Introduction
There are an estimated 9.4 million foodborne illnesses caused by known pathogens in the USA every year [Reference Scallan1]. Although most are sporadic, outbreak-associated illnesses are an important source of information about the foods and pathogens causing illness [Reference Gould2, 3]. Identifying the source of an outbreak is a critical part of containment and removal of the contaminated source from the food supply.
Several factors can affect the quantity and variety of food an individual or family consumes, including income, sex, age, race and ethnicity and health status [Reference Shiferaw4–Reference Dehghan, Akhtar-Danesh and Merchant12]. For example, men are more likely to consume ‘high risk’ foods, including unpasteurised milk, raw shellfish, runny eggs and pink hamburgers than women [Reference Shiferaw4–Reference Shiferaw6]. This difference was also observed for school-aged boys and girls [Reference Shiferaw6–Reference Wardle8]. Women are more likely to consume fruits and vegetables, including alfalfa sprouts, a high-risk food [Reference Shiferaw6]. Differences in consumption patterns between school-aged children and adults have also been shown in national surveys; children are more likely to consume raw fruits and tomatoes, and adults more likely to eat dark green vegetables, cantaloupe and strawberries [Reference Kimmons10].
Given the sex and age differences in food preferences, it remains unknown whether these differences are reflected in the demographics of outbreak-associated foodborne illness. Using data from foodborne disease outbreaks in the USA, we analysed the associations among contaminated food sources and demographics (age and sex) of outbreak-associated illnesses.
Methods
Since 1973, the Centers for Disease Control and Prevention (CDC) has collected data on foodborne disease outbreaks (defined as two or more persons with a similar illness and exposure to a common food) through the Foodborne Disease Outbreak Surveillance System (FDOSS). FDOSS is a passive national surveillance system with state, local, territorial and federal public health agencies reporting outbreaks caused by bacterial, viral, parasitic and chemical agents [Reference Gould2]. Data collected for each outbreak include the implicated food, number of illnesses, reporting state, location of food preparation (e.g. restaurant), etiologic agent, the number and/or proportion of men and women, number and/or proportion of cases aged <5-years-old, 5–19-years-old, 20–49-years-old and ⩾50-years-old. Only confirmed aetiologic agents were included in analyses. Data are reported in aggregate for each outbreak and information on individual cases are not captured in the FDOSS system.
Outbreaks with first illness onset from 1 January 1998 to 31 December 2015, were reported to FDOSS by 20 December 2016, occurred outside of a correctional institute and had a single confirmed implicated food source category (as defined by the Interagency Food Safety Analytics Collaboration) were eligible for inclusion [Reference Braden13]. The 19 categories included beef, pork, chicken, turkey, game, dairy, eggs, fish, shellfish, oils-sugars, grains-beans, nuts-seeds, fruits, fungi, herbs, root-underground vegetables (e.g. carrots, potatoes), seeded vegetables (e.g. legumes, tomatoes), sprouts and vegetable row crops (e.g. asparagus, lettuce) [Reference Braden13]. Outbreaks with ‘other’ (e.g. other poultry) and nonspecific (e.g. land animals) implicated food sources were excluded. During those years, there were 18 938 outbreaks, which caused 355 239 illnesses (median 8, range 2–1939) and of those, 4008 outbreaks causing 75 845 illnesses met the inclusion criteria and were included in the analysis. The majority of excluded outbreaks (n = 10 345, 72%) were excluded due to not having a confirmed implicated food source. Counts of males, females and persons in each age category were calculated using reported proportions when counts were not directly reported by the health department. Overall, outbreak records were missing data on sex for 17 357 (23%) persons and were missing data on age for 29 985 (40%) persons. This missing data were assumed to be missing completely at random, and thus assumed not to bias the estimation of the relationship of sex and age on food category [Reference Little and Rubin14].
