The high prevalence of malnutrition in hospitalized children has led to an interest in routine screening on admission(Reference Aurangzeb, Whitten and Harrison1). However, malnutrition screening tools (MSTs) validated in children are still scarce, particularly in their association to clinical outcomes. The study aimed to determine the associations between 3 MSTs and clinical outcomes (length of stay-LOS; complications: infection, delayed wound healing, transfer to another hospital or unplanned use artificial nutrition; decreased weight during hospitalisation) in children admitted to a tertiary referral hospital, compared to baseline weight and body composition (BC) scores.
Paediatric patients (n = 152, mean age 10·7 yr; 50 % male; 51·3 % surgical) with an expected stay >3d were enrolled in the study. 3 MSTs (Paediatric Yorkhill Malnutrition Score-PYMS; Screening Tool for the Assessment of Malnutrition in Paediatrics-STAMP; Screening Tool for Risk of Impaired Nutritional Status and Growth-STRONG) were used. Weight (WT), height and BC measurements (lean (LM) and fat mass (FM) using dual Energy X-ray Absorptiometry) were obtained within 48 hours of admission and SD scores (SDS) calculated using UK BC reference data(Reference Wells, Williams and Chomtho2). Discharge WT, LOS and complications during stay were also recorded.
Most patients were classified as moderate risk (MR) by STAMP and STRONG, and low risk (LR) by PYMS. All MSTs had a significant association with increased LOS and, although HR patients had a tendency for higher complication rates, this was not significant. A decreased weight during hospitalization as marker for worsening nutritional status was found in 43 % of HR patients by PYMS, but was not significant for the other tools. In comparison, low WT or BC scores on admission were significantly associated with an increased LOS and, particularly in the case of low LM, complications and worsening nutritional status.
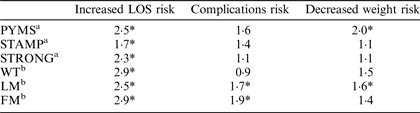
aRisk ratio for HR patients compared to MR or LR. bRisk ratio for patients with a SDS<−2 compared to those with normal SDS; * significantly increased risk P < 0·05
The results confirm children have a high risk of malnutrition on admission, with proportions varying according to the MST used. All MSTs had significant associations with LOS and, in the case of PYMS, for worsening nutritional status. Baseline BC, particularly low LM, was better able to predict these clinical outcomes. Thus, different MSTs seem to show strengths and limitations, as compared to BC/WT measurements, that suggest further validation might be necessary for different settings using specific clinical outcomes.


