The prevalence of obesity is increasing among Chinese urban adults due to rapid economic development and lifestyle changes in China( Reference Reynolds, Gu and Whelton 1 – Reference Meguid El Nahas and Bello 3 ). In a national survey carried out from 2000 to 2001, Reynolds et al. ( Reference Reynolds, Gu and Whelton 1 ) reported high overweight and obesity prevalence rates of 52·5 and 13·1 %, respectively, for men and 48·4 and 12·8 %, respectively, for women in urban regions. Obesity significantly elevates the risk of CVD, diabetes, insulin resistance and other metabolic disorders( Reference Zalesin, Franklin and Miller 4 , Reference Nordmann, Nordmann and Briel 5 ). BMI is a widely used anthropometric index for measuring body fatness in clinical practice and epidemiological studies; additionally, BMI is independently associated with CVD risk factors( Reference Berrington de Gonzalez, Hartge and Cerhan 6 , Reference Deurenberg, Yap and van Staveren 7 ). However, indices of central obesity, such as waist circumference (WC) and waist:height ratio (WHtR), are suggested to be better indicators of cardiometabolic risk because they reflect body fat distribution and upper body adiposity( Reference Zhu, Wang and Heshka 8 – Reference Ashwell, Lejeune and McPherson 10 ). Because WC does not account for differences in height, WHtR has been considered a superior predictor than BMI and WC for discriminating CVD risk factors( Reference Park, Choi and Lee 11 – Reference Hsieh and Muto 13 ).
Asians are more likely to have a higher percentage of body fat at lower BMI and WC than Europeans, which may lead to the greater prevalence of CVD risk factors at a relatively lower BMI in Asian populations( Reference Deurenberg, Deurenberg-Yap and Guricci 14 – Reference Chen, Ho and Lam 16 ). The WHO suggests that the cut-off values for public health action for Asians are BMI values ≥ 23 kg/m2 to represent an increased risk of CVD and BMI values ≥ 27·5 kg/m2 to represent a high risk of CVD( 15 ). The International Diabetes Federation has proposed ethnicity-specific WC cut-off points as a prerequisite component of the metabolic syndrome (MetS), with the values ranging from 80 to 90 cm in Asians( Reference Zimmet, Magliano and Matsuzawa 17 ). In response to the recommendations, the Working Group on Obesity in China (WGOC) has suggested that a BMI in excess of 24 kg/m2 or a WC exceeding 85 cm in men and 80 cm in women signifies overweight or central obesity in the general Chinese population, according to thirteen population studies conducted in the 1990s( Reference Bei-Fan 18 ). However, evidence regarding whether different cut-off values are appropriate in Chinese is insufficient( Reference Meguid El Nahas and Bello 3 ). On the other hand, several studies have attempted to determine the optimal cut-off values for WHtR to predict various CVD risk factors based on data from either small-scale or cross-sectional studies, mostly conducted in Taiwan and Hong Kong( Reference Tseng, Chong and Chan 19 – Reference Lin, Lee and Chen 21 ). Most of the available data indicate that a cut-off WHtR value is needed for the general population in Mainland China( Reference He, Zhai and Ma 22 – Reference Liu, Tong and Tong 24 ). Thus, the present population-based study aimed to determine the associations between three anthropometric indices (BMI, WC and WHtR) and common CVD risk factors, including diabetes, hypertension, dyslipidaemia and the MetS; it also aimed to evaluate the optimal cut-off values of these anthropometric indices for urban Chinese adults.
