improve the prognosis. Differentiating true cases from false positives (with psychotic-like or spontaneously resolving symptoms), however, continues to be problematic.
In-patient units
A focus on early intervention minimises the need for later traumatic and restrictive forms of care, including involuntary hospital admission (Reference McGorry, Johanessen and LewisMcGorry 2010a). Nevertheless, the majority of people with first-episode psychosis require at least one in-patient admission (Reference Wade, Harrigan and HarrisWade 2006). For these individuals, it is important to reduce iatrogenicity by avoiding exposure to adult wards, with their high rates of seclusion, chronically ill older patients and overreliance on rapidly titrated high-dose antipsychotics (Reference Murphy, Simms and DowlingMurphy 2009). In-patient care should be provided either in specialised early psychosis units that are age and developmentally appropriate or on a youth ward. Wards should be small in bed numbers and have enough staff to prevent locking of the unit (Reference Bertolote and McGorryBertolote 2005).
Subprogramme development
A significant effect of focusing specialised services on first-episode cohorts has been an increased understanding of the variable trajectories of illness progression. The original ‘one size fits all’ model of early intervention services has revealed subgroups of patients with unmet need. These include people with premorbid cognitive risk factors, dissociative borderline personality features, antisocial and/or drug-induced psychosis, and treatment resistance, all of which are conditions that benefit from bespoke treatment initiatives. Articulation of inclusion criteria inherently serves to identify and characterise subgroups, and leads to a more practical focus for research and future funding.
Specialised formal subprogrammes might include neuropsychology and intensive case management for patients at high risk of homicide, suicide and/or disengagement, treatment resistance or persisting negative symptoms, comorbid autism-spectrum disorders, and psychosis with a predominantly Axis II and/or substance-induced foundation.
Effectiveness of early intervention
It is difficult to appraise and synthesise the literature on effectiveness of early intervention in psychosis: the complexity of multicomponent intervention means it is unlikely that specialised teams are identical, making comparisons difficult (Reference Marshall and RathboneMarshall 2006). This is reflected in the Cochrane Database findings, which quantitatively reviewed the efficacy of RCTs of early intervention. Of the 65 studies identified, 58 were excluded for methodological reasons, resulting in inconclusive findings (Reference Marshall and RathboneMarshall 2006). Nevertheless, there is gathering evidence of the benefits of specialised early intervention services across a range of study designs (Reference Catts, O'Toole and CarrCatts 2010). Indeed, there is more evidence supporting early intervention in psychosis than all other recent mental healthcare service initiatives, including assertive community treatment and home treatment services (Reference Lester, Birchwood and BryanLester 2009).
Several RCTs in the UK, Norway and Denmark have demonstrated various beneficial results, including improved clinical, social and vocational outcomes, reduced in-patient stays and better engagement (Reference SinghSingh 2010). Early intervention services have also been found to significantly reduce the risk of a second episode (Reference Alvarez-Jimenez, Parker and HetrickAlvarez-Jiménez 2011) and are highly valued by service users and carers (Reference Lester, Birchwood and BryanLester 2009). Identifying and treating patients with a shorter DUP results in less severe symptoms, reduced suicidality (Reference Melle, Larsen and HaahrMelle 2004; Reference Larsen, Melle and AuestadLarsen 2006) and better functional and social outcomes at 2 years (Reference Melle, Larsen and HaahrMelle 2008; Reference Larsen, Melle and AuestadLarsen 2011). Patients with a longer DUP, and consequently an expected poorer prognosis, are also engaged and treated earlier and more effectively in early intervention than in generic services (Reference Friis, Vaglum and HaahrFriis 2005), supporting the argument that even the cohort with the most severe symptoms benefits from early specialised care. Providing general practitioners with education sessions and easy access to early intervention services increases referrals, but does not necessarily reduce DUP (Reference Power, Iacoponi and ReynoldsPower 2007).
Duration of treatment
It does appear that length of tenure determines outcome in the longer term, and that gains made are lost when patients are discharged to generic services (Reference Bertelsen, Jeppesen and PetersenBertelsen 2009; Reference Gafoor, Nitsch and McCroneGafoor 2010; Reference Henry, Amminger and HarrisHenry 2010). Rather than indicating a failure of early intervention services, this is more likely to reflect an insufficient period of exposure to their therapeutic benefits. A study showing a well-functioning cohort on discharge from early intervention services who subsequently deteriorate would help clarify this. There remains uncertainty about how long such intensive early intervention should last and whether all patients need the same length of care (Reference SinghSingh 2010). Most services provide 2–3 years of care (Reference Tiffin and GloverTiffin 2007). However, it appears intuitive to ensure intensive intervention to cover the ‘critical period’ for at least the more severely ill patients, and some services are now retaining selected patients for this duration (Reference Murphy, Simms and DowlingMurphy 2009).
Although it is clear that there is a humanitarian imperative to offer bespoke treatment at onset, the concept of the critical period itself presents a dilemma. Although there is evidence of neurobiological and neurocognitive changes prior to, and at, early onset, these are relatively unstable (Reference Pantelis, Yucel and BoraPantelis 2009). Recent evidence does indicate that neurobiological interventions are beneficial in ameliorating transition to psychosis, but further longitudinal research is required (Reference McGorry, Nelson and AmmingerMcGorry 2009).