We calculated odds ratios using logistic regression on sex and age group (categorised as <5, 5–19, 20–49 (reference) and ⩾50-years-old) for each food category. We used contrast statements to compare individual categories of age to all other ages combined. For multiple comparison testing, we adopted a Bonferroni correction and a P-value < 0.003 was considered statistically significant (at the nominal significance of 0.05). All analyses were performed using SAS 9.4 (SAS Institute., Cary, NC, USA). Institutional Review Board (IRB) exemption was received from Emory University.
Results
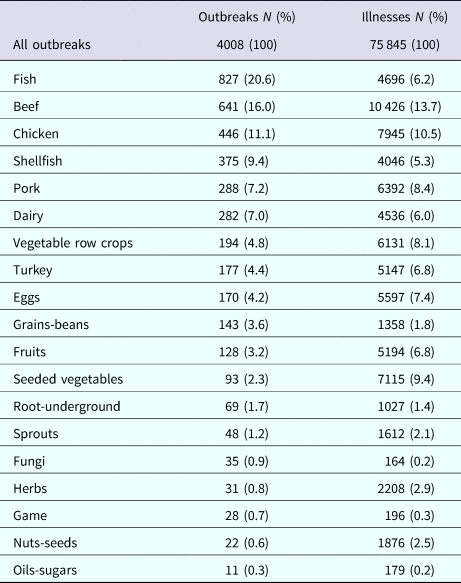
Among the 4008 included outbreaks, fish (21%), beef (16%), chicken (11%), shellfish (9%) and pork (7%) were the five most common implicated food categories (Table 1). Outbreak-associated illnesses were slightly more likely to be in females (54%) than males (46%). By age group, 6% of all cases were <5-years-old, 19% were between 5 and 19-years-old, 47% were between 20 and 49-years-old and 28% were ⩾50-years-old.
Table 1. Frequency of food categories in outbreaks with a single implicated food source and reported to FDOSS between 1998 and 2015

Outbreak aetiology was identified in 59% (n = 2345) of outbreaks, which accounted for 76% of cases (n = 57 992). The most common outbreak categories with viral aetiologies (219 outbreaks) were row crops (25%), shellfish (21%) and beef (12%). Among bacterial outbreaks (1473 outbreaks), over half of all outbreaks were caused by beef (18%), chicken (13%), dairy (14%) and pork (10%) and over half of parasitic outbreaks (n = 43) were caused by game (n = 15, 35%) and fruit (n = 10, 23%). Almost all outbreaks caused by fish toxins (537 outbreaks) were in fish (97%), compared with shellfish (3%). Fish also made up over half (n = 42, 58%) of all outbreaks caused by ‘other’ aetiologies (73 outbreaks).
Males were more likely to be involved in outbreaks attributed to beef (OR 1.17, 95% CI 1.12–1.23), shellfish (OR 1.62, 95% CI 1.50–1.75), pork (1.32, 95% CI 1.25–1.39), dairy (OR 1.24, 95% CI 1.16–1.32) and game (OR 2.55, 95% CI 1.86–3.50), (Table 2). On the other hand, females were more likely to be involved in outbreaks attributed to vegetable row crops (OR 1.41, 95% CI 1.32–1.50), grains-beans (OR 1.27, 95% CI 1.12–1.44), fruits (OR 1.45, 95% CI 1.36–1.54), seeded vegetables (OR 1.10, 95% CI 1.04–1.16), sprouts (OR 1.24, 95% CI 1.10–1.40) and nuts-seeds (OR 1.26, 95% CI 1.14–1.38).
