Introduction
Over the past decade, the use of long-acting reversible contraceptive methods has increased among women in the United States (USA); however, more widespread use was limited by patients and physicians’ concerns (Batur P et al. Reference Batur, Bowersox and McNamara2016). In Lebanon, research on contraception, especially among younger adults, is relatively modest. It was only until 2009 that the first study on contraception use among university students in Lebanon, i.e. the non-married population, was carried out. This study reported that 73.3% of men aged between 18 and 22 years have already had sexual intercourse versus 21.8% of women; and that 86.1% of male students have used a condom while 75.6% of women had never used contraception. That study highlighted the difference among younger men and women in terms of sexual activity outside wedlock and a greater awareness about contraception among men (Barbour B and Salameh P Reference Barbour and Salameh2009). A more recent study enrolling students from 17 universities (including the Lebanese University that enrolled 40% of all students), reported slightly different findings. In fact, 65.2% of men reported having engaged in sexual relations compared to 14.9% of women, and 72.8% of all sexually active participants (21.9% of study population) had used contraception (Salameh P et al. Reference Salameh, Zeenny, Salamé, Waked, Barbour, Zeidan and Baldi2015). Both studies pointed at the impact of religion and family pressure on sexual relations before marriage. However, men might exaggerate their sexual activity to brag about their virility, leading to an overestimation of sexual relations among them (Salameh P, Zeenny R et al. Reference Salameh, Zeenny, Salamé, Waked, Barbour, Zeidan and Baldi2015).
Although Lebanon is reputed to be less conservative than other Middle Eastern countries, with a more liberal lifestyle and mentality, traditional practices still prevail in some Lebanese communities. In particular, female virginity is highly valued in most Arab and Muslim countries, which entails promotion of sexual abstinence outside wedlock and puts pressure on youth, and especially young women, to keep their sexual life limited (Al-Shdayfat NM and Green G Reference Al-Shdayfat and Green2012; AlQuaiz AM et al. Reference AlQuaiz, Kazi and Al Muneef2013). Moreover, parents and overall family relationships exert a strong normative influence on youth in terms of sexual behaviour and practices (Dei M et al. Reference Dei, Bruni, Bettini, Leonetti, Balzi and Pasqua2004). Female empowerment through education also associates with improved contraception (Alabi O et al. Reference Alabi, Odimegwu, De-Wet and Akinyemi2019). The 2009 study reported a greater awareness among female students about sexually transmitted diseases, but also about the side effects associated with contraceptives (Barbour B and Salameh P Reference Barbour and Salameh2009). In addition, urban living, education level and having children (preferably sons) seem to correlate with greater contraception use among Arabs (Farid S Reference Farid1986). On the other side, the Western world remains more open about sexual practices. Over 20 years ago in France, most sexually active women (75% of women in the reproductive age) who did not wish to become pregnant used contraception (Moreau C et al. Reference Moreau, Spira and Bajos2009). In 2016, a survey conducted among French women showed that 71.9% of them used contraceptives, mostly the pill. Intrauterine devices (IUD) were the most commonly adopted method among women (mostly mothers) over the age of 35 years. Teenagers preferred the condom, while implants came third among young women aged between 20 and 24 years, after the pill and condom (Rahib D et al. Reference Rahib, Guen and Lydie2016). Between 2008 and 2014 in the USA, 60% of women used one of the four most common contraceptive methods: pill, female sterilization, condoms and IUDs, in that order (Rahib D, Guen ML et al. Reference Rahib, Guen and Lydie2016). However, a more recent study estimated higher figures at around 85% (Frederiksen BN et al. Reference Frederiksen, Ahrens, Moskosky and Gavin2017).
The aim of the present study was to estimate the extent of awareness, knowledge and use of contraception among university students in Lebanon. Specifically, this study examined the proportion of contraception users among this population, their perceptions about birth control efficacy and adverse effects of long-term contraception use.
Methods
Study design
This was a cross-sectional study designed to enquire about the usage of contraception, and the knowledge and attitudes towards contraception methods among youths in Lebanon. This survey-based study was approved by the Ethics Committee of the Saint Joseph University in Beirut (USJ).
Setting
The study was carried out in nine universities (one public and the rest private) across Lebanon.
