Patients who occupy in-patient psychiatric beds for prolonged periods have attracted interest in the UK for over 25 years. They have been the focus of two national surveys (Reference Mann and CreeMann & Cree, 1976; Reference Lelliott, Wing and CliffordLelliott et al, 1994) as well as local studies (Reference Lawrence, Cumella and RobertsonLawrence et al, 1988; Reference O'Driscoll, Marshall and ReedO’Driscoll et al, 1990; Reference Patrick and HollowayPatrick & Holloway, 1990; Reference Clifford, Charman and WebbClifford et al, 1991;Reference Thornicroft, Margolius and JonesThornicroft et al, 1992; Reference Kurian, George and BallardKurian et al, 1994; Reference Rowlands, Milner and WingRowlands et al, 1998; Reference Holloway, Wykes and PetchHolloway et al, 1999). A need for longer-term provision for this group was demonstrated by a survey of acute inpatient units, which found that 46% of new long-stay patients were considered inappropriately placed but remained as in-patients on account of their need for specialised rehabilitation places (Reference Shepherd, Beardsmore and MooreShepherd et al, 1997).
The national pattern of provision of longer-term care for adult mental illness is mixed. Overall access to longer-stay beds within the National Health Service (NHS) has been declining. Between 1994/5 and 2000/1 there was a loss of 3630 NHS long-stay beds nationally (not including secure or elderly provision) - a 46% drop. This loss was offset by a gain of 5040 places for adult mental illness in staffed residential homes, small registered residential homes and private nursing homes or hospitals (Department of Health, 2005).
Our study aimed to establish the inception rate into new long-stay status in the admission wards of a service with poor access to long-stay beds and to examine the outcome of these admissions.
Method
The survey took place in Sandwell, a metropolitan borough with a population of 290 091 at the 1991 census, of whom 173 792 were in the 16- to 65-year age-group. Sandwell is a materially deprived, post-industrial area of the West Midlands with an average Townsend score of +4.9 and an unemployment rate of 13.3%. Black and minority ethnic groups comprised 14.7% of the population in 1991. There have been 72 acute in-patient beds available since 1991 and at the time of the study the average length of stay was 35 days. There has been no access to long-stay beds since 1991, and access to contracted rehabilitation beds provided by another trust reduced from four beds in 1996 to none in 1999. After this date all longer-stay in-patient care was on an individual out-of-area placement basis. At the time of the survey there were no assertive outreach or intensive case management teams in operation, nor any specialist rehabilitation team. Community mental health teams have been operating since 1992 and focus on severe mental illness.
During the period of the study the borough had no nursing home for adult mental illness but did have 51 places in highly staffed and 26 places in mid-staffed residential care homes, as defined by Lelliott et al (Reference Lelliott, Audini and Knapp1996). There were also 17 places in supported group homes and 31 supported tenancies. These are relatively low levels of provision when compared with the findings of the national residential care survey (Reference Lelliott, Audini and KnappLelliott et al, 1996). The borough can thus be seen as a good site for examining the experience of new long-stay patients where there is no local access to non-acute hospital beds and limited provision of local supported accommodation.
The study described here retrospectively reviews clinical and demographic data concerning all who entered new long-stay status on admission wards during a 3-year period. Since May 1997 there has been a quarterly census of admission bed occupancy by new long-stay patients using in-patient admission ward lists generated by the trust information department. The practice of the national audit (Reference Lelliott, Wing and CliffordLelliott et al, 1994) was followed in defining the new long-stay group as admissions lasting between 6 months and 3 years.
The hospital records were reviewed of all patients on general adult admission wards aged 16-65 years at admission who reached new long-stay status between May 1997 and April 2000. Data collection was standardised using a pro forma and one investigator (C.C.) reviewed all hospital records. Records from other hospitals were used to obtain outcome data where the patient had moved to another district. Health authority records show five Sandwell patients becoming new long-stay in-patients without entering the admission unit during the period, all in medium secure settings. Approval for the study was obtained from the Sandwell local research ethics committee.
Results
Forty-three new long-stay patients were identified using computerised hospital records. No record could be found for 2 of these, leaving 41 records to be examined. Five were found on looking at the notes to have had stays shorter than the 6 months indicated by the computerised records and were consequently excluded. This left 36 patients in the study and 39 inceptions into new long-stay status, since 3 patients had two episodes each. This gives average inception rates per annum of 4.5 per 100 000 total population. Out of the 39 inceptions, 8 (21%) reached 1 year on the admission ward and 12 reached 1 year in any kind of in-patient setting, including medium-stay facilities provided by other services, giving an inception rate of 1.4 per 100 000 per annum. If the five cases of people who became new long-stay patients outside the local unit are added, the figures become 5.1 per 100 000 per annum and 2.0 per 100 000 for stays over 6 months and over 1 year, respectively.