Table 2. Odds of being involved in an outbreak for males, compared with females, given the category in outbreaks reported to FDOSS between 1998 and 2015
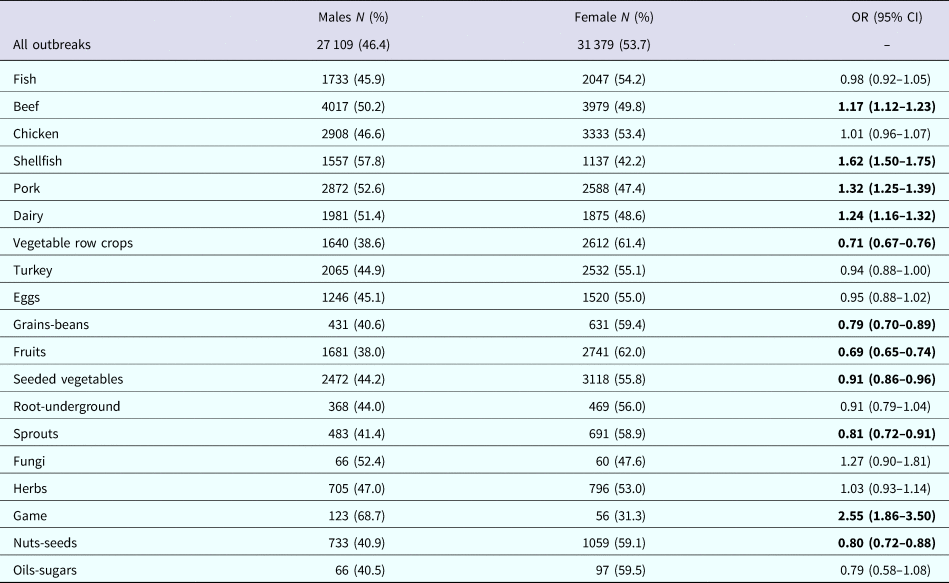
OR, odds ratio; CI, confidence interval.
Bold indicates the significance of P < 0.003 (Bonferroni corrected).
As age increased, the odds of being involved in a dairy outbreak significantly decreased, with children <5-years-old about 3 times as likely (OR 3.18, 95% CI 2.85–3.54), 5–19-yearsold about twice as likely (OR 2.25, 95% CI 2.07–2.45) and adults ⩾50-years-old significantly less likely to be involved (OR 0.71, 95% CI 0.64–0.79) compared with 20–49-years-old (Table 3). To determine whether certain age categories were at the highest or lowest risk compared with those of other ages, we also tested contrasts comparing each age group to all other age groups combined. In these analyses, children <5-years-old were most likely to be involved in dairy (OR 3.18, 95% CI 2.85–3.54), fruit (OR 2.55, 95% CI 2.25–2.89) and seeded vegetable (OR 2.13, 95% CI 1.89–2.40) outbreaks and least likely to be involved in pork (OR 0.65, 95% CI 0.56–0.76), vegetable row crop (OR 0.54, 95% CI 0.45–0.66), or grain-bean (OR 0.57, 95% CI 0.40–0.81) outbreaks. Children 5–19-years-old were most likely to be involved in beef (OR 1.79, 95% CI 1.67–1.92) and game (OR 3.07, 95% CI 1.97–4.78) outbreaks. Adults 20–49-years-old were most likely to be involved in fish (OR 2.72, 95% CI 2.45–3.03), shellfish (OR 4.00, 95% CI 3.29–4.86), root-underground (OR 1.88, 95% CI 1.52–2.34) and sprout (OR 2.12, 95% CI 1.79–2.51) outbreaks and least likely to be involved in nut-seed (OR 0.42, 95% CI 0.41–0.49) outbreaks. Finally, adults ⩾50-years-old were most likely to be involved in turkey (OR 1.94, 95% CI 1.76–2.14) and herb (OR 1.51, 95% CI 1.26–1.82) outbreaks and least likely to be involved in chicken (OR 0.64, 95% CI 0.59–0.69) outbreaks. Egg, fungi and oil-sugar outbreaks had no single age group that was significantly at higher or lower odds than all other age groups combined.