Study population and sampling strategy
The study included male and female students, aged between 18 and 25 years, enrolled in university. A 30-item-long questionnaire was broadcasted to 500 students in English (N = 150) or in French (N = 350), via a link shared on WhatsApp® application. The questionnaire collects information about previous or current contraceptive usage: the different contraceptive methods, the reason behind the responders’ choice, their perception on efficacy, on adverse effects and on possible long-term complications. The questionnaire was used as a data collection form, in a series of structured questions on demographics, educational/professional status, experience with contraception, personal stance on contraception use, perceived effectiveness in controlling birth and potential harms that they believe could be incurred by contraception use. Depending on the exact purpose set out by the investigators for each question, responders could either select several answers or only one modality.
Data collection
Data were collected electronically and entered manually on a Microsoft Excel worksheet, by two independent operators. Data were cleaned by a third operator who also reconciled possible entry errors.
Data analysis
Descriptive statistics were performed using Microsoft Excel. Numeric variables were summarized as follows: number of observed values, number of missing data, median, mean and standard deviation (SD). Categorical variables were summarized using frequencies and percentages. Fisher’s exact test was used to evaluate statistical significance, with a threshold set at P < 0.05. Significance was only reported when comparing answers in subgroups of interest (gender-based, age-based and medical versus non-medical studies).
Results
Characteristics of participants
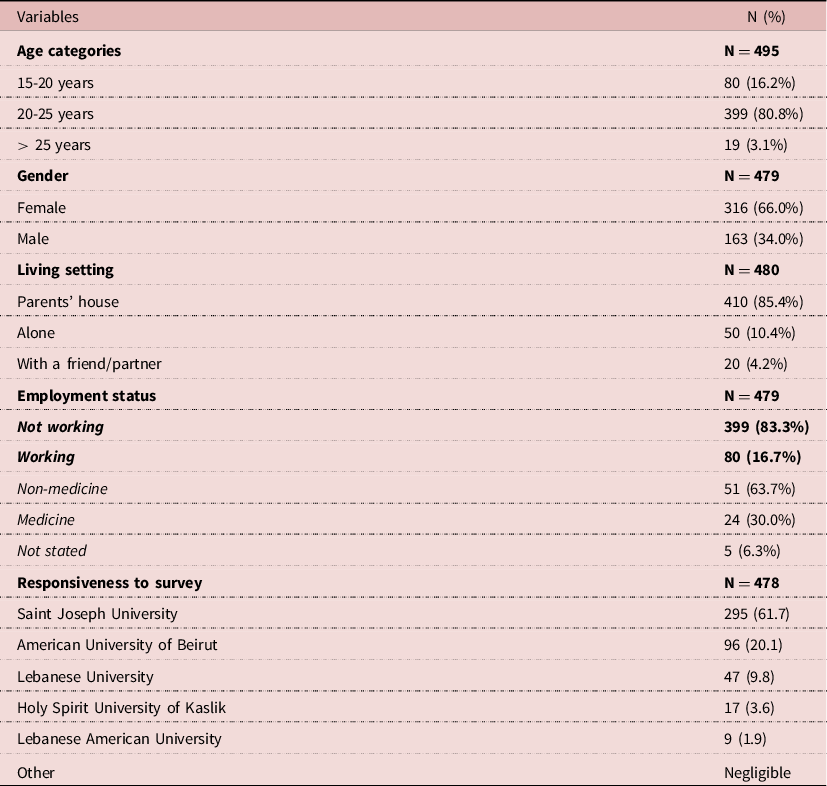
A total of 498 students responded to this survey (Table 1), of which 337 (71.6%) were in medical school. Most responders reported living with their parents (85.4%) and not being employed at the time of the survey (83.3%). Most students who held a job (80 responders [16.7%]) were 20-25 years old. All working non-medical students held non-medical jobs, and only 30.0% of students in the medical field held related. The vast majority of medical students belonged to the medical schools of the USJ (69.1%) or the American University of Beirut (AUB, 27.7%), and student distribution in universities significantly depended on medicine versus non-medicine majors; i.e. most medical students were indeed enrolled in either the USJ or the AUB medical schools.
Table 1. Characteristics of participants
Contraception use
Among responders (N = 476), 39.9% have ever used (currently using or previously used) contraceptive methods, while 60.1% never have (Figure 1A). More students in the medical field used contraception (146 [43.5%]), compared to their non-medicine counterparts (43 [32.6%], P < 0.05). Answers about the use of contraception were significantly different among age groups (15-20 years old [28.6%] compared to 20-25 years old [42.1%], P < 0.01). However, among contraception users, there was a higher proportion of female students (63.7%) compared to male students (36.3%), but this difference did not reach statistical significance (Figure 1A). Among those who have used contraceptive methods, some have used them for over 5 years (7.3%), close to a third have used them for over a year (28.3%), 19.2% for 6-12 months, 19.2% for 1-6 months and others for less than a month (26.0%).
