CASE REPORT
We report a case of Sweet syndrome presenting as a febrile rash in a traveller returning from Cuba. The diagnosis was confirmed on biopsy, and the patient had an excellent response to steroid therapy.
A 46-year-old woman with no previous medical history or known allergies presented to an emergency department with a severely painful rash and fever while on vacation in Cuba. The rash appeared as raised maculopapular lesions on her limbs and trunk with sparing of her head and neck. She had no myalgia, arthralgia, chest pain, shortness of breath, or abdominal pain. She denied sick contacts, ocean exposure, animal bites, sexual contacts, new medications, or intravenous (IV) drug use. Initial treatment with dimenhydrinate provided little relief.
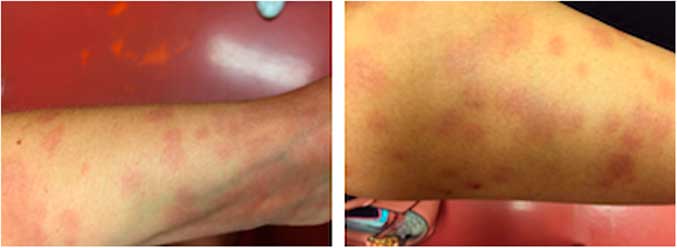
On examination, the patient was hemodynamically stable, febrile, alert, and oriented. She was in a significant amount of pain requiring parenteral opioid therapy. Her physical exam was highlighted by an extremely tender, violaceous, confluent maculopapular rash over her extremities (Figure 1). There were no blisters or vesicles, and Nikolsky sign was negative. There was no mucous membrane or conjunctival involvement. She had a normal oropharynx and no adenopathy. Her neck was supple, her chest clear, and her abdomen was soft.
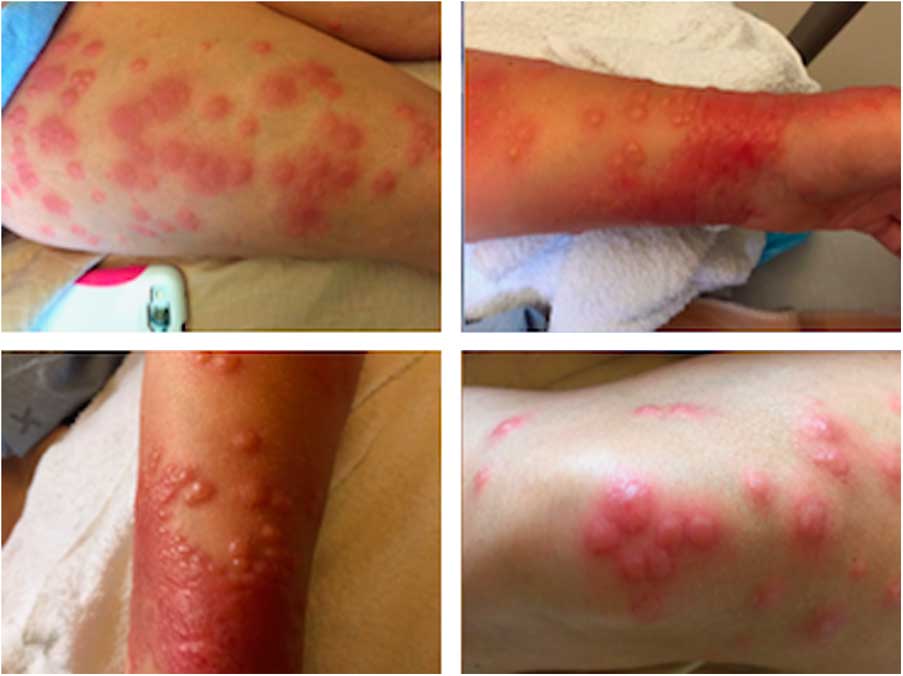
Figure 1 The rash as it appeared on presentation to the emergency department. It is raised and exquisitely tender to the touch. Clockwise from top-left: The patient’s right thigh, left wrist, left knee, and left wrist again.
Initial laboratory findings included an elevated white blood count of 21.9, an absolute neutrophil count of 19.1, an elevated erythrocyte sedimentation rate (ESR) of 104, and a C-reactive protein (CRP) of 80. The remainder of her routine blood work was non-contributory.
The patient was admitted for pain management and additional investigations. Further workup, including blood cultures, hepatitis panel, venereal disease research laboratory (VDRL), human immunodeficiency virus (HIV), rheumatoid arthritis (RA), antinuclear antibody (ANA), dengue, and chikungunya serology were all negative. A skin biopsy demonstrated a nodular infiltrative neutrophilic dermatosis.
The presentation of symptoms and biopsy results were consistent with Sweet syndrome. The patient was started on methylprednisone, 75 mg IV daily during her 24-hour stay and discharged home on 40 mg of prednisone daily with specialist follow-up. The patient experienced rapid and complete resolution of her pain within 72 hours of starting therapy, and the rash faded over several weeks (Figure 2).