Table 3. Odds of being involved in an outbreak among individuals <5-years-old, 5–19-years-old and ⩾50-years-old, compared with 20–49-years-old, stratified by food category in outbreaks reported to FDOSS between 1998 and 2015
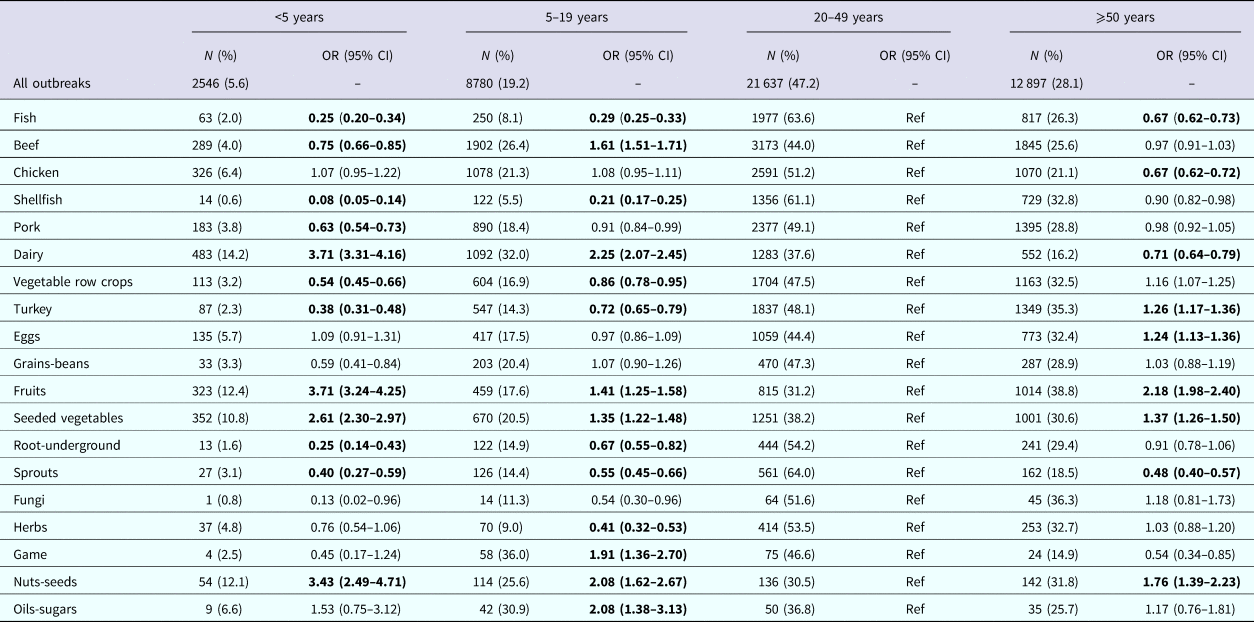
OR, odds ratio; CI, confidence interval.
Bold indicates the significance of P < 0.003 (Bonferroni corrected).
Discussion
Based on an analysis of 18 years of FDOSS data, our results suggest that specific sex and age groups are associated with a higher odds of being in outbreaks from certain foods. These associations might assist in the investigation of the cause of foodborne disease outbreaks. Outbreaks associated with red meats, dairy and shellfish had more males and outbreaks associated with vegetable row crops, grains-beans, fruits, seeded vegetables, sprouts and nuts-seeds were more likely to involve females. Age distributions in outbreaks also varied by food category. Young children (<5-years-old) were most likely to be involved in outbreaks attributed to dairy, fruits and seeded vegetables and children 5–19-years-old were most likely to be involved in outbreaks attributed to beef and game. Additionally, adults 20–49 were most likely to be associated with outbreaks involving fish, shellfish and sprouts and older adults (⩾50-years-old) were most likely to be involved in outbreaks attributed to turkey. This study demonstrates that the demographic distribution of outbreak illnesses might result from the demographically related food preferences. These results are consistent with previous studies of food consumption patterns across age and sex in the USA [Reference Shiferaw4–Reference Dehghan, Akhtar-Danesh and Merchant12]. It is also possible that these results reflect pathogen patterns, as foods can be associated with specific pathogens and age has been shown to be a risk factor for certain types of infections [Reference Painter15–Reference Blanton17].