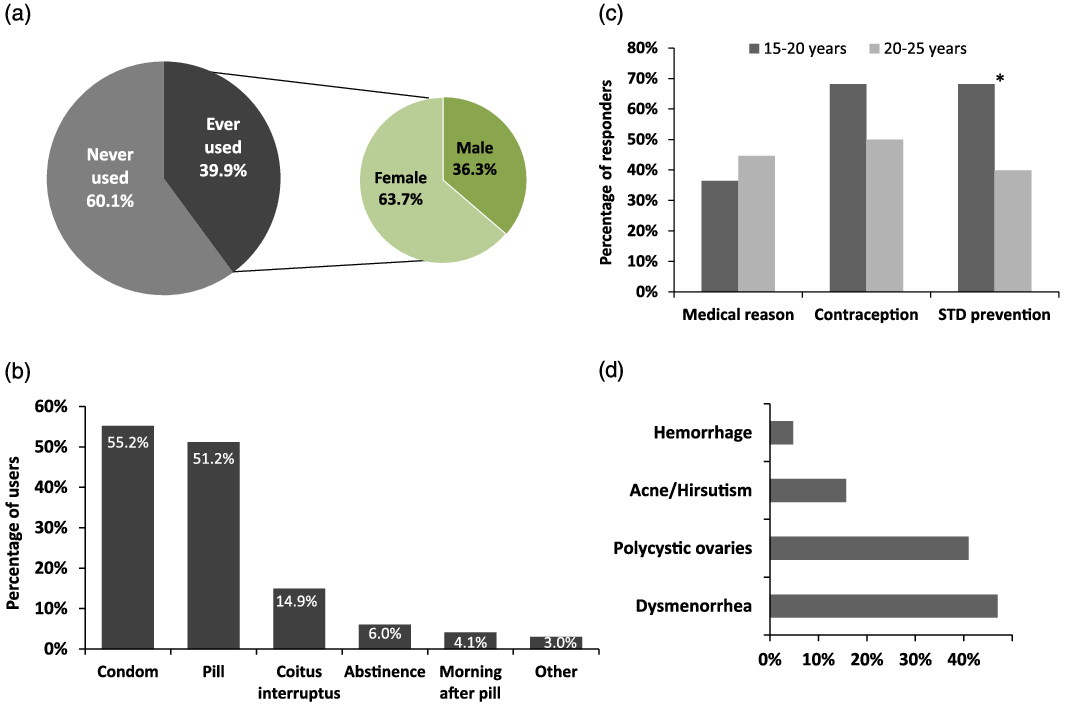
Figure 1. Contraceptive use. (A) Proportion of participants who have used contraceptives. (B) Types of contraceptive methods used. Females mostly use the pill and males mostly the condom, followed by coitus interruptus. (C) Major reasons for use of birth control methods. Students in the younger age group report a greater use of contraceptives for STD prevention than students in the older age group. There were no differences among genders. (D) Reasons for medical non-contraceptive use of the pill among age groups. More than one answer was possible to questions collecting data displayed in panels B, C and D.
Different contraceptive methods
Figure 1B displays the distribution of the different contraceptive methods. Condoms and pills topped the list, followed by coitus interruptus (pull-out method), abstinence, and the morning-after pill. Other methods include hormonal IUD, injectable contraceptives, contraceptive implant, vaginal ring, diaphragm and spermicide. Contraceptive methods were not significantly different among age groups or study field (medical versus non-medical). Out of 102 responders reporting using the pill, the vast majority were women (98%) and out of 110 condom users, men made up 63%. Females reporting use of the male condom as their contraception method probably referred to their partner’s usage of the condom. The total number of male responders reporting condom use was 69 out of 169 males; i.e. 40.8%. A total of 30 people reported withdrawal (coitus interruptus) as their contraception method (21.9% of male versus 10.9% of female contraception users).
A large proportion of responders (74.5%) believe that contraceptive use is easy in Lebanon, while 22.9% did not agree; explaining that some contraceptive methods are not available (26.3%) and the ones that are available are expensive (23.2%). Among responders who complained of the difficult access to contraception in Lebanon (92 students), around one third of medicine students attributed that to elevated prices, around one third of non-medicine students cited unavailability of contraceptives and influence of physician and age. Around a quarter of responders (94 responders [24.9%]) employed contraceptive methods without medical advice (more among medical than non-medical students, P < 0.01), mostly the condom (76.6%), the pill (27.7%) and coitus interruptus (11.7%).