Subjects and methods
Subjects
A large population-based cross-sectional study was carried out in seven nationwide health examination centres between 2008 and 2009. A two-stage cluster random-sampling design was used to determine the risk factors of chronic diseases among Chinese urban adults. In the first stage of sampling, the process was stratified by north v. south, as divided by the Yangtze River. According to economic development and geographical regions, three cities (Beijing, Shijiazhuang and Changchun) from northern China and four cities (Chongqing, Changsha, Hangzhou and Chengdu) from southern China were selected. In the second stage of sampling, one local representative health check-up centre was randomly selected from each city. All individuals who visited the health check-up centre were then selected for the present study. A total of 244 266 examinees aged ≥ 20 years were found to be eligible for the study. Among these, 16 798 subjects without relevant data on demography, blood pressure, and glucose and lipid concentrations, 5780 subjects with a history of cancer that might affect the measurements of anthropometric factors, and 418 subjects who were pregnant or lactating at the time of examination were excluded. The remaining subjects comprised 137 256 men (mean age 45·61 (sd 14·28) years) and 84 014 women (mean age 43·79 (sd 13·58) years). The present study was conducted according to the guidelines laid down in the Declaration of Helsinki and was approved by the Ethics Committee of the Chinese People's Liberation Army General Hospital and the Chinese Society of Health Management. Written informed consent was obtained from all subjects.
Measurements
Anthropometric measurements were conducted in subjects in barefoot and light clothing. Height, WC (measured to the nearest 0·1 cm) and weight (measured to the nearest 0·1 kg) were measured by trained personnel using standardised techniques and equipments. WC was measured midway between the inferior margin of the last rib and the crest of the ileum in a horizontal plane. BMI was calculated as weight (kg) divided by height squared (m2). WHtR was calculated as WC (cm) divided by height (cm). After 10 min of rest while seated, the same staff measured systolic blood pressure and diastolic blood pressure in the right arm using an appropriate electronic sphygmomanometer. A venous blood sample was collected in the morning after a fast of at least 8 h; this blood sample was used for measuring plasma glucose, TAG, total cholesterol and HDL-cholesterol concentrations in the clinical laboratory of the People's Liberation Army General Hospital. LDL-cholesterol was quantified using the Friedewald formula:
Definitions
Diabetes was defined as either having fasting plasma glucose concentrations ≥ 7·0 mmol/l or physician-diagnosed diabetes. Hypertension was defined as having systolic blood pressure ≥ 140 mmHg and/or diastolic blood pressure ≥ 90 mmHg or as physician-diagnosed hypertension. Dyslipidaemia was defined as having plasma total cholesterol concentrations ≥ 6·22 mmol/l and/or fasting TAG concentrations ≥ 2·26 mmol/l and/or LDL-cholesterol concentrations ≥ 4·14 mmol/l and/or HDL-cholesterol concentrations < 1·04 mmol/l( 25 ). The MetS was defined as the presence of at least two of the following: plasma TAG concentrations >1·70 mmol/l; HDL-cholesterol concentrations < 1·04 mmol/l; blood pressure >130/85 mmHg; fasting plasma glucose concentrations >5·6 mmol/l; 2 h oral glucose tolerance test plasma glucose concentrations >7·8 mmol/l, which are similar to those used in recently published studies( Reference Dong, Liu and Yang 23 ).
Statistical analyses
All variables are expressed as means and standard deviations or percentages where appropriate. Groups were compared using Student's t test for continuous variables and the χ2 test for categorical variables. Receiver operating characteristic (ROC) analyses were carried out to compare predictive ability and to calculate optimal cut-off values for each anthropometric parameter and risk condition. The area under the ROC curve (AUROC) is a measure of the diagnostic power of a test. An AUROC of 1 indicates a perfect prediction and an AUROC of 0·5 indicates the absence of predictive power. Optimal cut-off values were defined as the points on the ROC curve where Youden's index (sensitivity+specificity − 1) was the highest. Differences between two AUROC were tested with Z values:
![]() $$Z = \frac {( A _{A} - A _{B})}{\sqrt {( S _{EA}^{2} + S _{EB}^{2})}}, $$
with Z>1·96, P< 0·05, and with Z>2·58, P< 0·01. OR were calculated by applying logistic regression models. Statistical inference was based on 95 % CI and 5 % P values, respectively. All statistical analyses involved the use of SPSS version 19.0 (IBM, Inc.).
$$Z = \frac {( A _{A} - A _{B})}{\sqrt {( S _{EA}^{2} + S _{EB}^{2})}}, $$
with Z>1·96, P< 0·05, and with Z>2·58, P< 0·01. OR were calculated by applying logistic regression models. Statistical inference was based on 95 % CI and 5 % P values, respectively. All statistical analyses involved the use of SPSS version 19.0 (IBM, Inc.).