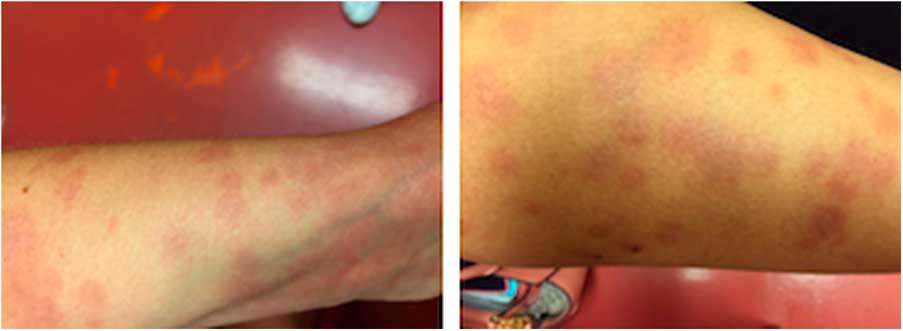
Figure 2 The same rash, as it appeared 1 month following initial steroid therapy. The lesions are flat and non-tender. Left to right: Patient’s left leg, right thigh.
DISCUSSION
A patient presenting with an unusual rash can be diagnostically challenging to even seasoned emergency physicians. A rash arising in a febrile patient returning from the tropics can also be more concerning for zoonoses and other rare diseases that may cloud the clinical picture.
Avoiding such pitfalls is critical. Broadly speaking, most returning travellers with fever will not be suffering from a tropical illness. However, and more specific to our case, a rash presenting without pruritus but with frank pain requiring opiate analgesia is a rash not to be dismissed as benign.
Acute febrile neutrophilic dermatosis, better known as Sweet syndrome, falls under this spectrum. Although the confirmatory test is not available in the emergency setting, Sweet syndrome is a disease pattern that can be readily identified and effectively treated by the astute clinician.
First described in 1964,Reference Sweet 1 reports of Sweet syndrome have been numerous in the literature worldwide and thus should not be relegated as diagnostic esoterica.Reference Tasaduq, Duncan and Wani 2 - Reference Cohen and Kurzrock 4 The disease arises with a heavy prevalence in women but does not appear to discriminate based on race or geography.Reference Abbas, Libbi and Rubeiz 5 Patients can appear severely ill and present, as in our case, with significant pain and distress. Fever typically precedes a focal or disseminated erythematous to violaceous papular or vesicular rash. The syndrome is often associated with arthralgias, myalgias, and a sense of malaise.Reference Cohen and Kurzrock 6 , Reference Cohen and Kurzrock 7 It is not uncommon for this illness to be initially confused with infectious etiologies or, as with our patient, other more benign skin eruptions.Reference Withrow, Shenenberger and Kalish 8 Failure to identify the true etiology leads to a delay in treatment and prolonged suffering.
Unfortunately, the symptoms of Sweet syndrome are as non-specific as its laboratory findings that include neutrophilia and a raised ESR and CRP. Sweet syndrome can be diagnosed only by a skin biopsy, and therefore it is imperative for the emergency department physician to facilitate an urgent biopsy.Reference Abbas, Libbi and Rubeiz 5 , Reference Anzalone and Cohen 9
Sweet syndrome is a disease not to be missed, because it may be associated with undiagnosed underlying malignancies, other inflammatory conditions, or medications.Reference Maalouf, Battistella and Bouaziz 10 , Reference Paydas 11 The patient in our report went on to receive a full age specific malignancy workup, including endoscopy and computed tomography scanning as a result of the strong paraneoplastic associations in patients with Sweet syndrome. The most common inciting pharmaceuticals include granulocyte colony stimulating factor (GCSF), retinoic acids, as well as certain antibiotics and anti-epileptics.Reference Maalouf, Battistella and Bouaziz 10 A thorough medication history should thus be taken because removing the offending agent is imperative.
As soon as the diagnosis is established on biopsy or recognized clinically, treatment is simple and effective. Beyond removing any offending agent and treating underlying causes, pharmacological therapy for Sweet syndrome consists of a course or oral prednisone 0.5 – 1.5 mg/kg/day with a 2- to 6-week taper. Although the rash may persist several days to weeks, the pain will begin to diminish rapidly as it did in 24 hours, in our case. Refractory cases can be treated with 3 days of pulsed high dose methylprednisolone at a dose of 1000 mg/day.Reference Cohen and Kurzrock 7 , Reference Schadt and Callen 12 This case highlights several salient points for the emergency physician to consider. First, not all fevers in returning travellers are from tropical sources. Second, the constellation of signs and symptoms in Sweet syndrome, if recognized early and appropriately, can offer rapid and satisfactory relief to an otherwise suffering patient. Finally, any rash suspicious for Sweet syndrome merits close follow-up and should not be discharged without arranging proper malignancy-related investigations.
Competing interests: None declared.