Reasons for using contraception
Among those who have used contraception (189 [40.4%]), only around a half (99 responders [52.4%]) did so for birth control purposes. In fact, responders reported using contraceptives also for medical reasons (84 responders) and/or protection from sexually transmitted diseases (79 responders), as reported in Figure 1C. Figure 1D reports the proportion of contraception use for the different medical reasons, which included majorly dysmenorrhea (47.6% out of 84 contraceptive users for medical reasons) and polycystic ovary syndrome (PCOS, 40.5%).
Although there was no significant difference among contraception users attending public or private universities, results showed that the university type significantly impacted the willingness to use contraception in the future, for any reason or for birth control in particular (P < 0.001). Similarly, higher age (> 25 years) was associated with greater willingness to use of contraception for any reason (P < 0.001).
Participants were also asked about the possibility of using birth control in the future. Positive answers came from 330 responders (77.0%), mostly for birth control purposes (78.5%) or for medical reasons (21.5%). Participants who responded negatively argued that contraceptives entail adverse effects and complications (46.2%) or are not acceptable for religious reasons (30.8%).
Encountered adverse events
Among the 181 responders having previously used contraceptives and who provided answers to that question, 61.9% reported never experiencing any adverse events, while the rest (38.1%) reported having experienced some. Figure 2A displays the different answers in decreasing order. Mood swings, weight gain and headaches were the most frequently reported adverse events, with weight gain being more frequently reported among the younger age group. In fact, this latter side effect was reported in six out of the eight responders (75.0%) aged 15-20 years who have experienced adverse events compared with 20 out of 61 (32.8%) of those aged 20-25 years (P < 0.05). Expectedly, significantly more female (73 [26.7%]) than male (1 [0.7%]) responders have experienced adverse effects of contraception (P < 0.001).

Figure 2. Adverse effects and potential long-term complications of contraceptive use. (A) Mood swings, weight gain, headaches and nausea were the most frequently reported adverse events to contraceptives. (B) List of medical conditions that can be associated with birth control uses according to responders. Pattern-filled bars indicate items that were differently reported or perceived according to age groups (P < 0.05). All adverse effects were reported by female responders (73 students). Responders could report more than one adverse effect or long-term complication.
Knowledge about contraceptive methods
Perception of effectiveness
Among the 165 responders who have used contraception, 15.2% of participants believe that the contraceptive tool they used was not effective, while 83.6% were satisfied with the efficacy of the method used. More medical (231 [68.6%] than non-medical (74 [55.2%]) students considered the pill as effective (P < 0.01); similar trends were reported for the hormonal IUD (P < 0.001), the contraceptive implant (P < 0.05), and male and female condom (P < 0.001). Although statistically not significant, more female contraceptive users (87 [59.2%]) than male users (60 [40.8%]) reported 100% effectiveness of their contraception method.
Perception of the consequences of long-term use of contraceptives
Participants were asked to select items from a list of possible complications that might arise from the chronic use of contraception. Breast, ovarian and endometrial cancer, pulmonary embolism and stroke were the most commonly perceived risks (Figure 2B). Responders belonging to the two age-groups considered for analysis had significantly different perceptions of potential complications that might arise upon chronic contraceptive use. In fact, more students in the 20-25-year-old subgroup considered that pulmonary embolism (P < 0.001), phlebitis (P < 0.001), myocardial infarction (P < 0.05), stroke (P < 0.001) and breast cancer (P < 0.01) were more likely to occur, compared to the younger age-group. Expectedly, a significantly higher proportion of medicine than non-medicine students cited the aforementioned conditions, in addition to diabetes and depression, as potential complications (P < 0.01). There were no gender differences among perceived complications from contraception use, except for depression; 95 female students (29.2%) versus 24 male students (14.2%) attribute the risk of depression to contraception use (P < 0.001).
Discussion
Findings and interpretation
This survey-based study examined the use of contraception among university youths in Lebanon to assess the frequency and the reasons of use, the most common types and the perceptions of individuals regarding efficacy and potential long-term complications. Although a non-negligible proportion of participants (41%) have used contraception, Lebanon ranks below western countries in birth control use; over 70% of women in France have used contraception in 2016 and over 45% of men solely used condoms. In the United States, 85% of women used contraception between 2011 and 2015. In 2009, a study in Lebanon reported higher figures for contraception use among university students (55%); this difference could be due to the fact that over one third of responders were medical field students and over 80% came from the USJ and the AUB, which do not represent 80% of university students in Lebanon.