Results
The characteristics of the study population according to sex and 10-year age groups are given in Table 1. Men aged 20–69 years had higher BMI values than women, while men and women aged ≥ 70 years had similar BMI values. Men and women of a similar age were more likely to have higher WC values in all age groups; men aged 50–59 years also had higher WHtR values. Significant age-related differences were also observed: all anthropometric measures tended to reach the highest level by the late 50s in men, while they gradually increased with age in women. In addition, men were more likely to have higher fasting glucose concentrations, higher blood pressure values and more adverse lipid profiles when compared with women. The percentage of men with diabetes, hypertension, dyslipidaemia and the MetS was significantly higher than that of women in each age group. Dyslipidaemia and the MetS were more prevalent in men than in women. The prevalence of all risk factors increased substantially with an increase in age in both sexes, except for a slight drop in the risk of dyslipidaemia in men aged ≥ 60 years.
Table 1 Characteristics of the study population (Mean values and standard deviations; number of participants and percentages)

WC, waist circumference; WHtR, waist:height ratio; FBG, fasting blood glucose; SBP, systolic blood pressure; DBP, diastolic blood pressure; TC, total cholesterol; HDL-C, HDL-cholesterol; LDL-C, LDL-cholesterol; MetS, metabolic syndrome.
Mean value was significantly different from that of women within an age group: * P< 0·05, *** P< 0·001.
ROC curves are shown in Fig. 1. The OR and AUROC for BMI, WC and WHtR in relation to CVD risk factors are given in Table 2. Expressed per 1 sd increment in anthropometric indices, WHtR corresponded to significantly higher OR for hypertension, dyslipidaemia and the MetS in men, while WC corresponded to higher OR for all CVD risk factors in men when compared with other indices in women. The AUROC for BMI ranged between 0·626 and 0·708 kg/m2 for men and between 0·599 and 0·765 kg/m2 for women. The AUROC for WC ranged between 0·642 and 0·711 cm for men and between 0·615 and 0·775 cm for women. The AUROC for WHtR ranged between 0·645 and 0·721 for men and between 0·626 and 0·773 for women. Generally speaking, WHtR had the largest AUROC for all risk factors in both sexes, followed by WC and BMI (P< 0·05). Although WC had larger AUROC than BMI for dyslipidaemia in men, there were no significant differences in the AUROC for WC and BMI (P>0·05). WHtR and WC also performed similarly well for diabetes in women (P>0·05). The AUROC for diabetes, hypertension and the MetS were larger in women than in men, but the AUROC for dyslipidaemia were larger in men than in women (P< 0·05).

Fig. 1 Receiver operating characteristic curves for BMI (![]() ), waist circumference (
), waist circumference (![]() ) and waist:height ratio (
) and waist:height ratio (![]() ) in relation to (a) diabetes, (b) hypertension, (c) dyslipidaemia and (d) the metabolic syndrome. Areas for the curves in men and women are summarised in Table 2. (A colour version of this figure can be found online at http://www.journals.cambridge.org/bjn).
) in relation to (a) diabetes, (b) hypertension, (c) dyslipidaemia and (d) the metabolic syndrome. Areas for the curves in men and women are summarised in Table 2. (A colour version of this figure can be found online at http://www.journals.cambridge.org/bjn).
Table 2 Areas under the receiver operating characteristic curves (AUROC) for various anthropometric indices and CVD risk factors and the metabolic syndrome (MetS) in men and women† (Adjusted odds ratios and 95 % confidence intervals)

WC, waist circumference; WHtR, waist:height ratio.
a,b,cValues with unlike letters were significantly different for AUROC in descending order by sex.
Significantly different between three pairwise comparisons (BMI v. WC, BMI v. WHtR, and WC v. WHtR): * P< 0·05, ** P< 0·01.
† OR were adjusted for age.