While this study focused on aggregated outbreak data, age and sex differences in individual outbreaks can be quite striking, making these associations potentially even more useful. For example, in a 2009 multistate outbreak (228 cases, 13 states) involving alfalfa sprouts, 69% of patients were female and the median age was 29 [Reference Safranek18]. And in a 2014 outbreak involving raw milk in Utah (99 cases), 44% of cases were in children <18 years of age, despite this age group only making up roughly 1/4 of all outbreak cases [Reference Davis19]. Moreover, information on food consumption patterns has already been used to further confirm the identification of contamination sources in foodborne disease outbreaks. In a 2004 outbreak of Salmonella Enteritidis infections in Oregon, hypothesis-generating interview results were compared with the food consumption patterns of Oregon residents and helped identify raw almonds as the source of the outbreak [20]. In 2008, the source of an outbreak of Salmonella Agona infections was further confirmed by comparing the percentage of cases reported eating puffed rice cereal with the total ready-to-eat cereal market share in the USA [Reference Russo21]. Recently, a similar prediction tool by White et al. was created to assist in food category identification, specifically for Shiga toxin-producing Escherichia coli outbreaks [Reference White22]. They found that sex distributions predicted the implicated food- with women being more likely to be involved in vegetable outbreaks-, although their analyses were limited to outbreaks caused by beef, vegetables and dairy products. Our analyses also suggest that sex, as well as age, may help in the identification of implicated foods during outbreak investigations.
A limitation of this study is that sex and age are reported in aggregate and therefore interactions between the two variables could not be meaningfully assessed. Future studies could refine these estimates by using datasets where both the age and sex of each case is known. Additional research into more specific food groups may also be required. For example, while young children were most likely to be involved with a nut-seed outbreak, this category included outbreaks caused by whole nuts, nut butter (including peanut butter), crushed/ground seeds (e.g. chia seed powder) and seed paste (e.g. tahini). In this analysis, almost 80% of nut-seed outbreak cases were involved in a peanut butter outbreak and it is very possible that young children may not be more likely to be in outbreaks caused by all of these different nut-seed foods. There was also a high proportion of missing data which we assumed to be missing completely at random and not to be a source of bias in our results, which may not be true. Additionally, FDOSS is a dynamic surveillance system and the results of this study may differ from prior or future reports. Finally, only a small proportion of foodborne illnesses are identified as being associated with outbreaks and many outbreaks never have a food source identified and/or have unknown etiologies. In FDOSS, roughly half of all foodborne outbreaks have no implicated food source and were excluded from this analysis.
Knowledge about associations among outbreak demographic characteristics and contaminated food sources is still limited. As novel contamination routes and outbreak sources continue to become more prevalent, new methods for outbreak source identification will need to be developed. This study suggests that outbreak demographic information may be useful to assist investigators in narrowing down potential contaminated food sources in outbreaks. Additional research is needed to improve food profiling in outbreak investigations.
Author ORCIDs
P. D. Strassle 0000-0002-1072-1560.
Acknowledgements
We thank Daniel Dewey-Mattia and the entire National Outbreak Reporting System (NORS) Team of the Enteric Diseases Epidemiology Branch, Division of Foodborne, Waterborne and Environmental Diseases, National Center for Emerging and Zoonotic Infectious Diseases, Centers for Disease Control and Prevention for their help with this study. The authors would also like to acknowledge state and local health departments for collecting and reporting outbreak data. This research received no specific grant from any funding agency, commercial, or not-for-profit sectors.
Conflict of interest
The authors have no conflicts of interest to disclose. The findings and conclusions are those of the authors and do not necessarily represent the official position of the CDC.