Clinical and demographic findings
The mean age of the patient studied at index admission was 35.1 years (range 17-64). In 20 admissions (51%) the patients were male. In 27 admissions (69%) the patient was single, 5 (13%) married and 7 (18%) divorced or separated; in 14 (36%) the patient had children; in all cases the patient was unemployed. Prior to the index admission, 18 (46%) had been living alone or with sole care of a child, 15 (38%) with family members, 3 (8%) were in supported accommodation and 3 (8%) were homeless. In 24 (62%) admissions the patient’s diagnosis was of schizophrenia, in 7 (18%) it was schizoaffective disorder, in 4 (10%) bipolar affective disorder, in 2 (5%) depressive disorder, in 1 (3%) adjustment disorder and in 1 (3%) personality disorder. The three people who were admitted twice had diagnoses respectively of schizophrenia, schizoaffective disorder and bipolar disorder on both occasions.
Duration of illness ranged from 1 to 28 years, with a mean of 12.0 years. The number of previous admissions also varied widely, from 0 to 41, with a mean of 7.6 and a median of 5.0. The total time spent as an inpatient in the 5 years before the index admission ranged from 0 to 243 weeks, with a mean of 43.2 weeks and median of 31.0 weeks. Although in 24 (62%) of admissions the patient had not been in hospital during the 3 months before the index admission, in 8 (20%) the patient had been hospitalised within the previous month and in 7 (18%) 1-3 months prior to the index admission.
In 30 cases (77%) the patient had been compulsorily detained in the past: 21% under section 2 only and 56% under section 3. In 31 cases (80%) the patient had been compulsorily detained at some point during the index admission, 13 (33%) at admission and 21 (54%) remained detained at inception into new long-stay status. Twelve (46%) of the informal admissions had become formal by inception. None was subject to a restriction order.
Outcome
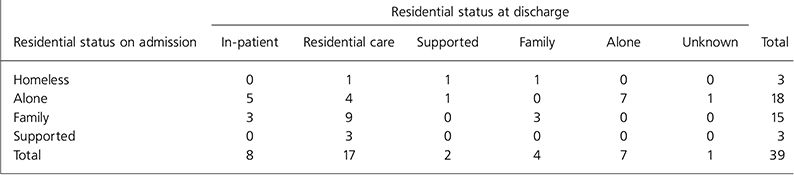
The total length of stay for the index admission ranged from 182 days to 774 days with a mean of 301 days and a median of 250 days. These 39 admissions accounted for approximately 12% of available bed-days in the admission wards over the 3 years. Discharge locations are shown in Table 1. The residential status at discharge compared with residential status prior to admission is shown in Table 2, where family residence includes living with either parents or partner. In residential status prior to admission, the ‘supported’ category includes all kinds of supported living, from supported tenancies to residential care.
Table 1. Discharge locations of new long-stay patients

| Location | n (%) |
|---|---|
| Long-term in-patient | 7 (18) |
| Secure accommodation | 1 (3) |
| Residential care | 17 (44) |
| Supported tenancy | 2 (5) |
| Unsupported alone | 7 (18) |
| Family | 4 (10) |
| Unknown | 1 (3) |
Table 2. Residential status of new long-stay patients at admission v. residential status at discharge
| Residential status at discharge | |||||||
|---|---|---|---|---|---|---|---|
| Residential status on admission | In-patient | Residential care | Supported | Family | Alone | Unknown | Total |
| Homeless | 0 | 1 | 1 | 1 | 0 | 0 | 3 |
| Alone | 5 | 4 | 1 | 0 | 7 | 1 | 18 |
| Family | 3 | 9 | 0 | 3 | 0 | 0 | 15 |
| Supported | 0 | 3 | 0 | 0 | 0 | 0 | 3 |
| Total | 8 | 17 | 2 | 4 | 7 | 1 | 39 |
In 15 (38%) admissions the patient was readmitted in the year after discharge from the admission ward, with the mean time spent in hospital being 47 days. None of those transferred to another in-patient unit was readmitted during the subsequent year, but out of those discharged to the community, 48% were readmitted at some point in the following year.
Discussion
In 36% of the index admissions the patient had been discharged less than 3 months previously, suggesting that the original discharge plans and community services had not proved adequate for individual need. The high levels of compulsory detention at the point of inception into new long-stay status are consistent with results in admission wards elsewhere (Reference Rowlands, Milner and WingRowlands et al, 1998). With 39 admissions taking up 12% of available admission ward capacity, these patients made demands on inpatient services that were greatly disproportionate to their numbers. Discharges in this group appeared to be of limited success, as 48% of those discharged to the community were readmitted over the following year.
New long-stay admissions appear to redirect patients formerly living alone or with family into supported settings. This might indicate that these admissions represent the coping abilities of families or community mental health teams finally being exceeded on account of the severity of need.
Inception rates into new long-stay care over 1 year at 2.0 per 100 000 total population were substantially lower than the estimate of 3.3 per 100 000 from the national audit (Reference Lelliott and WingLelliott & Wing, 1994). The most likely explanation is that discharges take place at an earlier stage on average in a service with limited direct access to longerstay beds. Longer-stay units will have a less hurried approach to discharge than the admission wards, and greater access to such beds will inevitably increase the proportion of new long-stay admissions progressing beyond 1 year.
New long-stay patients still present mental health services with clinical challenges and demands on resources. It is likely that there is a ‘ difficult to place’ subgroup of new long-stay patients, perhaps with treatment-resistant illness, who would benefit from more prolonged in-patient rehabilitation, with the remainder principally needing earlier access to a greater range and availability of highly supported community settings.





eLetters
No eLetters have been published for this article.