The AUROC for various anthropometric indices stratified by 10-year age groups are summarised in Table S1 (available online). In men, the AUROC for CVD risk factors were larger in the younger age groups than in the older age groups. In women, all indices had better discriminatory power for selected metabolic conditions in the middle age groups. WC or WHtR had the largest AUROC for diabetes and dyslipidaemia in both sexes, while BMI had apparently larger AUROC for hypertension. Although BMI had larger AUROC for the MetS in the older age groups of men, there were no significant differences in AUROC for BMI, WC and WHtR in women.
The optimal cut-off values of anthropometric indices determined using the ROC analyses in both sexes are summarised in Tables 3 and 4. In men, the BMI cut-off values that were found to optimally predict the risk of diabetes, hypertension, dyslipidaemia and the MetS ranged from 24·2 to 24·3 kg/m2. The optimal WC cut-off values ranged from 83·8 to 86·3 cm and the optimal WHtR cut-off values varied from 0·50 to 0·51. In women, the optimal BMI cut-off values ranged from 22·4 to 23·3 kg/m2 and the optimal WC cut-off values varied from 73·8 to 77·8 cm. The optimal WHtR cut-off values ranged from 0·47 to 0·49. In addition, the optimal cut-off values of BMI, WC and WHtR were mostly higher for men than for women in each age group, and the differences between sexes decreased with an increase in age (see online supplementary Tables S2 and S3). Men in the middle age groups had higher cut-off values than those in other age groups, while women in younger age groups tended to have lower cut-off values. The optimal cut-off values of BMI and WC varied greatly by sex, age and CVD risk factors, while the optimal cut-off values of WHtR had an upper limit of 0·50 that could be applied in the majority of age groups in both sexes.
Table 3 Cut-off values of BMI, waist circumference (WC) and waist:height ratio (WHtR) that are predictive of CVD risk factors in men

MetS, metabolic syndrome.
* Proposed overweight and obesity criteria according to the Working Group on Obesity in China.
† Obesity criteria for Caucasians according to the WHO.
Table 4 Cut-off values of BMI, waist circumference (WC) and waist:height ratio (WHtR) that are predictive of CVD risk factors in women

MetS, metabolic syndrome.
* Proposed overweight and obesity criteria according to the Working Group on Obesity in China.
† Obesity criteria for Caucasians according to the WHO.
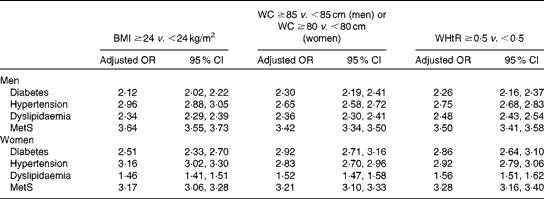
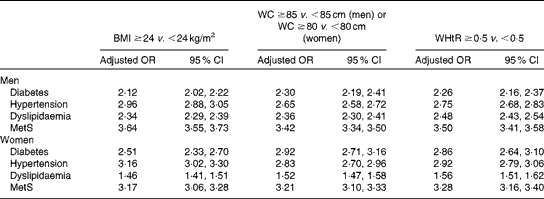
Using the cut-off values of BMI and WC recommended by the WGOC as well as the cut-off value of WHtR determined in the present study, all these obesity indices were found to have a greater than 2-fold increased risk for CVD risk factors, except for dyslipidaemia in women (Table 5). WC and WHtR were superior to BMI in their association with diabetes and dyslipidaemia, whereas BMI was better able to predict the risk of hypertension in both sexes. When compared with other indices, a higher BMI for men and a higher WHtR for women usually had the highest risk predictive power for the MetS. The combined effects of BMI, WC and WHtR are summarised in Table 6. Men and women with a BMI ≥ 24·0 kg/m2 and a WC ≥ 85 (in men) or ≥ 80 cm (in women) had a significantly increased risk than those with a BMI < 24·0 kg/m2 and a WC < 85 (in men) or < 80 cm (in women). Similar results were also obtained for subjects with a BMI ≥ 24·0 kg/m2 and a WHtR ≥ 0·5 in both sexes, suggesting that simultaneous use of both parameters could much improve the predictive power. Higher indices of central obesity were associated with a greater risk of diabetes and dyslipidaemia in normal-weight subjects (BMI < 24·0 kg/m2). However, a higher BMI without a concomitantly higher WC or WHtR was associated with a moderate increased risk for the development of hypertension and the MetS.