Sexual activities outside wedlock and use of contraception remain against social custom in some Lebanese communities and are tightly governed by religious and cultural values. While around 22% of participants were sexually active, similar to figures reported in 2015 (Salameh P, Zeenny R et al. Reference Salameh, Zeenny, Salamé, Waked, Barbour, Zeidan and Baldi2015), over 25% of responders declared that they would not use contraception, mostly due to religious constraints or fear of adverse effects. The Catholic Church forbids artificial contraception and sexual acts outside marriage (Mullady B and Ruppersberger L Reference Mullady and Ruppersberger2013), while Islam remains open to contraception (except for minority Islamist jurists), but rejects sexual sterilization (Atighetchi D Reference Atighetchi1994). Barring medical indications, Judaism bans all male contraception methods (abstinence, coitus interruptus, and condoms) but permits female contraception methods (Schenker JG Reference Schenker1987). In addition to religion, cultural factors also influence the acceptance and use of contraception by people from different backgrounds (Srikanthan A and Reid RL Reference Srikanthan and Reid2008); people with lower educational levels and limited finances have less access to birth control and family planning services (Parks C and Peipert JF Reference Parks and Peipert2016; Morse JE et al. Reference Morse, Ramesh and Jackson2017). A recent study indicated that alcohol consumers, living in a Christian-majority area of Lebanon and attending private universities significantly correlated with higher sexual activity (Salameh P, Zeenny R et al. Reference Salameh, Zeenny, Salamé, Waked, Barbour, Zeidan and Baldi2015). The current study did not specifically evaluate the impact of religious and cultural dissimilarities on the differential use of contraceptive methods among Lebanese youth; although religion was mentioned by 30% of students against contraception.
The pill and the male condom topped the list of employed birth control methods (50% of users), given the ease of obtaining them, their relatively low cost and better perceived benefits over other contraceptives; in line with contraception preferences reported by earlier studies among university students. In 2009, over 85% of men have used the condom (Barbour B and Salameh P Reference Barbour and Salameh2009) and in 2015, close to 73% (Salameh P, Zeenny R et al. Reference Salameh, Zeenny, Salamé, Waked, Barbour, Zeidan and Baldi2015); while in the current survey, only 40.8% of male responders reported using the male condom. In addition, among contraception users, close to 50% have used them for medical reasons only, such as menstruation regulation, treatment for PCOS, acne or hirsutism. These indications are justified and beneficial. In fact, some recent studies have reported a favourable effect of the birth control pill to control vaginal bleeding by 35-69% (Kaunitz A Reference Kaunitz2019) and to treat amenorrhea and hirsutism that can be associated with PCOS (Barbieri R and Ehrmann D Reference Barbieri and Ehrmann2019). While in 2009, none of the 1410 responders mentioned healthcare professionals as a source of information on sexual health and contraception use, only 25% of responders in the current study employed contraception without medical advice (Barbour B and Salameh P Reference Barbour and Salameh2009).
The pill, the male condom and the hormonal (levonorgestrel-releasing) IUD were viewed as the most effective contraceptive methods. In fact, long-acting contraceptives can either be reversible or irreversible (such as tube ligation or vasectomy). Among reversible long-acting contraceptives, the subcutaneous implant, the levonorgestrel-releasing IUD and the birth control pill rank low on the Pearl index. The Pearl index, despite some controversy (Trussell J Reference Trussell1991), remains frequently used to report on the effectiveness of a contraceptive selection; a low Pearl index indicates a low pregnancy rate among users of a certain contraceptive (actual versus perfect use) (Pearl R Reference Pearl1933). The effectiveness of the implant, the levonorgestrel-releasing IUD and the birth control pill is comparable to that of the vaginal ring, combined patch and progesterone injection (Chung D et al. Reference Chung, Luzzi, Musy and Narring2015). Of note, the subcutaneous implant was considered most effective due to the inherent absence of the risk of forgetting a dose, contrary to the pill. In the current survey, half of the responders complained about the effectiveness of contraception, which might be attributed to confusion or lack of experience in the matter; indeed the contraceptive pill is often used as a comparator in studies evaluating the effectiveness of contraception methods (Lopez LM et al. Reference Lopez, Grimes, Gallo, Stockton and Schulz2013) and is highly effective if used properly (Stewart M and Black K Reference Stewart and Black2015). In addition, emergency contraception is effective in 95% of cases and should be offered to all women at risk of unwanted pregnancy or who conceive upon sexual assault or contraception failure (World Health Organization 2018).