Areas for further research
Future research should attempt to clarify not only which patients are likely to benefit from extended care, but the key therapeutic ingredients of early intervention services that are effective. This, in turn, would inform on elements of maintenance care when patients are discharged to generic services (Reference SinghSingh 2010). There is no reason why early intervention initiatives cannot be subsumed within generic programmes, provided that the key therapeutic ingredients are resourced and maintained. This would, however, require a significant change in philosophy for generic service providers, who have traditionally failed to deliver, thus providing the rationale for development of early intervention services in the first place. It is a moot point whether any of the specialised subprogrammes or research findings would have been produced within a generic service structure.
Undoubtedly, healthy debate is to be encouraged, and those few within generic services who advocate for the delivery of sustained specialised intervention are to be applauded (Reference Castle, Bosanac and PattonCastle 2010), but a focus on resourcing clinical research frameworks that further characterise and refine these subgroups is likely to be a more productive way forward.
Finally, regarding cost-effectiveness, there is a growing, consistent body of evidence, all of which reports the economic benefits of early intervention services, mainly due to reduced bed-days (Reference Catts, O'Toole and CarrCatts 2010; Reference SinghSingh 2010).
Extended care
Determining which patients will need extended tenure (and which will not) is crucial for the continuing viability and effectiveness of early intervention services. Furthermore, early identification of schizophrenia in first-episode psychosis may help avoid inappropriate treatment and enhance long-term outcomes (Reference Ramirez, Arranz and SalavertRamirez 2010).
The DUP
Although the meaning of ‘duration of untreated psychosis’ might seem clear – it is the period from onset of psychosis to the start of treatment – precise definitions vary widely in practice and there is no consensus over when it begins and, to a lesser degree, ends (Reference SinghSingh 2007). In early intervention services, the DUP is commonly used as a stand-alone predictor of outcome, despite its modest abilities in predicting recovery in both the short and medium term (Reference Marshall, Lewis and LockwoodMarshall 2005; Reference Perkins, Gu and BotevaPerkins 2005). There has been justifiable criticism of this usage (Reference Bosanac, Patton and CastleBosanac 2010), but the overemphasis on DUP in the early intervention community may be related to its historical importance in justifying capital funding.
The use of the DUP as a stand-alone measure of prognosis has a number of limitations. First, it fails to capture the true ‘pathogenic portrait’ for many individuals with psychosis who have suffered significant premorbid adjustment problems. Second, it does not inform on the prodrome, which may extend for a number of years before the onset of psychosis. Finally, since the offset of the DUP coincides with treatment, it does not take into account the toxic effects of ongoing psychosis that affect many patients.
Prognosis in schizophrenia
There are a host of known and putative premorbid risk factors for schizophrenia that might add prognostic weight (for a review see Reference MurphyMurphy 2010), yet are not routinely used. Among them is premorbid adjustment, which has a distinguished track record in prognosis (Reference McGlashanMcGlashan 2008). Although there is currently no predictive model incorporating premorbid risk factors, it makes sense to map them clinically to gain a more accurate sense of which patients are likely to progress to schizophrenia and, of those that do, which are likely to have worse outcomes. In this mapping, the presence of known risk factors can be combined with DUP, clinical characteristics and other prognostic indicators – including the postmorbid risk factors of ongoing positive, negative and cognitive symptoms, medication non-adherence and ongoing substance misuse (Reference MurphyMurphy 2010). By engaging in this process, early intervention services should be able to better predict those who would benefit from continued treatment, titrating care against need.
In the second of our two articles in this issue (Reference Murphy and BrewerMurphy 2011), we discuss clinical aspects of early intervention.
MCQs
Select the single best option for each question stem
-
1 The city considered to be the cradle of early intervention in psychosis is:
-
a Vancouver
-
b Melbourne
-
c London
-
d Stockholm
-
e New York.
-
-
2 Which of the following is not a key principle of service provision?
-
a youth-friendly in-patient and out-patient services
-
b targeted psychological interventions
-
c focus on early detection, recovery and relapse prevention
-
d in-patient admission to ensure comprehensive assessment of all first-episode cases
-
e low-dose antipsychotic medication.
-
-
3 Most early intervention services have fixed case-loads of:
-
a 5
-
b 10
-
c 15
-
d 20
-
e 25.
-
-
4 Which of the following is not a specialised component of early intervention services?
-
a a crisis team
-
b an in-patient unit
-
c a prodrome clinic
-
d a community and referrer education and awareness programme
-
e a speech therapy clinic.
-
-
5 The critical period refers to the following length of time from psychosis onset:
-
a 1 week
-
b 1 month
-
c 1 year
-
d 3–5 years
-
e 5–10 years.
-
MCQ answers
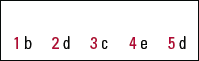
| 1 | b | 2 | d | 3 | c | 4 | e | 5 | d |



eLetters
No eLetters have been published for this article.