Discussion
The present study, carried out using data obtained from more than 220 000 urban adults from Mainland China, showed that WHtR and WC performed better than BMI as a central measure of obesity for discriminating CVD risk factors. The optimal cut-off values for men and women were approximately 24·0 and 23·0 kg/m2 for BMI, 85·0 and 75·0 cm for WC, and 0·50 and 0·48 for WHtR, respectively. It also supports the idea that the combination of BMI and central obesity measures, corresponding to the well-established cut-off values, identifies a particularly greater CVD risk than either of them alone in both sexes.
WHtR has been found to have a stronger association with multiple CVD risk factors in several studies conducted in China( Reference Tseng, Chong and Chan 19 – Reference Lin, Lee and Chen 21 ), Korea( Reference Park, Choi and Lee 11 ), Japan( Reference Hsieh, Yoshinaga and Muto 26 ) and other ethnic groups( Reference Lee, Huxley and Wildman 27 , Reference Ashwell, Gunn and Gibson 28 ). Among the three anthropometric indices, WHtR had the largest AUROC for all CVD risk factors, except for diabetes in women. When the relative risk for a 1-unit change in standard deviation was calculated after controlling for age, WHtR was found to have a stronger association with hypertension, dyslipidaemia and the MetS in men, while WC was found to be a better predictor for all CVD risk factors in women. Thus, our data support the superiority of WHtR and WC over BMI for detecting CVD risk factors in both men and women.
The public health message derived from the data on WHtR is simple: keep your WC to less than half your height( Reference Ashwell and Hsieh 29 ). Optimal cut-off values that fell within the same narrow range of 0·48–0·52 in both sexes were reported by one study carried out in Taiwan( Reference Tseng, Chong and Chan 19 ). Ho et al. ( Reference Ho, Lam and Janus 20 ) recommended an optimal cut-off value of 0·48 for Hong Kong Chinese individuals of both sexes, and He et al. ( Reference He, Zhai and Ma 22 ) defined an optimal cut-off value of 0·50 for predicting the risk of diabetes in both sexes in the Chinese population. Furthermore, Lin et al. ( Reference Lin, Lee and Chen 21 ) reported that a WHtR of 0·48 for men and that of 0·45 for women may be the appropriate cut-off values using health examination data. In addition, several meta-analyses on CVD outcomes carried out on data obtained from Caucasian, Asian and Central American populations in prospective and cross-sectional studies have suggested that a WHtR cut-off value of 0·5 could be applied to different sexes and age groups( Reference Lee, Huxley and Wildman 27 , Reference Ashwell, Gunn and Gibson 28 , Reference Browning, Hsieh and Ashwell 30 ).
A number of studies have shown that Asians have a higher percentage of body fat than Caucasian at lower BMI and WC( Reference Deurenberg, Deurenberg-Yap and Guricci 14 , Reference Deurenberg-Yap, Chew and Deurenberg 31 ). The current definitions of overweight and central obesity are based on Western populations and probably need to be modified for the Chinese population. The WGOC has recently developed the cut-off values for overweight (24·0 kg/m2) using BMI and central obesity (85·0 cm for men and 80·0 cm for women) and WC for the general Chinese population( Reference Bei-Fan 18 ). In the present study, the optimal cut-off values for urban Chinese male and female adults were found to be 24·0 and 23·0 kg/m2 for BMI and 85·0 and 75·0 cm for WC, respectively. Compared with WGOC definitions, these values were very similar in men, but apparently lower in women. Previous studies have indicated that the cut-off values for observed risk varied from 24 to 26 kg/m2 for BMI and from 85 to 87 cm for WC in Taiwanese men and from 22 to 23 kg/m2 for BMI and from 74 to 83 cm for WC in Taiwanese women; similar to the present study population, this study also enrolled subjects from health examination centres( Reference Tseng, Chong and Chan 19 ). Studies in other Asian countries have also reported a BMI cut-off value of 22–24 kg/m2 for men and women and WC cut-off values of about 80–85 cm for men and 75–80 cm for women( Reference Pua and Ong 32 – Reference Moon, Kim and Jang 34 ). Similar to these results, our data suggested that the cut-off points for Chinese urban women might be lower than the criteria suggested by the WGOC, but our data were in agreement with the cut-off values reported for Asian populations with a higher economic status.