Nevertheless, dissatisfaction might be due to adverse effects associated with contraception. Responders in the current survey mostly experienced mood swings, weight gain, headache, nausea, breast tenderness, spotting, decreased libido and amenorrhea. However, a 2016 review argues against a direct link between contraception and mood swings, except in women with mood swing predisposition (Schaffir J et al. Reference Schaffir, Worly and Gur2016). Another recent meta-analysis uncouples weight gain and contraceptive use, upon lack of scientific evidence (Gallo MF et al. Reference Gallo, Lopez, Grimes, Carayon, Schulz and Helmerhorst2014). Similarly, headaches are only rarely due to contraception (2%) and are subject to broad variability (Headache Classification Committee of the International Headache Society (IHS) 2013); just like libido change. In fact, over 63.6% of women on contraceptives reported no libido changes, while some reported enhanced libido (21.7%) and only 14.7% decreased libido (Burrows LJ et al. Reference Burrows, Basha and Goldstein2012). Spotting is, however, a common by-product of the pill, especially during the first cycle (Emans SJ et al. Reference Emans, Grace, Woods, Smith, Klein and Merola1987; Rosenberg MJ et al. Reference Rosenberg, Waugh and Stevens1996) and amenorrhea might result due to the limited proliferation of the endometrial mucosa (Fritz MA and Speroff L Reference Fritz and Speroff2011). When asked about long-term complications due to contraception, responders expressed concern about breast cancer, pulmonary embolism, phlebitis, endometrial and ovarian cancer, stroke and other conditions. However, the yearly risk of developing pill-related phlebitis remains 0.006% (Lidegaard Ø et al. Reference Lidegaard, Løkkegaard, Svendsen and Agger2009; Solymoss S Reference Solymoss2011), the risk of arterial thrombosis is 1.6-fold higher in women on the pill (Roach RE et al. Reference Roach, Helmerhorst, Lijfering, Stijnen, Algra and Dekkers2015), and the absolute stroke risk is 5-10 per 100,000 women (Bousser MG et al. Reference Bousser, Conard, Kittner, de Lignières, MacGregor, Massiou, Silberstein and Tzourio2000; Tepper NK et al. Reference Tepper, Whiteman, Zapata, Marchbanks and Curtis2016). Conversely, though associated with a higher risk of breast (Collaborative Group on Hormonal Factors in Breast Cancer 1996) or cervical cancer (Shanta V et al. Reference Shanta, Krishnamurthi, Gajalakshmi, Swaminathan and Ravichandran2000), the pill confers protection against endometrial and ovarian cancer (Iversen L et al. Reference Iversen, Sivasubramaniam, Lee, Fielding and Hannaford2017; Bartz DA et al. Reference Bartz, Roe and Douglas2019). The overall benefits of contraception outweigh the potential risks, which could be mitigated by the use of different contraceptives and close gynaecological follow-up.
Weaknesses
This cross-sectional survey took a snapshot of university students’ attitude and knowledge about contraception in Lebanon. One limitation is the population sample, which might not represent all youths within considered age-groups. Out-of-school youths might indeed have different views and beliefs. In addition, the student sample attending the Lebanese University (public university) was rather limited in comparison with students attending private universities, which does not reflect the reality in Lebanon.
Conclusion
Contraception is frequent among Lebanese university youths, despite some misconceptions identified in this survey. In fact, responders did not know enough about contraceptive efficacy and mistakenly attribute weight gain, mood swings, headaches and libido decrease to contraception use. Female students seemed more inclined to using contraception than their male counterparts, despite having experienced some adverse effects of contraceptives. Contraception and family planning among Lebanese youths should be scaled up, through sexual education, correction of misconceptions, lifting of taboo on sexual health and improved access to contraception.
Acknowledgements
The authors would like to acknowledge the statistical, writing and editing support provided by KBP-Biomak, a contract research organization.
Author contribution
GAT was in charge of study concept and he oversaw the overall conduct of the study and supervised data analysis and manuscript writing. KK, AK, SM, EA and HZ participated in survey elaboration and methodology design, data collection alongside FM, SS and MAA. All authors participated in writing or revising the manuscript, and they all approved the final version.
Conflict of interest
The authors have no conflicts of interest to declare.
Funding
This research received no specific grant from any funding agency, commercial entity or not-for-profit organization.
Disclaimer
The findings and views expressed in the submitted article are not an official position of the participating institutions or authors’ affiliation.