Under the current WGOC recommendations, BMI is a more sensitive indicator of hypertension in men and women, while WHtR and WC are better indicators of diabetes and dyslipidaemia. This is agreement with the results of the ROC curve analyses carried out in the present study after stratification by age groups. Dong et al. ( Reference Dong, Liu and Yang 23 ) reported that BMI is more strongly associated with hypertension than WC and WHtR in Chinese men. Another previous study carried out in 29 079 Chinese adults has suggested that the best indicator of hypertension is WHtR in men and BMI in women( Reference Zhou, Hu and Chen 35 ). However, Park et al. ( Reference Park, Choi and Lee 11 ) analysed the OR of each obesity index according to the quartiles and found that WC and WHtR are superior to BMI for predicting the risk of hypertension and other CVD risk factors. The direct comparison between obesity indices based on the OR value becomes less convincing unless a standard unit increment for each measurement is clearly defined and widely accepted. Further studies should assess the association between overall/central obesity and hypertension using different methods. In addition, previous studies have suggested that the combination of BMI and WC has a better predictive power for CVD risk factors than either measure alone( Reference Zhu, Heshka and Wang 36 , Reference Du, Ma and Li 37 ). The results of the present study support the conclusion that those with both BMI and WC values above the cut-off values have a greater risk of diabetes, hypertension, dyslipidaemia and the MetS in both sexes. Similar results were also obtained when BMI and WHtR were used together. In the present study, 12·2 % of normal-weight people had higher WC values ( ≥ 85 cm for men or ≥ 80 cm for women), while 13·3 % had higher WHtR values ( ≥ 0·5 for men and women). This indicates that some non-obese people may already have a central fat distribution with a higher CVD risk than when BMI cut-off values are used alone. These findings suggest that the combined measures of BMI and indices of central obesity are effective for identifying individuals at a higher risk.
The present study investigated the associations between obesity indicators and CVD risk factors in a large population of Mainland China. There are still no clear cut-off values for obesity indices in Asians. The present study used a very large sample covering most age groups to estimate optimal cut-off values to predict CVD risk factors. These data are appropriate for defining cut-off values of BMI, WC and WHtR in Chinese populations. In addition, the high quality of the anthropometric measurements and laboratory data reduced the potential biases and measurement errors. A major limitation of the present study is its cross-sectional design, which cannot be used to establish temporal relationship and causality. Further longitudinal studies are needed to determine these associations. Second, the results should be interpreted with caution because data were collected from individuals who came for health check-ups. Although these individuals were generally more concerned about their health than non-participants, it is unlikely to cause a bias in determining the actual associations between obesity indices and CVD risk factors. Furthermore, data on potential confounders such as smoking and other lifestyles were not collected, which represents another limitation.
In conclusion, the present study showed that WHtR and WC may be better than BMI for discriminating CVD risk factors. Our data suggest that the cut-off values for BMI and WC to define obesity should be much lower in China than in Western countries. Moreover, a global WHtR cut-off value of 0·50 may also be the appropriate upper limit for Chinese urban adults.
Supplementary material
To view supplementary material for this article, please visit http://dx.doi.org/10.1017/S0007114514002657
Acknowledgements
The present study was supported by the State Science and Technology Support Program (grant no. 2012BAI37B04) and the Military Eleventh Five Year Health Promotion Program (grant no. 10BJZ18).
The authors’ contributions are as follows: Q. Z. and Y. H. designed the study; Y. H. analysed the data and wrote the manuscript; Y. H. and S. D. collected and assembled the data; Q. Z., X. Z., Z. C., Z. S., G. C., F. Y. and Y. W. interpreted the data, provided advice or consultation, and approved the final manuscript; Q. Z. obtained funding.
None of the authors has any conflicts of interest to declare.